- Departments of Neurosurgery Kindai University Faculty of Medicine, Osaka-Sayama, Osaka, Japan.
- Departments of Microbiology, Kindai University Faculty of Medicine, Osaka-Sayama, Osaka, Japan.
Correspondence Address:
Takayuki Nakao
Departments of Neurosurgery Kindai University Faculty of Medicine, Osaka-Sayama, Osaka, Japan.
DOI:10.25259/SNI-106-2019
Copyright: © 2019 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Takayuki Nakao, Takeshi Okuda, Mitsugu Fujita, Amami Kato. A case of leptomeningeal metastases of human epidermal growth factor receptor 2-positive breast cancer that responded well to lapatinib plus capecitabine. 28-Jun-2019;10:131
How to cite this URL: Takayuki Nakao, Takeshi Okuda, Mitsugu Fujita, Amami Kato. A case of leptomeningeal metastases of human epidermal growth factor receptor 2-positive breast cancer that responded well to lapatinib plus capecitabine. 28-Jun-2019;10:131. Available from: http://surgicalneurologyint.com/surgicalint-articles/9439/
Abstract
Background: Leptomeningeal metastases (LM) pose the most difficult form of cancer metastasis to treat and portend a poor prognosis. Standard treatment has yet to be established, and intrathecal chemotherapy and whole- brain radiotherapy are administered on an empirical basis.
Case Description: We report on a 46-year-old woman with LM from human epidermal growth factor receptor 2 (HER2)-positive breast cancer. She was suffering from intractable headaches, severe nausea and vomiting, and cerebellar ataxia. Contrast-enhanced magnetic resonance imaging (MRI) revealed diffuse enhancement of the meninges, mainly in the posterior cranial fossa, and compression of the cerebellum by the profoundly thickened meninges. The first step in the treatment was decompression of the posterior cranial fossa to relieve intracranial hypertension. After surgery, her symptoms immediately improved. The second step was treatment with lapatinib at 1250 mg and capecitabine 1200 mg, which dramatically improved her symptoms and disappeared diffuse abnormal signal enhancement on MRI.
Conclusion: We treated a patient with LM from primary HER2-positive breast cancer who responded well to lapatinib plus capecitabine.
Keywords: Breast cancer, Capecitabine, Human epidermal growth factor receptor 2, Lapatinib, Leptomeningeal metastases
INTRODUCTION
Leptomeningeal metastases (LM) occur when cancer cells invade the pia mater, arachnoid mater, subarachnoid space, and cerebrospinal fluid of the central nervous system.[
CASE PRESENTATION
A 46-year-old woman had undergone mastectomy for breast cancer (estrogen receptor 2+, progesterone receptor 3+, and HER2 3+) 5 years before presentation and had subsequently remained under observation without any postoperative adjuvant therapy. Multiple lung, liver, and bone metastases were identified in year 3 postoperatively, and systemic chemotherapy was introduced. The chemotherapy regimen included docetaxel, trastuzumab, pertuzumab, and bisphosphonates, and radiotherapy for lumbar spinal bone metastases (20 Gy/5 Fr). However, she developed multiple brain metastases (BM) 1 year later, which were treated with whole-brain radiotherapy (30 Gy/10 Fr) and placement of a ventriculoperitoneal shunt for hydrocephalus. The systemic chemotherapy regimen was subsequently switched to trastuzumab emtansine, but further LM developed, and the patient was referred to our hospital.
