- Department of Life, Health and Environmental Sciences (MESVA), University of L’Aquila, L’Aquila, Italy
- Department of Neurosurgery, San Salvatore City Hospital, L’Aquila, Italy
Correspondence Address:
Danilo De Paulis
Department of Life, Health and Environmental Sciences (MESVA), University of L’Aquila, L’Aquila, Italy
DOI:10.4103/2152-7806.185777
Copyright: © 2016 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Vitantonio HD, Paulis DD, Maestro MD, Ricci A, Dechordi SR, Marzi S, Millimaggi DF, Galzio RJ. Dural repair using autologous fat: Our experience and review of the literature. Surg Neurol Int 07-Jul-2016;7:
How to cite this URL: Vitantonio HD, Paulis DD, Maestro MD, Ricci A, Dechordi SR, Marzi S, Millimaggi DF, Galzio RJ. Dural repair using autologous fat: Our experience and review of the literature. Surg Neurol Int 07-Jul-2016;7:. Available from: http://surgicalneurologyint.com/surgicalint_articles/dural-repair-using-autologous-fat-experience-review-literature/
Abstract
Background:Various materials have been proposed to obliterate dead spaces and to reconstruct dural defects during a neurosurgical approach. This study describes our technique of using the abdominal autologous fat graft and evaluates the complications and characteristics related to the use of this tissue during cranial procedures.
Methods:Autologous fat grafts were used in 296 patients with basicranial and convexity extraaxial tumors from April 2005 to January 2015. The adipose tissue was removed from the paraumbilical abdominal region and was transformed into a thin foil. When possible, a watertight suture was made between the dural or bone edge with a fat graft. We always used fibrin glue to reinforce the dural closure.
Results:Complications occurred between 2 days and 1 year following procedure. Cerebrospinal fluid leaks were found in 11 cases. No case of mortality, pseudomeningoceles, fistula, infections, bacterial meningitides, or lipoid meningitides was reported. No patient required removal of the graft. No adhesion was observed between the brain and the autologous fat. Other fat-related complications observed were 2 cases of fat necrosis in the abdomen and 2 cases of abdominal hemorrhage.
Conclusion:The technique of harvesting and applying fat grafts is fairly simple, although it must be performed meticulously to be effective. Our experience has led us to believe that the use of fat grafts presents low morbidity and mortality. However, a neurosurgeon should never forget the possible late or early complications related to the use of fat grafts.
Keywords: Autologous fat graft, dural repair, dural substitute, watertight suture
INTRODUCTION
Both the reconstruction of dural defects after cranial surgery and the obliteration of the dead space after resection of large basicranial tumors are required.[
Dural substitutes could be autologous tissues (pericranium, fascia lata, fat, muscle) or artificial dural substitutes. The latter are generally derived from bovine tendon, bovine pericardium/dura, porcine collagen, polyurethane, polyglactin, polytetrafluoroethylene-based sheets, human acellular dermis, human fibrinogen and thrombin with equine collagen, and agents including polyglycolic acid mesh.[
This study presents our experience in using abdominal subcutaneous autologous fat in a series of patients who required the dural graft implantation and, when necessary, the obliteration of the dead space during cranial procedures. In addition, it examines the frequency and nature of complications.
MATERIALS AND METHODS
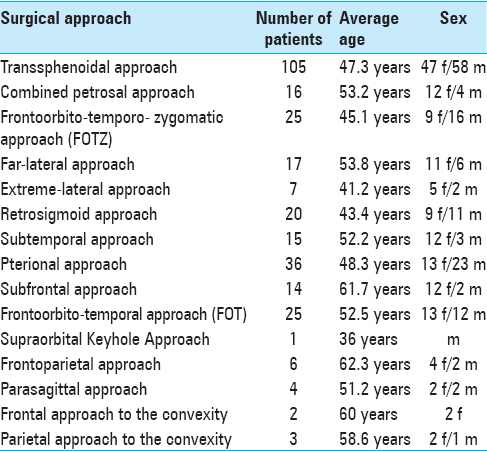
Between April 2005 and January 2015, 296 patients underwent autologous fat graft during basicranial and convexity extraaxial tumor resections at our Department of Neurosurgery; all patients are included in our retrospective study. The data regarding surgical approach, sex, and average age are reported in
No patient underwent a preoperative or postoperative radiotherapy. All patients were previously informed regarding methods and risks of the withdrawal of abdominal fat. The antibiotic prophylaxis was done with second-generation cephalosporins administered intravenously 30–60 min before the skin incision. The autologous fat was used in 281 procedures on the skull base and in 15 procedures on the convexity. The patients’ charts were analyzed to determine their demographic parameters, diagnosis, surgical approach, complications, treatment, and outcome.
