- Departments of Spine Service, Indian Spinal Injuries Center, New Delhi, India.
- Departments of Biostatistics, Indian Spinal Injuries Center, New Delhi, India.
Correspondence Address:
Sulaiman Sath
Departments of Spine Service, Indian Spinal Injuries Center, New Delhi, India.
DOI:10.25259/SNI_242_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Kalyan Kumar Varma Kalidindi, Sulaiman Sath, Gayatri Vishwakarma, Harvinder Singh Chhabra. Magnetic resonance imaging findings in intervertebral disc herniation: Comparison of canal compromise and canal size in patients with and without cauda equina syndrome. 27-Jun-2020;11:171
How to cite this URL: Kalyan Kumar Varma Kalidindi, Sulaiman Sath, Gayatri Vishwakarma, Harvinder Singh Chhabra. Magnetic resonance imaging findings in intervertebral disc herniation: Comparison of canal compromise and canal size in patients with and without cauda equina syndrome. 27-Jun-2020;11:171. Available from: https://surgicalneurologyint.com/surgicalint-articles/10107/
Abstract
Background: Surgical decompressions are typically warranted in patients with magnetic resonance (MR) and clinical evidence of cauda equina syndromes (CESs). However, it is still unclear what MR findings best correlate with such CES. Here, we compared MR-documented canal size and level/extent of compromise in 52 patients with and 56 others without CES attributed to lumbar disc herniation.
Methods: This was a retrospective study of 52 patients with and 56 patients without CES attributed to MR- documented lumbar disc herniations (IDHs). The anteroposterior diameters of the spinal canal and the levels of maximal compression were documented and compared utilizing MR scans from both groups.
Results: The 52 patients with CES had more extensive narrowing of the canal diameters at the L4-L5 and L5- S1 levels and higher mean canal compression ratios versus 56 patients without CES. The mean percentage of compression in the CES group at L4-L5 and L5-S1 levels (70% and 67.5%, respectively) was less versus L2-L3 and L3-L4 levels (89.7% and 81.8%, respectively).
Conclusion: The 52 patients with CES due to IDH had greater canal compromise versus 56 without CES. Further, the percentage of canal compromise was less at L4-L5 and L5-S1 levels compared to other levels in patients with CES.
Keywords: Cauda equina syndrome, Diagnosis, Disc prolapse, Magnetic resonance imaging, Spinal canal
INTRODUCTION
Cauda equina syndrome (CES) is one of the few surgical emergencies in spine surgery and most surgeons consider it a reason for urgent/emergent surgical decompression.[
MATERIALS AND METHODS
This retrospective study included patients with (n = 52) or without (n = 56) CES attributed to intervertebral IDH (2015–2018). Although multiple clinical variables were studied, we focused on the MR documented canal diameter, and levels and extent of compression for both groups [
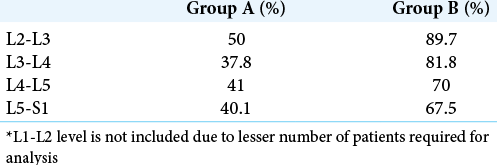
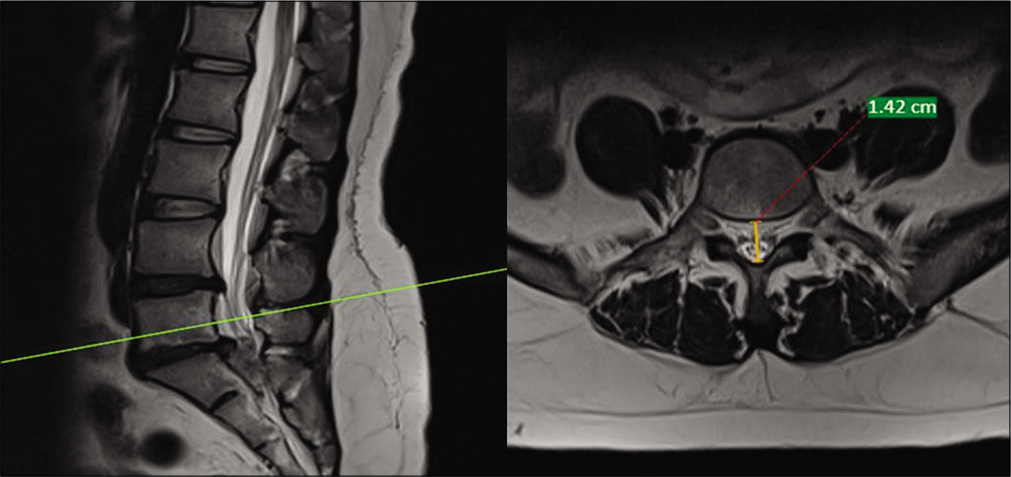
Figure 1:
T2 sagittal and axial magnetic resonance imaging cut of the lumbar spine showing the measurement of anteroposterior diameter of the spinal canal at the mid-vertebral level in a case of intervertebral disc herniation. It was measured from the midpoint of the posterior vertebral body to the anterior ligamentum flavum. Green line on left side depicts a line through L5 midvertebral level (pedicle level) in T2 sagittal magnetic resonance imaging with corresponding T2 axial cut on right side. Orange line shows maximum anterio-posterior diameter at midvertebral level (Pedicle level) in an axial magnetic resonance imaging cut with corresponding sagittal cut on left side. Red line which is a dotted line with 1.42 cm at the end shows the measurement of orange line, that is maximum anterio-posterior diameter at L5 midvertebral level (Pedicle level).
