- Department of Neurosurgery, Hospital do Servidor Público Estadual de São Paulo, São Paulo, Brazil
- Department of Neurosurgery, DFV Neuro, São Paulo, Brazil
Correspondence Address:
Matheus Fernandes de Oliveira
Department of Neurosurgery, Hospital do Servidor Público Estadual de São Paulo, São Paulo, Brazil
DOI:10.4103/2152-7806.183502
Copyright: © 2016 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Pahl FH, de Oliveira MF, André Luiz Beer-Furlan, José Marcus Rotta. Surgical flow modification of the anterior cerebral artery-anterior communicating artery complex in the management of giant aneurysms of internal carotid artery bifurcation: An alternative for a difficult clip reconstruction. Surg Neurol Int 03-Jun-2016;7:
How to cite this URL: Pahl FH, de Oliveira MF, André Luiz Beer-Furlan, José Marcus Rotta. Surgical flow modification of the anterior cerebral artery-anterior communicating artery complex in the management of giant aneurysms of internal carotid artery bifurcation: An alternative for a difficult clip reconstruction. Surg Neurol Int 03-Jun-2016;7:. Available from: http://surgicalneurologyint.com/surgicalint_articles/surgical-flow-modification-of-the-anterior-cerebral-artery%e2%80%91anterior-communicating-artery-complex-in-the-management-of-giant-aneurysms-of-internal-carotid-artery-bifurcation-an-alternative-for/
Abstract
Background:Internal carotid artery bifurcation (ICAb) aneurysms account for about 2–15% of all intracranial aneurysms. In giant and complex cases, treatment may be difficult and dangerous, once some aneurysms have wide neck and anterior cerebral artery (ACA) and middle cerebral artery (MCA) may arise from the aneurysm itself. Clip reconstruction may be difficult in such cases. Whenever possible, the occlusion of ACA transform the bifurcation in a single artery reconstruction (ICA to MCA), much easier than a bifurcation reconstruction.
Methods:In patients with giant and complex ICAb aneurysms, we propose routine preoperative angiography with anatomical evaluation of anterior communicating artery (ACoA) patency during cervical common carotid compression with concomitant contralateral carotid artery injection. This allowed visualization of the expected reversal of flow in the A1 segment–ACoA complex. When test is positive, we can perform ipsilateral ACA (A1 segment) clip occlusion and flow modification of the ACA-ACoA complex transforming a three vessel (ICA, ACA, and MCA) reconstruction into a two vessel (ICA and MCA) reconstruction.
Results:Two patients were treated, with 100% of occlusion and good outcome.
Conclusions:Surgical treatment of giant and complex ICAb may be achieved with acceptable morbidity.
Keywords: Endovascular, intracranial aneurysm, surgery, treatment
INTRODUCTION
Internal carotid artery bifurcation (ICAb) is a location of high hemodynamic stress, where the largest intracranial vessel divides in an abrupt manner into the anterior cerebral artery (ACA) and middle cerebral artery (MCA). ICAb aneurysms account for about 2–15% of all intracranial aneurysms,[
The advocated surgical strategy to treat ICAb aneurysms include delicate dissection of its dome and reconstruction of its walls with preservation of the ACA, MCA, recurrent artery of Heubner, basal vein of Rosenthal, deep sylvian veins, and lenticulostriate perforators.[
This surgical strategy might be difficult to achieve in cases of giant, complex, and partially thrombosed aneurysms. Direct clipping and clip reconstruction may be hindered due to the intraluminal thrombus, wide neck of the aneurysm, and the ACA and MCA that may arise from its walls.[
In such cases, even the three-dimensional angiography may fail to correlate the preoperative images with intraoperative findings and its potential intraoperative complications such as aneurysm rupture, unintended arterial occlusion, and incomplete aneurysmal exclusion.[
This report describes the successful treatment of giant and complex ICAb aneurysms with surgical flow modification of the ACA-anterior communicating artery (ACoA) performed after direct clipping and clip reconstruction of the failed ICAb. The proposed management strategy is illustrated by two clinical cases.
