- Neurosurgery Service at Sarah Network of Rehabilitation Hospitals, Brasília, Federal District, Brazil
Correspondence Address:
Romel Corecha Santos
Neurosurgery Service at Sarah Network of Rehabilitation Hospitals, Brasília, Federal District, Brazil
DOI:10.4103/sni.sni_409_17
Copyright: © 2018 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Romel Corecha Santos, Ricardo de Amoreira Gepp. Benefits of spinal meningioma resection. 25-Jan-2018;9:16
How to cite this URL: Romel Corecha Santos, Ricardo de Amoreira Gepp. Benefits of spinal meningioma resection. 25-Jan-2018;9:16. Available from: http://surgicalneurologyint.com/surgicalint-articles/benefits-of-spinal-meningioma-resection/
Abstract
Background:Spinal meningiomas account for approximately 40% of intradural extramedullary tumors. As they are usually slow growing, some patients are often diagnosed late in the clinical course when they have developed myelopathy.
Methods:Here, we retrospectively studied a cohort of 51 patients undergoing surgery for spinal meningiomas. The median follow-up period was 45.9 months (range, 1–168 months). Assessment included evaluation of functional outcomes (e.g., comparison of the pre and postoperative status using the modified McCormick Functional Scale) and identification of prognostic factors.
Results:Seventeen patients with grade IV (McCormick Scale) neurological deficits on admission underwent surgical resection; 4 of 5 grade III (McCormick Scale) and 14 patients (Grade IV) improved within 2.11 months (mean time) postoperatively. There was no surgical mortality and the morbidity rate was 16%.
Conclusion:Patients with advanced neurological deficits/myelopathy (Grades III or IV on the McCormick Scale) improved following surgical resection of spinal meningiomas.
Keywords: Meningioma, rehabilitation, spinal canal, surgery
INTRODUCTION
Spinal meningiomas account for approximately 40% of intradural extramedullary tumors; in fact, 90% are intradural, 5% are extradural, and 5% are both intradural/extradural. Of interest, 68% are located in the lateral spinal canal, whereas 17% are posterior and 15% are anterior. The typical ratio of female/male patients is 4:1.[