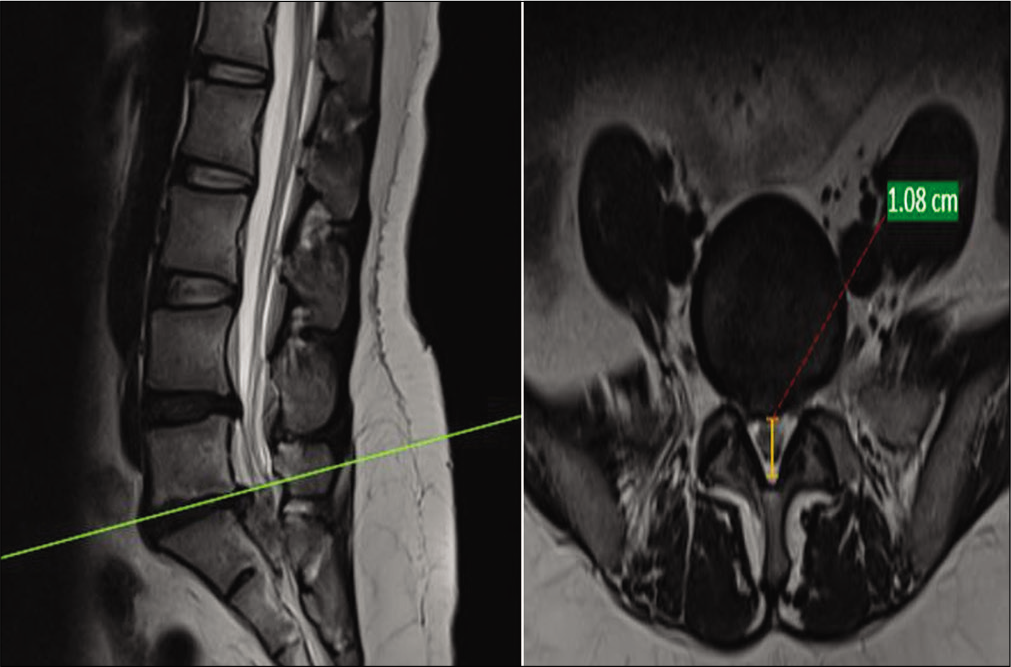
Figure 2:
T2 axial magnetic resonance imaging cuts of the lumbar spine showing the measurement of anteroposterior diameter of the spinal canal at the disc level (level of maximum compression) in a case of intervertebral disc herniation without cauda equina syndrome. It was measured from the posterior disc border to the anterior ligamentum flavum. Green line depicts cut through L5-S1 disc level in a T2 sagittal magnetic resonance imaging on left side with corresponding T2 axial cut on right side at level of maximum compression in a patient without cauda equina syndrome. Orange line shows anterio-posterior diameter in axial magnetic resonance imaging cut at level of maximum compression in a patient with L5-S1 disc herniation without cauda equina syndrome. Red dotted line with 1.08 cm at the end shows measurement of orange line.
