- Department of Neurosurgery, Tenri Hospital, Tenri, Nara, Japan.
DOI:10.25259/SNI_328_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Masahiko Itani, Satoshi Shitara, Yoshinori Akiyama. A convexity meningioma presenting with an acute subdural hematoma. 29-Aug-2020;11:263
How to cite this URL: Masahiko Itani, Satoshi Shitara, Yoshinori Akiyama. A convexity meningioma presenting with an acute subdural hematoma. 29-Aug-2020;11:263. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=10231
Abstract
Background: Meningiomas presenting with acute subdural hematomas are extremely rare. To the best of our knowledge, only 45 cases have been reported to date. We report on a case of a meningioma mimicking an acute subdural hematoma as well as a thorough literature review.
Case Description: A 67-year-old man with no history of trauma was referred to our hospital with sudden onset of decreased level of consciousness and left hemiplegia. Computed tomography revealed an acute convexity subdural hematoma. Emergency surgery to remove the hematoma was performed. The hematoma was found to exist in the extra-axial space and the attached dura mater and pia mater remained intact. Pathological examination revealed a transitional meningioma, the World Health Organization Grade 1. Detailed medical history taken postoperatively revealed that a convexity meningioma had been diagnosed incidentally at another facility 1 year earlier.
Conclusion: Acute subdural hematomas due to meningiomas are rare, and establishing the cause is challenging. Prompt and precise diagnosis of such entities may afford patients a better prognosis.
Keywords: Hemorrhagic manifestation, Meningioma, Nontraumatic acute subdural hematoma
INTRODUCTION
Meningiomas are one of the most common benign intracranial tumors and account for 13– 27% of all primary intracranial tumors.[
CASE PRESENTATION
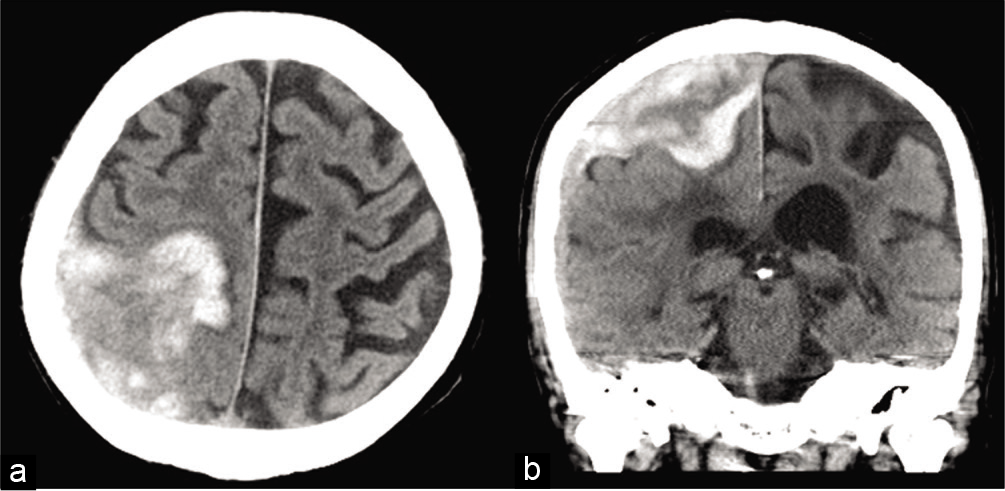
A 67-year-old man was referred to our hospital with sudden onset of a decreased level of consciousness and left hemiplegia with no history of trauma. Computed tomography revealed a 5 cm ASDH located in the right parietal and frontal lobes [
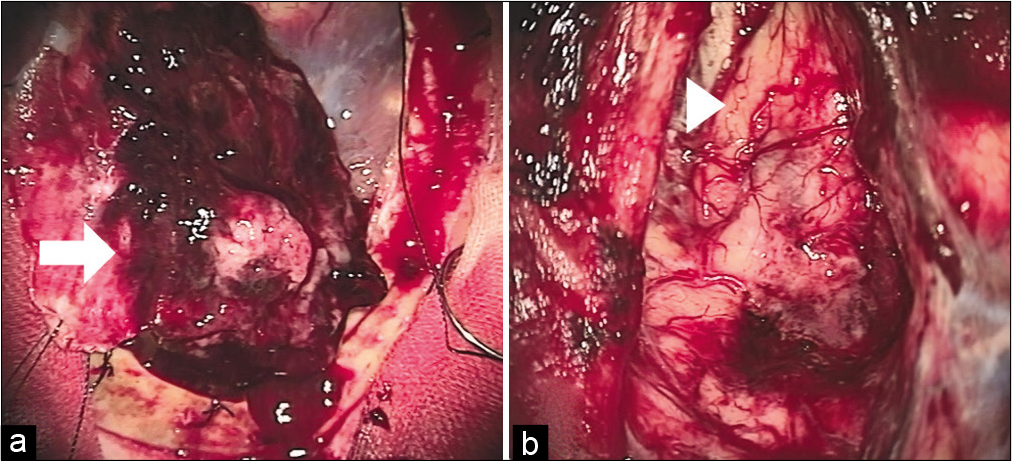
Urgent hematoma evacuation was recommended and performed with the consent of his family. A right parietal craniotomy was performed that revealed a swollen dura mater and a hematoma. The ASDH included parenchyma components and was located extra-axially with intact pia mater and dura mater attached [
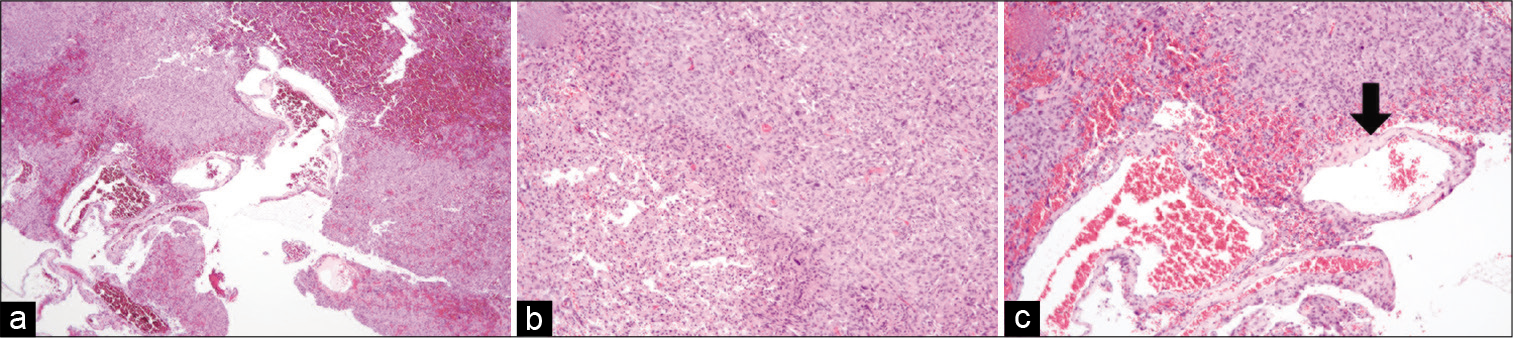
Pathology findings revealed lobular and fascicular foci with conspicuous tight whorls and psammoma bodies. The tumor was highly vascularized with expanded thin-walled vessels detected in parts [
