- School of Medicine, Case Western Reserve University, Cleveland, Ohio, United States.
- Department of Neurosurgery, University Hospitals Cleveland Medical Center, Cleveland, Ohio, United States.
Correspondence Address:
Alia M. Hdeib M.D. Department of Neurosurgery, University Hospitals Cleveland Medical Center, Cleveland, Ohio, United States.
DOI:10.25259/SNI_623_2021
Copyright: © 2021 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Uma V. Mahajan1, Mohit Patel2, Alia M. Hdeib2. Cervical schwannoma with acute worsening and intratumoral hemorrhage. 16-Aug-2021;12:409
How to cite this URL: Uma V. Mahajan1, Mohit Patel2, Alia M. Hdeib2. Cervical schwannoma with acute worsening and intratumoral hemorrhage. 16-Aug-2021;12:409. Available from: https://surgicalneurologyint.com/surgicalint-articles/cervical-schwannoma-with-acute-worsening-and-intratumoral-hemorrhage/
Abstract
Background: Primary spinal tumors are rare and include schwannomas. In the cervical region, these lesions can cause pain, radiculopathy, and/or myelopathy.
Case Description: A 53-year-old male presented with 9 months of chronic neck pain and left upper extremity radiculopathy/myelopathy. The MRI revealed an intradural extramedullary C6-C7 left-sided mass with foraminal extension. Following a C5-C7 laminectomy with C5-T2 instrumented fusion, the diagnosis of schwannoma with evidence of recent hemorrhage was confirmed by biopsy. Three weeks postoperatively, the patient was pain free, no longer taking opioids, and neurologically intact. Although the MRI 6 months later showed no tumor, the MRI 15 months later documented a recurrent enhancing C6-C7 lesion. The patient elected to be treated with external beam radiotherapy and remained asymptomatic.
Conclusion: A 53-year-old underwent resection of a cervical C6-C7 schwannoma with intratumoral hemorrhage. Fifteen months following C5-C7 laminectomy with C5-T2 fusion, the tumor recurred and required external beam radiation therapy.
Keywords: Cervical radiculopathy, Cervical schwannoma, Intratumoral hemorrhage, Spinal tumor
INTRODUCTION
Primary spinal tumors are rare (i.e. 2 cases/100,000/year).[
CASE ILLUSTRATION
Initial presentation
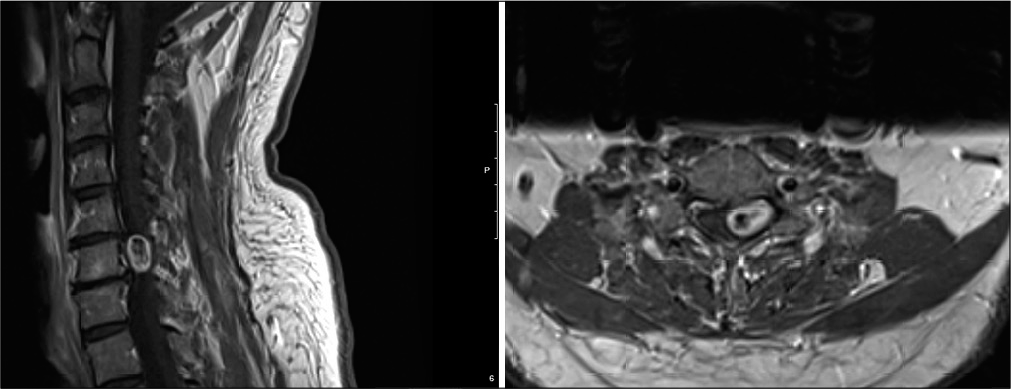
A 53-year-old male presented with 9 months of chronic neck pain and worsening left upper extremity radiculopathy. The cervical magnetic resonance imaging (MRI) showed a left-sided C6-C7 intradural extramedullary mass extending into the neural foramen, resulting in cord/root compression [
Surgery
A C5-C7 laminectomy with C5-T2 instrumentation and fusion was performed, the tumor was removed under direct intraoperative neurophysiologic monitoring and stimulation, and biopsy revealed benign schwannoma.