Surgical technique
During the neurosurgical procedures, performed in a supine or lateral position, the adipose subcutaneous tissue is removed from the paraumbilical abdominal region. The excision of the subcutaneous fat is performed through a horizontal skin incision of 3 cm.
The anatomy of the abdominal subcutaneous fat is divided into superficial and deep layer.[
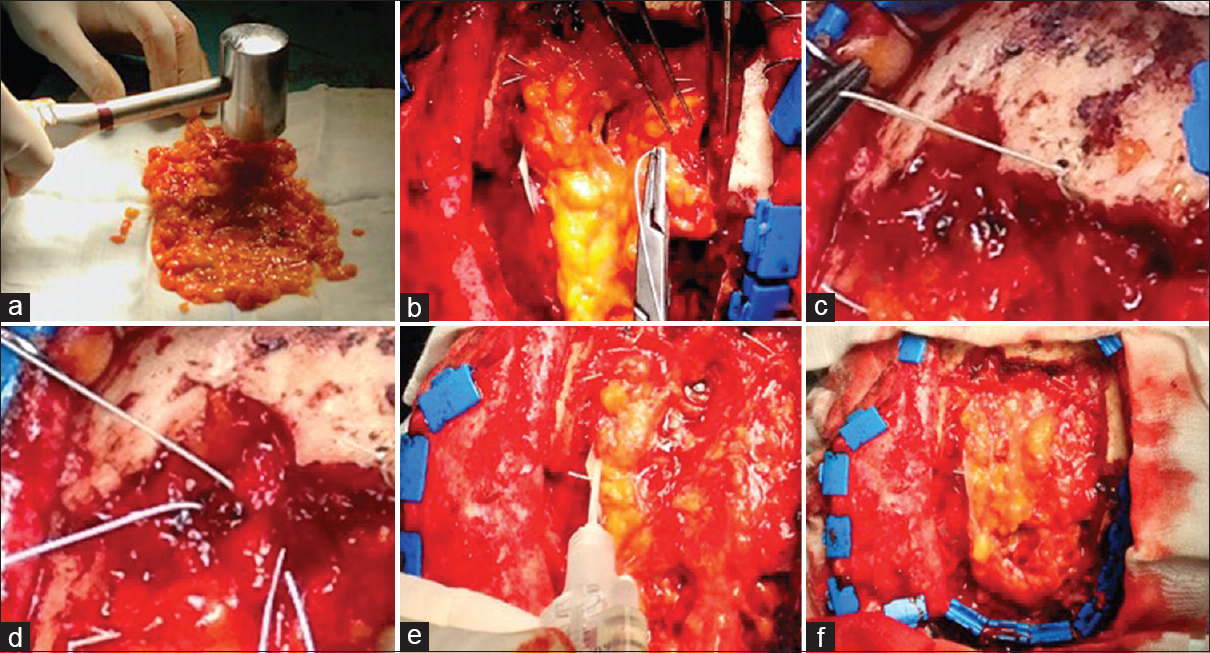
Figure 1
The fat graft can be used after being flattened with the use of a surgical hammer and is transformed into a thin foil (a). For the dural reconstruction, the fat is positioned below the free dural edge and sutured (b). When there is no free dural margin, the fat is positioned below the edge of the bone and then fixed (c) The fat can be turned on the sutured dural edge, thus forming another layer (d). At the end, the entire suture is reinforced with fibrin glue (e, f)
When necessary, for example during a transsphenoidal approach, the surgical dead cavity is obliterated with a large “pancake” of autologous fat, which is then fixed with a film of fibrin glue to complete the sealing. In addition, according to Spaziante et al.,[
For the dural reconstruction, the fat is positioned below the free dural edge and secured with Expanded Polytetrafluoroethylene (ePTFE) Nonabsorbable Monofilament No. 4-0. Subsequently, the fat is turned on the sutured dural edge, thus forming another layer, and then the entire suture is reinforced with fibrin glue [Figure
When there is no free dural margin, the fat is positioned below the edge of the bone and then fixed to the bone with ePTFE No. 3-0 through small drill holes prepared into the bony margins [
RESULTS