Figure 3:
Hematoxylin and eosin (H and E) staining revealed a transitional meningioma (a-c). Lobular and fascicular foci appeared with conspicuous tight whorls and psammoma bodies (a, b). Expanded vessels with thin walls were visible within the tumor itself (c). Original magnification ×40 (a) and ×100 (b, c).
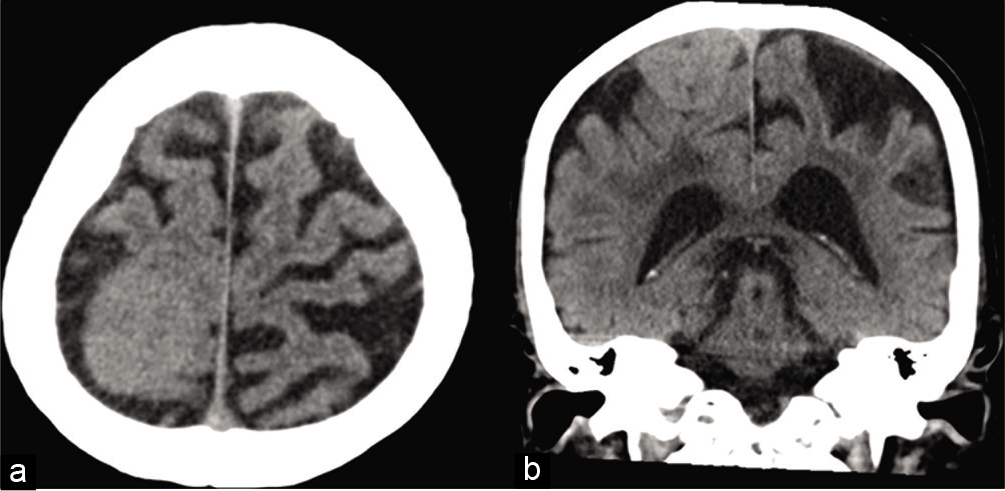
Postoperatively, the medical history taken from the patient’s family revealed the fact that he had an incidental finding of a small right convexity meningioma 1 year previously by another clinician [
DISCUSSION
Here, we have illustrated the case of an ASDH that arose from an extra-axial tumor. Spontaneous intracranial hemorrhage (sICH) associated with a brain tumor occurs in 1.7–9.6% of cases and accounts for 0.9–10.2% of all sICH.[
Among the 45 cases reported in the literature, the mean age at diagnosis was 67 years (32–85 years), and there were 27 females (58%). The most common locations of ASDH were the convexity (66%) followed by the falx/parasagittal (26%). Several reports discussed the association between the location of the meningioma and the rate of hemorrhage, but no consensual view has been obtained.[
Pathologically, we found that the most common type is meningothelial meningioma (44%, 20 out of 45 cases) followed by transitional meningioma and angioblastic meningioma (17%, 8 cases).[
The mechanism of hemorrhage remains unclear. Okuno et al. and Aloraidi et al. suggested that expansion of the meningioma stretches the bridging vein and subdural vein, consequently making these vessels fragile and vulnerable to minor trauma.[
CONCLUSION
We have highlighted the case of a meningioma presenting with an ASDH. This suggests that careful history taking, and the possibility of underlying tumors such as meningioma, should be considered when assessing a nontraumatic ASDH.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Aloraidi A, Abbas M, Fallatah B, Alkhaibary A, Ahmed ME, Alassiri AH. Meningioma presenting with spontaneous subdural hematoma: A report of two cases and literature review. World Neurosurg. 2019. 127: 150-4
2. Boŝnjak R, Derham C, Popović M, Ravnik J. Spontaneous intracranial meningioma bleeding: Clinicopathological features and outcome. J Neurosurg. 2005. 103: 473-84
3. Chaskis C, Raftopoulos C, Noterman J, Flament-Durand J, Brotchi J. Meningioma associated with subdural haematoma: Report of two cases and review of the literature. Clin Neurol Neurosurg. 1992. 94: 269-74
4. . Committee of Brain Tumor Registry of Japan. Brain tumor registry of Japan (2001-2004). Neurol Med Chir (Tokyo). 2014. 54: 1-102
