- Pars Advanced and Minimally Invasive Medical Manners Research Center, Pars Hospital, Iran University of Medical Sciences, Tehran, Iran.
DOI:10.25259/SNI_456_2019
Copyright: © 2019 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Abolfazl Rahimizadeh. Kyphosis and canal compromise due to refracturing of an L1 cemented vertebra managed with posterior surgery alone. 01-Nov-2019;10:212
How to cite this URL: Abolfazl Rahimizadeh. Kyphosis and canal compromise due to refracturing of an L1 cemented vertebra managed with posterior surgery alone. 01-Nov-2019;10:212. Available from: http://surgicalneurologyint.com/surgicalint-articles/9732/
Abstract
Background:An already cemented vertebral body rarely refractures and its occurrence may be signaled by the reappearance of pain and/or significant vertebral collapse/kyphosis resulting in canal compromise and neurological deterioration.
Case Description:An 81-year-old male originally underwent an L1 kyphoplasty for an osteoporotic compression fracture. Nine months later, he presented with the late onset of recurrent collapse of the cemented vertebral body, leading to pain, kyphosis, and canal compromise. Surgery warranted total L1 corpectomy, reconstruction of the anterior column, and a posterior fixation through a purely posterior approach (posterior vertebral column resection [pVCR]).
Conclusion:Here, we presented the safety/efficacy of utilizing a purely posterior approach (e.g., including L1 corpectomy, reconstruction of the anterior column, and posterior fusion: pVCR) in the management of a repeated fracture of a cemented L1 vertebra resulting in kyphosis and canal compromise.
Keywords: Cemented vertebra percutaneous kyphoplasty, Percutaneous vertebroplasty, Refracture
INTRODUCTION
Percutaneous vertebroplasty (PVP) and percutaneous kyphoplasty (PKP) are increasingly used to treat osteoporotic vertebral compression fractures. However, one of the late, but rare complications, is the refracturing of the cemented vertebra.[
