- Pars Advanced and Minimally Invasive Medical Manners Research Center, Pars Hospital, Iran University of Medical Sciences, Tehran, Iran,
- Department of Neurosurgery, Loghman Hakim Hospital, Shaheed Beheshti University of Medical Sciences, Tehran, Iran.
Correspondence Address:
Abolfazl Rahimizadeh
Department of Neurosurgery, Loghman Hakim Hospital, Shaheed Beheshti University of Medical Sciences, Tehran, Iran.
DOI:10.25259/SNI_540_2019
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Abolfazl Rahimizadeh, Guive Sharifi. Spinal intramedullary epidermoid cysts: Three case presentations and literature review. 07-Feb-2020;11:17
How to cite this URL: Abolfazl Rahimizadeh, Guive Sharifi. Spinal intramedullary epidermoid cysts: Three case presentations and literature review. 07-Feb-2020;11:17. Available from: https://surgicalneurologyint.com/surgicalint-articles/9866/
Abstract
Background: True intramedullary epidermoid cysts (IECs) not associated with congenital anomalies or previous spinal procedures are extremely rare. In a review of the literature since 1992, only 29 such cases have been reported. Here, we add three new cases in this category.
Case Description: Three adults presented with spastic paraparesis attributed to thoracic IECs. Gross total microsurgical removal was achieved in two cases, while one case was a partial resection due to capsular adherence to the cord. In all three cases, patients sustained complete recoveries of neurological function and remained symptom free for an average of 5 years follow-up.
Conclusion: IECs are rare lesions; here, the three located in the thoracic spine, contributed to slow, progressive spastic paraparesis with/without incontinence, and resolved following total (2 patients) and partial (1 patient) resection.
Keywords: Epidermoid cyst, Intramedullary tumor, Paraparesis, Spinal cord, Thoracic spine
INTRODUCTION