Management strategy
In patients with giant and complex ICAb aneurysms, we propose routine preoperative angiography with anatomical evaluation of ACoA patency during cervical common carotid compression with concomitant contralateral carotid artery injection. This allowed visualization of the expected reversal of flow in the A1 segment–ACoA complex.
The test is considered positive when the ACoA is patent with adequate flow through both ACA from the contralateral ACA.
The positive test provides an intraoperative alternative for a difficult clip reconstruction of the aneurysm. Ipsilateral ACA (A1 segment) clip occlusion and flow modification of the ACA-ACoA complex may be performed and facilitate aneurysm treatment by transforming a three vessel (ICA, ACA, and MCA) reconstruction into a two vessel (ICA and MCA) reconstruction.
It is only possible to analyze and evaluate the feasibility of the initial surgical strategy after aneurysm exposure. Hence, a wide opening of the sylvian fissure with complete exposure of the ICA, M1, and its branches, ACA, and aneurysm must be performed.
In the cases where clip reconstruction is not feasible even after flow modification of the ACA-ACoA, an external carotid artery-MCA bypass is advocated together with the occlusion of the end of the carotid artery, transforming the ICAb in a terminal circulation contributing to the occlusion of the aneurysm [
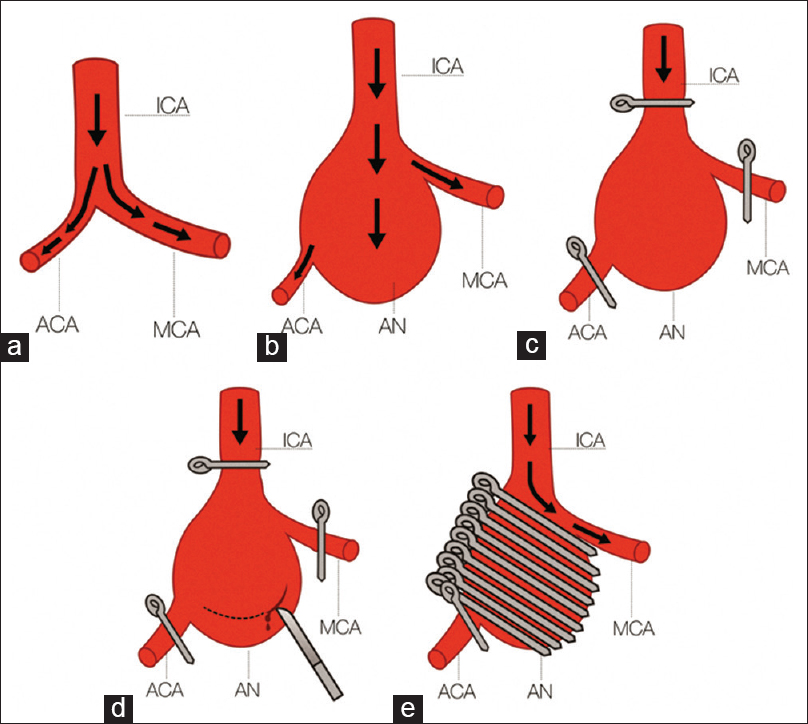
