- Department of Neurosurgery, Miguel Servet University Hospital, Zaragoza, Spain.
DOI:10.25259/SNI_166_2021
Copyright: © 2021 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Laura Beatriz López López, Jesús Adrián Moles Herbera, Silvia Vázquez Sufuentes, David Fustero de Miguel, Amanda Avedillo Ruidíaz, Javier Orduna Martínez, Juan Casado Pellejero. Supracerebellar transtentorial approach for left parahippocampal cavernous malformation. 10-May-2021;12:216
How to cite this URL: Laura Beatriz López López, Jesús Adrián Moles Herbera, Silvia Vázquez Sufuentes, David Fustero de Miguel, Amanda Avedillo Ruidíaz, Javier Orduna Martínez, Juan Casado Pellejero. Supracerebellar transtentorial approach for left parahippocampal cavernous malformation. 10-May-2021;12:216. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=10799
Abstract
Background: Lesions in the temporomesial region can be reached by various approaches: subtemporal, transsylvian, transcortical, interhemispheric parieto-occipital, or supracerebellar transtentorial (SCTT). The choice varies according to the characteristics of the lesion and neighboring structures.
Case Description: In this clinical case, it is presented a 56-year-old man with long-term evolution of drug-resistant epilepsy secondary to a cavernoma in the left parahippocampal gyrus. After assessing the lesion, it was decided a SCTT approach for its resection in a semi-sitting position, to avoid language disorders or visual damage. The surgery was uneventful and the patient did not present epileptic seizures during 6-month follow-up.
Conclusion: Performing a SCTT is safe and feasible option for resection of lesions located in the basal temporomesial region without causing damage to neighboring structures, especially those located in the middle and posterior two-thirds of temporal region.
Keywords: Cavernoma, Epilepsy, Supracerebellar, Transtentorial
INTRODUCTION
Mediobasal temporal region can be approached by multiple routes. The most appropriate one will be chosen depending on the features of the lesion, location, and relationship with neighboring structures. In neurosurgical practice, subtemporal, transtemporal, transsylvian, or transcortical temporal approaches are frequently used, especially to access the anterior two-thirds of the temporomesial region. For the posterior one-third, other techniques are commonly used, such as the parietooccipital interhemispheric, or less frequently the supracerebellar transtentorial approach (SCTT). For huge lesions or those covering the entire temporal lobe, a combination of several approaches is usual, either in the same surgical time or deferred.
In the following case, we chose a SCTT corridor in semi-sitting position, which was first described by Voigt and Yasargil in 1976 for the resection of a right hippocampal cavernoma.[
CASE REPORT
We present a 56-year-old male with no drug allergies and a history of dyslipidemia and structural partial epilepsy since the age of 27, who was followed up by a neurologist.
The seizures consisted of absence-type focal seizures with altered consciousness for 2–3 min with postcritical period with slurred speech and bradypsychia. The patient did not present auras or any other type of seizures. Their frequency was 6–8 per month and was triggered by stress and work situations.
Since the diagnosis, the patient had been treated with multiple antiepileptic drugs without success, either because of the appearance of adverse effects or their ineffectiveness in seizure control.
At the time of the surgery, the patient was under treatment with levetiracetam 1000 mg/12 h, perampanel 8 mg/24 h, and 3 eslicarbazepine 800 mg tablets every 48 h.
