- Neurological Center, American British Cowdray Medical Center, Mexico City, México
- Department of Neuroanesthesiology, National Institute for Neurology and Neurosurgery “Manuel Velasco Suárez”, Mexico City, México
- Department of Neurosurgery, High Speciality Medical Unit, La Raza Hospital, Mexican Social Security Institute, Mexico City, México
Correspondence Address:
Enrique de Font-Réaulx Rojas
Department of Neuroanesthesiology, National Institute for Neurology and Neurosurgery “Manuel Velasco Suárez”, Mexico City, México
DOI:10.4103/sni.sni_58_18
Copyright: © 2018 Surgical Neurology International This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.How to cite this article: Enrique de Font-Réaulx Rojas, Edith Elizabeth Martínez Ochoa, Ramón López López, Luis Guillermo López Díaz. Infrared thermography brain mapping surveillance in vascular neurosurgery for anterior communicating artery aneurysm clipping. 20-Sep-2018;9:188
How to cite this URL: Enrique de Font-Réaulx Rojas, Edith Elizabeth Martínez Ochoa, Ramón López López, Luis Guillermo López Díaz. Infrared thermography brain mapping surveillance in vascular neurosurgery for anterior communicating artery aneurysm clipping. 20-Sep-2018;9:188. Available from: http://surgicalneurologyint.com/surgicalint-articles/9021/
Abstract
Background:Infrared thermography (IT) is a noninvasive, real-time diagnostic method that requires no contact with the patient and has a broad spectrum of potential applications in neurosurgery. It has been previously demonstrated the high sensitivity and specificity that IT has to detect brain blood flow changes.
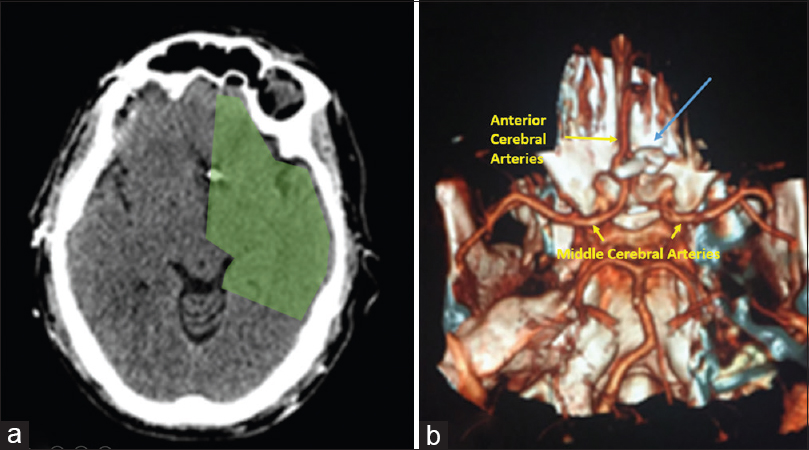
Case Description:The case is based on a 64-year-old diabetic and hypertensive male, to whom an anterior communicating artery (ACoA) incidental aneurysm was discovered. We performed the basal infrared thermography mapping (ITM) and immediately after the transitory clip placement in both A1 segments of the anterior cerebral artery (A1-ACA), we performed a second ITM of the exposed brain cortex. After the definitive clip placement in the neck of the ACoA aneurysm, we removed the transitory clips of both A1-ACA and performed a third ITM of the cortical surface, without finding any cortical cooling or significative temperature differences (Ϫt) compared to the basal ITM. The postoperatory computed tomography (CT) and angio-CT did not show any ischemic damage and confirmed the accurate aneurysm clipping.
Conclusions:The ITM seems to be a real-time, safe, and useful brain mapping method to identify different temperature zones and temperature dispersion gradients in the human brain cortex. More studies are needed to evaluate the potential applications of IT mapping of the human brain and its use in neurosurgery and vascular neurosurgery.
