- Perelman School of Medicine, University of Pennsylvania, Philadelphia, Pennsylvania, USA
- Department of Neurosurgery, Hospital of the University of Pennsylvania, Philadelphia, Pennsylvania, USA
Correspondence Address:
Jayesh P. Thawani
Department of Neurosurgery, Hospital of the University of Pennsylvania, Philadelphia, Pennsylvania, USA
DOI:10.4103/2152-7806.194059
Copyright: © 2016 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Michael Randazzo, Jared M. Pisapia, Nickpreet Singh, Jayesh P. Thawani. 3D printing in neurosurgery: A systematic review. 14-Nov-2016;7:
How to cite this URL: Michael Randazzo, Jared M. Pisapia, Nickpreet Singh, Jayesh P. Thawani. 3D printing in neurosurgery: A systematic review. 14-Nov-2016;7:. Available from: http://surgicalneurologyint.com/surgicalint_articles/3d-printing-neurosurgery-systematic-review/
Abstract
Background:The recent expansion of three-dimensional (3D) printing technology into the field of neurosurgery has prompted a widespread investigation of its utility. In this article, we review the current body of literature describing rapid prototyping techniques with applications to the practice of neurosurgery.
Methods:An extensive and systematic search of the Compendex, Scopus, and PubMed medical databases was conducted using keywords relating to 3D printing and neurosurgery. Results were manually screened for relevance to applications within the field.
Results:Of the search results, 36 articles were identified and included in this review. The articles spanned the various subspecialties of the field including cerebrovascular, neuro-oncologic, spinal, functional, and endoscopic neurosurgery.
Conclusions:We conclude that 3D printing techniques are practical and anatomically accurate methods of producing patient-specific models for surgical planning, simulation and training, tissue-engineered implants, and secondary devices. Expansion of this technology may, therefore, contribute to advancing the neurosurgical field from several standpoints.
Keywords: Additive manufacturing, surgical planning, surgical simulation, three-dimensional printing
INTRODUCTION
Three-dimensional (3D) printing has revolutionized the practice of rapid prototyping since its initial emergence in the 1980s. This technique has enabled the fabrication of physical, 3D models from computer-aided designs through additive manufacturing, in which successive layers of material are deposited onto underlying layers to construct 3D objects.[
The field of neurosurgery, in particular, has experienced substantial progress as a result of the usage of 3D printing. Because most of the surgical procedures and corresponding pathology that neurosurgeons encounter involve intricate, minute anatomical structures that cannot be outwardly observed, neuroimaging has become an integral component of clinical practice.[
This technology can also serve as a tool for prototyping and production of innovative surgical devices similar to its utility in the manufacturing industry. This application may enable surgeons and researchers to create instruments and implants that correspond to individual patient anatomy for a personalized approach to treatment. Because of recent advancements, biological materials can additionally be utilized as a printing medium to construct engineered, inert scaffolds that can be populated with patient cells for the purpose of transplantation.
Studies involving the incorporation of 3D printing in neurosurgery have focused upon three main areas, i.e., the creation of patient-specific anatomical models for surgical planning, training, and education, the design of neurosurgical devices for assessment and treatment of neurosurgical diseases, and the development of biological tissue-engineered implants. In this article, we will review these studies within each subspecialty area within neurosurgery to assess the progress of the field.
MATERIALS AND METHODS
A systematic review of the published literature was performed to assess the current use of 3D printing in the field of neurosurgery. Three medical databases (Compendex, Scopus, PubMed) were searched using keywords for relevant literature between database inception to December 2015. Inclusion criteria included articles referencing both “three dimensional printing” or “additive manufacturing” and “neurosurgery” in addition to common variations of those terms. Results were then manually filtered according to more specific criteria; only human studies related to the brain or spine were considered and no studies concerning craniofacial reconstruction were included. Only studies published in English were included.
