- Department of Neurosurgery, Japanese Red Cross Otsu Hospital, Otsu, Japan
- Department of Neurosurgery, Hikone Chuo Hospital, Hikone, Japan
- Department of Neurosurgery, Kobe City Medical Center General Hospital, Kobe, Japan.
Correspondence Address:
Toshinari Kawasaki, Department of Neurosurgery, Japanese Red Cross Otsu Hospital, Otsu, Japan.
DOI:10.25259/SNI_254_2023
Copyright: © 2023 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Toshinari Kawasaki1, Motohiro Takayama1, Yoshinori Maki2, Kota Nakajima3, Tamaki Kobayashi1, Masaaki Saiki1, Yoshihiko Ioroi1. A case of anterior arch fracture of the atlas associated with C1 laminectomy. 14-Apr-2023;14:136
How to cite this URL: Toshinari Kawasaki1, Motohiro Takayama1, Yoshinori Maki2, Kota Nakajima3, Tamaki Kobayashi1, Masaaki Saiki1, Yoshihiko Ioroi1. A case of anterior arch fracture of the atlas associated with C1 laminectomy. 14-Apr-2023;14:136. Available from: https://surgicalneurologyint.com/surgicalint-articles/12258/
Abstract
Background: Spontaneous anterior arch fracture of the atlas after a C1 laminectomy (CIL) is an extremely rare complication.
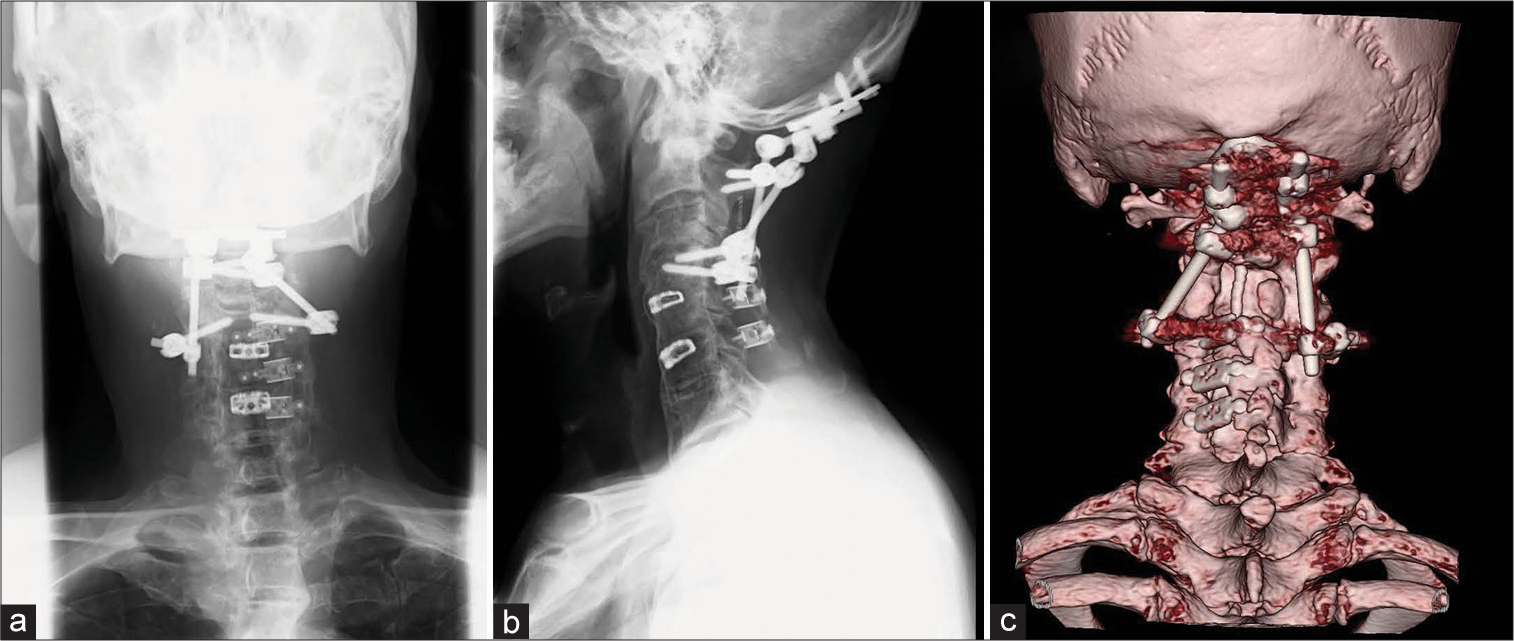
Case Description: A 72-year-old male presented with the sudden onset of neck pain. His prior history included; a CIL for atlantoaxial subluxation, shunt closure for a spinal dural arteriovenous fistula at C3, a cervical laminoplasty from C3 to C6 for stenosis, and a prior anterior C4/5 and C5/6 fusion 14 years ago. Once the computed tomography documented a right C1 anterior arch fracture, and occipital-cervical fusion was performed utilizing C2 laminar screws and C4 pedicle screws with halo-vest placement. Postoperatively, the neck pain resolved and he remained stable.
