- Department of Neurosurgery, Salford Royal Foundation Trust, Salford, United Kingdom.
Correspondence Address:
Mohammad Saleem Saleemi, Department of Neurosurgery, Salford Royal Foundation Trust, Salford, United Kingdom.
DOI:10.25259/SNI_151_2022
Copyright: © 2022 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Mohammad Saleem Saleemi, Ahmed Ossama Yassin Abdelwahab, Muhammad Ossama Yassin Abdelwahab, K. Joshi George. A case of a giant thoracic schwannoma. 06-May-2022;13:188
How to cite this URL: Mohammad Saleem Saleemi, Ahmed Ossama Yassin Abdelwahab, Muhammad Ossama Yassin Abdelwahab, K. Joshi George. A case of a giant thoracic schwannoma. 06-May-2022;13:188. Available from: https://surgicalneurologyint.com/surgicalint-articles/11584/
Abstract
Background: Giant solitary schwannomas are rare, benign, and typically slow-growing tumors reaching up to 20 cm in size.
Case Description: A 43-year-old male presented with shortness of breath and chest pain. The thoracic MRI showed a giant mass 15 cm in diameter filling the left chest cavity. The lesion was resected utilizing intrathoracic approach and required a multilevel approach. Vertebrectomy with instrumented fusion was performed. The pathological diagnosis was benign schwannoma without nuclear atypia. Postoperatively, the patient fully recovered without sequelae.
Conclusion: A 43-year-old male presented with a 15 cm diameter chest mass that proved to be a schwannoma that was resected without long-term sequelae.
