- Department of Neurological Surgery, Feinberg School of Medicine, Northwestern University, Chicago, IL - 60611, United States
- Faculty of Medicine, American University of Beirut, Riad El-Solh
- Department of Neurosurgery, Neuroscience Research Center, Faculty of Medical Sciences, Lebanese University, Beirut, Beyrouth - 1102 2801, Lebanon
DOI:10.25259/SNI-97-2019
Copyright: © 2019 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Fares J, Fares MY, Fares Y. Natural killer cells in the brain tumor microenvironment: Defining a new era in neuro-oncology. Surg Neurol Int 26-Mar-2019;10:43
How to cite this URL: Fares J, Fares MY, Fares Y. Natural killer cells in the brain tumor microenvironment: Defining a new era in neuro-oncology. Surg Neurol Int 26-Mar-2019;10:43. Available from: http://surgicalneurologyint.com/surgicalint-articles/9241/
INTRODUCTION
Malignant brain tumors cultivate a variety of mechanisms to escape local and systemic immunity. Current treatments are restricted to neurosurgical procedures, chemotherapy, and radiotherapy.[
Brain tumor cells are equipped with the ability of secreting numerous chemokines, cytokines, and growth factors that stimulate the infiltration of various neural cells and a range of immune cells into the tumor. Altogether, these cells create a special niche called the tumor microenvironment, which is crucial for cancer proliferation, spread, and response to treatment. The tumor microenvironment has the ability of reprogramming attacking immune cells through local release of cytokines and chemokines,[
Natural killer (NK) cells are large granular lymphocytes that play an important role in antitumor immunity. On activation, NK cells induce target cell apoptosis through contact-dependent cytotoxicity primarily mediated by perforin and granzyme B[
NK CELLS AND THE BRAIN TUMOR MICROENVIRONMENT
NK cells constitute an integral part of the intratumoral immune cell population in the brain tumor microenvironment. Multiple studies have investigated NK cell numbers and activity in patients with brain tumors. Using suboptimal antibody techniques, Stevens et al.[
The functioning of NK cells is often affected in patients with brain tumors due to the immunosuppressive factors released by tumor cells. Glioma cells, for example, highly express a special form of major histocompatibility complex Class I molecules,[
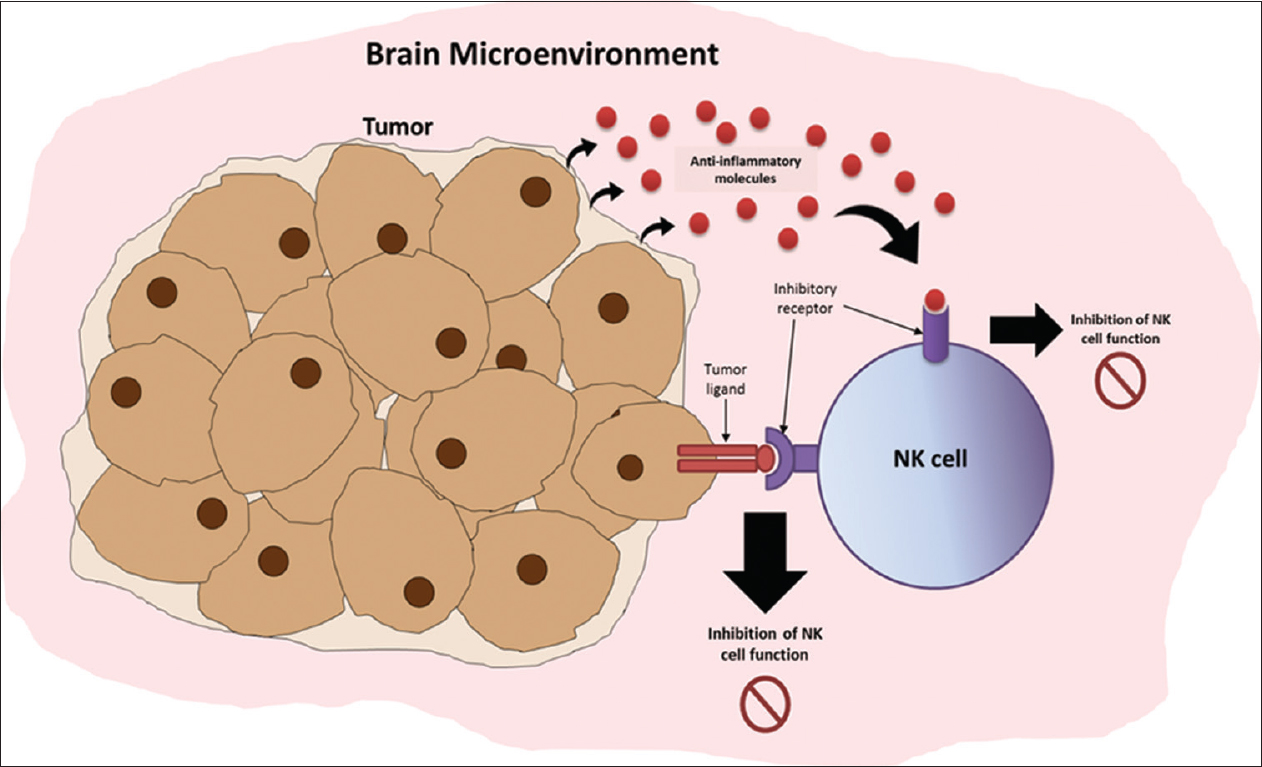
Figure 1
Immune evasion mechanisms of brain tumors against natural killer (NK) cell surveillance and killing in the brain microenvironment. Tumor cells can secrete anti-inflammatory molecules (e.g., tumor necrosis factor-β) that bind and interact with NK cell receptors and eventually downregulate the frequency and cytotoxic activity of NK cells in the brain microenvironment. Tumor cells can also express ligands that bind to the inhibitory receptors of NK cells, which further downregulate their activity.