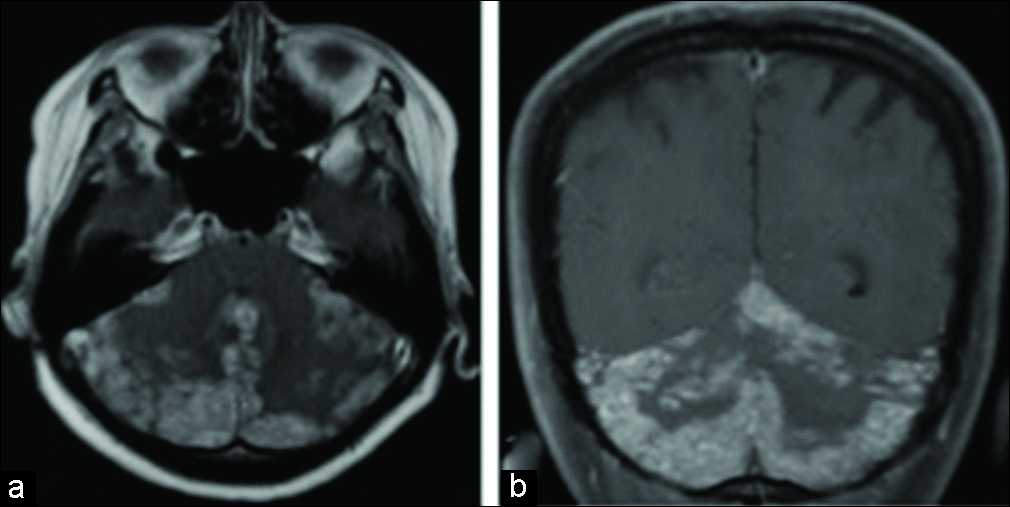
At the time of referral, Eastern Cooperative Oncology Group (ECOG) performance status was 4, level of consciousness as assessed by Glasgow coma scale score was E3V4M6, and she was suffering from intractable headaches, severe nausea and vomiting, and cerebellar ataxia. T1-weighted gadolinium- enhanced magnetic resonance imaging (MRI) revealed diffuse contrast enhancement of the meninges, mainly in the posterior cranial fossa, with compression of the cerebellum by the significantly thickened meninges [
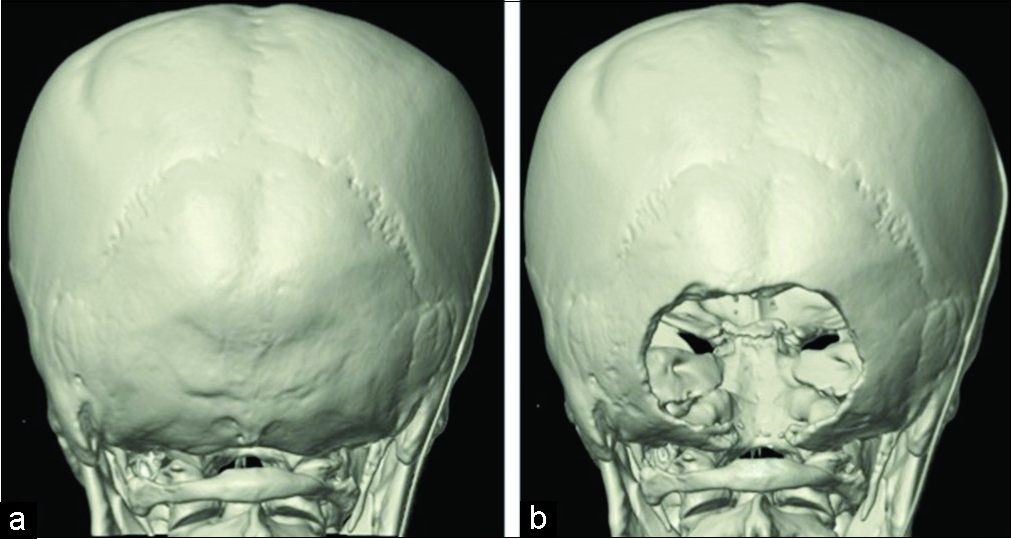
However, the patient requested further therapy, and given her good karnofsky performance status (KPS), an aggressive treatment strategy was pursued. The first step in the treatment was to relieve intracranial hypertension, and decompression of the posterior cranial fossa was performed [