Keywords: Ancient schwannoma, Fusion, Giant, Thoracic spine, Vertebrectomy
INTRODUCTION
Spinal schwannomas are slow-growing benign tumors.[
CASE REPORT
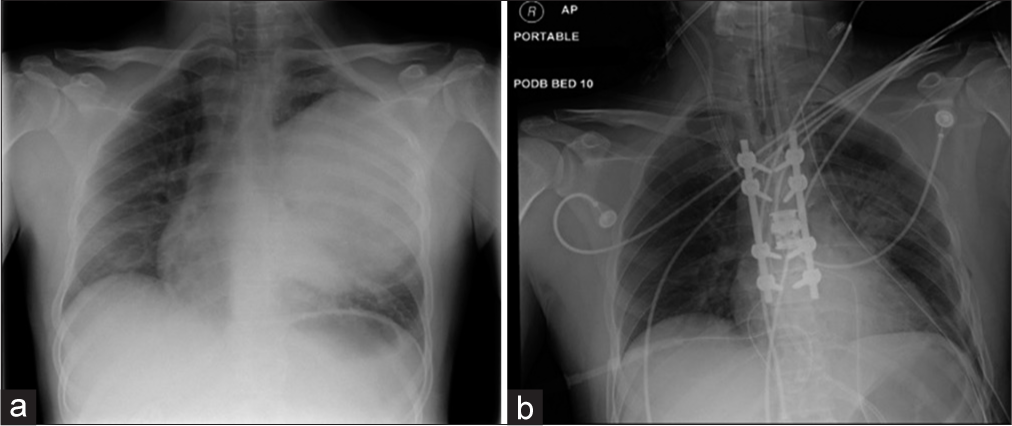
A 43-year-old male presented with shortness of breath, bilateral upper limb tingling, and chest pain. The chest x-ray [
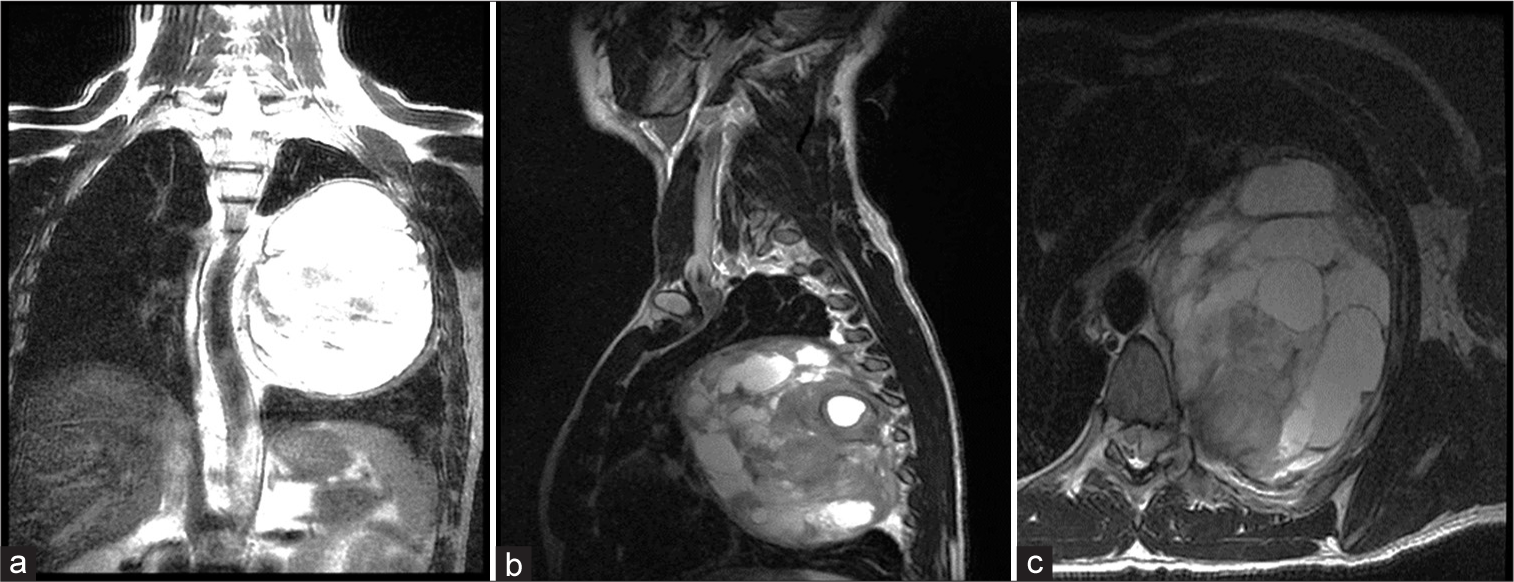
Figure 2:
Preoperative MRI a massive left-sided chest tumor which measures approximately 10 × 15 × 12 cm in diameter with solid and metacystic appearance, there is an intraspinal component of this tumor which enters the spinal canal at the T6-7 level. (a) Coronal section T2, (b) sagittal section T2, and (c) axial section T2.
DISCUSSION
Rare giant solitary schwannomas
Giant solitary schwannomas are rare benign tumors that typically involve more than 2 vertebral levels and can range from a few millimeters to more than 20 cm.[
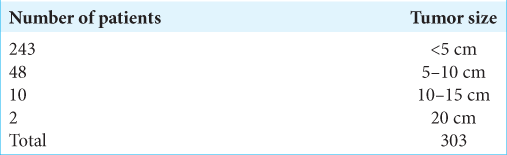
In a study of 303 benign solitary schwannomas, Das Gupta et al. found 10 patients with lesions between 10 and 15 cm in maximum diameter; only two were over 20 cm in diameter [
Intraspinal schwannoma with foraminal extension into the chest typically arises from the intercostal and sympathetic nerves, but only rarely presents as predominantly intrapulmonary masses.[
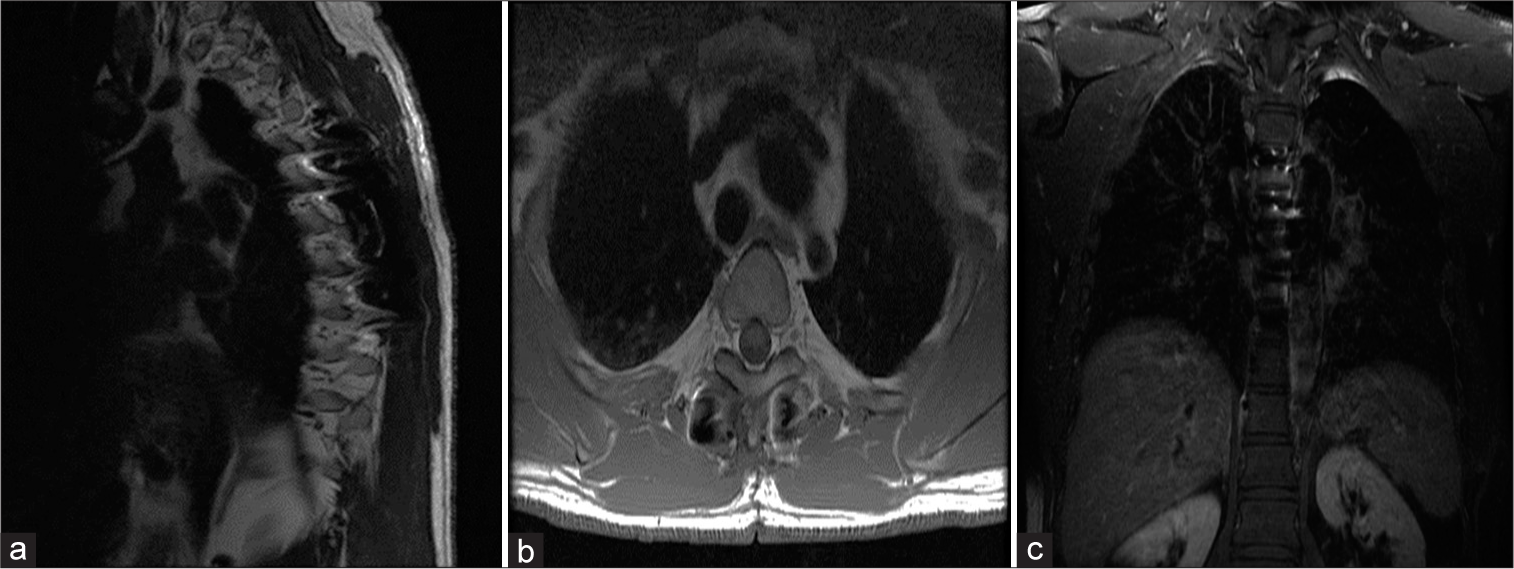
CT and MR studies of thoracic schwannomas