Follow-up
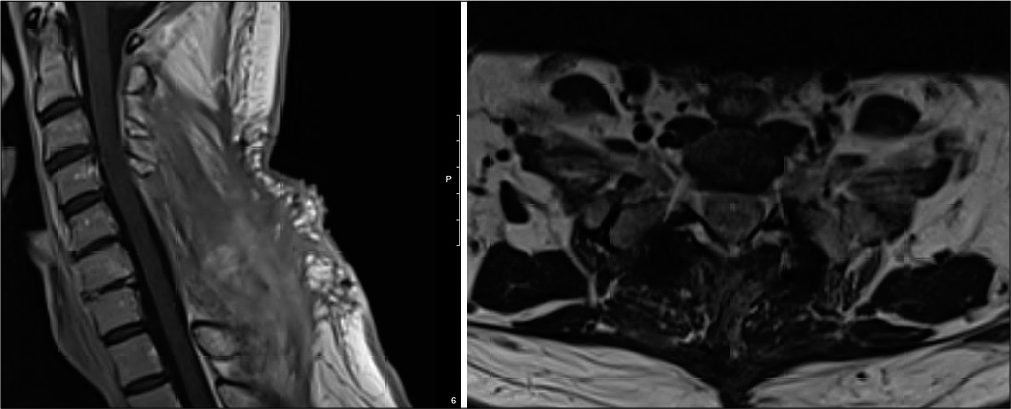
Three weeks postoperatively, the patient was neurologically intact, pain free, and no longer taking opioids [
DISCUSSION
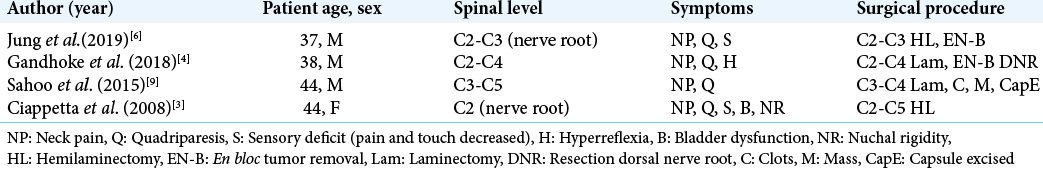
We identified four published cases of cervical schwannomas presenting with intratumoral hemorrhages. All patients underwent urgent tumor resection and fully recovered neurological function.
Jung et al. reported a single case of C2-C3 left-sided spinal cord compression due to a schwannoma compressing the cord and attached to the left nerve root.[
Surgical techniques include tumor excision with neural preservation or sacrifice, tumor enucleation between adjacent healthy nerve fibers, and tumor emptying with tumor capsule preservation.[
CONCLUSION
Here, we report a 53-year-old patient who presented with a cervical C6-C7 schwannoma accompanied by an intratumoral hemorrhage contributing to cervical radiculopathy. Following a C5-C7 laminectomy for tumor excision and a C5-T2 fusion, the foraminal portion of the lesion recurred 15 months later warranting the utilization of focal radiation therapy.
Statement of ethics
Informed consent from the patient was obtained for this report and for all accompanying figures. IRB approval was not sought because the patient had given permission for his clinical information to be shared and had completed signed authorization for release of this information. Identifiers for the patient were not included in the publication.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Alemi AS, Heaton CM, Ryan WR, El-Sayed I, Wang SJ. Volumetric growth of cervical schwannoma as a predictor of surgical intervention. Otolaryngol Head Neck Surg. 2017. 156: 152-5
2. Ansari I, Ansari A, Graison AA, Patil AJ, Joshi H. Head and neck schwannomas: A surgical challenge-a series of 5 cases. Case Rep Otolaryngol. 2018. 2018: 4074905
3. Ciappetta P, D’Urso PI, Colamaria A. Giant craniovertebral junction hemorrhagic schwannoma: Case report. Neurosurgery. 2008. 62: E1166
4. Gandhoke CS, Syal SK, Singh D, Batra V, Nallacheruvu Y. Cervical C2 to C4 schwannoma with intratumoral hemorrhage presenting as acute spastic quadriparesis: A rare case report. Surg Neurol Int. 2018. 9: 142
5. Givan G, Simons SM, Yount R. Cervical schwannoma presenting as neck pain following motor vehicle accident. Curr Sports Med Rep. 2011. 10: 37-9
6. Jung GS, Lee YM, Kim YZ, Kim JS. Intratumoral hemorrhage of the cervical spinal schwannoma presenting: Acute quadriparesis. Brain Tumor Res Treat. 2019. 7: 160-3
7. Keles E, Eroglu O, Ozercan IH, Ozel I. Schwannoma in the supraclavicular region: Case report. Turk Arch Otorhinolaryngol. 2018. 56: 54-7
8. Kuroiwa M, Yako T, Goto T, Higuchi K, Kitazawa K, Horiuchi T. Inter-capsular resection of cervical vagus nerve schwannoma. J Clin Neurosci. 2018. 54: 161-4
9. Sahoo RK, Das PB, Sarangi GS, Mohanty S. Acute hemorrhage within intradural extramedullary schwannoma in cervical spine presenting with quadriparesis. J Craniovertebr Junction Spine. 2015. 6: 83-5
10. Yafit D, Horowitz G, Vital I, Locketz G, Fliss DM. An algorithm for treating extracranial head and neck schwannomas. Eur Arch Otorhinolaryngol. 2015. 272: 2035-8