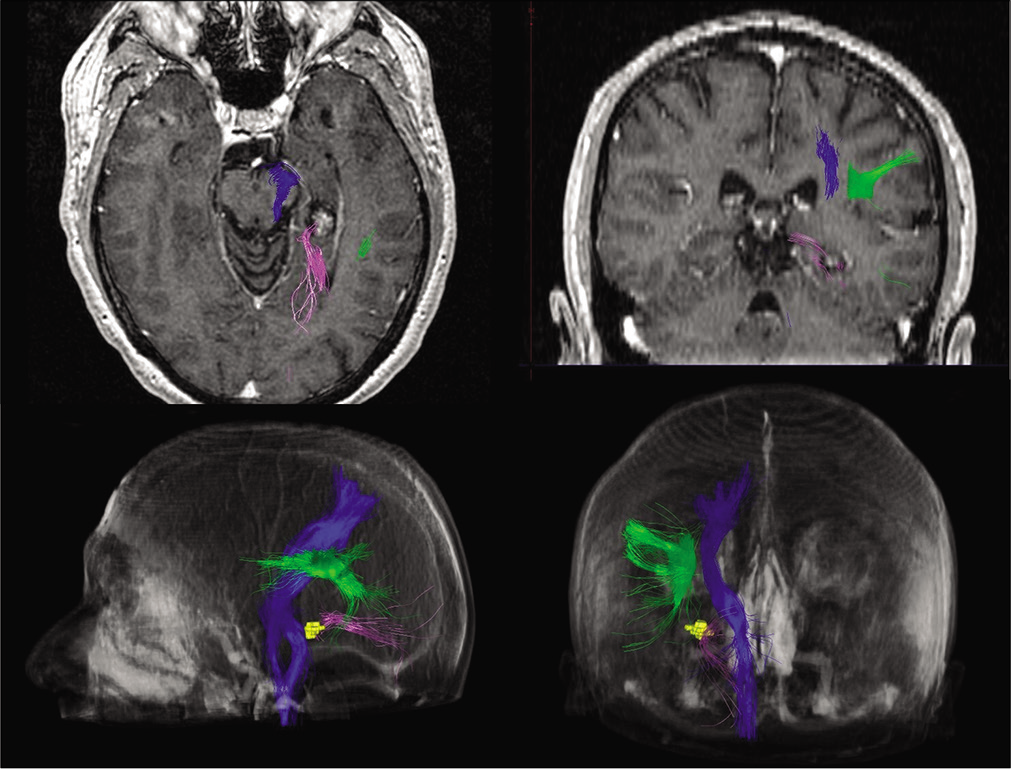
A magnetic resonance imaging showed a left temporal parahippocampal lesion suggestive of cavernous angioma with pathological activity on the left posterior temporal lobe in electroencephalogram [
Due to a diagnosis of a drug-resistant epilepsy secondary to a left parahippocampal cavernoma, the patient was referred to our department for the evaluation of surgical treatment.
Subsequently, informed consent including the use of diagnostic and intraoperative images for educational and academic purposes was obtained from the patient.
A transtentorial supracerebellar approach in semi-sitting position was chosen [
Video 1
The patient was operated in semi-sitting position with his head fixed, elevated, and flexed to expose the suboccipital region. An external lumbar drain was placed to evacuate approximately 50 cc to aid cerebral relaxation and better retraction during surgery.
A left paramedial vertical incision was made, one-third superior to the transverse sinus and two-thirds inferior. After muscle dissection, the left suboccipital craniotomy was achieved exposing the transverse sinus. The dura mater was dissected in a C shaped and lifted up to increase the corridor view and elevate the tentorium.
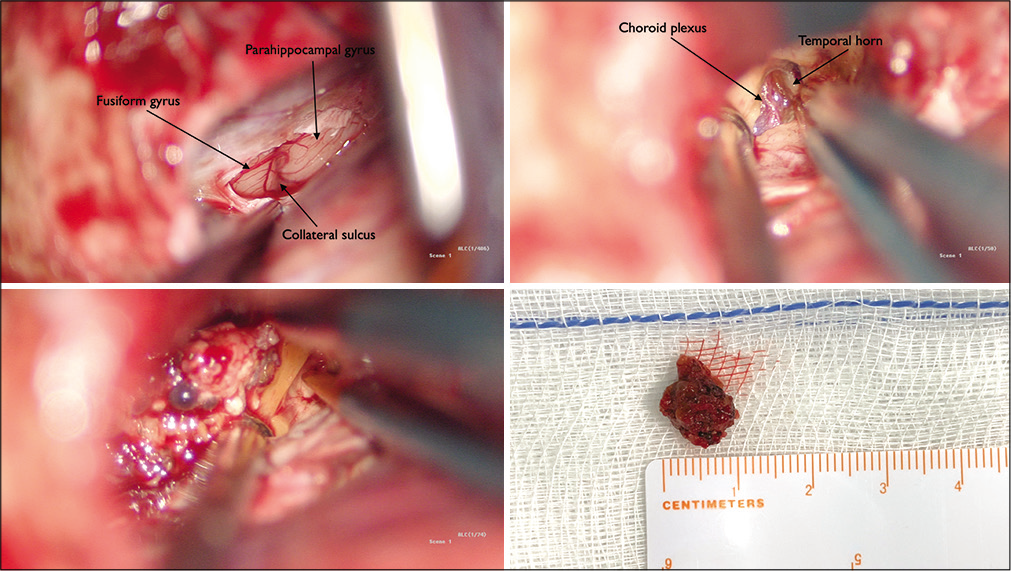
The tentorial incisura was reached preserving the bridging veins and the opening of the ambient and quadrigeminal cisterns was performed to relieve cerebral pressure avoiding the placement of retractors. Neuronavigation-guided assistance was used to execute the tentorial incision, reaching the medial temporal lobe. The fusiform and parahippocampal gyrus along with the collateral sulcus were located. After performing corticotomy in the parahippocampal gyrus with the support of neuronavigation-guided monitoring, the cavernous angioma was located [
The resection was performed without surgical or anesthetic incidents and the patient remained in the intensive care unit for 24 h.