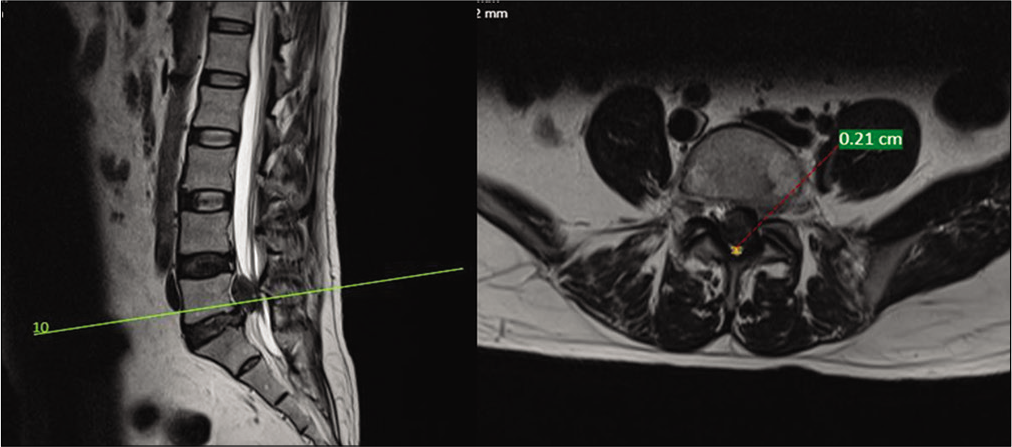
Figure 3:
T2 axial magnetic resonance imaging cuts of the lumbar spine showing the measurement of anteroposterior diameter of the spinal canal at the disc level in a case of cauda equina syndrome. Green line in a T2 sagittal magnetic resonance imaging on left side depicts at line through L5-S1 cephalic disc migration with corresponding T2 axial cut on right side at level of maximum compression in a case of cauda equina syndrome. Orange line depicts anterio-posterior diameter at level of maximum compression in case of L5-S1 cephalic disc migration with cauda equina syndrome. Red dotted line with 0.21 cm shows measurement of orange line which shows severely compromised thecal space.
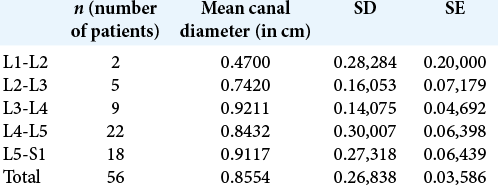
RESULTS
The details were retrieved for 56 patients (33 males and 23 females) in Group A (without CES) and compared to those for 52 patients (25 males and 27 females) in Group B (with CES). Our analysis showed that both groups were statistically matched regarding age (P > 0.1) and gender (P > 0.17). The most common level of disc herniations was L4-L5 followed by L5-S1 in both the groups. Notably, patients in Group B with CES had more motor deficits (39 vs. 28), sensory deficits (45 vs. 41), impaired perianal sensation (33 vs. 2), and impaired voluntary anal contraction (45 vs. 14) versus Group A patients [
MR studies
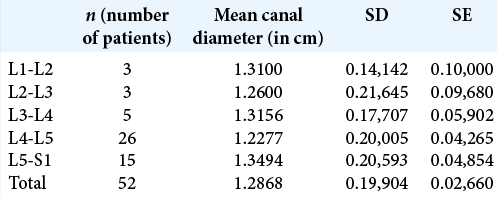
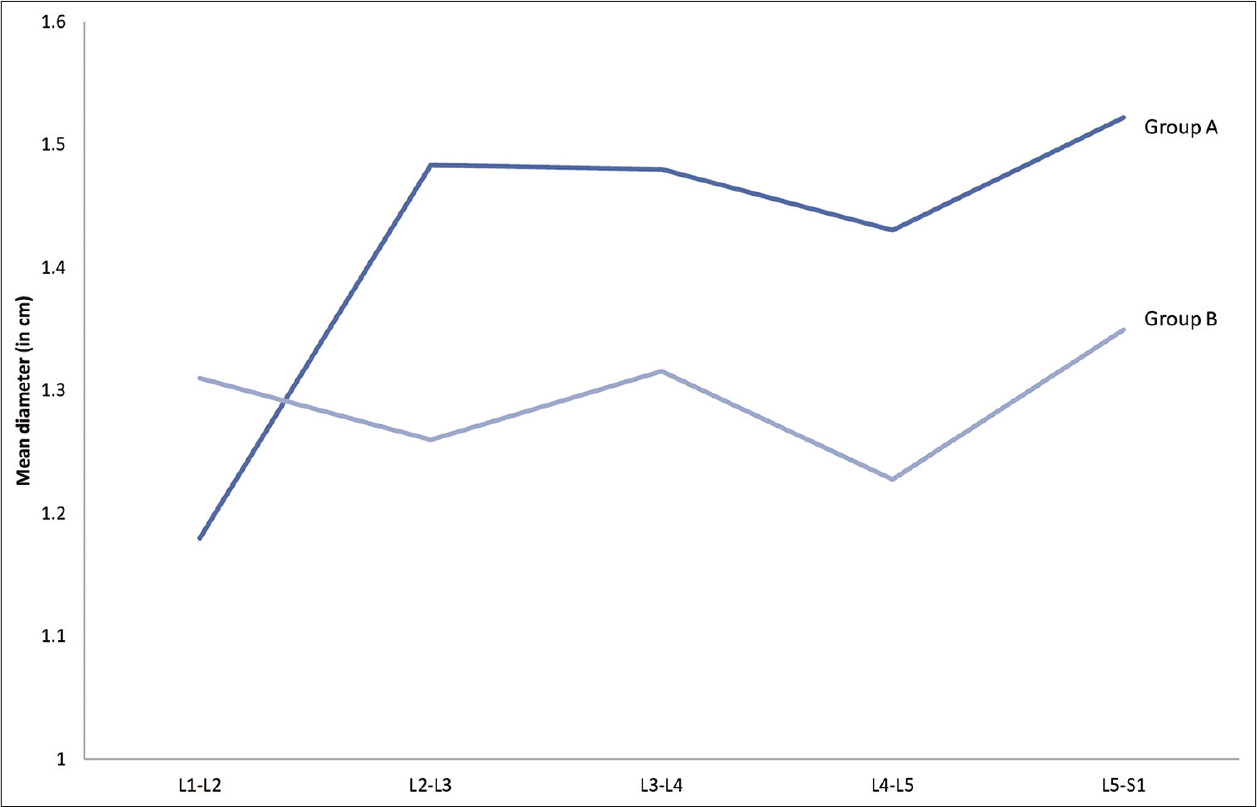
Comparison of AP canal diameters between the two groups showed no significant differences from L1-L2 (P = 0.4), L2-L3 (P = 0.39), to L3-L4 (P = 0.36) levels [