Impaired immune function and increased anti-inflammatory molecules are common in patients with glioma. In patients with glioblastoma multiforme, Fadul et al.[
NK CELL-BASED THERAPIES IN NEURO-ONCOLOGY
Although studies show that NK cells account for a minority of infiltrating leukocytes in brain tumors,[
NK cells may play an important role in antitumor immune responses in patients with various brain tumors. Castriconi et al.[
In pediatric brain tumors, it has been suggested that NK cells may also be effective against medulloblastoma. A phase 1 clinical trial is currently undergoing whereby autologous expanded NK cells are injected into the brain of patients who have undergone resection of recurrent infratentorial tumors (NCT02271711). Phase 2 clinical trials are employing expanded autologous NK cells in combination with T cells to attack high-risk pediatric brain tumors (NCT01804634 and NCT02100891). It is believed that combination therapies involving NK cells might enhance the effectiveness and/or overcome brain tumor immune escape mechanisms.[
While these early phase trials are vital to realize the optimal dose, safety, and efficacy of NK cell therapies, combination tactics are likely compulsory to fully reap the benefits of adoptive cell therapy. Potentiating the immunogenicity of the brain tumor microenvironment through immunotherapy may be necessary to fully exploit the effects of NK cell therapy.[
Although NK cell-based therapy exhibits limited neurological toxicity, it can produce immune reactions, such as graft versus host syndrome.[
CONCLUSION
In general, NK cells play an important role in antitumor immunity and have been shown to be present in brain tumor settings. Initial preclinical and clinical studies based on autologous NK cell therapies against brain tumors have shown some promise. Further trials and research are needed to elucidate more the mechanisms through which tumor cells evade NK cell-mediated surveillance and attacks. Combination strategies with immune checkpoint inhibitors may be effective in antagonizing the tumor-induced immunosuppression and increasing the functionality of the NK cells in the brain tumor settings, among other cancers. Investigating pure NK cell fractions and/or stimulating endogenous NK cells could ease the development of efficient and cost-effective therapeutic approaches that exploit NK cells as anticancer agents. Achieving clinical success with NK cells will get us one step closer from removing the “terminal illness” tag associated with many brain tumors.
Disclaimer
The views and opinions expressed in this article are those of the author and do not necessarily reflect the official policy or position of the Journal or its management.