Spinal epidermoid tumors are rare benign lesions, representing < 1% of all intraspinal tumors; most are intradural and extramedullary in location.[
CASE DESCRIPTION
Here, we present three cases of true IEC and review the literature concerning their overall clinical/radiographic presentation and surgical management.
Case 1
A 40-year-old female presented with a progressive spastic paraparesis and a sensory level bilaterally at T5 over 1 year (e.g. American Spinal Injury Association [ASIA] D classification). The magnetic resonance imaging (MRI) revealed a well-circumscribed intramedullary tumor at the T3-T4 level that was hypointense on T1 weighted and hyperintense on T2-weighted sequences [
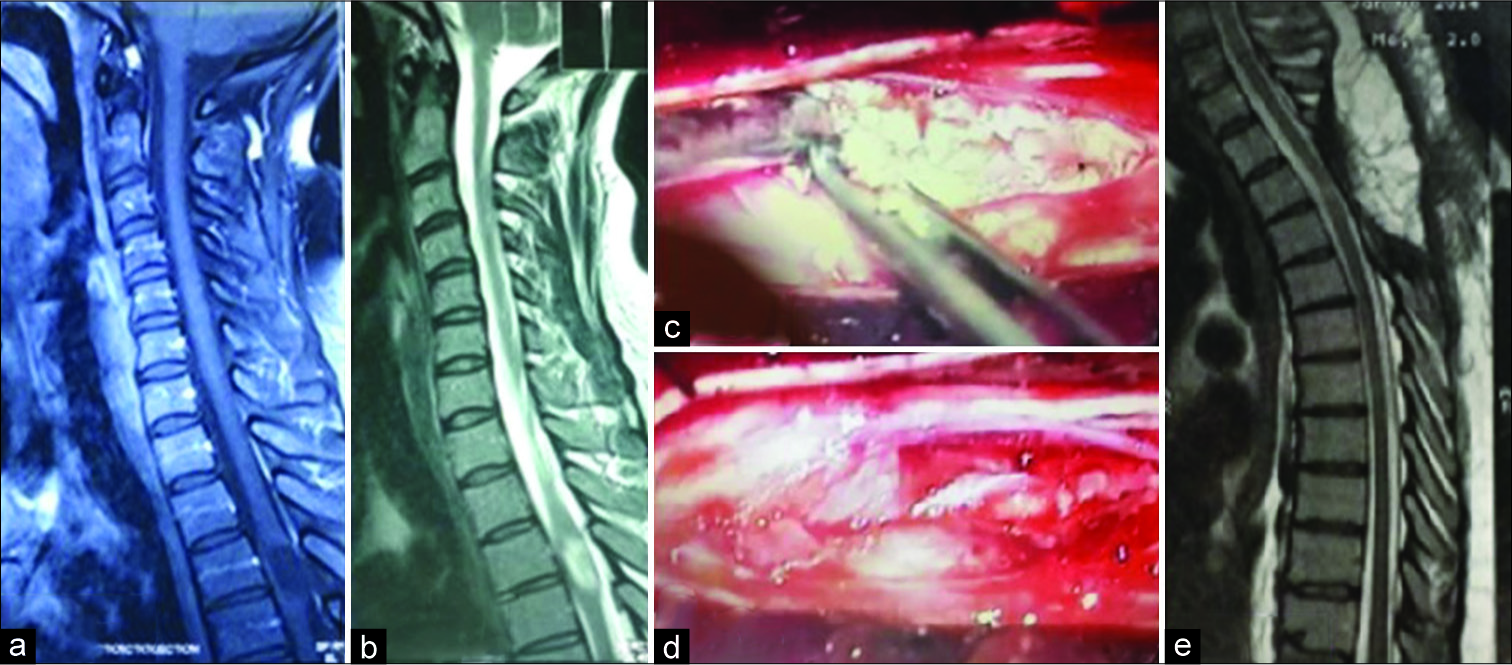
Figure 1:
(a) Cervicothoracic T1-weighted magnetic resonance imaging (MRI) a hypointense tumor at T3-T4 level, (b) in T2-weighted MRI the mass is hyperintense, (c) intraoperative photograph; a white avascular tumor inside the cord, (d) after total removal, (e) postoperative T2-weighted MRI which is clear from residue.
Case 2
Progressively over a 3-year period, a 37-year-old female also presented with a spastic paraparesis and paresthesia/sensory level T5 bilaterally (ASIA C classification). The cervicothoracic sagittal MRI showed an intramedullary mass at the T3-T4 level; there was a mixture of hypo and hyperintensities on the T1- and T2-weighted images [
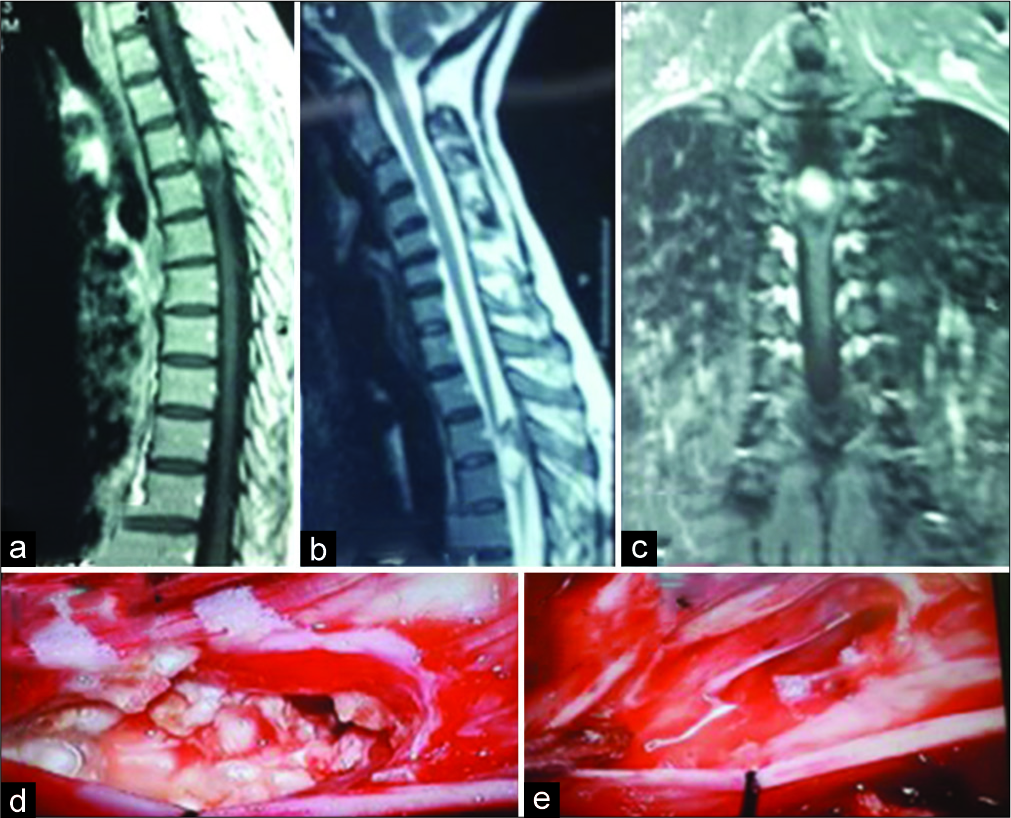
Figure 2:
(a) Cervicothoracic T1-weighted sagittal magnetic resonance imaging (MRI) shows a mixed hypo-hyperintense mass at T3-T4 level, (b) in T2-weighted image, the mass is also hypo-hyperintense which is not usual in intramedullary epidermoid cysts, (c) but in fat-suppressed MRI the whole of the tumor is hyperintense, (d) intraoperative photograph; a milky white tumor is demonstrated after midline myelotomy, (e) after total removal of the mass.