As these are usually slow growing tumors, some patients are diagnosed late in the clinical course with significant myelopathy. Using the McCormick Rating Scale system, this study retrospectively evaluated a prospective cohort of 51 patients with spinal meningiomas, many of whom had McCormick Grade III/IV deficit, who benefited from spinal surgical intervention.
PATIENTS AND METHODS
This retrospective study (1996–2014) involved assessment of a cohort of 51 patients undergoing spinal surgery for meningiomas. There were 40 females and 11 males, averaging 57.6 years of age. Multiple clinical and radiological (preoperative magnetic resonance) factors were assessed. In addition, patients were neurologically assessed preoperatively and postoperatively using the McCormick Functional Scale [
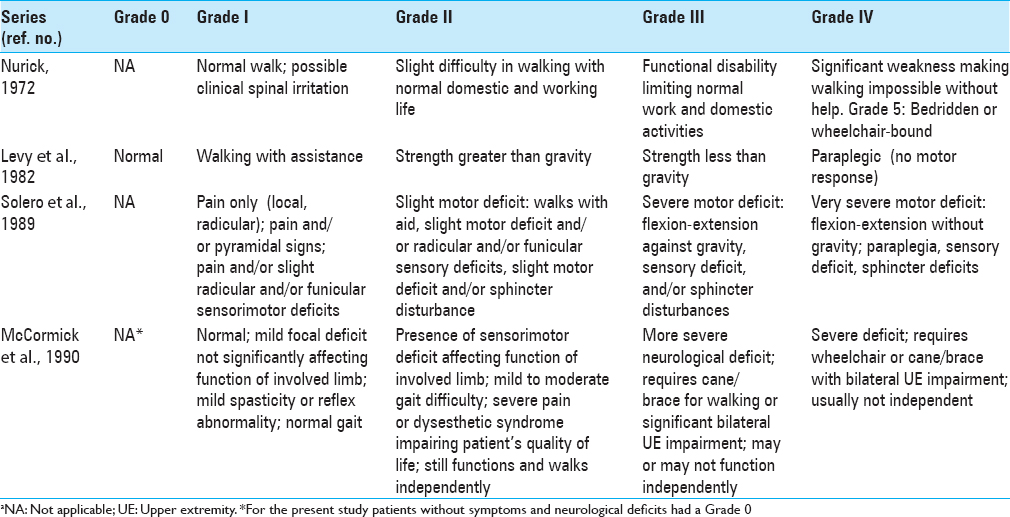
Table 1
Score systems for the evaluation of patients with spinal processesa[
Statistical analysis
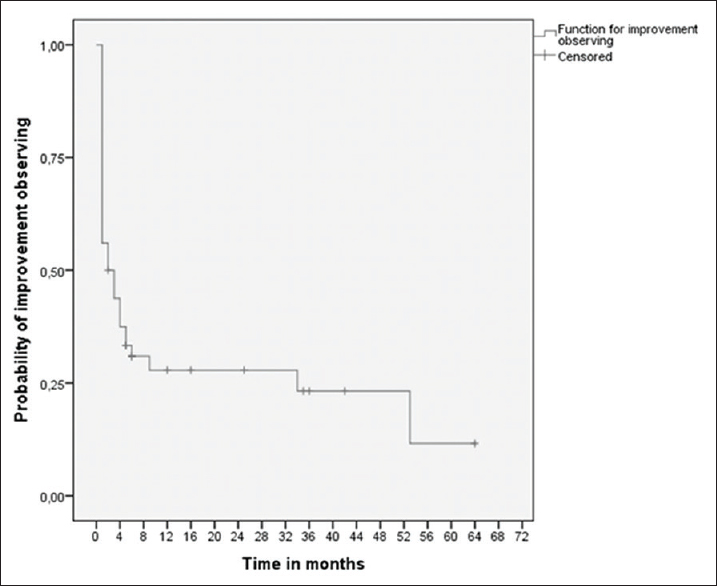
Statistical analyses were performed using the IBM-SPSS software, version 21.0. Differences between categorical variables related to the McCormick scale assessments pre and postoperatively were analyzed using the McNemar–Bowker test. Significance was assigned as a P value of less than 0.001. The observation time for the improvement of the neurological state was analyzed using the Kaplan–Meir method.
RESULTS
Clinical symptoms
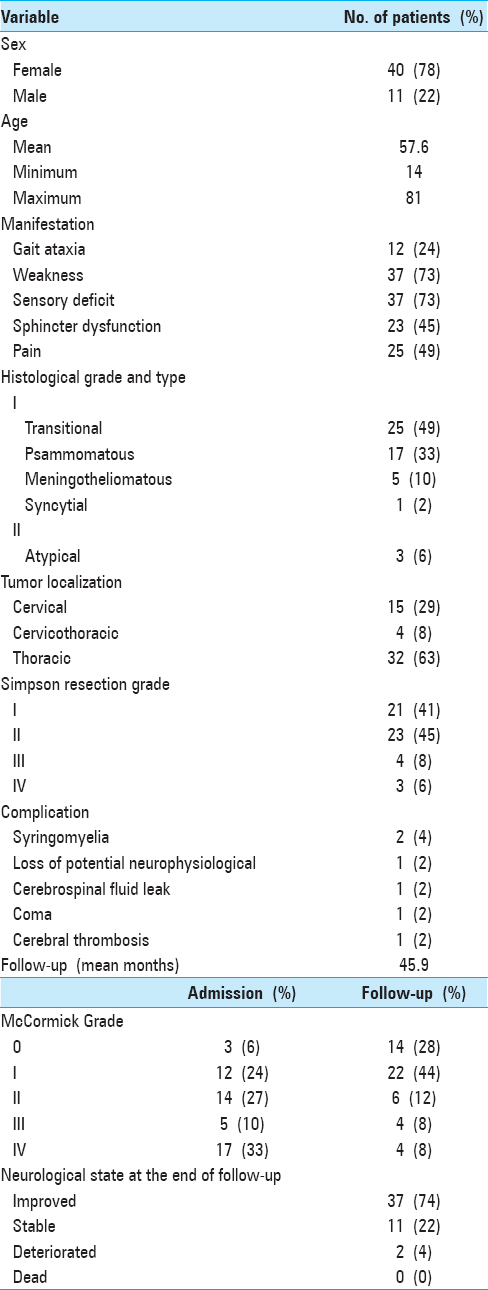
Patients were symptomatic for an average of 20 months (range 3–120 months) preoperatively; 5 were classified as grade III (McCormick Scale, 9.8%) and 17 as grade IV (McCormick Scale, 33.3%). Neurological deficits reflected significant myelopathy in many of these patients: sphincter alteration in 23 patients, ataxia 12 patients, weakness 37 patients, sensory deficit 37 patients, and pain 25 patients [
Surgical access and degree of resection
Surgery for 23 (47.1%) patients included a laminectomy, whereas 19 patients (37.3%) underwent laminotomies. Twenty-three (45.1%) patients had Simpson Grade 2 [
Table 3
Simpson Grading System for removal of meningiomas[
Functional outcome
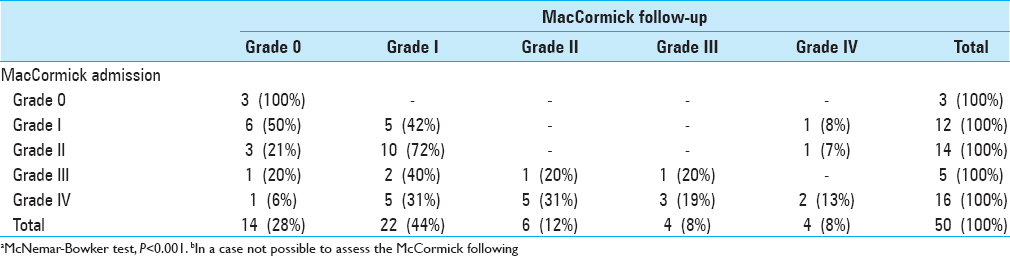
Fourteen patients considered McCormick Grade IV improved with surgery as did 4 of the 5 patients considered Grade III (P < 0.001). The mean time of the first functional improvement was 2.11 months (range, 1–9 months).