References
1. Alizadeh D, Zhang L, Brown CE, Farrukh O, Jensen MC, Badie B. Induction of anti-glioma natural killer cell response following multiple low-dose intracerebral cpG therapy. Clin Cancer Res. 2010. 16: 3399-408
2. Avril T, Vauleon E, Hamlat A, Saikali S, Etcheverry A, Delmas C. Human glioblastoma stem-like cells are more sensitive to allogeneic NK and T cell-mediated killing compared with serum-cultured glioblastoma cells. Brain Pathol. 2012. 22: 159-74
3. Baggio L, Laureano ÁM, Silla LM, Lee DA. Natural killer cell adoptive immunotherapy: Coming of age. Clin Immunol. 2017. 177: 3-11
4. Blaylock RL. Cancer microenvironment, inflammation and cancer stem cells: A hypothesis for a paradigm change and new targets in cancer control. Surg Neurol Int. 2015. 6: 92-
5. Böttcher JP, Bonavita E, Chakravarty P, Blees H, Cabeza-Cabrerizo M, Sammicheli S. NK cells stimulate recruitment of cDC1 into the tumor microenvironment promoting cancer immune control. Cell. 2018. 172: 1022-37.e17
6. Caligiuri MA. Human natural killer cells. Blood. 2008. 112: 461-9
7. Campbell KS, Hasegawa J. Natural killer cell biology: An update and future directions. J Allergy Clin Immunol. 2013. 132: 536-44
8. Castriconi R, Daga A, Dondero A, Zona G, Poliani PL, Melotti A. NK cells recognize and kill human glioblastoma cells with stem cell-like properties. J Immunol. 2009. 182: 3530-9
9. Cho D, Campana D. Expansion and activation of natural killer cells for cancer immunotherapy. Korean J Lab Med. 2009. 29: 89-96
10. Choi I, Yoon SR, Park SY, Kim H, Jung SJ, Jang YJ. Donor-derived natural killer cells infused after human leukocyte antigen-haploidentical hematopoietic cell transplantation: A dose-escalation study. Biol Blood Marrow Transplant. 2014. 20: 696-704
11. Domingues PH, Teodósio C, Ortiz J, Sousa P, Otero A, Maillo A. Immunophenotypic identification and characterization of tumor cells and infiltrating cell populations in meningiomas. Am J Pathol. 2012. 181: 1749-61
12. Dunn GP, Dunn IF, Curry WT. Focus on TILs: Prognostic significance of tumor infiltrating lymphocytes in human glioma. Cancer Immun. 2007. 7: 12-
13. Fadul CE, Fisher JL, Gui J, Hampton TH, Côté AL, Ernstoff MS. Immune modulation effects of concomitant temozolomide and radiation therapy on peripheral blood mononuclear cells in patients with glioblastoma multiforme. Neuro Oncol. 2011. 13: 393-400
14. Fares J, Fares MY, Fares Y. Immune checkpoint inhibitors: Advances and impact in neuro-oncology. Surg Neurol Int. 2019. 10: 9-
15. Fares J, Kanojia D, Cordero A, Rashidi A, Miska J, Schwartz CW. Current state of clinical trials in breast cancer brain metastases. Neurooncol Pract. 2019. p.