RESULTS
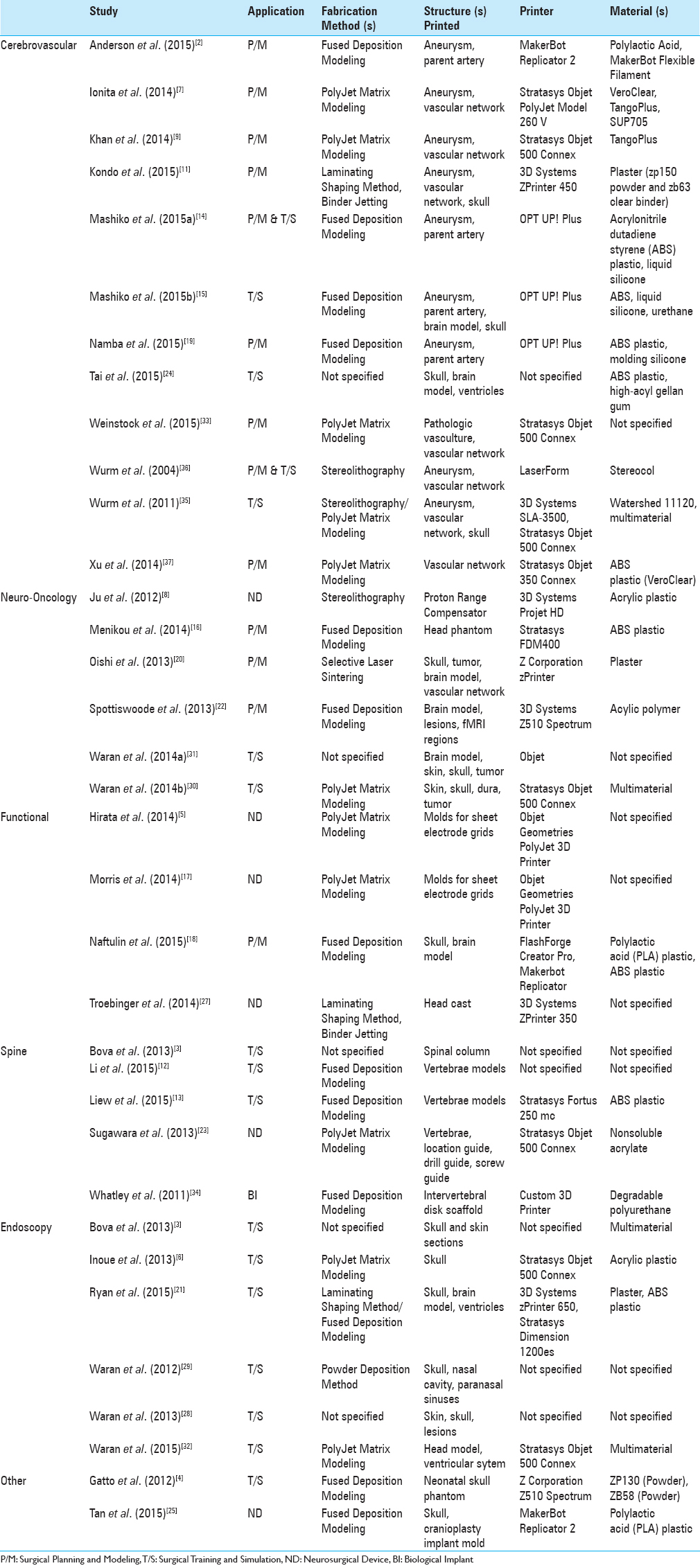
In total, the described search terms yielded 201 articles from the Compendex database, 288 articles from Scopus, and 265 articles from PubMed. Results were manually reviewed for clinical applications of 3D printing in the field of neurosurgery, and a subset of 36 articles was identified that fulfilled the inclusion criteria. Of the selected articles, 12 were related to cerebrovascular applications, 6 were related to neuro-oncology, 4 were related to functional neurosurgery, 5 were related to spine surgery, 6 were related to catheter and endoscopic applications, 2 were review articles, and 2 were related to other subspecialties of neurosurgery. One article discussed both spinal and endoscopic applications.
