- Departments of Neurosurgery, Augusta University Hospital, Augusta, Georgia, United States.
- Departments of Orthopedic Surgery, Augusta University Hospital, Augusta, Georgia, United States.
Correspondence Address:
Dayton Grogan
Departments of Neurosurgery, Augusta University Hospital, Augusta, Georgia, United States.
DOI:10.25259/SNI_189_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Taylor Waitt, Vamsi Reddy, Dayton Grogan, Pearce Lane, Joseph Kilianski, John DeVine, Alexander Post. A case of dual three-column thoracic spinal fractures following traumatic injury. 13-Jun-2020;11:150
How to cite this URL: Taylor Waitt, Vamsi Reddy, Dayton Grogan, Pearce Lane, Joseph Kilianski, John DeVine, Alexander Post. A case of dual three-column thoracic spinal fractures following traumatic injury. 13-Jun-2020;11:150. Available from: https://surgicalneurologyint.com/surgicalint-articles/10079/
Abstract
Background: Thoracic spine fracture-dislocations due to motor vehicle accidents (MVAs) rarely involve double- level, noncontiguous lesions.
Case Description: A 19-year-old male following an MVA was paraplegic; he exhibited full motor/sensory loss below the T4 level (i.e., ASIA scale Grade A). The chest X-ray, magnetic resonance, and computed tomography studies confirmed T3–T5 and T11–12 fractures, warranting T3–L3 thoracolumbar decompression and fusion. Despite surgical intervention, the patient’s neurological status remained unchanged.
Conclusion: This case illustrates the rare presentation of noncontiguous, posttraumatic thoracic spinal lesions requiring simultaneous decompression/fixation.
Keywords: Noncontiguous spinal injury, Spondyloptosis, Thoracic spinal injury, Trauma
INTRODUCTION
Noncontiguous double-level thoracic spine fracture-dislocations are quite rare. Typically, they are attributed to high-impact trauma resulting in complete spinal cord injuries.[
CASE DESCRIPTION
A 19-year-old male, following a major motor vehicle accident (MVA), presented with a Glasgow Coma Scale (GCS) of 15. On examination, he was intact in the upper extremities but had a complete American Spinal Injury Association (ASIA) “A” injury below the T4 level (total motor and sensory loss).
EXAMINATION/IMAGING
X-ray and computed tomography (CT) imaging
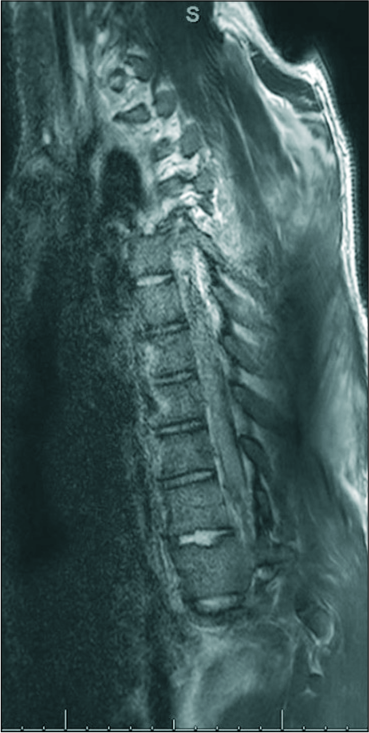
The chest X-ray revealed left pulmonary contusions and multiple posterior left-sided rib fractures. In addition, spondyloptosis at the T11/T12 level and fracture/left lateral subluxation at T3–T5 were noted on imaging. From T3–T5, the CT showed a T3 spinous process fracture and left displacement of T4 on T5. The lower injury was accompanied by rotation and 8 mm of traumatic retrolisthesis. Intracanalicular gas signaled the presence of a prevertebral T4– T5 hematoma. At T11/12, there were spondyloptosis, shearing of the superior T12 endplate, obliteration of the spinal canal, intracanalicular gas, and a prevertebral hematoma. There was also a chronic dextroscoliotic deformity of the mid-thoracic spine centered at T8.