CASE REPORT
An 81-year-old male presented with a mild paraparesis of 2 months duration. Nine months before admission, he had undergone an L1 PKP for an osteoporotic fracture.
Radiological assessment
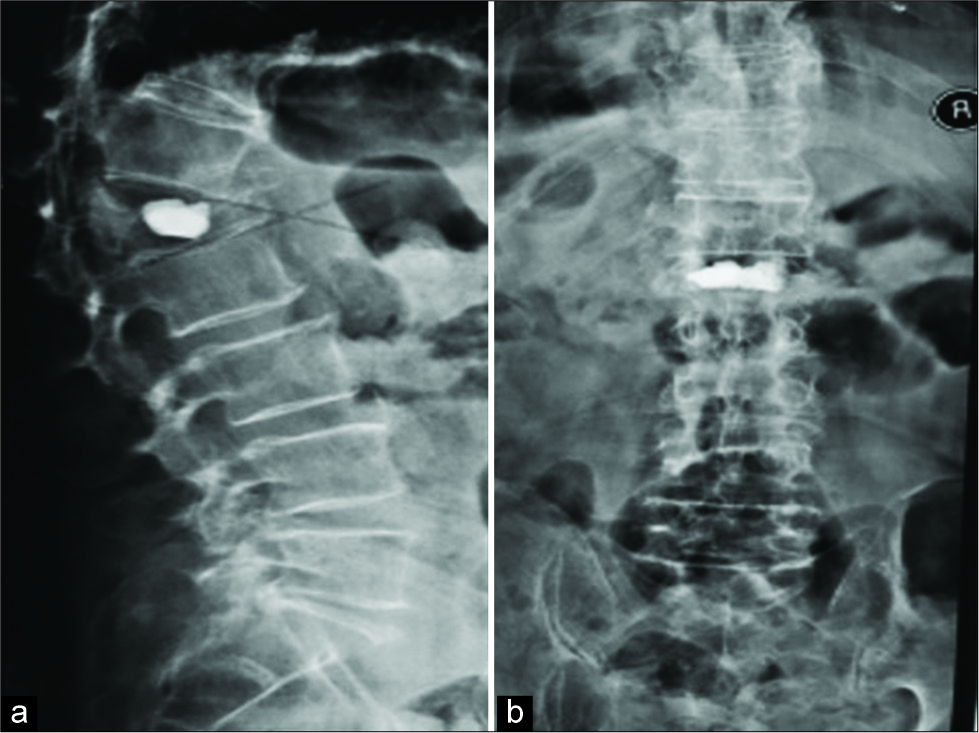
The anteroposterior (AP) thoracolumbar plain radiograph showed two symmetric kyphoplasty cement collections within the L1 vertebral body, while the lateral radiograph showed two wedge-shaped lateral compartments which were attached with a narrow medial bridge. Although the height of the anterior compartment was preserved with the PKP, the wedge-shaped posterior compartment was now significantly kyphotic and had migrated dorsally into the spinal canal resulting in significant conus/cauda equina compression [
Surgery
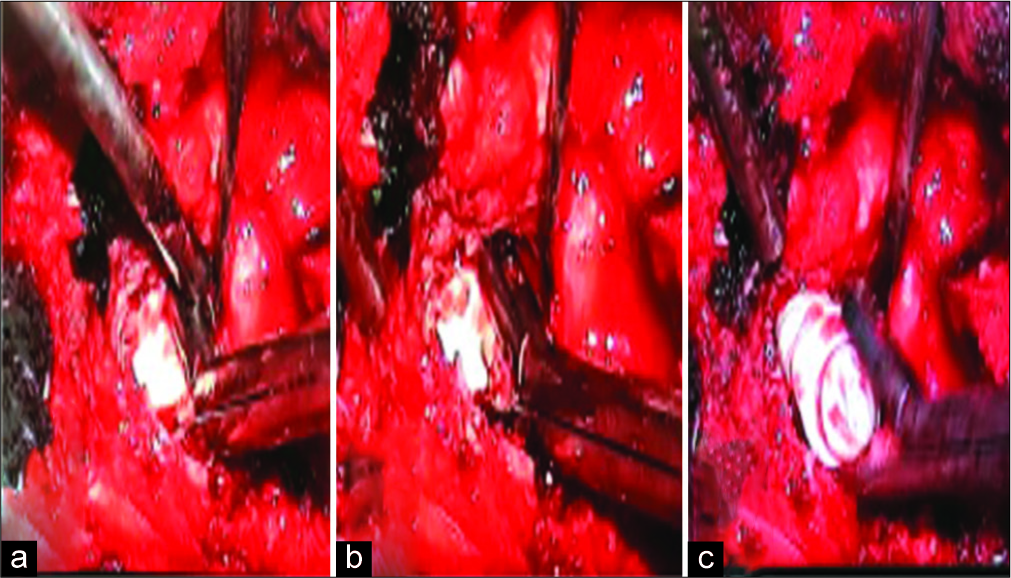
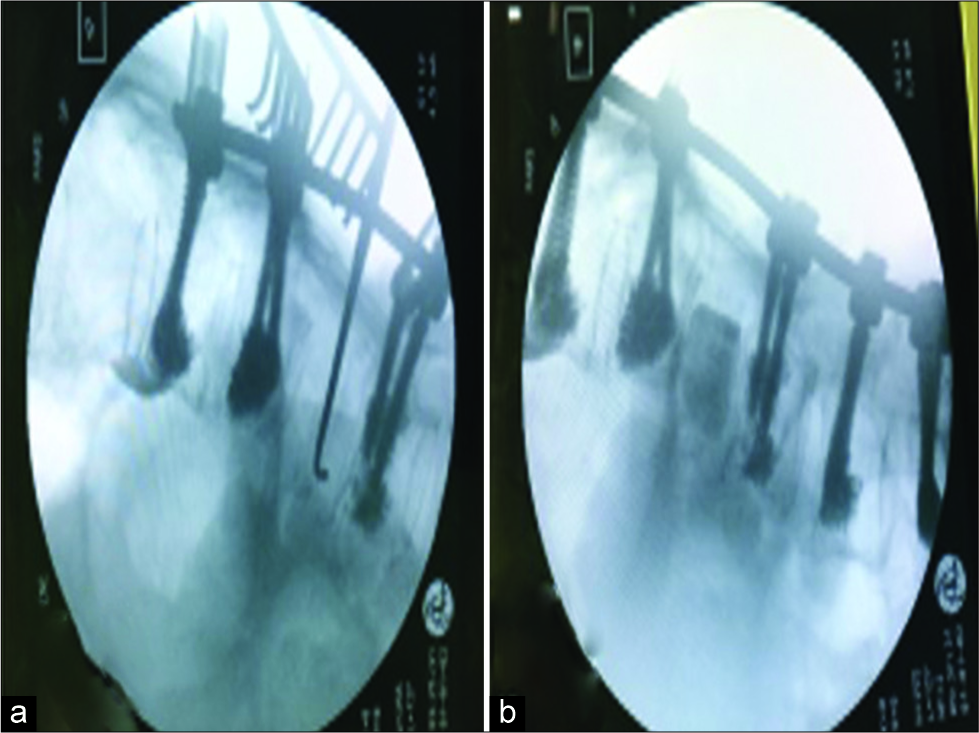
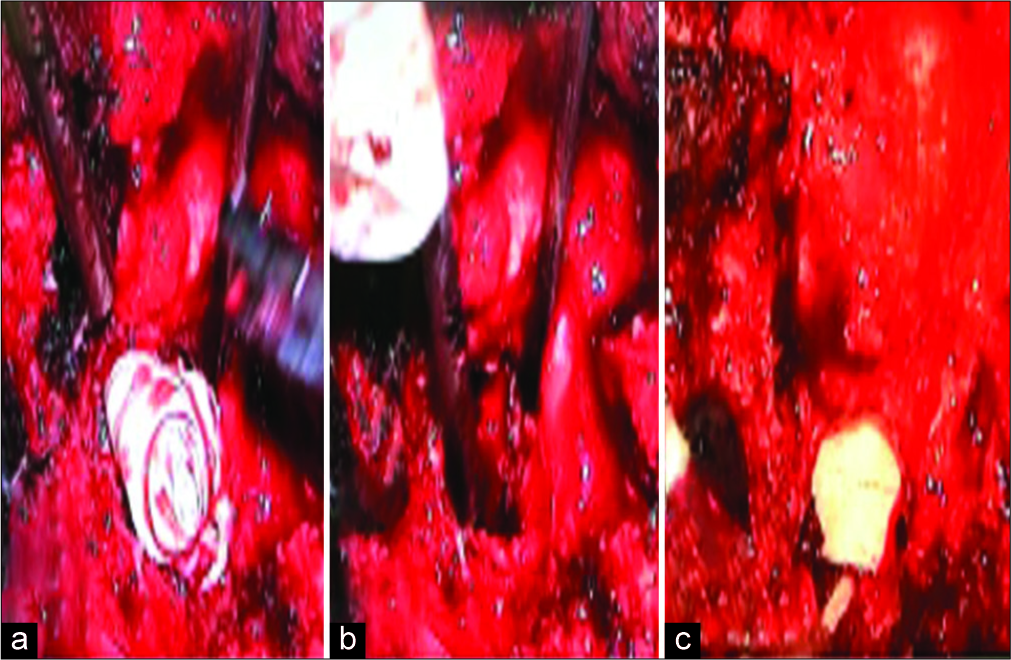
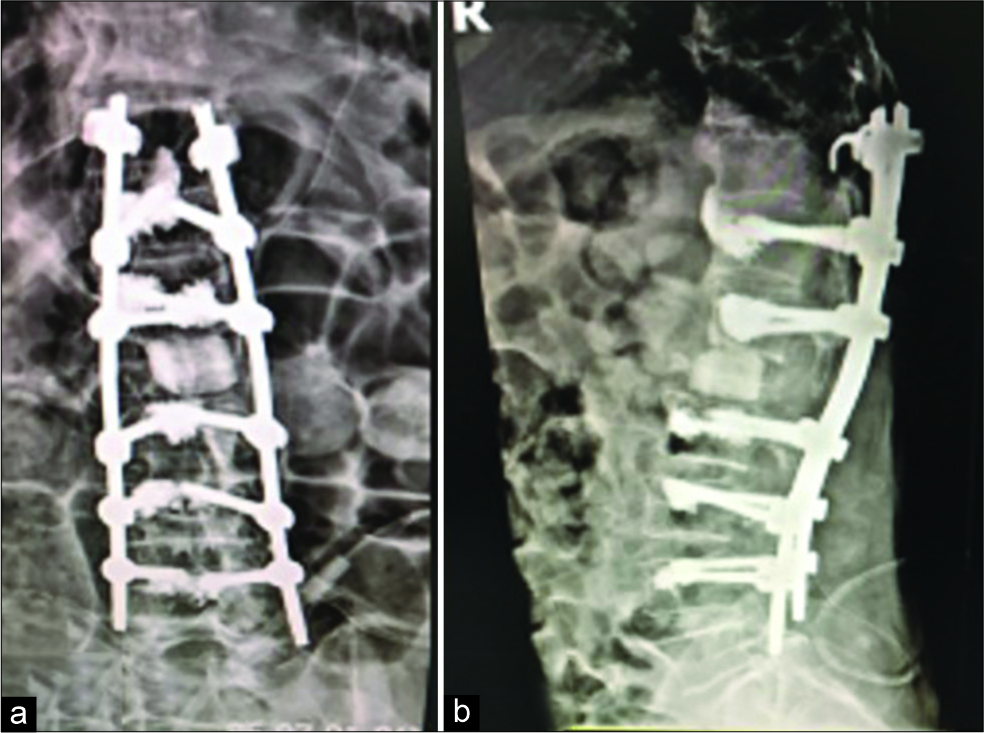
The pVCR of the L1 vertebra first required pedicle screw fixation placed above and below the fractured L1 vertebral level. Next, an L1 corpectomy was performed to reset the previously cemented L1 vertebra followed by reconstruction of the anterior column utilizing a tibial shaft allograft [
DISCUSSION
One of the late sequelae of PVP and PKP procedures is the refracturing of cemented vertebrae that can occur from 0.56% to 3.7% of PVP and from 9.7% to 12.5% of PKP cases.[
Pathogenesis and rates of PVP and PKP refractures
Several studies have demonstrated that the increased “distance between polymethylmethacrylate and the endplate” increases the rate of refracture.[
Distribution of cement
The distribution pattern for cement is classified into two types: (1) local solid lumps or (2) the trabecular/diffuse types.[
Rates of vertebral recollapse
