- Department of Stereotactic and Functional Neurosurgery, University Hospital of Cologne, Cologne, Germany,
- Department of Neurosurgery Maastricht University Medical Center, Maastricht, Limburg, Netherlands,
- Department of Radiology and Nuclear Medicine, Maastricht University Medical Center, Maastricht, Limburg, Netherlands,
- Department of Nuclear Medicine, University Hospital RWTH Aachen, Aachen, Germany,
- Schoool for Mental Health and Neuroscience, Maastricht University, Maastricht, Limburg, Netherlands.
Correspondence Address:
Pablo Andrade
Department of Neurosurgery Maastricht University Medical Center, Maastricht, Limburg, Netherlands,
Schoool for Mental Health and Neuroscience, Maastricht University, Maastricht, Limburg, Netherlands.
DOI:10.25259/SNI_609_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Pablo Andrade1, Jasper van Aalst2, Matthias Bauwens3, Andreas Vogg4, Marinus J. van Kroonenburgh3, Felix M. Mottaghy3,4, Onno P. Teernstra2, Govert Hoogland2,5. Radionuclide tumor necrosis factor-alpha activity in herniated lumbar disc correlates with severe leg pain. 15-Oct-2020;11:344
How to cite this URL: Pablo Andrade1, Jasper van Aalst2, Matthias Bauwens3, Andreas Vogg4, Marinus J. van Kroonenburgh3, Felix M. Mottaghy3,4, Onno P. Teernstra2, Govert Hoogland2,5. Radionuclide tumor necrosis factor-alpha activity in herniated lumbar disc correlates with severe leg pain. 15-Oct-2020;11:344. Available from: https://surgicalneurologyint.com/surgicalint-articles/10331/
Abstract
Background: Lumbar disc herniation is often associated with an inflammatory process. In this context, inflammation has been considered a key factor in the modulation of pain. Here, we present a case of inflammatory activity directly documented in a patient with a lumbar disc herniation.
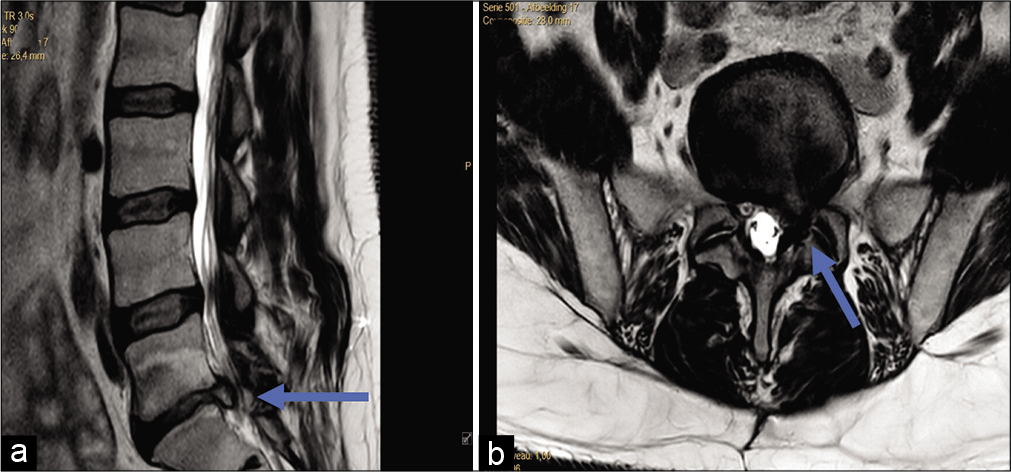
Case Description: A 49-year-old male presented with progressive low back pain and left-sided S1 radiculopathy, without a focal neurological deficit. The lumbar MR revealed a prominent herniated disc at the L5-S1 level, with compression of the left S1 root. The patient underwent a L5-S1 discectomy using a standard interlaminar approach. Although initially he was pain free, he required three additional operations to address recurrent pain complaints. As research indicates that local inflammation contributes to neuropathic pain, we had the patient undergoes single-photon emission computed tomography (SPECT) imaging using technetium-99m-labeled-infliximab (an anti-tumor necrosis factor [TNF]-alpha monoclonal antibody) before a proposed fourth operation. The SPECT study documented a strong signal at the site of the herniated disc, thus confirming the diagnosis of a pro-inflammatory process involving the S1 nerve root. Nine months after the fourth operation, the patient was pain free. Of interest, the second SPECT study in the now asymptomatic patient demonstrated no detectable/ residual signal at the operative/disc site.