The patient did not present any complications during the postoperative period and was discharged 4 days after surgery.
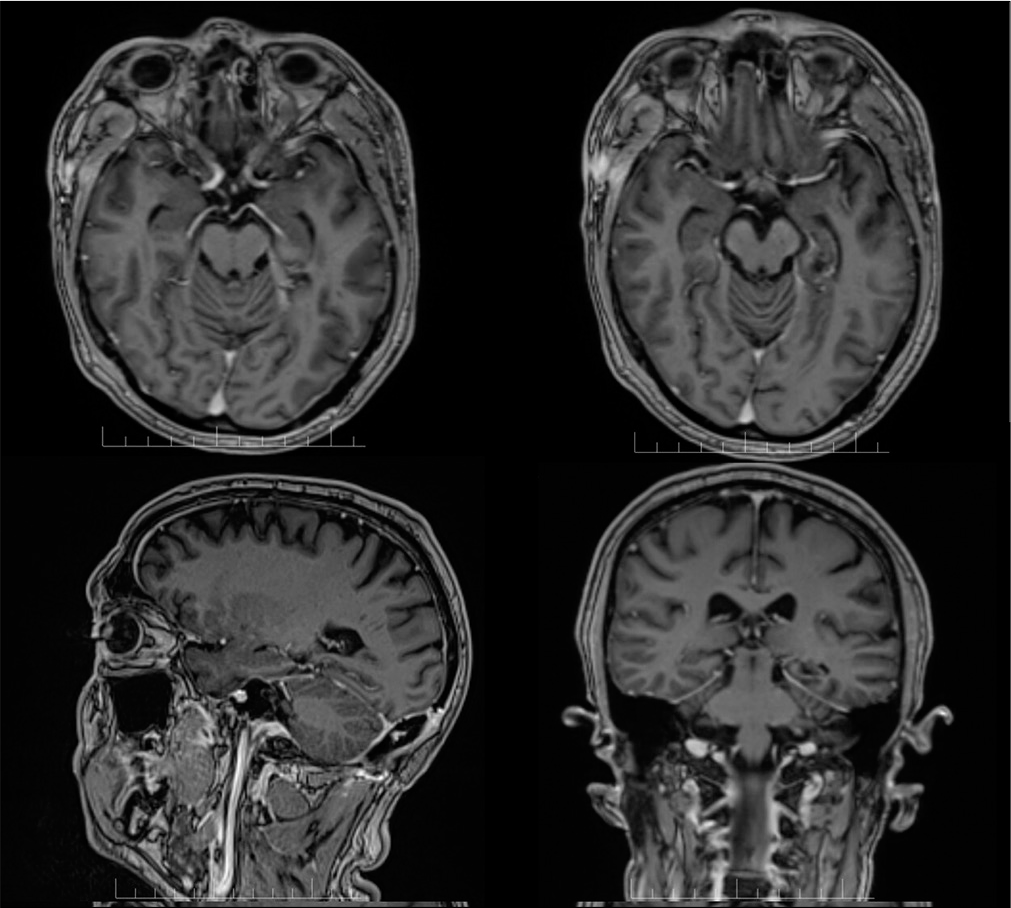
After 6-month follow-up, the patient is seizure free (Engel IA). [
DISCUSSION
Voigt and Yasargil[
In our case, SCTT approach was chosen due to the posterior and basal location of the cavernoma, in the parahippocampal gyrus of the left temporal lobe. Since it is the dominant hemisphere, SCTT avoids temporal cortex injury, which can be harmed in other approaches such as subtemporal or transtemporal.
The main disadvantage of the subtemporal approach is the retraction of the temporal lobe, which can lead to parenchymal damage or venous infarction due to compression of Labbé’s vein, complications that are more noticeable in the dominant hemisphere. On the other hand, the transcortical approach implies the transgression of the parenchyma to reach the medial part of temporal lobe, compromising optic radiations.