Recollapse of a previously cemented vertebral body most often occurs within the thoracolumbar region. Infrequently, it is seen involving the low lumbar levels and only rarely within the thoracic spine itself.[
Clinical presentation of recurrent vertebral recollapse
Clinically, the refracturing of a vertebral body following initial PKP and PVP results in recurrent localized pain and/ or progressive kyphosis with canal compromise and focal neurological deficits. This can be managed with repeated vertebroplasty (e.g., using a single Jamshidi needle).[
CONCLUSION
With the appearance of localized pain after prior PVP or PKP, or the onset of kyphosis with a neurological deficit, routine AP and lateral radiographs may document recurrent vertebral body fracture that may be managed with a posterior only technique (pVCR) that offers unique 360° spinal correction.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Belkoff SM, Mathis JM, Jasper LE, Deramond H. The biomechanics of vertebroplasty. The effect of cement volume on mechanical behavior. Spine (Phila Pa 1976). 2001. 26: 1537-41
2. Chen LH, Hsieh MK, Liao JC, Lai PL, Niu CC, Fu TS. Repeated percutaneous vertebroplasty for refracture of cemented vertebrae. Arch Orthop Trauma Surg. 2011. 131: 927-33
3. Choi SS, Hur WS, Lee JJ, Oh SK, Lee MK. Repeat vertebroplasty for the subsequent refracture of procedured vertebra. Korean J Pain. 2013. 26: 94-7
4. Fattahi A, Daneshi A. Traumatic thoracic spine spondyloptosis treated with spondylectomy and fusion. Surg Neurol Int. 2018. 9: 158-
5. Feng L, Feng C, Chen J, Wu Y, Shen JM. The risk factors of vertebral refracture after kyphoplasty in patients with osteoporotic vertebral compression fractures: A study protocol for a prospective cohort study. BMC Musculoskelet Disord. 2018. 19: 195-
6. Heo DH, Chin DK, Yoon YS, Kuh SU. Recollapse of previous vertebral compression fracture after percutaneous vertebroplasty. Osteoporos Int. 2009. 20: 473-80