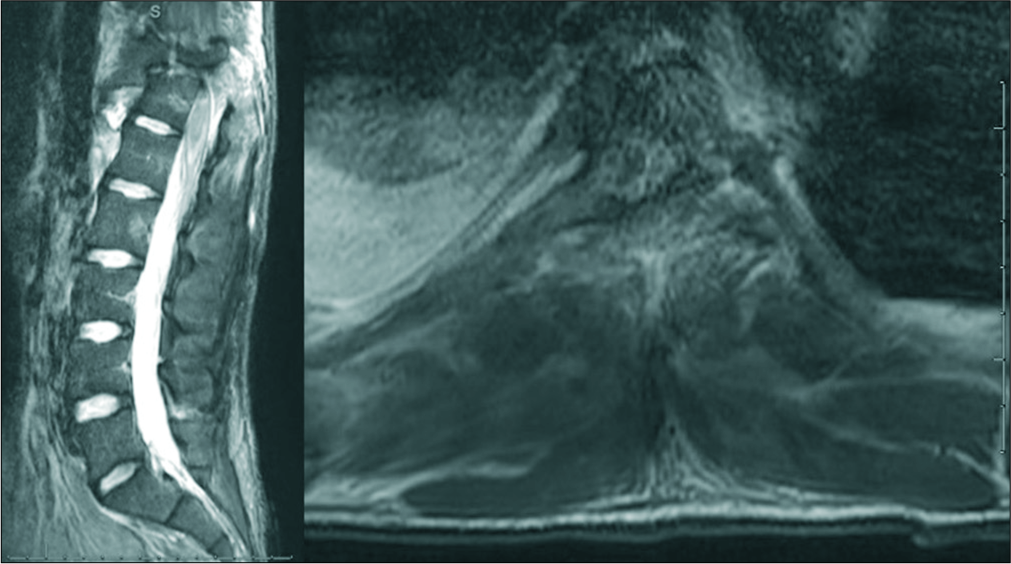
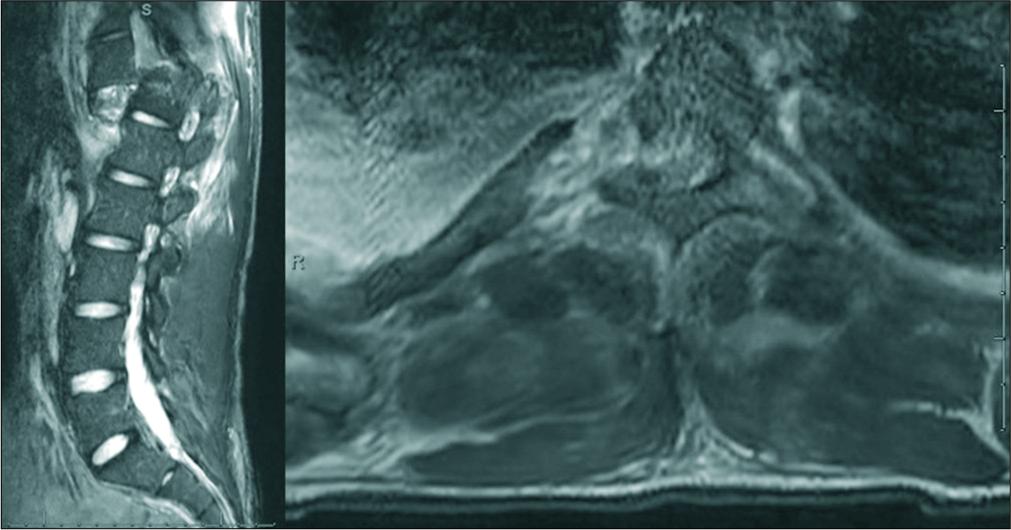
Magnetic resonance findings
Magnetic resonance imaging of the thoracic and lumbar spine confirmed traumatic dislocation/spondyloptosis of T11/T12 (i.e., with T11 projecting nearly 3.0 cm anterior to T12). Fragmentation of articular pillars/neural arches at T11–T12 and bone fragments projecting into the spinal canal [
Treatment/Diagnosis
The patient underwent T3–L3 surgical decompression/ fusion under fluoroscopic guidance of his spinal fractures from T3–T5, spondyloptosis at T11/12, and scoliotic deformity. This warranted the placement of pedicle screws bilaterally from T3–L2. Unilateral placement of pedicle screws also occurred on the right at T7 and on the left at T8. The intraoperative CT scan showed good reduction/alignment at the T4–T5 and T11–T12 levels. Neuromonitoring signals did not change after the placement of screws, reduction of spondyloptosis, laminectomy, rod placement, or decompression.
DISCUSSION
Classification systems of T3–5 and T11-12 fractures/ dislocations
In the setting of trauma, Vacarro et al. have proposed two different methods of classification to distinguish injuries of the spinal column.[
History of missed secondary thoracic spinal injuries
There is a long history of the literature regarding missed secondary spinal injuries.[
CONCLUSION
With complex thoracic trauma due to MVA, patients may have neurological examinations that do not clearly correlate with noncontiguous dual thoracic spinal cord injuries. Nevertheless, they should undergo full thoracic spinal MR/ CT screening to avoid missing noncontiguous traumatic lesions, as demonstrated in this case.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Kanna RM, Gaike CV, Mahesh A, Shetty AP, Rajasekaran S. Multilevel non-contiguous spinal injuries: Incidence and patterns based on whole spine MRI. Eur Spine J. 2016. 25: 1163-9
2. Salehani AA, Baum GR, Howard BM, Holland CM, Ahmad FU. Floating thoracic spine after double, noncontiguous three-column spinal fractures. World Neurosurg. 2016. 91: 670.e7-11
3. Takami M, Okada M, Enyo Y, Iwasaki H, Yamada H, Yoshida M. Noncontiguous double-level unstable spinal injuries. Eur J Orthop Surg Traumatol. 2017. 27: 79-86
4. Vaccaro AR, Lehman RA, Hulbert RJ, Anderon PA, harris M, Hedlund R. A new classification of thoracolumbar injuries: The importance of injury morpholy, the integrity of the posterior ligamentous complex, and neurologic status. Spine (Phila Pa 1976). 2005. 30: 2325-33
5. Vaccaro AR, Oner C, Kepler CK, Dvorak M, Schnake K, Bellabarba C. AOSpine thoracolumbar spine injury classification system: Fracture description, neurological status, and key modifiers. Spine (Phila Pa 1976). 2013. 38: 2028-37