Abdominal fat grafts were used in 296 patients with convexity [
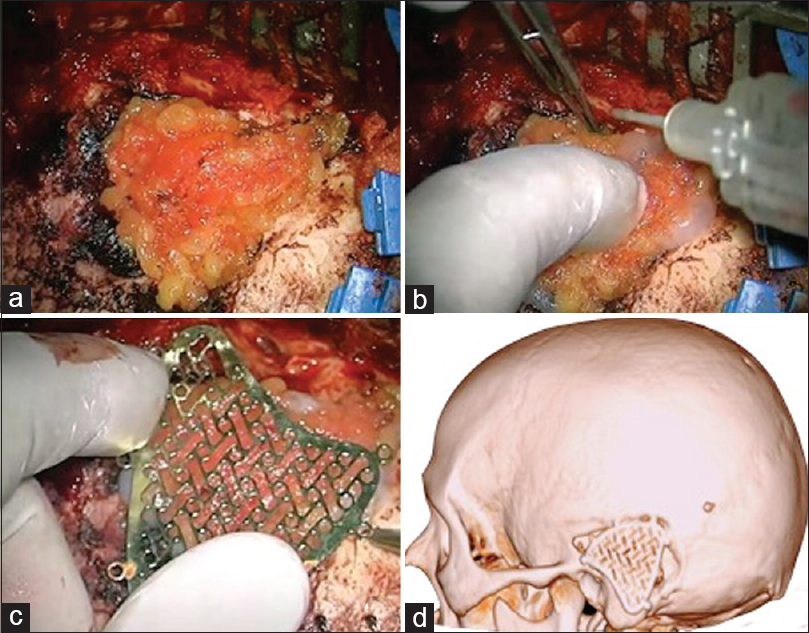
Figure 2
A 47-year-old male patient with “recidive chordoma,” arising from the posterior wall of the petrous apex, was operated. The lesion was exposed through a left petrosal retrolabyrinthine approach. The reconstruction of the approach was performed with autologous fat graft (a), fibrin glue and titanium mesh with the same shape of the mastoid process of the temporal bone (b and c). The postoperative computed tomography of the head in three-dimensional rendering showed the approach and its reconstruction (d). The follow-up at 1 year did not show any complication
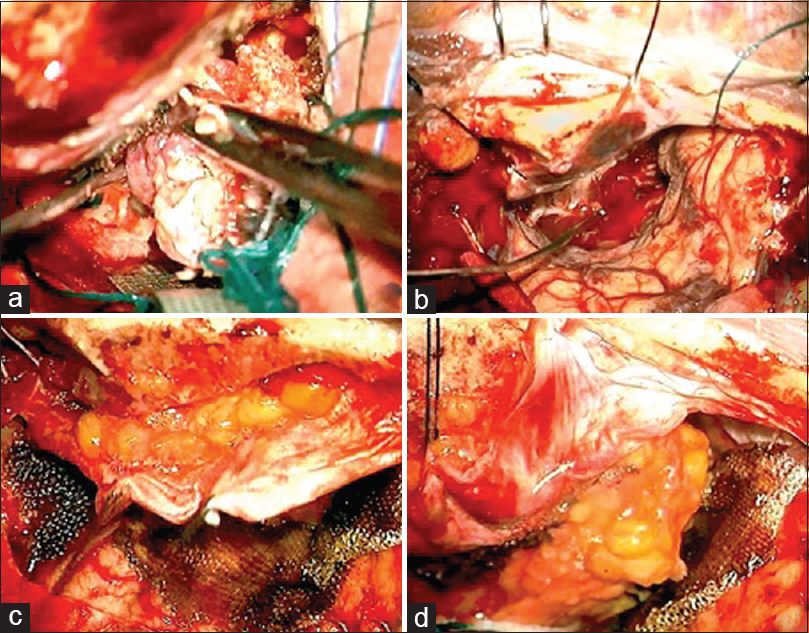
Figure 3
A 63-year-old female patient with “psammomatous meningioma” (WHO 1) originating from the floor of the anterior cranial fossa was operated. Through a left frontotemporal approach, a huge meningioma arising from the olfactory grove was exposed and removed (a and b). The floor of the anterior cranial fossa eroded by the lesion and the dura mater of the frontal convexity were reconstructed with abdominal fat graft avoiding cerebrospinal fluid fistula (c and d). The follow-up at 1 year did not show any complication
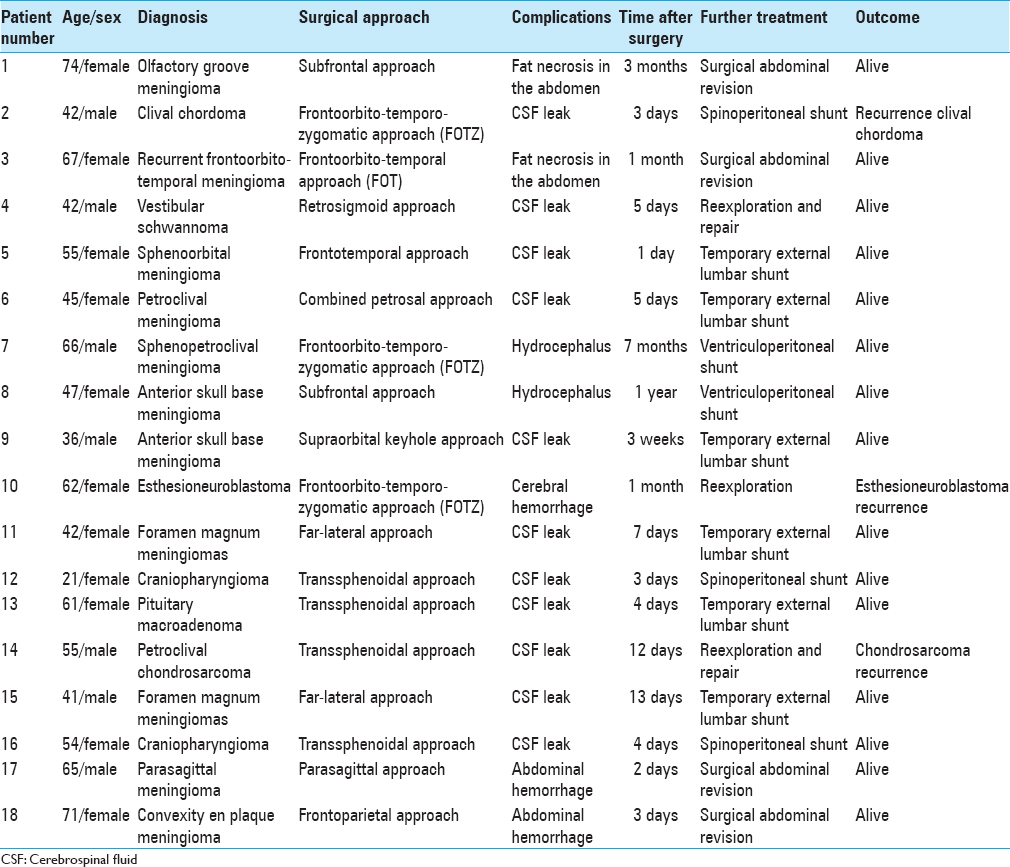
Complications were observed in only 18 patients (7 males, 11 females) and their onset occurred between 2 days and 1 year. Clinical characteristics, diagnosis, surgical approach, treatment, and outcome of patients with complications are reported in