The transsylvian approach may lead to insular or optic radiations lesions. Other approaches reported in the literature are the parietooccipital interhemispheric approach, which requires retraction of occipital lobe and may cause visual disturbances, or SCTT. The main advantages of the latter are the direct access to the temporal basal region without retraction or disruption of the parenchyma and thus, the lower probability of language and visual disturbances. Although it may seem an approach with limited surgical field, a cadaver study by Chau et al. compares the depth, angle approach, maneuverability area, and width of the different types of approaches mentioned for temporobasal lesions of the fusiform gyrus. Their conclusions highlight that SCTT is the approach with the greatest maneuverability area and broadness and the lowest working depth.[
There is controversy regarding the anatomical limits of SCTT.[
CONCLUSION
The SCTT approach is safe and feasible for resection of lesions in the basal temporomesial region without causing damage to neighboring structures, especially those located in the middle and posterior two-thirds. Therefore, we believe this approach should be considered for interventions involving the posterior temporomesial region given the advantages it offers.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Video available on:
www.surgicalneurologyint.com
Acknowledgments
We are thankful all the staffs of Miguel Servet University Hospital involved in care of our patients.
References
1. Chau AM, Gagliardi F, Smith A, Pelzer NR, Stewart F, Mortini P. The paramedian supracerebellar transtentorial approach to the posterior fusiform gyrus. Acta Neurochir (Wien). 2016. 158: 2149-54
2. De Oliveira JG, Párraga RG, Chaddad-Neto F, Ribas GC, De Oliveira EP. Supracerebellar transtentorial approach-resection of the tentorium instead of an opening-to provide broad exposure of the mediobasal temporal lobe: Anatomical aspects and surgical applications: Clinical article. J Neurosurg. 2012. 116: 764-72
3. Fernández-Miranda JC, de Oliveira E, Rubino PA, Wen HT, Rhoton AL. Microvascular anatomy of the medial temporal region: Part 1: Its application to arteriovenous malformation surgery. Neurosurgery. 2010. 67: ons237-76
4. Grigoryan YA, Sitnikov AR, Timoshenkov AV, Grigoryan GY. An aneurysm of the medial posterior choroidal artery: A case report and a literature review. Zh Vopr Neirokhir Im N N Burdenko. 2017. 81: 101-7
5. Harput MV, Türe U. The paramedian supracerebellartranstentorial approach to remove a posterior fusiform gyrus arteriovenous malformation. Neurosurg Focus. 2017. 43: 34752
6. Izci Y, Seçkin H, Ateş Ö Başkaya MK. Supracerebellar transtentorial transcollateral sulcus approach to the atrium of the lateral ventricle: Microsurgical anatomy and surgical technique in cadaveric dissections. Surg Neurol. 2009. 72: 509-14
7. Marcus HJ, Sarkar H, Mindermann T, Reisch R. Keyhole supracerebellar transtentorial transcollateral sulcus approach to the lateral ventricle. Neurosurgery. 2013. 73: onsE295-301
8. Mascitelli J, Burkhardt JK, Gandhi S, Lawton MT. Contralateral supracerebellar-infratentorial approach for resection of thalamic cavernous malformations. Oper Neurosurg (Hagerstown). 2018. 15: 404-11
9. Moftakhar R, Izci Y, Baskaya MK. Microsurgical anatomy of the supracerebellar transtentorial approach to the posterior mediobasal temporal region: Technical considerations with a case illustration. Neurosurgery. 2008. 62: 1-7
10. Otani N, Fujioka M, Oracioglu B, Muroi C, Khan N, Roth P. Thalamic cavernous angioma: Paraculminar supracerebellar infratentorial transtentorial approach for the safe and complete surgical removal. Acta Neurochir (Wien). 2008. 103: 29-36
11. Türe U, Harput MV, Kaya AH, Baimedi P, Firat Z, Türe H. The paramedian supracerebellar-transtentorial approach to the entire length of the mediobasal temporal region: An anatomical and clinical study-laboratory investigation. J Neurosurg. 2012. 116: 773-91
12. Voigt K, Yaşargil M. Cerebral cavernous haemangiomas or cavernomas. Minim Invasive Neurosurg. 1976. 19: 59-68
13. Weil AG, Middleton AL, Niazi TN, Ragheb J, Bhatia S. The supracerebellar-transtentorial approach to posteromedial temporal lesions in children with refractory epilepsy. J Neurosurg Pediatr. 2015. 15: 45-54
14. Yonekawa Y, Imhof HG, Taub E, Curcic M, Kaku Y, Roth P. Supracerebellar transtentorial approach to posterior temporomedial structures. J Neurosurg. 2001. 94: 339-45