Case 3
A 41-year-old male who also was paraparetic, had an intramedullary IEC at the T3-T4 level that was similarly grossly totally removed, resulting the in the patient’s eventual full and sustained recovery at 8 years follow-up (ASIA Class E) [
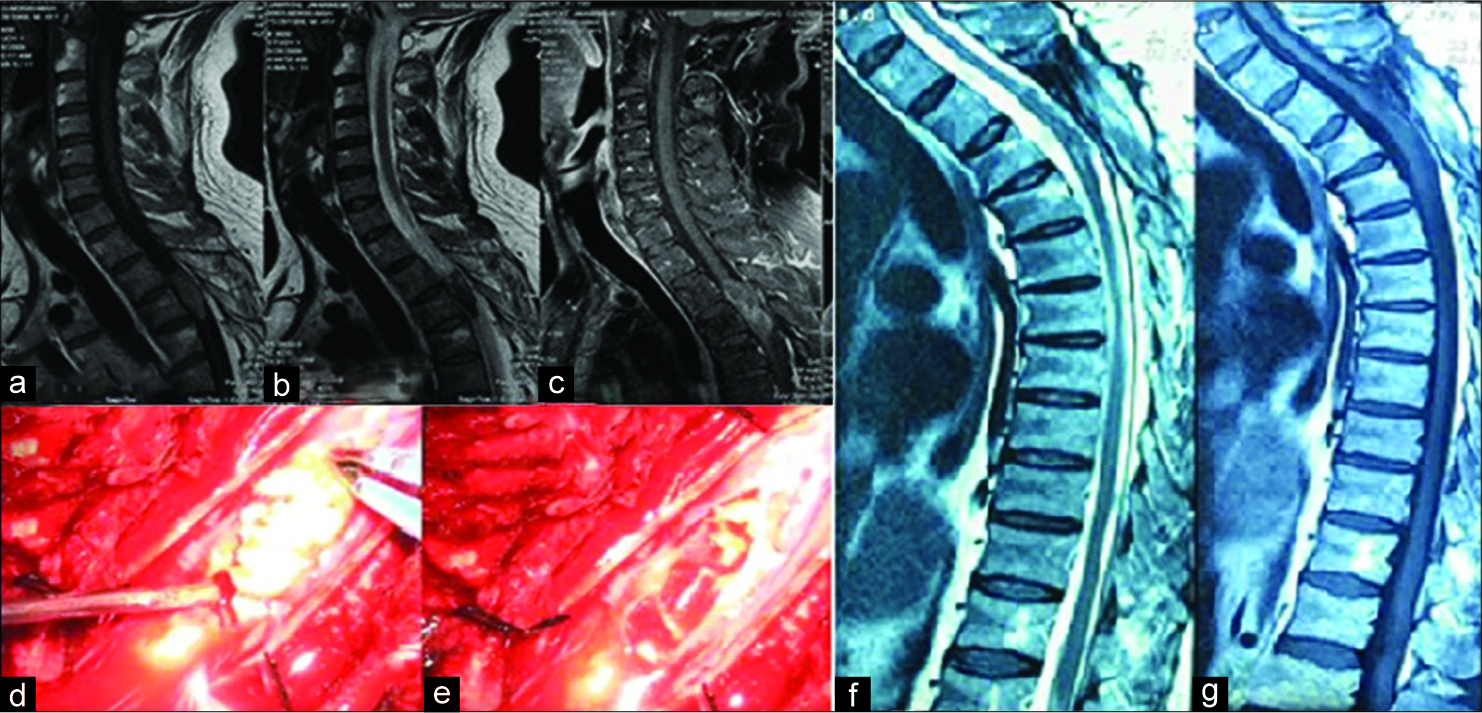
Figure 3:
(a) Cervicothoracic T1-weighted magnetic resonance imaging (MRI) the tumor is isointense, (b) in T2-weighted mage it is hypointense which is unusual for intramedullary epidermoid cysts, (c) but in fat-suppressed MRI the hyperintense mass is compatible with epidermoid, (d) intraoperative photograph shows the characteristic features of and epidermoid cyst, (e) after total removal, (f) T1-weighted MRI at 10-year follow-up shows neither residue nor recurrence, (g) T2-weighted image also is clear.