CSF leaks were found in 11 of 18 cases. All these leaks were short-term complications because they appeared during the first 2 weeks after surgery. In 4 cases, the CSF leaks occurred after a transsphenoidal approach, and in 2 cases after a far-lateral approach. The remaining 5 cases of CSF leaks occurred after a frontoorbital-temporal approach, frontotemporal approach, retrosigmoid approach, combined petrosal approach, and supraorbital keyhole approach. No CSF leak occurred on the approaches to the convexity. Six cases were managed successfully with the placement of a temporary lumbar shunt for 3 days, whereas in 3 cases it was necessary to place a lumboperitoneal shunt. In 2 cases with persistent CSF leaks, a surgical reexploration and repair with another patch of autologous fat and fibrin glue were performed. Another short-term complication was the abdominal hemorrhage that in 2 cases presented during the second and third day after surgery. In both cases, it was necessary to make a surgical abdominal revision. Medium-term complications were identified between the 1st and the 3rd month after surgery. During this period, 2 cases of fat necrosis in the abdomen and 1 case of cerebral hemorrhage in a patient with esthesioneuroblastoma occurred. All cases were treated with appropriate revision of the surgical cavity in the abdomen and skull, respectively. Hydrocephalus was the only long-term complication observed. Two different patients, who underwent a resection of meningioma through a frontoorbito-temporal-zygomatic approach and a subfrontal approach, developed hydrocephalus after 7 months and 1 year. A ventriculoperitoneal shunt was implanted in both cases with resolution of hydrocephalus. No adhesion was observed between the brain and the autologous fat after reoperation for recurrence of some extraaxial tumors.