16. Friese MA, Wischhusen J, Wick W, Weiler M, Eisele G, Steinle A. RNA interference targeting transforming growth factor-beta enhances NKG2D-mediated antiglioma immune response, inhibits glioma cell migration and invasiveness, and abrogates tumorigenicity in vivo. Cancer Res. 2004. 64: 7596-603
17. Gieryng A, Pszczolkowska D, Walentynowicz KA, Rajan WD, Kaminska B. Immune microenvironment of gliomas. Lab Invest. 2017. 97: 498-518
18. Godard S, Getz G, Delorenzi M, Farmer P, Kobayashi H, Desbaillets I. Classification of human astrocytic gliomas on the basis of gene expression: A correlated group of genes with angiogenic activity emerges as a strong predictor of subtypes. Cancer Res. 2003. 63: 6613-25
19. Holtan SG, Pasquini M, Weisdorf DJ. Acute graft-versus-host disease: A bench-to-bedside update. Blood. 2014. 124: 363-73
20. Hsu J, Hodgins JJ, Marathe M, Nicolai CJ, Bourgeois-Daigneault MC, Trevino TN. Contribution of NK cells to immunotherapy mediated by PD-1/PD-L1 blockade. J Clin Invest. 2018. 128: 4654-68
21. Ishikawa E, Tsuboi K, Saijo K, Harada H, Takano S, Nose T. Autologous natural killer cell therapy for human recurrent malignant glioma. Anticancer Res. 2004. 24: 1861-71
22. Jachimowicz RD, Fracasso G, Yazaki PJ, Power BE, Borchmann P, Engert A. Induction of in vitro and in vivo NK cell cytotoxicity using high-avidity immunoligands targeting prostate-specific membrane antigen in prostate carcinoma. Mol Cancer Ther. 2011. 10: 1036-45
23. Kmiecik J, Poli A, Brons NH, Waha A, Eide GE, Enger PØ. Elevated CD3+and CD8+tumor-infiltrating immune cells correlate with prolonged survival in glioblastoma patients despite integrated immunosuppressive mechanisms in the tumor microenvironment and at the systemic level. J Neuroimmunol. 2013. 264: 71-83
24. Kmiecik J, Zimmer J, Chekenya M. Natural killer cells in intracranial neoplasms: Presence and therapeutic efficacy against brain tumours. J Neurooncol. 2014. 116: 1-9
25. Luetke-Eversloh M, Killig M, Romagnani C. Signatures of human NK cell development and terminal differentiation. Front Immunol. 2013. 4: 499-
26. Mittelbronn M, Simon P, Löffler C, Capper D, Bunz B, Harter P. Elevated HLA-E levels in human glioblastomas but not in grade I to III astrocytomas correlate with infiltrating CD8+cells. J Neuroimmunol. 2007. 189: 50-8
27. Moretta A, Locatelli F, Moretta L. Human NK cells: From HLA class I-specific killer ig-like receptors to the therapy of acute leukemias. Immunol Rev. 2008. 224: 58-69
28. Ogbomo H, Cinatl J, Mody CH, Forsyth PA. Immunotherapy in gliomas: Limitations and potential of natural killer (NK) cell therapy. Trends Mol Med. 2011. 17: 433-41
29. Perng P, Lim M. Immunosuppressive mechanisms of malignant gliomas: Parallels at non-CNS sites. Front Oncol. 2015. 5: 153-
30. Poli A, Wang J, Domingues O, Planagumà J, Yan T, Rygh CB. Targeting glioblastoma with NK cells and mAb against NG2/CSPG4 prolongs animal survival. Oncotarget. 2013. 4: 1527-46
31. Shirahata M, Iwao-Koizumi K, Saito S, Ueno N, Oda M, Hashimoto N. Gene expression-based molecular diagnostic system for malignant gliomas is superior to histological diagnosis. Clin Cancer Res. 2007. 13: 7341-56
32. Sonabend AM, Rolle CE, Lesniak MS. The role of regulatory T cells in malignant glioma. Anticancer Res. 2008. 28: 1143-50
33. Stevens A, Klöter I, Roggendorf W. Inflammatory infiltrates and natural killer cell presence in human brain tumors. Cancer. 1988. 61: 738-43
34. Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ. Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med. 2005. 352: 987-96
35. Vauléon E, Tony A, Hamlat A, Etcheverry A, Chiforeanu DC, Menei P. Immune genes are associated with human glioblastoma pathology and patient survival. BMC Med Genomics. 2012. 5: 41-
36. Vivier E, Ugolini S. Natural killer cells: From basic research to treatments. Front Immunol. 2011. 2: 18-
37. Yang I, Han SJ, Kaur G, Crane C, Parsa AT. The role of microglia in central nervous system immunity and glioma immunology. J Clin Neurosci. 2010. 17: 6-10
38. Yang I, Han SJ, Sughrue ME, Tihan T, Parsa AT. Immune cell infiltrate differences in pilocytic astrocytoma and glioblastoma: Evidence of distinct immunological microenvironments that reflect tumor biology. J Neurosurg. 2011. 115: 505-11