Conclusion:
Keywords: Chronic pain, Disc herniation, Infliximab, Low back pain, Technetium-99m, Tumor necrosis factor-alpha
INTRODUCTION
Several preclinical/clinical studies have shown the nociceptive action of pro-inflammatory cytokines on nervous tissue reflecting how inflammation plays a role in the modulation of pain.[2,4-7] We previously reported that tumor necrosis factor (TNF)-alpha levels, present in biopsies from operated herniated lumbar discs, helped predict outcomes/postoperative pain scores.[1,2] Here, we describe how in vivo inflammatory activity documented utilizing single- photon emission computed tomography (SPECT) imaging (i.e., technetium-99m-labeled-infliximab) could be correlated with TNF-alpha levels before and after lumbar disc surgery.
CASE DESCRIPTION
A 49-year-old male presented with progressive low back pain and left S1 radiculopathy in the absence of a focal neurological deficit. The MRI scan revealed a large left-sided disc herniation at the L5-S1 level that markedly compressed the S1 root. Following a bilateral interlaminar discectomy at L5-S1, he was pain free. However, 2 months postoperatively, the patient recurred in the same distribution. The new MRI scan showed a small residual left-sided L5-S1 disc herniation. He underwent discectomy again but only on the left side. He was well for 5 years, at which point lower extremity sciatica recurred in the same left-sided S1 distribution. The MRI scan now revealed a new large herniated disc again at the same location. A third discectomy was performed, after which symptoms resolved. However, 3 months later, he again developed left S1 radiculopathy, where a new herniated disc was revealed at the same level was [
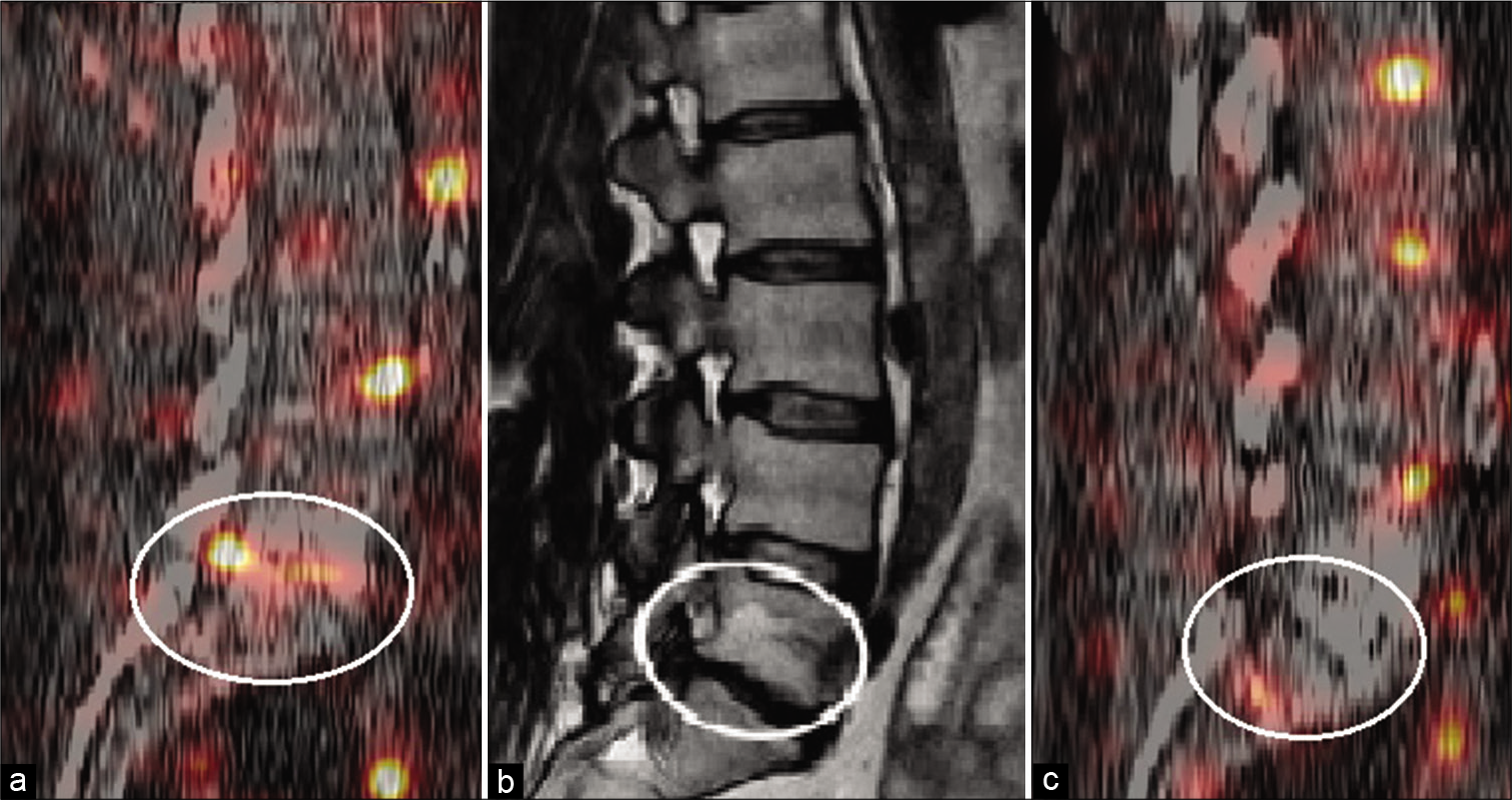
Figure 2:
(a) Positive distribution of technetium-99m-labeled-infliximab at the intervertebral space and the herniated disc in the spinal canal before surgery. (b) Preoperative MRI showing the herniated disc at the L5/S1 level with intraforaminal sequester. (c) Negative distribution of technetium-99m-labeled-infliximab at the intervertebral at the L5/S1 level or the spinal canal after surgery.
DISCUSSION