Cerebrovascular
Surgical planning and modeling
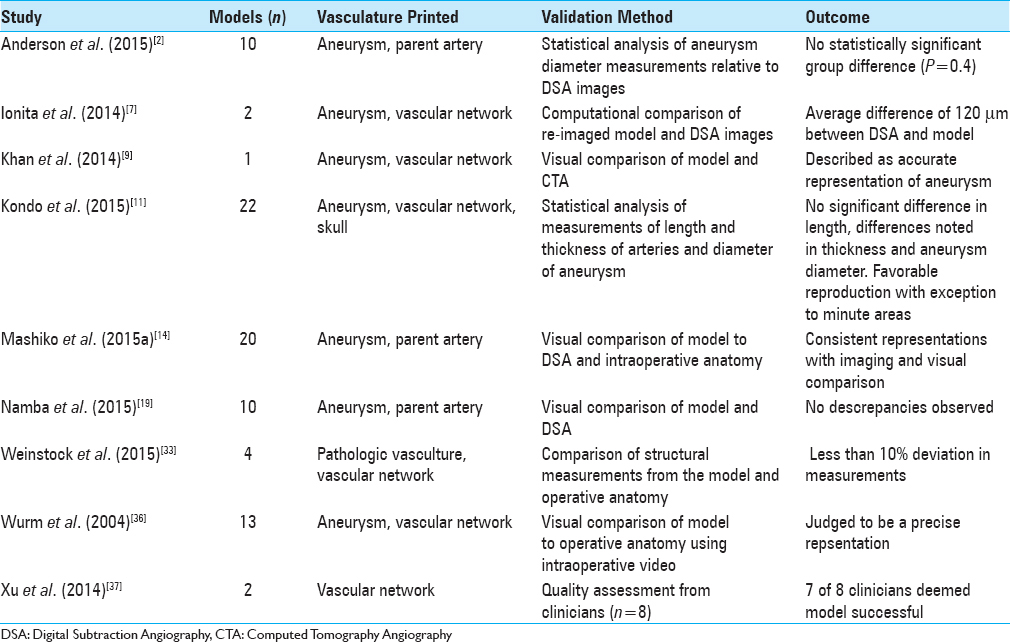
Cerebral aneurysm surgery requires a thorough understanding of the intricate 3D structure of individual aneurysms in addition to precise knowledge about associated parent vessels and surrounding anatomic structures. Importantly, diagnostic imaging has evolved in past decades from 2D angiography that force surgeons to mentally construct complicated vasculature to 3D computed tomographic angiography (3D-CTA) and digital subtraction angiography (DSA) that provide computationally reconstructed 3D visualizations.[
Figure 1
(a) Arteriovenous malformation. Using stereolithography (.STL) files created from DICOM images, the authors have generated models of a patient's vascular malformation. Using specialized software, arterial and venous phases can be segmented within the model. (b, c): Low-grade glioma and white matter tracts. Using diffusion tractography data, a patient's white matter anatomy (corpus callosum, arcute fasciculus, corticospinal tract) and tumor were similarly generated. In the composite model (c), a scaffold has been printed to support the structure during prototyping. Using an alkaline solution, the scaffold is dissolved
Numerous studies have demonstrated that complex vasculature obtained from patient scans can be printed using this technology and have additionally assessed the accuracy of the resulting models.[
Using these anatomically accurate models, surgical planning can be potentially improved to produce better patient outcomes. In two cases of pediatric arteriovenous malformations, intraoperative time was reduced by 12% compared to matched control cases, suggesting that printed models may facilitate planning.[
Surgical training and simulation
Surgical education has undergone a recent paradigm shift toward simulation-based training as opposed to the traditional experience-based training program. This change reflects the need for a safe teaching environment separated from the risk-inherent operating room, thus enabling teaching faculty to focus on training during simulations and patient care during operations. Other factors have also contributed to the shift including instituted training restrictions that have limited patient interactions, which are essential for procedural learning. The capabilities of 3D printing are well suited for the development of these physical simulators, which is evident from the literature.