Conclusion: Neurosurgeons should be aware of the risk of anterior arch fractures following a CIL and may alternatively consider a C1 laminoplasty in the future.
Keywords: Anterior arch, Atlas, Cervical laminectomy, Fracture, Spine
INTRODUCTION
The atlas (C1) is a simple ring structure composed of an anterior and a posterior arch with two lateral masses that play a crucial role in stabilizing the craniocervical junction. Atlas fractures account for 3–13% of cervical spine injuries, most of which are attributed to traffic accidents and falls.[
CASE DESCRIPTION
A 72-year-old male presented with the sudden, spontaneous onset of neck pain. He had a history of two cervical operations; a ½ years ago, he had a C1 laminectomy (CIL) for atlantoaxial subluxation, shunt closure for a spinal dural arteriovenous fistula at the C3 level, and, a cervical laminoplasty from C3 to C6 for stenosis. Fourteen years before that, he had undergone a C4/5–C5/6 anterior cervical. An old cervical computed tomography (CT) 3 months after the operation had documented the prior surgical procedures without a C1 arch fracture [
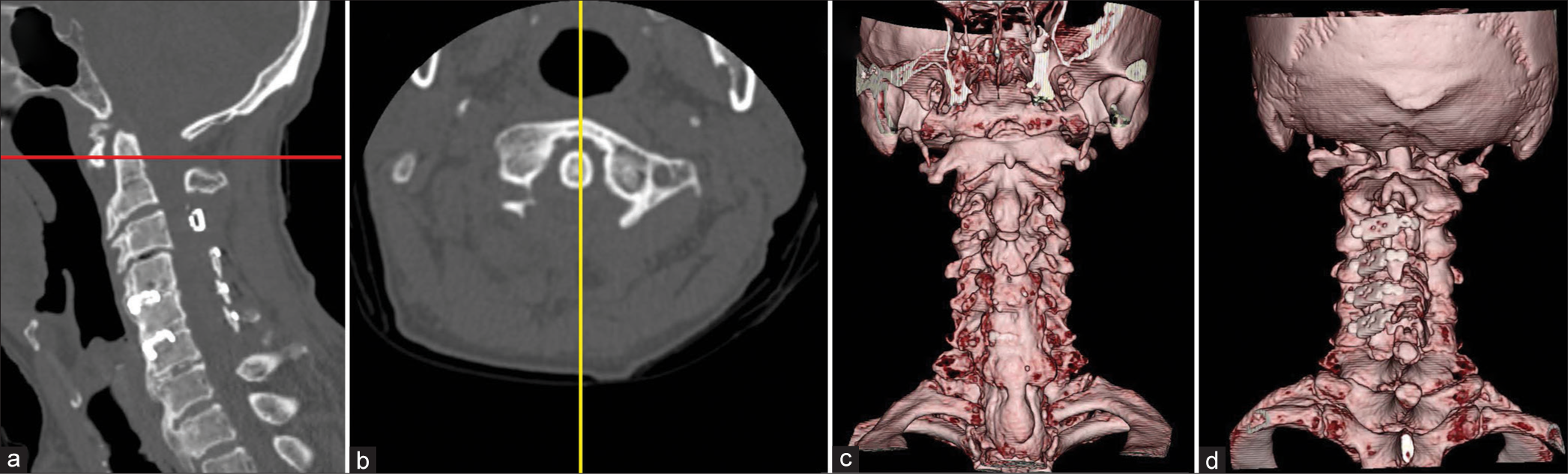
Figure 1:
Latest postoperative computed tomography (CT) of sagittal-view (a) and axial-view (b) showed C1 laminectomy, cervical laminoplasty, anterior cervical fusion, and no anterior arch fracture of C1. (b) was at the level of the red line in (a). (a) was at the level of the yellow line in (b). Anterior view (c) and posterior view (d) three-dimensional CT scans.