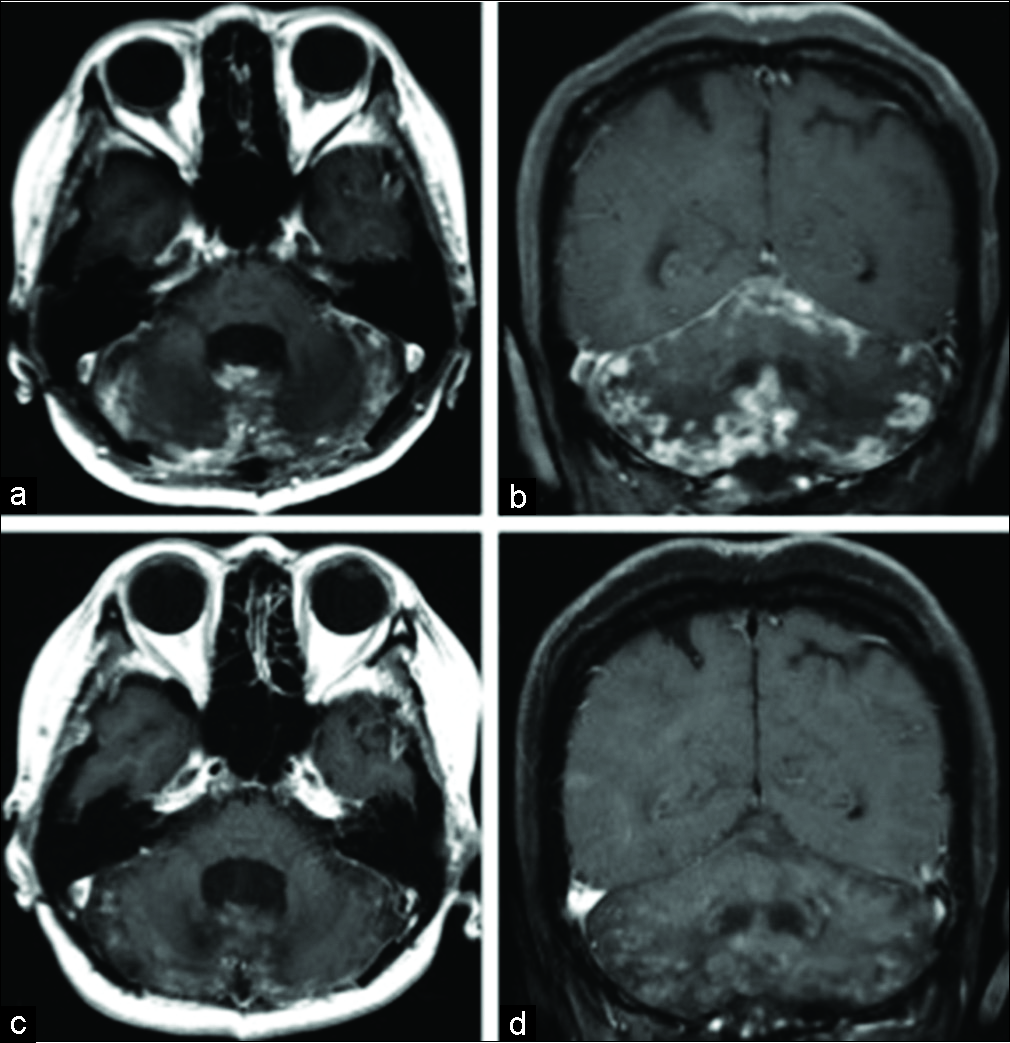
Treatment with lapatinib at 1250 mg and capecitabine 1200 mg was started on postoperative day 14. As early as 2 weeks later, the diffuse abnormal signal enhancement across her tissues shrunk dramatically on T1-weighted gadolinium- enhanced MRI after starting this new regimen [
Figure 3:
Magnetic resonance imaging images (a,b) T1-weighted gadolinium-enhanced MRI (axial and coronal images) after 2 weeks. Diffuse enhancement of the meninges has improved markedly. (c,d) T1-weighted gadolinium-enhanced MRI (axial and sagittal images) after 2 months. Diffuse enhancement of the meninges has almost disappeared.