7. Kim DJ, Kim TW, Park KH, Chi MP, Kim JO. The proper volume and distribution of cement augmentation on percutaneous vertebroplasty. J Korean Neurosurg Soc. 2010. 48: 125-8
8. Kim YY, Rhyu KW. Recompression of vertebral body after balloon kyphoplasty for osteoporotic vertebral compression fracture. Eur Spine J. 2010. 19: 1907-12
9. Lavelle WF, Cheney R. Recurrent fracture after vertebral kyphoplasty. Spine J. 2006. 6: 488-93
10. Leslie-Mazwi T, Deen HG. Repeated fracture of a vertebral body after treatment with balloon kyphoplasty: Case illustration. J Neurosurg Spine. 2006. 4: 270-
11. Li X, Lou X, Lin X, Du J. Refracture of osteoporotic vertebral body concurrent with cement fragmentation at the previously treated vertebral level after balloon kyphoplasty: A case report. Osteoporos Int. 2014. 25: 1647-50
12. Li YX, Guo DQ, Zhang SC, Liang , Yuan K, Mo GY. Risk factor analysis for re-collapse of cemented vertebrae after percutaneous vertebroplasty (PVP) or percutaneous kyphoplasty (PKP). Int Orthop. 2018. 42: 2131-9
13. Rahimizadeh A, Hassani V, Mohsenikabir N, Rahimizadeh A, Karimi M, Asgari N. Intraoperative tension pneumothorax during posterior vertebral column resection in a child with congenital scoliosis. Surg Neurol Int. 2019. 10: 155-
14. Rahimizadeh A, Rahimizadeh A. Management of traumatic double-level spondyloptosis of the thoracic spine with posterior spondylectomy: Case report. J Neurosurg Spine. 2015. 23: 715-20
15. Summa A, Crisi G, Cerasti D, Ventura E, Menozzi R, Ormitti F. Refractures in cemented vertebrae after percutaneous vertebroplasty and pain relief after a second procedure: A retrospective analysis. Neuroradiol J. 2009. 22: 239-43
16. Yu W, Xu W, Jiang X, Liang , Jian W. Risk factors for recollapse of the augmented vertebrae after percutaneous vertebral augmentation: A systematic review and meta-analysis. World Neurosurg. 2018. 111: 119-29






Jim Ausman
Posted December 1, 2019, 7:13 am
Very nice work. Excellent result Congratulations