Figure 1
Illustration of the technique. (a) Normal anatomy, with internal carotid artery dividing into anterior cerebral artery and middle cerebral artery. (b) The presence of a giant aneurysm in internal carotid artery bifurcation. (c) Clipping of internal carotid artery, anterior cerebral artery, and middle cerebral artery to allow the manipulation of aneurysm. (d) Opening aneurysm and performing removal of aneurysmal clot. (e) Reconstruction with exclusion of aneurysm and clipping of anterior cerebral artery; middle cerebral artery becoming a terminal circulation
CASE ILLUSTRATIONS
Case 1
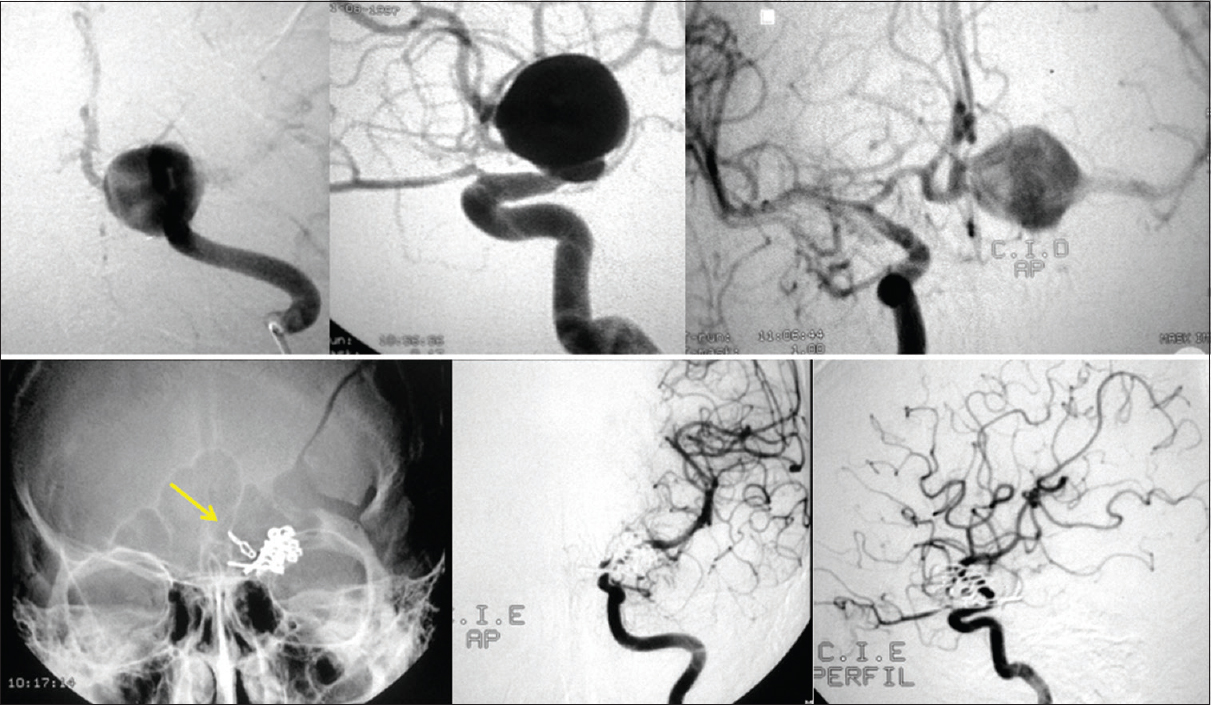
A 23-year-old man was admitted to the emergency department with the diagnosis of SAH, Hunt-Hess 2, and Fisher Grade 2. The angiography revealed a left-sided giant (25 mm) ICAb aneurysm with patency of the ACoA during cervical carotid compression test.
He underwent surgical treatment of the aneurysm, with occlusion of ACA and clip reconstruction of the ICA to the MCA. Postoperative angiography revealed a flow modification with the occlusion of the left A1 with preserved flow on the left ACA supplied by the contralateral ACA. There was also adequate flow to the left MCA [
The postoperative period was uneventful and the patient was discharged home with no deficit. On the 5-year follow-up visit, the patient's neurological examination was unchanged (mRs 0).