Keywords: Aneurysm clipping, infrared thermography, infrared thermography mapping, real-time brain mapping, vascular neurosurgery
INTRODUCTION
Intracranial aneurysms affect 3–5% of the adult population, with prevalence between the fourth and sixth decades of life. With the technological advances like the use of magnetic resonance imaging (MRI) and computed tomography (CT), the detection of nonruptured aneurysms has increased, allowing for early surgery or endovascular treatment.[
IT has become a new diagnostic method to assess thermal variations in tissues and blood. It is a remote method of imaging based on the detection of infrared radiation. This represents a part of the electromagnetic spectrum and its intensity is proportional to the surface temperature of the radiant object. In the past, this technique has been applied in coronary artery bypass surgery to measure the cooling effect during cardioplegia or to evaluate perfusion and permeability of grafts. Recent advances in infrared technology now make it possible to obtain images to evaluate the distribution of heat in the cerebral cortex.[
We are publishing the first anterior circulation aneurysm clipping with infrared thermography mapping (ITM) surveillance during transitory and definitive clipping in vascular neurosurgery.
CASE DESCRIPTION
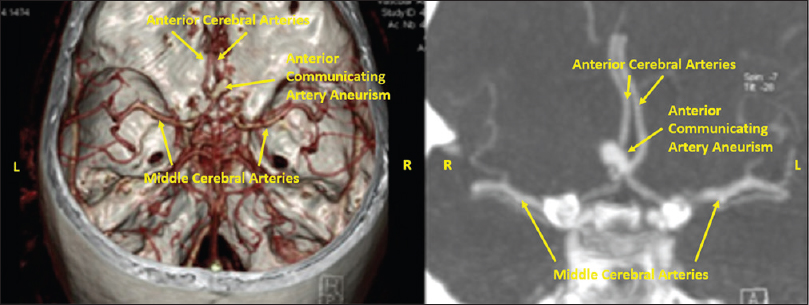
A 64-year-old diabetic and hypertensive male had a check-up that included a brain CT. An incidental, nonruptured, anterior communicating artery (ACoA) aneurysm was diagnosed [
DESCRIPTION OF THE PROCEDURE AND RESULTS
Under entropy-monitored general endovenous anesthesia, we performed a conventional frontotemporal right craniotomy. Immediately after the dura incision, we performed a basal ITM of the exposed brain surface using a handheld thermal imaging camera that combines the functions of surface temperature and real-time thermal imaging. We used a professional, precise, and efficient infrared imaging device. Our infrared thermal imager can turn a thermal image into a visible image. It quickly evaluates the different thermal gradients of the brain and it can also blend the visible and infrared images [resolution of infrared image/visible image: 3600 pixels/0.3 mega pixels; display: 2.4-inch full viewing angle high-resolution color screen; resolution: 60 × 60; resolution of visible image: 0.3 mega pixels; total pixel: 3600; FOV/shortest focal length: 20 × 20/0.5 m; thermal sensitivity: 0.5°C; measuring mode: thermopile; temperature range: −20°C to 300°C (−4°F to 572°F); measuring accuracy: ±2% or ±2°C (±4°F); wavelength range: 8–14 μm; emissivity: 0.1–1.0 (adjustable); image frequency: 6 HZ; focus mode: fixed; palette: iron red, rainbow, rainbow high contrast, gray scale (white glow), and gray scale (black glow); vision option: 5 kinds of full infrared to the full visual, mixing visible, and infrared; image storage: SD card (4G); file format: bmp; battery type: 4 × 1.5 V AA battery; authentication: CE; operating temperature: −5°C to 40°C (23°F to 104°F); relative humidity: 10–80%] [