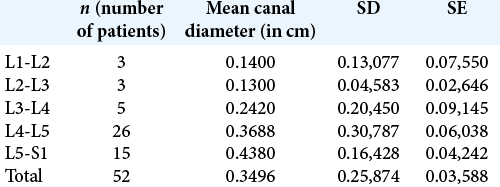
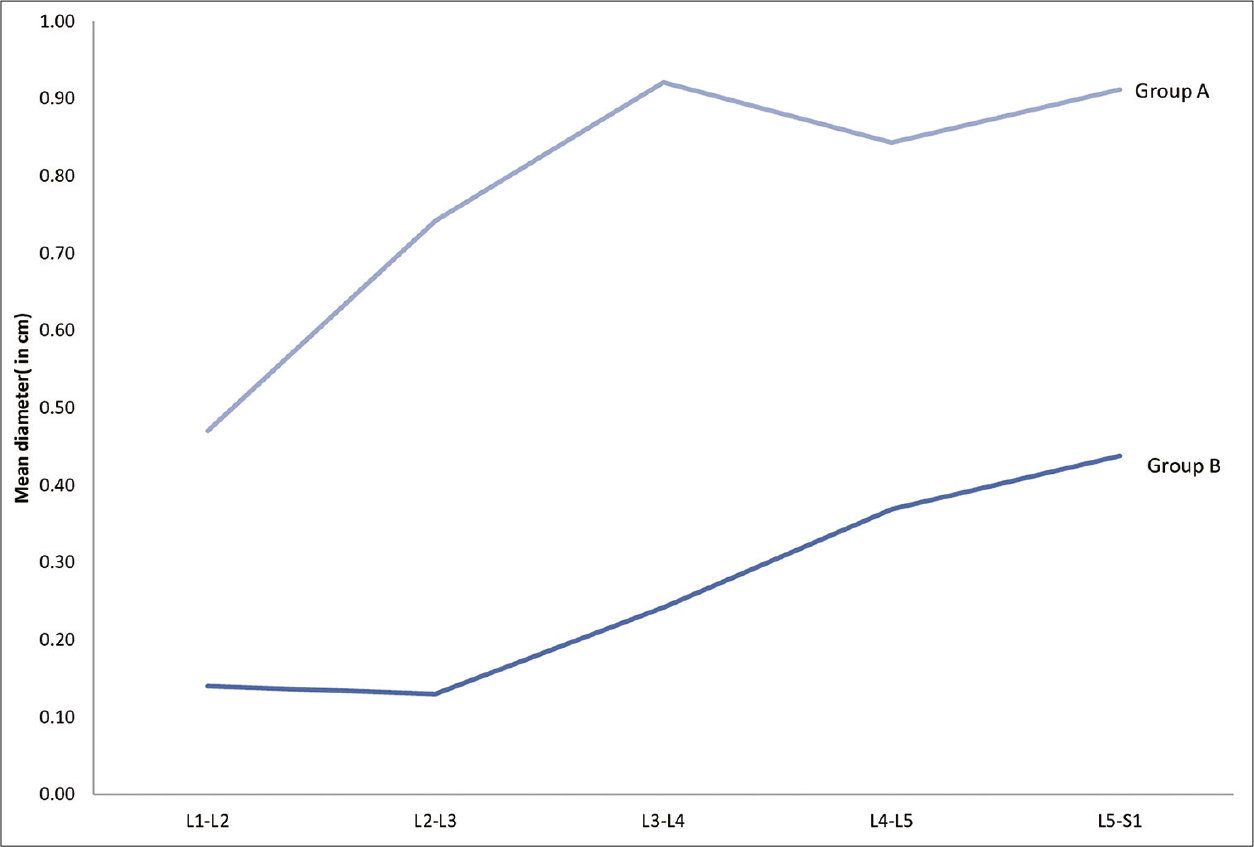
At the levels of maximal compression, Group B patients had statistically greater mean neural/canal compression versus Group A [
The mean percentage of compression in Group B versus Group A patients was greater at both the L4-L5 (70% vs. 41%) and L5-S1 (67.5% vs. 40.1%) levels [
DISCUSSION
Quantifying the amount of compression on lumbar MR’s should provide objective evidence to establish a patient’s relative risk for developing a CES attributed to a IDH. At present, there are no clear MR measurements that readily correlate with a patient’s risk for developing a CES secondary to a IDH.[
Does the percent of MR-documented canal compromise help predict whether a patient develops a CES with a IDH?
Bell et al. and Domen et al. determined that the extent of cauda equina compression best correlates with the clinical findings of a CES.[
Korse et al. also reported statistically significant differences in the normal spinal canal diameters between patients with versus those without CES.[
Lumbar disc-related canal compression on lumbar MR best correlated with clinical CES
Greater thecal sac compression was seen on 52 lumbar MR scans of patients clinically presenting with CES due to IDH versus 56 patients with lumbar discs without CES. Knowing the mean MR-documented compression at the lower lumbar levels can help identify those patients with IDH at greater risk for developing CES warranting early surgical intervention.