Case 2
A 56-year-old woman with a 2-month history of headache, vertigo, and normal neurologic examination was referred to the neurosurgery clinic after radiological investigation. The head computed tomography (CT) and magnetic resonance imaging revealed a giant right carotid bifurcation aneurysm. Angiography was performed and confirmed the location of the 25 mm aneurysm and the patency of ACoA during cervical carotid compression test [
She underwent surgical treatment of the aneurysm, with occlusion of ACA and clip reconstruction of the ICA to the MCA [
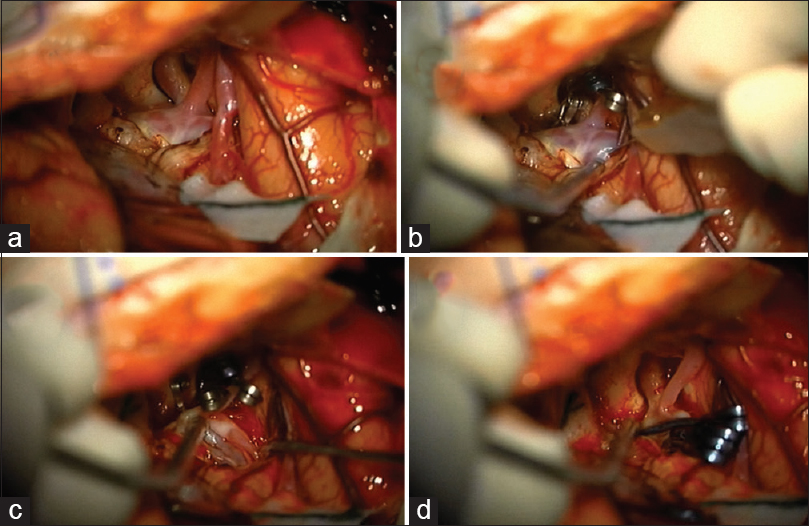
Figure 4
Intraoperative images of Case 2. (a) Right pterional approach showing internal carotid artery bifurcation aneurysm, anterior cerebral artery, and middle cerebral artery. (b) Clipping of anterior cerebral artery and temporary clipping of internal carotid artery and middle cerebral artery to explore aneurysm. (c) Aneurismal sac opening and aspiration. (d) Aneurismal reconstruction and removal of temporary clips of internal carotid artery and middle cerebral artery, remaining a definite clip in anterior cerebral artery
On the postoperative period, the patient developed left-sided hemiparesis. The head CT scan showed infarction of the posterior knee of the internal capsule, probably due to unintended occlusion of a lenticulostriate perforator. Such complication was not related to the occlusion of ACA, but to aneurysmal fundus dissection.
One year after surgery, the patient had a persistent left-sided Grade 4 hemiparesis (mRs 2).
DISCUSSION
Wide-neck and giant ICAb aneurysms are rare entities and its management remains challenging independently of the choice between endovascular or surgical treatment.[
The main difficulty in the surgical management of these aneurysms is the preservation of perforating arteries surrounding or adherent to the dome while performing the reconstruction of the ICA, ACA, and MCA.[
Surgical series are rarely reported in literature since the first experiences of Gupta et al.[
Cohen-Gadol[
More recently, Konczalla et al.[
Endovascular management of ICAb aneurysms are also challenging due to unfavorable morphologic features, complexity of Y stenting or balloon-assisted coiling techniques, and variable occlusion, recanalization and retreatment rates.[
Nossek et al.[
Our surgical flow modification of the ACA-ACoA complex is conceptually similar to the endovascular strategy proposed by Nossek et al.[
The preoperative angiographic evaluation revealing the patency of ACoA and flow through both ACA from the contralateral ACA indicates that proximal ACA occlusion may be performed as a valuable surgical option. The illustrative cases demonstrate that ACA-ACoA flow modification is a reliable intraoperative alternative for giant ICAb aneurysms with acceptable risks and complications.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Cohen-Gadol AA. Microsurgical management of giant (>5 cm) internal carotid artery bifurcation aneurysms presenting with brainstem compression using radial artery interposition bypass graft: Technique. Neurosurgery. 2014. 10: 368-
2. González-Darder JM, González-López P, Botella-Maciá L. Microsurgical treatment of internal carotid bifurcation aneurysms. Neurocirugia (Astur). 2010. 21: 205-10
3. Gupta SK, Khosla VK, Chhabra R, Mohindra S, Bapuraj JR, Khandelwal N. Internal carotid artery bifurcation aneurysms: Surgical experience. Neurol Med Chir (Tokyo). 2007. 47: 153-7
4. Hacein-Bey L, Connolly ES, Mayer SA, Young WL, Pile-Spellman J, Solomon RA. Complex intracranial aneurysms: Combined operative and endovascular approaches. Neurosurgery. 1998. 43: 1304-12