DISCUSSION
The use of autologous fat in neurosurgery appeared in the early twentieth century. The first neurosurgeon to use fat to repair a large dural defect was Harvey Cushing in 1912.[
In our study, complications were observed in 6.1% of cases. CSF leaks were described in 3.7% of cases, mainly during the transsphenoidal approach. Abdominal hemorrhage presented in 0.7% of cases. Fat necrosis and liquefaction, leading to a sterile oily transudate leaking from the wound in the abdomen, were described in 0.7% of cases. Exploration with removal of the necrotic fat was necessary in all cases. Hydrocephalus was developed in 0.7% of patients after approximately 1 year [
CSF leaks after neurosurgical procedures can occur in 0.9–42% of cases[
Different from the observations of Ahmed, we had no cases of fat liquefaction in the skull, but only in the abdomen. However, the exact cause of fat liquefaction has not yet been clearly described in the literature.[
The postoperative lipoid meningitis is a rare phenomenon because of the presence of fat in the subarachnoid space.[
The structural units of adipose tissue are fat lobules, the vascular supply of each lobule being complete and independent.[
The mechanism by which the fat aids in the sealing of dural defects is still being investigated; it is now hypothesized that mesenchymal stem cells, pluripotent stem cells known to contribute to the maintenance of the supportive connective tissue, are an important contributor.[
The criteria for determining the ideal dural substitute include prevention of CSF leaks, no increase in infection rate, minimal adhesions, minimal foreign bodies or allergic reactions, economy, ease of application, and availability.[
There are many advantages to the use of fat grafts; they are impervious to water, cause relatively little scarring, and also allow for a watertight closure of dura mater to prevent CSF leaks.[
The disadvantages of using fat grafts are; increased risk of chemical or lipoid meningitis,[
The morbidity related to the use of autologous fat grafts is extremely rare, and these grafts should be considered a safe and effective method for the dural reconstruction.[
CONCLUSIONS
The factors involved in the successful repair of dural defects are multivariable, however, they depend on the size and location of the defect, as well as on the type of repair material used. The technique of harvesting and applying fat grafts is fairly simple, although it must be performed meticulously to be effective. When possible, we suggest the additional use of fibrin glue to apply on the edges of the watertight suture in order to decrease the risk of CSF leaks. Our experience has led us to believe that the use of fat grafts presents low morbidity and mortality. Furthermore, it has several qualities that make it an ideal dural substitute; flexibility, adaptability, no reactivity, no toxicity, easy availability, low cost, direct watertight suture, and no creation of adhesions. However, a neurosurgeon should never forget the possible late or early complications related to the use of fat grafts.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgements
The authors thank Maria Silvia Marottoli for her assistance in the translation.