Studies of large/giant schwannomas have typical features on CT and MR studies [
CONCLUSION
Here, we reported a 15 cm diameter left-sided spinal T6-t7 foraminal/intrathoracic schwannoma that was totally excised utilizing a combined intraspinal/intrathoracic approach without further long-term sequelae.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Bhowmik A, Bisht S, Toe KK, George KJ. Giant posterior mediastinal schwannoma requiring a thoracoabdominal approach for excision: Case report and literature review. Surg Neurol Int. 2021. 12: 241
2. Das Gupta TK, Brasfield RD, Strong EW, Hajdu SI. Benign solitary Schwannomas (neurilemomas). Cancer. 1969. 24: 355-66
3. Gueldich M, Hentati A, Chakroun A, Abid H, Kammoun S, M’saad S. Giant cystic schwannoma of the middle mediastinum with cervical extension. Libyan J Med. 2015. 10: 27409
4. Kato M, Shiota S, Shiga K, Takagi H, Mori H, Sekiya M. Benign giant mediastinal schwannoma presenting as cardiac tamponade in a woman: A case report. J Med Case Rep. 2011. 5: 61
5. Peng X, Li Z, Zhou L, Zhao L, Wu X, Yang Y. Giant posterior pararenal schwannoma: A case report and review of literature. Mol Clin Oncol. 2018. 9: 325-8
6. Sridhar K, Ramamurthi R, Vasudevan MC, Ramamurthi B. Giant invasive spinal schwannomas: Definition and surgical management. J Neurosurg. 2001. 94: 210-5
7. Yu NH, Lee SE, Jahng TA, Chung CK. Giant invasive spinal schwannoma: Its clinical features and surgical management. Neurosurgery. 2012. 71: 58-67