Patients with different forms of chronic pain show increased levels of local inflammation.[4,5] Here, the SPECT scan revealed a pro-inflammatory cytokine (TNF-alpha) located specifically at the symptomatic left S1 site.[1] Furthermore, we documented that the patient’s resolution of pain correlated with the absence of this marker on the postoperative SPECT scan.
If these results were to be confirmed in larger cohorts, SPECT scans could become another tool to reveal where surgery is indicated, and when it has been effective.
CONCLUSION
With SPECT nuclear imaging utilizing technetium-99m-labeled-infliximab, we were able to identify a focus of inflammation at the site of a recurrent lumbar disc herniation on the left at the L5-S1 level. When the pain disappeared, so did the SPECT levels of TNF-alpha.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Andrade P, Visser-Vandewalle V, Philippens M, Daemen MA, Steinbusch HW, Buurman WA. Tumor necrosis factor-α levels correlate with postoperative pain severity in lumbar disc hernia patients: Opposite clinical effects between tumor necrosis factor receptor 1 and 2. Pain. 2011. 152: 2645-52
2. Andrade P, Hoogland G, Garcia MA, Steinbusch HW, Daemen MA, Visser-Vandewalle V. Elevated IL-1β and IL-6 levels in lumbar herniated discs in patients with sciatic pain. Eur Spine J. 2013. 22: 714-20
3. D’Alessandria C, Malviya G, Viscido A, Aratari A, Maccioni F, Amato A. Use of a 99mTc labeled anti-TNFalpha monoclonal antibody in Crohn’s disease: In vitro and in vivo studies. Q J Nucl Med Mol Imaging. 2007. 51: 334-42
4. Krämer HH, Eberle T, Uçeyler N, Wagner I, Klonschinsky T, Müller LP. TNF-α in CRPS and ‘normal’ trauma--significant differences between tissue and serum. Pain. 2011. 152: 285-90
5. Langjahr M, Schubert AL, Sommer C, Üçeyler N. Increased pro-inflammatory cytokine gene expression in peripheral blood mononuclear cells of patients with polyneuropathies. J Neurol. 2018. 265: 618-27
6. Sacerdote P, Franchi S, Trovato AE, Valsecchi AE, Panerai AE, Colleoni M. Transient early expression of TNF-alpha in sciatic nerve and dorsal root ganglia in a mouse model of painful peripheral neuropathy. Neurosci Lett. 2008. 436: 210-3
7. Youn DH, Wang H, Jeong SJ. Exogenous tumor necrosis factor-alpha rapidly alters synaptic and sensory transmission in the adult rat spinal cord dorsal horn. J Neurosci Res. 2008. 86: 2867-75