CONCLUSION
Patients with L4-L5 and L5-S1 IDH presenting with CES have greater MR-documented preoperative canal compromise (Group B) versus those with IDH without CES and lesser canal compromise (Group A).
Declaration of patient consent
Patient’s consent not obtained as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Balasubramanian K, Kalsi P, Greenough CG, Seetharam MP. Reliability of clinical assessment in diagnosing cauda equina syndrome. Br J Neurosurg. 2010. 24: 383-6
2. Bell DA, Collie D, Statham PF. Cauda equina syndrome: What is the correlation between clinical assessment and MRI scanning?. Br J Neurosurg. 2007. 21: 201-3
3. Domen PM, Hofman PA, van Santbrink H, Weber WE. Predictive value of clinical characteristics in patients with suspected cauda equina syndrome. Eur J Neurol. 2009. 16: 416-9
4. Fairbank J, Hashimoto R, Dailey A, Patel AA, Dettori JR. Does patient history and physical examination predict MRI proven cauda equina syndrome?. Evid Based Spine Care J. 2011. 2: 27-33
5. Kalidindi KK, Chhabra HS, Suman D, Mannem A, Bhat MR. Cauda equina syndrome: False-positive diagnosis of neurogenic bladder can be reduced by multichannel urodynamic study. Eur Spine J. 2020. 29: 1236-47
6. Korse NS, Kruit MC, Peul WC, Vleggeert-Lankamp CL. Lumbar spinal canal MRI diameter is smaller in herniated disc cauda equina syndrome patients. PLoS One. 2017. 12: e0186148-
7. Qureshi A, Sell P. Cauda equina syndrome treated by surgical decompression: The influence of timing on surgical outcome. Eur Spine J. 2007. 16: 2143-51