One field where learning has generally been constrained to the operating room is aneurysm clipping. With the increase in the treatment of aneurysms through coil embolization and the lack of realistic cadaveric tissue, simulation-based training has become a pertinent training strategy. Mashiko et al. created hollow elastic replicas of various aneurysms within their vascular networks from a printed model and provided trainees with the opportunity to gain experience determining the clipping direction, selecting the appropriate clip, and understanding the shape of the aneurysm.[
Neuro-oncology
Surgical planning and modeling
Current surgical planning for the resection of brain tumors involves using MRI technology to differentiate between tumor and surrounding brain tissue. Nonetheless, even when this distinction is clear, it can be difficult for surgeons to appreciate the relationships between adjacent anatomical landmarks during the procedure. 3D printing technology has enabled MRI data to be translated into patient-specific models depicting the associations between tumor, skull, vasculature, and surrounding nonpathologic brain tissue [
Printed head models have also had a role in the planning and development of novel treatments for brain tumors. Phantoms that replicate the properties of the skull and cerebral tissue were produced to evaluate the potential for MRI-guided focused ultrasound to be used in the noninvasive thermocoagulation of brain tumors.[
Surgical training and simulation
Similar to the motives in the field of cerebrovascular surgery, surgical training for the excision of brain tumors has experienced the inclusion of simulation-based training methods. Critically, the use of 3D printers has lead to the development of simulators created from a multitude of materials with varying consistencies and densities.[
Neurosurgical devices
Apart from producing anatomical models for surgical planning or simulation, 3D printing has also been applied to the development of functional, patient-specific devices. One such application for brain tumor treatment has been the creation of a proton range compensator, which provides a conformal dose distribution during proton therapy to protect organs near the targeted tumor tissue.[
Functional
Surgical planning and modeling
Prior to the surgical monitoring and treatment of patients with medication-resistant epilepsy, an interdisciplinary team typically decides where intracranial electrodes will be implanted. However, often times, this planning does not involve defining specific intended locations due to a difficulty in visualizing possible electrode placements. To address this issue, Naftulin et al. have described a streamlined, cost-effective method for printing a patient-specific replica of the brain and skull. As a result, clinicians can place electrodes directly onto the model to plan surgical coverage.[
Neurosurgical devices
Intracranial electrode arrays used for treatment and research purposes are generally fabricated with standard electrode spacing and patterning. Therefore, patients receive the same electrode grids regardless of their gyral and sulcal patterns and intended recording area. 3D printing technology has enabled researchers to create printed molds from which personalized silicone sheets with embedded electrodes can be produced.[
Rapid prototyping with additive manufacturing has also proven to be a valuable tool in noninvasive forms of recording brain activity, as in magnetoencephalography (MEG). To maximize the signal to noise (SNR) ratio and minimize the error introduced as a result of varying head positions within the MEG scanner, a printed patient-specific head cast was developed to conform to both the patient's head and the inside of the helmet.[
Spine
Surgical training and simulation
Identification and understanding of anatomy is a fundamental component to learning about the surgical treatment of spine fractures. Neuroimaging techniques, such as CT and MRI, have substantially advanced the capabilities to recognize these fractures, however, they can still be challenging to interpret when visualized as 2D image slices. Li et al. investigated whether printed 3D representations of such images could promote a greater understanding of pathology by medical students compared to 2D CT images and 3D virtual renderings.[
Procedural skills for spinal surgery have similarly been addressed with 3D printing technology in the form of simulation. Analogous to their ventriculostomy simulator, Bova et al. have developed a tool that utilizes a 3D spinal construct paired via surgical instruments to a virtual interface that displays corresponding patient images.[
Neurosurgical devices
Pedicle screw fixation is a common spinal procedure that has a potential risk of injury associated with the accuracy of implantation. Drill templates have been previously developed to combat this issue; however, significant deviations have still been recorded. Therefore, Sugawara et al. have designed a multistep, patient-specific screw guide that locks onto the lamina to prevent erroneous movement.[
Biological implants
The field of spinal surgery has additionally begun to explore tissue-engineered solutions using 3D printing for the treatment of intervertebral disk (IVD) degeneration. Efforts have currently focused on a method to regenerate the IVD as an alternative to spinal fusion and artificial disk replacement. This regeneration has been attempted with elastic scaffolds created from depositing successive substrate layers and seeding the scaffold with cells.[
Catheter and endoscopic applications
Surgical training and simulation
Another common and related neurosurgical procedure that has been the subject of interest for simulation development using rapid prototyping is ventriculostomy.[
Transnasal sphenoid endoscopy for pituitary tumor removal has been another important area that has pioneered the integration of 3D printing in simulation development. In associated studies, skull replicas have been created to practice and assess surgical approaches guided by endoscopy.[
DISCUSSION
Rapid prototyping 3D-printing technologies provide a practical and anatomically accurate means to produce patient-specific and disease-specific models. These models allow for surgical planning, training and simulation, tissue-engineered transplants, and devices for the assessment and treatment of neurosurgical disease. Expansion of this technology in neurosurgery will serve practitioners, trainees, and patients.