DISCUSSION
In 1992, Roux et al. reviewed all true IECs within medical literature and could find 47 cases including a case of their own.[
MRI characteristically demonstrates a nonhomogeneous, hypodense, or isointense mass on T1-weighted MRI scans attributed to the variable amounts of the lipids and proteins within the tumor. They are hyperintense on T2-weighted image due to the keratin content of the cyst.[
Surgical management
Surgical removal is the optimal management of IECs. At surgery, following midline myelotomy, the tumor is typically well demarcated; with a smooth, hypovascular, and capsule that is readily removed in over half of the patients. The other half may exhibit dense adhesions of the capsule to the cord, precluding total excision.[
CONCLUSION
IECs, most often found in the thoracic spine, typically contribute to progressive paraparesis. MR studies typically demonstrate well-circumscribed lesions that may be readily totally or partially excised, resulting in marked postoperative neurological recovery.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Agarwal A, Bhake A, Kakani A. Cervical intramedullary epidermoid cyst with liquid contents. Asian Spine J. 2011. 5: 59-63
2. Agrawal M, Gour SS, Borkar SA. Unusual calcification in intramedullary epidermoid cyst. World Neurosurg. 2019. 126: 99-100
3. Alvord EC. Growth rates of epidermoid tumors. Ann Neurol. 1977. 2: 367-70
4. Amato VG, Assietti R, Arienta C. Intramedullary epidermoid cyst: Preoperative diagnosis and surgical management after MRI introduction. Case report and updating of the literature. J Neurosurg Sci. 2002. 46: 122-6
5. Babayev R, Abbasov B, Ekşi MŞ. Thoracic intramedullary epidermoid cyst-timely fashion diagnosis and treatment. Childs Nerv Syst. 2015. 31: 793-6
6. Brohi SR, Qureshi SM, Rajput SS, Bhatti NK. Thoracic intramedullary epidermoid with paraplegia for 12 years. J Coll Physicians Surg Pak. 2010. 20: 135-6
7. Cataltepe O, Berker M, Akalan N. A giant intramedullary spinal epidermoid cyst of the cervicothoracic region. Pediatr Neurosurg. 2004. 40: 120-3
8. Chandra P, Manjari T, Devi B, Chandramouli B, Srikanth S, Shankar S. Intramedullary spinal epidermoid cyst. Neurol India. 2000. 48: 75-
9. Cincu R, Lázaro JF, Liesa JL, Callizo JR. Dorsal intramedullary spinal epidermoid cysts: Report of two cases and review of literature. Indian J Orthop. 2007. 41: 395-7
10. Elsebaey ME, Elgohary M. Thoracic spinal intradural intramedullary epidermoid cyst: Case report. Egypt Spine J. 2017. 22: 50-6
11. Fazio MG, Kil AM, Rooks VJ, Biega TJ. Diffusion-weighted magnetic resonance imaging of an intramedullary epidermoid cyst with dorsal dermal sinus tract in a toddler. Case Rep Radiol. 2013. 2013: 878713-
12. Fereydoonian NA, Bakhti S, Fereshtehnejad SM, Tabibkhooei AR. Intramedullary thoracic spine epidermoid cyst with myelopathic presentations: A report of a rare case. Clin Neurol Neurosurg. 2013. 115: 841-3
13. Ferrara P, Costa S, Rigante D, Mule A, D’Aleo C, Pulitanò S. Intramedullary epidermoid cyst presenting with abnormal urological manifestations. Spinal Cord. 2003. 41: 645-8
14. Gonzalvo A, Hall N, McMahon JH, Fabinyi GC. Intramedullary spinal epidermoid cyst of the upper thoracic region. J Clin Neurosci. 2009. 16: 142-4
15. Gotecha S, Ranade D, Sharma S, Punia P, Kotecha M. Giant intradural intramedullary epidermoid cyst Report of two cases with varied presentations. Asian J Neurosurg. 2014. 9: 244-