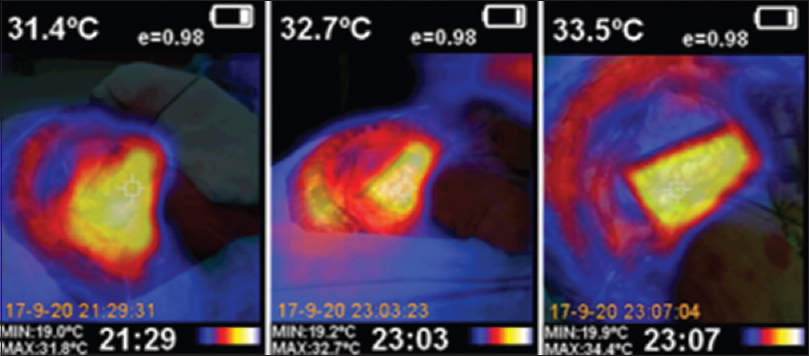
Figure 2
Image of the basal cortical metabolism measured by infrared thermography mapping (left). The temperature of the frontal lobe cortex is 31.4°C. Image of the second infrared thermography mapping during the transitory clipping of both A1-ACA (center). Image of the third infrared thermography mapping after definitive clipping of the neck of the anterior communicating artery aneurysm and removing of both transitory clips of both A1-ACA (right)
DISCUSSION
The evaluation by intraoperative image of intravascular blood flow and cerebral cortical perfusion is essential during vascular neurosurgical procedures, both to guide surgical progress and as a diagnostic method to identify changes of cerebral perfusion in real time. Different methods have been developed to achieve this objective, for instance surgical arteriography, which shows postclipping stenosis in 20% of cases.[
Thermography-based blood flow imaging has been widely investigated in cardiovascular procedures, establishing a quantitative correlation between blood flow and temperature (r = 0.96). Watson et al. observed that changes in blood temperature are related to changes in brain blood flow, whereas cortical brain temperature is determined by cerebral blood flow–metabolism coupling and the infrared image could be sufficiently sensitive to detect ischemia.[
Based on the previously described evidence, which establishes the usefulness that IT has to detect even subtle blood flow changes, we describe an anterior circulation aneurysm clipping surveillance using ITM, getting images in real time with a noninvasive method and without the use of contrast media. Using IT, we monitored the cortical temperature in critical moments during surgery, where the cerebral circulation and metabolism could be affected by the placement of transient clips and the definitive clip. We did not find a significant descent of cortical temperature in any of the three records. We consider that the ITM can be an additional method for transoperatory monitoring in both transient and final clipping of vascular structures as aneurysms. It can be used to register areas of different temperature gradients in real time, preventing secondary and permanent ischemic damage.
The use of IT in neurosurgery began in 2001 in patients with painful complex syndrome.[
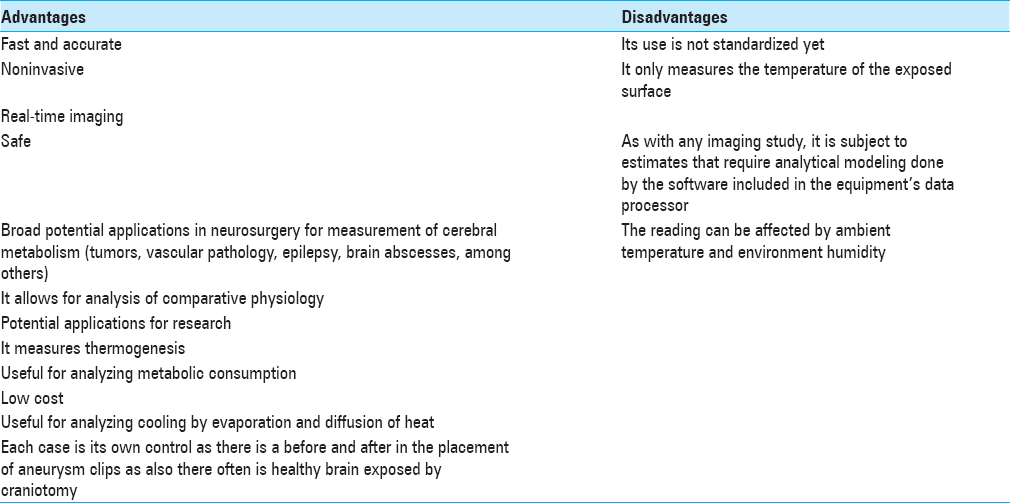
The patient we describe stayed within stable physiological hemodynamic parameters during the surgical procedure to maintain cerebral self-regulation. With ITM, we found a cortical temperature increase of 1.3°C during the transient clipping for 12 minutes of both A1-ACA and a second increase of 0.8°C after placing the final aneurysm clip and removing transient clips. Based on the high sensitivity that IT has to detect blood flow related tissue temperature changes, it allows us to assume that there were no important changes in blood flow or in the cerebral metabolism during surgical manipulation