Recent publications have described a range of applications for 3D printing in the various subspecialties of neurosurgery. These fields include cerebrovascular, neuro-oncologic, spinal, functional, and endoscopic neurosurgery, and relate to the treatment of pathologic cerebral vasculature, brain tumors, spinal cord conditions, treatment-resistant neurologic disorders, and remotely located pathology, respectively. Each field has uniquely applied 3D printing to advance surgical planning, training, and treatment.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Abla AA, Lawton MT. Three-dimensional hollow intracranial aneurysm models and their potential role for teaching, simulation, and training. World Neurosurg. 2015. 83: 35-6
2. Anderson JR, Thompson WL, Alkattan AK, Diaz O, Klucznik R, Zhang YJ. Three-dimensional printing of anatomically accurate, patient specific intracranial aneurysm models. J Neurointerv Surg. 2016. 8: 517-20
3. Bova FJ, Rajon DA, Friedman WA, Murad GJ, Hoh DJ, Jacob RP. Mixed-reality simulation for neurosurgical procedures. Neurosurgery. 2013. 73: 138-45
4. Gatto M, Memoli G, Shaw A, Sadhoo N, Gelat P, Harris RA. Three-Dimensional Printing (3DP) of neonatal head phantom for ultrasound: Thermocouple embedding and simulation of bone. Med Eng Phys. 2012. 34: 929-37
5. Hirata M, Morris S, Sugata H, Matsushita K, Yanagisawa T, Kishima H. Patient-specific contour-fitting sheet electrodes for electrocorticographic brain machine interfaces. Conf Proc IEEE Eng Med Biol Soc 2014. 2014. p. 5204-7
6. Inoue D, Yoshimoto K, Uemura M, Yoshida M, Ohuchida K, Kenmotsu H. Three-dimensional high-definition neuroendoscopic surgery: A controlled comparative laboratory study with two-dimensional endoscopy and clinical application. J Neurol Surg A Cent Eur Neurosurg. 2013. 74: 357-65
7. Ionita CN, Mokin M, Varble N, Bednarek DR, Xiang J, Snyder KV. Challenges and limitations of patient-specific vascular phantom fabrication using 3D Polyjet printing. Proc SPIE Int Soc Opt Eng. 2014. 9038: 90380M-
8. Ju SG, Kim MK, Hong CS, Kim JS, Han Y, Choi DH. New technique for developing a proton range compensator with use of a 3-dimensional printer. Int J Radiat Oncol Biol Phys. 2014. 88: 453-8
9. Khan IS, Kelly PD, Singer RJ. Prototyping of cerebral vasculature physical models. Surg Neurol Int. 2014. 5: 11-
10. Klein GT, Lu Y, Wang MY. 3D Printing and Neurosurgery—Ready for Prime Time?. World Neurosurg. 2013. 80: 233-5
11. Kondo K1, Nemoto M, Masuda H, Okonogi S, Nomoto J, Harada N. Anatomical Reproducibility of a Head Model Molded by a Three-dimensional Printer. Neurol Med Chir. 2015. 55: 592-8
12. Li Z, Li Z, Xu R, Li M, Li J, Liu Y. Three-dimensional printing models improve understanding of spinal fracture—A randomized controlled study in China. Sci Rep. 2015. 5: 11570-
13. Liew Y, Beveridge E, Demetriades AK, Hughes MA. 3D printing of patient-specific anatomy: A tool to improve patient consent and enhance imaging interpretation by trainees. Br J Neurosurg. 2015. 29: 712-4
14. Mashiko T, Otani K, Kawano R, Konno T, Kaneko N, Ito Y. Development of three-dimensional hollow elastic model for cerebral aneurysm clipping simulation enabling rapid and low cost prototyping. World Neurosurg. 2015. 83: 351-61
15. Mashiko T, Konno T, Kaneko N, Watanabe E. Training in Brain Retraction Using a Self-Made Three-Dimensional Model. World Neurosurg. 2015. 84: 585-90
16. Menikou G, Dadakova T, Pavlina M, Bock M, Damianou C. MRI compatible head phantom for ultrasound surgery. Ultrasonics. 2015. 57: 144-52
17. Morris S, Hirata M, Sugata H, Goto T, Matsushita K, Yanagisawa T. Patient Specific Cortical Electrodes for Sulcal and Gyral Implantation. IEEE Trans Biomed Eng. 2014. 62: 1034-41
18. Naftulin JS, Kimchi EY, Cash SS. Streamlined, Inexpensive 3D Printing of the Brain and Skull. PLoS One. 2015. 10: e0136198-