DISCUSSION
In this retrospective study of 51 patients with spinal meningiomas, many patients showed severe myelopathy (McCormick III: 5 patients; McCormick IV: 14 patients), and many improved after surgery [
In this study, our patients improved within the first 3 postoperative months (mean interval, 2.11 months) [
In a study by Riad et al.[
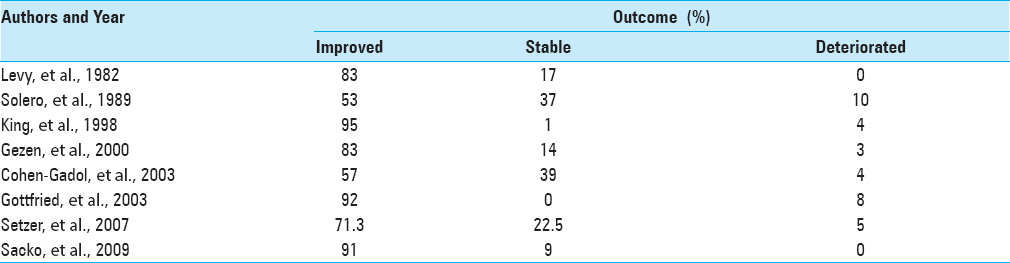
Several other studies have also shown various degrees of neurological improvement after spinal meningiomas were resected for patients with preoperative Grade II–IV status [
Table 5
Functional outcomes after surgery for spinal meningiomas[
CONCLUSION
Here, we performed a retrospective cohort study of 51 patients undergoing surgery for spinal meningiomas, many of whom were severely myelopathic in McCormick Grades III and IV. Even in those who were markedly impaired prior to surgery exhibited partial or total functional recovery following tumor resection.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgements
The study was supported by Sarah Network of Rehabilitation Hospitals, Brazil. No competing interests are reported.
References
1. Cohen-Gadol AA, Zikel OM, Koch CA, Scheithauer BW, Krauss WE. Spinal meningiomas in patients younger than 50 years of age: A 21-year experience. J Neurosurg Spine. 2003. 98: 258-63
2. Gezen F, Kahraman S, Çanakci Z, Bedük A. Review of 36 Cases of Spinal Cord Meningioma. Spine. 2000. 25: 727-31
3. Gottfried ON, Gluf W, Quinones-Hinojosa A, Kan P, Schmidt MH. Spinal meningiomas: Surgical management and outcome. Neurosurg Focus. 2003. 14: E2-
4. Levy WJ Jr, Bay J, Dohn D. Spinal cord meningioma. J Neurosurg. 1982. 57: 804-12
5. Riad H, Knafo S, Segnarbieux F. Spinal meningiomas: Surgical outcome and literature review. Neurochirurgie. 2013. 59: 30-4
6. Sacko O, Haegelen C, Mendes V, Brenner A, Sesay M, Brauge D. Spinal meningioma surgery in elderly patients with paraplegia or severe paraparesis: A multicenter study. Neurosurgery. 2009. 64: 503-10
7. Setzer M, Vatter H, Marquardt G, Seifert V, Vrionis FD. Management of spinal meningiomas: Surgical results and a review of the literature. Neurosurg Focus. 2007. 23: E14-
8. Solero CL, Fornari M, Giombini S, Lasio G, Oliveri G, Cimino C. Spinal meningiomas: Review of 174 operated cases. Neurosurgery. 1989. 25: 153-60