and during transient clipping of both A1-ACA that could have caused cerebral cortex cooling by hypoperfusion. Likewise, the ITM measurement after the placement of the final clip allowed us to establish an adequate cerebral perfusion by measuring an increase in cortical temperature in relation to the basal cortical temperature. We consider that ITM may be a promising adjuvant method for intraoperative monitoring in vascular neurosurgery. The main advantages and disadvantages of this initial experience are shown in
CONCLUSION
Metabolic mapping by IT is a real-time noninvasive method that requires no manipulation of the tissues. Nor does not it require the use of contrasts or filters. It is safe, efficient, and low cost; hence it can be a promising adjuvant for intraoperative monitoring in neurosurgery and vascular neurosurgery. Based on the evidence that IT is effective to detect tissue temperature changes related to blood flow, we consider that ITM could be a useful method of avoiding damage by ischemia while using temporary and definitive vascular clips. More cases are required to determine the potential use of IT in neurosurgery for metabolic mapping.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Etminan N, Rinkel GJ. Unruptured intracranial aneurysms: Development, rupture and preventive management. Nat Rev Neurol. 2016. 12: 699-713
2. Gorbach AM, Heiss J, Kufta C, Sato S, Fedio P, Kammerer WA. Intraoperative infrared functional imaging of human brain. Ann Neurol. 2003. 54: 297-309
3. Hollmach J, Hoffmann N, Schnabel C, Küchler S, Sobottka S, Kirsch M. Highly sensitive time-resolved thermography and multivariate image analysis of the cerebral cortex for intrasurgical diagnostics. Ther Diagn. 2013. 8565: 1605-7422
4. Mery F. Technology and neurosurgery. Rev Chil Neuropsiquiatr. 2010. 48: 173-4
5. Nakagawa A, Fujimura M, Arafune T, Sakuma I, Tominaga T. Intraoperative infrared brain surface blood flow monitoring during superficial temporal artery-middle cerebral artery anastomosis in patients with childhood moyamoya disease. Childs Nerv Syst. 2008. 24: 1299-305
6. Naydenov E, Minkin K, Penkov M, Nachev S, Stummer W. Infrared thermography in surgery of newly diagnosed glioblastoma multiforme: A technical case report. Case Rep Oncol. 2017. 10: 350-5
7. Neves EB, Vilaça-Alves J, Rosa C, Reis VM. Thermography in neurologic practice. Open Neurol J. 2015. 9: 24-7
8. Raabe A, Nakaji P, Beck J, Kim LJ, Hsu FP, Kamerman JD. Prospective evaluation of surgical microscope-integrated intraoperative near-infrared indocyanine green videoangiography during aneurysm surgery. J Neurosurg. 2005. 103: 982-9
9. Salles MS, da Silva SC, Salles FA, Roma LC, El Faro L, Bustos Mac Lean PA. Mapping the body surface temperature of cattle by infrared thermography. J Therm Biol. 2016. 62: 63-9
10. Watson JC, Gorbach AM, Pluta RM, Rak R, Heiss JD, Oldfield EH. Real-time detection of vascular occlusion and reperfusion of the brain during surgery by using infrared imaging. J Neurosurg. 2002. 96: 918-23