19. Namba K, Higaki A, Kaneko N, Mashiko T, Nemoto S, Watanabe E. Microcatheter Shaping for Intracranial Aneurysm Coiling Using the 3-Dimensional Printing Rapid Prototyping Technology: Preliminary Result in the First 10 Consecutive Cases. World Neurosurg. 2015. 84: 178-86
20. Oishi M, Fukuda M, Yajima N, Yoshida K, Takahashi M, Hiraishi T. Interactive presurgical simulation applying advanced 3D imaging and modeling techniques for skull base and deep tumors. J Neurosurg. 2013. 119: 94-105
21. Ryan JR, Chen T, Nakaji P, Frakes DH, Gonzalez LF. Ventriculostomy Simulation Using Patient-specific ventricular anatomy, 3D Printing, and Hydrogel Casting. World Neurosurg. 2015. 84: 1333-9
22. Spottiswoode BS, Van Den Heever DJ, Chang Y, Engelhardt S, Du Plessis S, Nicolls F. Preoperative three-dimensional model creation of magnetic resonance brain images as a tool to assist neurosurgical planning. Stereotact Funct Neurosurg. 2013. 91: 162-9
23. Sugawara T, Higashiyama N, Kaneyama S, Takabatake M, Watanabe N, Uchida F. Multistep pedicle screw insertion procedure with patient-specific lamina fit-and-lock templates for the thoracic spine. J Neurosurg Spine. 2013. 19: 185-90
24. Tai BL, Rooney D, Stephenson F, Liao P, Sagher O, Shih AJ. Development of a 3D-printed external ventricular drain placement simulator: Technical note. J Neurosurg. 2015. 123: 1-7
25. Tan ET, Ling JM, Dinesh SK. The feasibility of producing patient-specific acrylic cranioplasty implants with a low-cost 3D printer. J Neurosurg. 2016. 124: 1531-7
26. Thawani JP, Pisapia JM, Singh N, Petrov D, Schuster JM, Hurst RW. 3D-Printed Modeling of an Arteriovenous Malformation Including Blood Flow. World Neurosurg. 2016. 90: 675-83
27. Troebinger L, López JD, Lutti A, Bradbury D, Bestmann S, Barnes G. High precision anatomy for MEG. Neuroimage. 2014. 86: 583-91
28. Waran V, Pancharatnam D, Thambinayagam HC, Raman R, Rathinam AK, Balakrishnan YK. The utilization of cranial models created using rapid prototyping techniques in the development of models for navigation training. J Neurol Surg A Cent Eur Neurosurg. 2013. 75: 12-5
29. Waran V, Menon R, Pancharatnam D, Rathinam AK, Balakrishnan YK, Tung TS. The creation and verification of cranial models using three-dimensional rapid prototyping technology in field of transnasal sphenoid endoscopy. Am J Rhinol Allergy. 2012. 26: 132-6
30. Waran V, Narayanan V, Karuppiah R, Owen SL, Aziz T. Utility of multimaterial 3D printers in creating models with pathological entities to enhance the training experience of neurosurgeons. J Neurosurg. 2014. 120: 489-92
31. Waran V, Narayanan V, Karuppiah R, Pancharatnam D, Chandran H, Raman R. Injecting Realism in Surgical Training—Initial Simulation Experience With Custom 3D Models. J Surg Educ. 2014. 71: 193-7
32. Waran V, Narayanan V, Karuppiah R, Thambynayagam HC, Muthusamy KA, Rahman ZAA. Neurosurgical Endoscopic Training via a Realistic 3-Dimensional Model With Pathology. Simul Healthc. 2015. 10: 43-8
33. Weinstock P, Prabhu SP, Flynn K, Orbach DB, Smith E. Optimizing cerebrovascular surgical and endovascular procedures in children via personalized 3D printing. Neurosurgery. 2015. 16: 1-6
34. Whatley BR, Kuo J, Shuai C, Damon BJ, Wen X. Fabrication of a biomimetic elastic intervertebral disk scaffold using additive manufacturing. Biofabrication. 2011. 3: 015004-
35. Wurm G, Lehner M, Tomancok B, Kleiser R, Nussbaumer K. Cerebrovascular biomodeling for aneurysm surgery: Simulation-based training by means of rapid prototyping technologies. Surg Innov. 2011. 18: 294-306
36. Wurm G, Tomancok B, Pogady P, Holl K, Trenkler J. Cerebrovascular stereolithographic biomodeling for aneurysm surgery. Technical note. J Neurosurg. 2004. 100: 139-45
37. Xu WH, Liu J, Li ML, Sun ZY, Chen J, Wu JH. 3D printing of intracranial artery stenosis based on the source images of magnetic resonance angiograph. Ann Transl Med. 2014. 2: 74-