References
1. Barth M, Tuettenberg J, Thomé C, Weiss C, Vajkoczy P, Schmiedek P. Watertight dural closure: Is it necessary. A prospective randomized trial in patients with supratentorial craniotomies?. Neurosurgery. 2008. 63: S352-8
2. Black P. Cerebrospinal fluid leaks following spinal or posterior fossa surgery: Use of fat grafts for prevention and repair. Neurosurg Focus. 2000. 9: e4-
3. Byeon SW, Ban TH, Rhee CK. A Case of Acute Fulminant Fat Embolism Syndrome after Liposuction Surgery. Tuberc Respir Dis. 2015. 78: 423-7
4. Carvalho GA, Cervio A, Matthies C, Samii M. Subarachnoid fat dissemination after resection of a cerebellopontine angle dysontogenic cyst: Case report and review of the literature. Neurosurgery. 2000. 47: 760-3
5. Ferroli P, Acerbi F, Broggi M, Schiariti M, Albanese E, Tringali G. A novel impermeable adhesive membrane to reinforce dural closure: A preliminary retrospective study on 119 consecutive high-risk patients. World Neurosurg. 2013. 79: 551-7
6. Hwang PH, Jackler RK. Lipoid meningitis due to aseptic necrosis of a free fat graft placed during neurotologic surgery. Laryngoscope. 1996. 106: 1482-6
7. Izquierdo R, Origitano TC, al-Mefty O, Leonetti JP, Anderson DE, Reichman OH. Use of vascularized fat from the rectus abdominis myocutaneous free flap territory to seal the dura of basicranial tumor resections. Neurosurgery. 1993. 32: 192-6
8. Kumar P, Pandey AK, Kumar B, Aithal SK. Anatomical study of superficial fascia and localized fat deposits of abdomen. Indian J Plast Surg. 2011. 44: 478-83
9. Kuo JS, Hawkins C, Rutka JT, Weiss MH. A pilot study of fat allograft transplantation in immunocompetent rabbits for potential neurosurgical applications. J Neurosurg. 2011. 114: 441-5
10. Meyer J, Salamon A, Herzmann N, Adam S, Kleine HD, Matthiesen I. Isolation and differentiation potential of human mesenchymal stem cells from adipose tissue harvested by water jet-assisted liposuction. Aesthet Surg J. 2015. 35: 1030-9
11. Ozisik PA, Inci S, Soylemezoglu F, Orhan H, Ozgen T. Comparative dural closure techniques: A safety study in rats. Surg Neurol. 2006. 65: 42-7
12. Parlato C, di Nuzzo G, Luongo M, Parlato RS, Accardo M, Cuccurullo L. Use of a collagen biomatrix (TissuDura) for dura repair: A long-term neuroradiological and neuropathological evaluation. Acta Neurochir. 2011. 153: 142-7
13. Pettorini BL, Tamburrini G, Massimi L, Paternoster G, Caldarelli M, Di Rocco C. The use of a reconstituted collagen foil dura mater substitute in paediatric neurosurgical procedures—Experience in 47 patients. Br J Neurosurg. 2010. 24: 51-4
14. Ray J, D'souza AR, Chavda SV, Walsh AR, Irving RM. Dissemination of fat in CSF: A common finding following translabyrinthine acoustic neuroma surgery. Clin Otolaryngol. 2005. 30: 405-8
15. Ricaurte JC, Murali R, Mandell W. Uncomplicated postoperative lipoid meningitis secondary to autologous fat graft necrosis. Clin Infect Dis. 2000. 30: 613-5
16. Ross D, Rosegay H, Pons V. Differentiation of aseptic and bacterial meningitis in postoperative neurosurgical patients. J Neurosurg. 1988. 69: 669-74
17. Sekhar LN, Mai JC. Dural repair after craniotomy and the use of dural substitutes and dural sealants. World Neurosurg. 2013. 79: 440-2
18. Smahel J. Adipose tissue in plastic surgery. Handchir Mikrochir Plast Chir. 1984. 16: 111-4
19. Sommer B, Sattler G. Current concepts of fat graft survival: Histology of aspirated adipose tissue and review of the literature. Dermatol Surg. 2000. 26: 1159-66
20. Spaziante R, de Divitiis E, Cappabianca P, Schmidek HH, Sweet WH.editors. Repair of the sella after transsphenoidal surgery. Operative Neurosurgical Techniques, Indications, Methods and Results. Philadelphia: W.B. Saunders Co; 2000. p. 398-416
21. Taha AN, Almefty R, Pravdenkova S, Al-Mefty O. Sequelae of autologous fat graft used for reconstruction in skull base surgery. World Neurosurg. 2011. 75: 692-5
22. Verheggen R, Schulte-Baumann WJ, Hahm G, Lang J, Freudenthaler S, Schaake T. A new technique of dural closure-Experience with a vicryl mesh. Acta Neurochir. 1997. 139: 1074-9
23. Zaidi HA, Pendleton C, Cohen-Gadol AA, Quinones-Hinojosa A. Harvey Cushing's repair of a dural defect after a traumatic brain injury: Novel use of a fat graft. World Neurosurg. 2011. 75: 696-9