5. Douglas K, Mark B, Lothar R, Charles HT, Fleming JF, Vanderlinden RG. Significance of hemorrhage into brain tumors: Clinicopathological study. J Neurosurg. 1987. 67: 852-7
6. Hambra DV, Danilo DP, Alessandro R, Sara M, Juan GR. Meningioma associated with acute subdural hematoma: A review of the literature. Surg Neurol Int. 2014. 5: S469-71
7. Helle TL, Conley FK. Haemorrhage associated with meningioma: A case report and review of the literature. J Neurol Neurosurg Psychiatry. 1980. 43: 725-9
8. Lim JY, Kanodia AK, Abdelsadg M, Badran K, Sudarshan T, Prasad G. Transitional meningioma with intratumoural bleed and associated subdural haemorrhage: Case report and a review of literature. J Neurosci Neurosurg. 2018. 1: 110
9. Martínez-Lage JF, Poza M, Martinez M, Esteban JA, Antunez MC, Sola J. Meningiomas with haemorrhagic onset. Acta Neurochir (Wien). 1991. 110: 129-32
10. Masoudi MS, Zafarshamspour S, Ghasemi-Rad M, Soleimani N, Rakhsha A, Lincoln C. Acute subdural hemorrhage of a convexity meningioma in the postpartum period; case report and literature review. Bull Emerg Trauma. 2019. 7: 324-9
11. Matsuoka G, Eguchi S, Ryu B, Tominaga T, Ishikawa T, Yamaguchi K. Treatment strategy for recurrent hemorrhage from meningioma: Case report and literature review. World Neurosurg. 2019. 124: 75-80
12. Niiro M, Ishimaru K, Hirano H, Yunoue S, Kuratsu J. Clinico-pathological study of meningiomas with haemorrhagic onset. Acta Neurochir (Wien). 2003. 145: 767-72
13. Okuno S, Touho H, Ohnishi H, Karasawa J. Falx meningioma presenting as acute subdural hematoma: Case report. Surg Neurol. 1999. 52: 180-4
14. Sato K, Matsuo A, Hiu T, Kurohama H, Miura S, Ito K. Falx meningioma presenting with intratumoral hemorrhage and interhemispheric acute subdural hematoma: A case of report. No Shinkei Geka. 2020. 48: 413-22
15. Suzuki Y, Fujimoto M, Kawakita F, Asakura F, Murata H, Morooka Y. Tiny falx meningioma causing massive interhemispheric subdural hematoma: A case report. NMC Case Rep J. 2018. 5: 51-5
16. Wakai S, Yamakawa K, Manaka S, Takakura K. Spontaneous intracranial hemorrhage caused by brain tumor: Its incidence and clinical significance. Neurosurgery. 1982. 10: 437-44
17. Whittle IR, Smith C, Navoo P, Collie D. Meningiomas. Lancet. 2004. 363: 1535-43
18. Worm PV, Ferreira MP, Ferreira NP, Cechetti F. Subdural haematoma in a patient with meningioma. Arq Neuropsiquiatr. 2009. 67: 308-10
19. Ziyal IM, Bilginer B, Celik O, Ozcan OE, Ozgen T. Tentorial meningioma on follow-up presenting with sudden deterioration due to intra-and peritumoral hemorrhage. Acta Neurochir (Wien). 2006. 148: 1315-6