DISCUSSION
Recently, a number of cases have been reported of BM responding to systemic chemotherapy, particularly using molecular-targeted drugs. With lung cancer treatment, good therapeutic outcomes have been reported with the use of molecular-targeted drugs not only for BM but also for LM.[
Lapatinib has now succeeded trastuzumab as a new drug targeting HER2 and epidermal growth factor receptor, and its low molecular weight compared with trastuzumab gives support to the notion of greater efficacy against central nervous system lesions. We have reported herein a case in which LM responded well to combination therapy with lapatinib plus capecitabine. Although our patient had undergone decompression surgery to relieve symptoms of intracranial hypertension, the effects were certainly expected to be temporary only, and hence the second step treatment with lapatinib plus capecitabine was added. The effects of this combination of chemotherapy were rapidly apparent, and a good outcome for the patient was achieved.
The response rate with lapatinib monotherapy for recurrent BM after treatment with trastuzumab and radiotherapy is 2.6%–6.0% and this rate is further improved in combination therapy with capecitabine.[
The response assessment in a neuro-oncology working group recently proposed guidelines for the diagnosis and response assessment of LM.[
CONCLUSION
We treated a patient with LM from primary HER2- positive breast cancer who responded well to lapatinib plus capecitabine.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understands that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
None.
Conflicts of interest
There are no conflicts of interest.
References
1. Assi HI, Mahmoud T, Saadeh FS, Darsa HE. Management of leptomeningeal metastasis in breast cancer. Clin Neurol Neurosurg. 2018. 172: 151-9
2. Bachelot T, Romieu G, Campone M, Dieras V, Cropet C, Dalenc F. Lapatinib plus capecitabine in patients with previously untreated brain metastases from HER2-positive metastatic breast cancer (LANDSCAPE): A single-group phase 2 study. Lancet Oncol. 2013. 14: 64-71
3. Chamberlain M, Junck L, Brandsma D, Soffietti R, Ruda R, Raizer J. Leptomeningeal metastases: A RANO proposal for response criteria. Neuro Oncol. 2017. 19: 484-92
4. Hida T, Nokihara H, Kondo M, Kim YH, Azuma K, Seto T. Alectinib versus crizotinib in patients with ALK-positive non-small-cell lung cancer (J-ALEX): An open-label, randomised phase 3 trial. Lancet. 2017. 390: 29-39
5. Katayama T, Shimizu J, Suda K, Onozato R, Fukui T, Ito S. Efficacy of erlotinib for brain and leptomeningeal metastases in patients with lung adenocarcionoma who showed initial good response to gefitinib. J Thorac Oncol. 2009. 4: 1415-9
6. Lee DW, Lee KH, Kim JW, Keam B. Molecular targeted therapies for the treatment of leptomeningeal carcinomatosis: Current evidence and future directions. Int J Med Sci. 2016. 17: 1074-85
7. Lee E, Keam B, Kim DW, Kim TM, Lee SH, Chung DH. Erlotinib versus gefitinib for control of leptomeningeal carcinomatosis in non-small-cell lung cancer. J Thorac Oncol. 2013. 8: 1069-74
8. Lin NU, Carey LA, Liu MC, Younger J, Come SE, Ewend M. Phase II trial of lapatinib for brain metastases in patients with human epidermal growth factor receptor 2-positive breast cancer. J Clin Oncol. 2008. 26: 1993-9
9. Lin NU, Dieras V, Paul D, Lossignol D, Christodoulou C, Stemmler HJ. Multicenter phase II study of lapatinib in patients with brain metastases from HER2-positive breast cancer. Clin Cancer Res. 2009. 15: 1452-9
10. Peter S, Camidge R, Shaw AT, Gadgeel S, Ahn JS, Kim DW. ALEX trial investigators. Alectinib versus crizotinib in untreated ALK-positive non-small-cell lung cancer. N Engl J Med. 2017. 377: 829-38
11. Rhun EL, Taillibert S, Chamberlain MC. Carcinomatous meningitis: Leptomeningeal metastases in solid tumors. Surg Neurol Int. 2013. 4: S265-88
12. Sengupta S, Rojas R, Mahadevan A, Kasper EM, Jeyapalan S. CPT-11/bevacizumab for the treatment of refractory brain metastases in patients with HER2-neu-positive breast cancer. Oxf Med Case Reports. 2015. 4: 254-7