16. Halcrow SJ, Crawford PJ, Craft AW. Epidermoid spinal cord tumour after lumbar puncture. Arch Dis Child. 1985. 60: 978-9
17. Jadhav RN, Khan GM, Palande DA. Intramedullary epidermoid cyst in cervicodorsal spinal cord. J Neurosurg. 1999. 90: 161-
18. Jain N, Narayan S, Patil H, Songara A. Epidermoid cyst of the thoracic spine: A rare case. J Spinal Surg. 2016. 3: 59-62
19. Kukreja K, Manzano G, Ragheb J, Medina LS. Differentiation between pediatric spinal arachnoid and epidermoid-dermoid cysts: Is diffusion-weighted MRI useful?. Pediatr Radiol. 2007. 37: 556-60
20. Kumar A, Singh P, Jain P, Badole CM. Intramedullary spinal epidermoid cyst of the cervicodorsal region: A rare entity. J Pediatr Neurosci. 2010. 5: 49-51
21. Kumar R, Singh V. Intramedullary mass lesion of the spinal cord in children of a developing milieu. Pediatr Neurosurg. 2004. 40: 16-22
22. Lai SW, Chan WP, Chen CY, Chien JC, Chu JS, Chiu WT. MRI of epidermoid cyst of the conus medullaris. Spinal Cord. 2005. 43: 320-3
23. Lee JH, Shin JJ, Hwang YS, Kim TH, Shin HS, Park SK. Intramedullary epidermoid cyst in thoracolumbar junctiont: A case report. Korean J Spine. 2008. 5: 219-
24. Manno NJ, Uihlein A, Kernohan JW. Intraspinal epidermoids. J Neurosurg. 1962. 19: 754-65
25. Mishra AM, Prabhuraj AR, Pruthi N, Rao S. Adult intramedullary epidermoid cyst without spinal dysraphism: A case report. Surg Neurol Int. 2018. 9: 122-
26. Moon MS, Shim YS, Sun DH. Epidermoid cyst of the conus medullaris and cauda equina a case report. J Korean Soc Spine Surg. 2006. 13: 142-6
27. Musali SR, Mohammed I, Gollapudi PR, Maley SK. Dorsal spinal intradural intramedullary epidermoid cyst: A rare case report and review of literature. J Neurosci Rural Pract. 2019. 10: 352-4
28. Ogden AT, Khandji AG, McCormick PC, Kaiser MG. Intramedullary inclusion cysts of the cervicothoracic junction. Report of two cases in adults and review of the literature. J Neurosurg Spine. 2007. 7: 236-42
29. Ohara T, Maki S, Furuya T, Inada T, Kamiya K, Ota M. Elderly onset intramedullary epidermoid cyst in the conus medullaris: A case report. J Med Case Rep. 2015. 9: 7-
30. Rahimizadeh A, Sharifi G. Anterior cervical arachnoid cyst. Asian Spine J. 2013. 7: 119-25
31. Rahimizadeh A, Soufiani H. Intramedullary arachnoid cyst in association with cervical spondylosis: Case report. Spine J. 2013. 13: e21-5
32. Rahimizadeh A, Soufiani H. Upper cervical intermedullary lipoma with extension into the cistern magna in an elderly: Report of a case and review of the literature. World Spinal Column J. 2011. 2: 114-8
33. Rocha Júnior MA, de Carvalho GT, Faria MP, Faglioni W Jr, de Souza AA. Intramedullary epidermoid tumor: Case report. Arq Neuropsiquiatr. 2003. 61: 867-9
34. Roux A, Mercier C, Larbrisseau A, Dube LJ, Dupuis C, Del Carpio R. Intramedullary epidermoid cysts of the spinal cord. Case report. J Neurosurg. 1992. 76: 528-33
35. Scholz M, Märzheuser-Brands S, Gottschalk J, Böck JC, Lanksch WR. Intramedullary epidermoid cyst. A case report. Neurosurg Rev. 1994. 17: 89-93
36. Singh K, Pandey S, Gupta PK, Sharma V, Santhosh D, Ghosh A. Acquired dorsal intraspinal epidermoid cyst in an adult female. Surg Neurol Int. 2016. 7: S67-9
37. Yoon SH, Jahng TA, Kim KJ, Chung CK, Kim HJ. An extensive intramedullary epidermoid cyst with a longstanding history of paraplegia: A case report. J Neurol Surg A Cent Eur Neurosurg. 2013. 74: e1-3