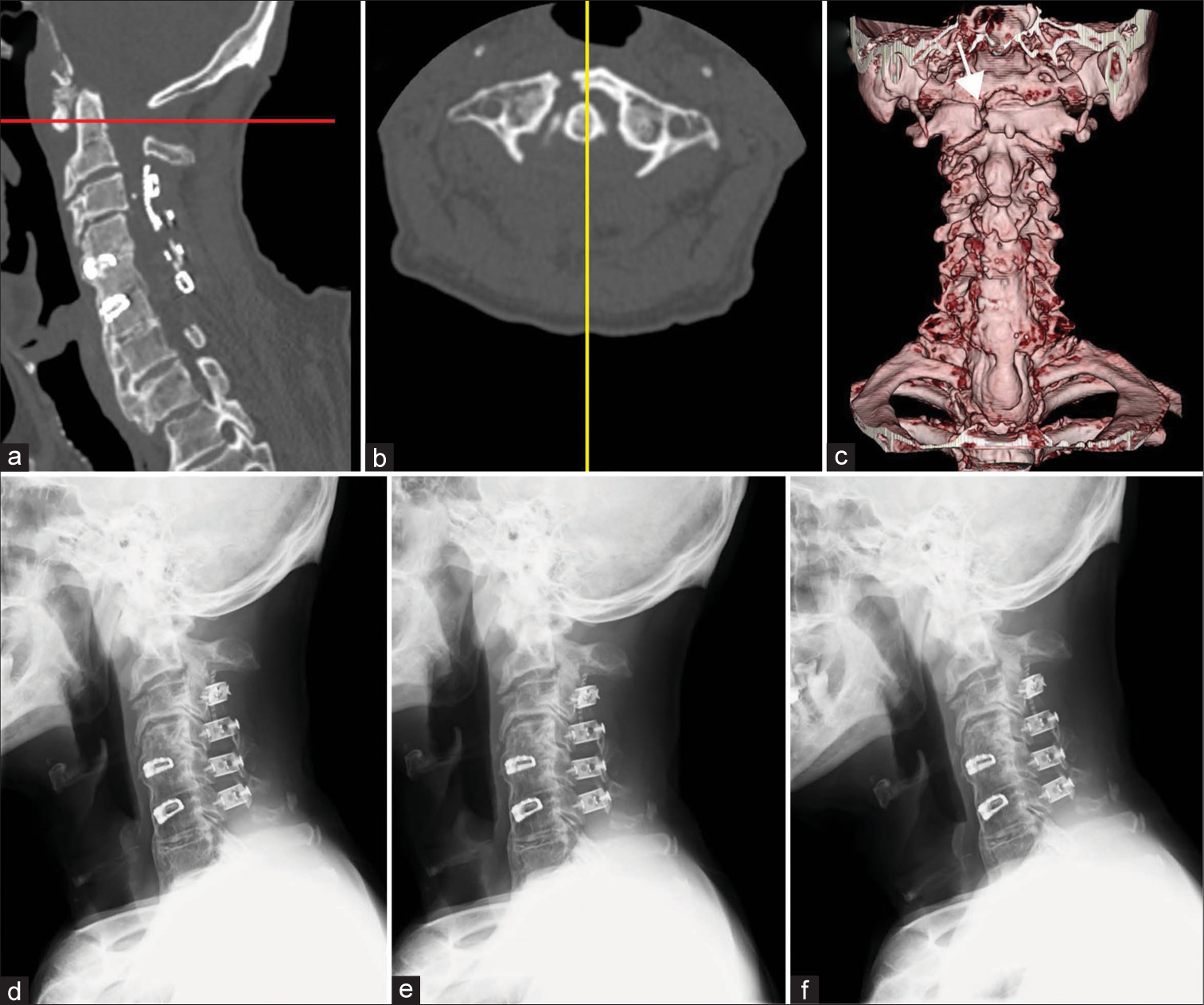
Figure 2:
Sagittal-view (a) and axial-view (b) after onset of neck pain showed right C1 anterior arch fracture. (b) was at the level of the red line in the sagittal-view image (a). (a) was at the level of the yellow line in (b). Anterior view (c) three-dimensional computed tomography scan. White arrow indicates right C1 anterior arch fracture. Cervical radiographs indicated instability between C1 and C2 (d: lateral neutral view, (e: extension view, (f: flexion view).
DISCUSSION
The mechanism of spontaneous C1 anterior arch fractures associated with C1L may be attributed to excessive, repeated axial loading forces on the C1 anterior arch caused by a lack of sufficient posterior support.[
Hypothesis: Use of C1 laminoplasty to prevent anterior C1 arch fractures
C1 laminoplasty would help prevent such anterior arch fractures following C1L. Tarukado et al. described how C1 laminoplasty performed for spinal cord compression at the C1/2 level resulted in favorable outcomes, and, therefore suggested this might be an effective alternative to CIL for patients without C1–C2 instability.[
CONCLUSION
Anterior arch fractures of the atlas after a C1L are extremely rare. Neurosurgeons should be aware of the risk of anterior arch fractures following C1L and may alternatively consider laminoplasty rather than C1L in the future.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.
References
1. Hirano Y, Mizuno J, Watanabe K, Sugawara A, Takeda M, Ogasawara K. Spontaneous C1 anterior arch fracture as a postoperative complication of foramen magnum decompression for Chiari malformation Type 1. Surg Neurol Int. 2011. 2: 138
2. Kakarla UK, Chang SW, Theodore N, Sonntag VK. Atlas fractures. Neurosurgery. 2010. 66: 60-7
3. Shimizu T, Otsuki B, Fujibayashi S, Kumamoto S, Hijikata Y, Shimizu Y. Incidence and risk factors of anterior arch fracture of the atlas following C1 laminectomy without fusion. Spine (Phila Pa 1976). 2018. 43: 667-74
4. Shimizu T, Otsuki B, Fujibayashi S, Takemoto M, Ito H, Sakamoto T. Spontaneous anterior arch fracture of the atlas following C1 laminectomy without fusion: A report of three cases and finite element analysis. J Orthop Sci. 2016. 21: 306-15
5. Tarukado K, Ikuta K, Iida K, Tono O, Doi T, Harimaya K. Radiographic and clinical results of C1 laminoplasty for the treatment of compressive myelopathy. Asian Spine J. 2020. 14: 459-65