5. Heller RS, Rahal JP, Malek AM. Y-Stent embolization technique for intracranial bifurcation aneurysms. J Clin Neurosci. 2014. 21: 1368-72
6. Iihara K, Maruyama D, Fukuda K, Nakajima N, Kataoka H. Tasuki clipping combined with high flow bypass for ruptured, previously coiled, partially thrombosed giant aneurysm at the carotid bifurcation. Neurol Med Chir (Tokyo). 2013. 53: 185-9
7. Konczalla J, Platz J, Brawanski N, Güresir E, Lescher S, Senft C. Endovascular and surgical treatment of internal carotid bifurcation aneurysms: Comparison of results, outcome, and mid-term follow-up. Neurosurgery. 2015. 76: 540-50
8. Ladner TR, He L, Davis BJ, Froehler MT, Mocco J. Simultaneous stent expansion/balloon deflation technique to salvage failed balloon remodeling. J Neurointerv Surg. 2016. 8: e15-
9. Laranjeira M, Sadasivan B, Ausman JI. Direct surgery for carotid bifurcation artery aneurysms. Surg Neurol. 1990. 34: 250-4
10. Lawton MT, Quiñones-Hinojosa A, Chang EF, Yu T. Thrombotic intracranial aneurysms: Classification scheme and management strategies in 68 patients. Neurosurgery. 2005. 56: 441-54
11. Lee WJ, Cho YD, Kang HS, Kim JE, Cho WS, Kim KM. Endovascular coil embolization in internal carotid artery bifurcation aneurysms. Clin Radiol. 2014. 69: e273-9
12. Lehecka M, Dashti R, Romani R, Celik O, Navratil O, Kivipelto L. Microneurosurgical management of internal carotid artery bifurcation aneurysms. Surg Neurol. 2009. 71: 649-67
13. Lehto H, Hernesniemi J. Tiny but significant: Perforators in aneurysm surgery. World Neurosurg. 2014. 82: 591-2
14. Lubicz B, Klisch J, Gauvrit JY, Szikora I, Leonardi M, Liebig T. WEB-DL endovascular treatment of wide-neck bifurcation aneurysms: Short- and midterm results in a European study. AJNR Am J Neuroradiol. 2014. 35: 432-8
15. Miyazawa N, Nukui H, Horikoshi T, Yagishita T, Sugita M, Kanemaru K. Surgical management of aneurysms of the bifurcation of the internal carotid artery. Clin Neurol Neurosurg. 2002. 104: 103-14
16. Morales-Valero SF, Brinjikji W, Murad MH, Wald JT, Lanzino G. Endovascular treatment of internal carotid artery bifurcation aneurysms: A single-center experience and a systematic review and meta-analysis. AJNR Am J Neuroradiol. 2014. 35: 1948-53
17. Nossek E, Chalif D, Chakraborty S, Setton A. O-020 modifying flow in the ICA bifurcation: Pipeline deployment from the supraclinoid ICA extending into the M1 segment: Clinical and anatomical results. J Neurointerv Surg. 2014. 6: A10-1
18. Nossek E, Chalif DJ, Levine M, Setton A. Modifying flow in the ACA-ACoA complex: Endovascular treatment option for wide-neck internal carotid artery bifurcation aneurysms. J Neurointerv Surg. 2015. 7: 351-6
19. Nurminen V, Lehecka M, Chakrabarty A, Kivisaari R, Lehto H, Niemelä M. Anatomy and morphology of giant aneurysms - Angiographic study of 125 consecutive cases. Acta Neurochir (Wien). 2014. 156: 1-10
20. Oishi H, Yamamoto M, Nonaka S, Arai H. Endovascular therapy of internal carotid artery bifurcation aneurysms. J Neurointerv Surg. 2013. 5: 400-4
21. Peach T, Cornhill JF, Nguyen A, Riina H, Ventikos Y. The ‘sphere’: A dedicated bifurcation aneurysm flow-diverter device. Cardiovasc Eng Technol. 2014. 5: 334-347
22. Pierot L, Klisch J, Gauvrit J, Szikora I, Leonardi M, Liebig T. P-009 WEB endovascular treatment of wide-neck bifurcation aneurysms: Short- and midterm results in a european study. J Neurointerv Surg. 2014. 6: A25-
23. Pritz MB. Perforator and secondary branch origin in relation to the neck of saccular, cerebral bifurcation aneurysms. World Neurosurg. 2014. 82: 726-32
24. Reynier Y, Lena G, Vincentelli F, Vigouroux RP. Aneurysm of the internal carotid artery bifurcation. Technical reflections apropos of a series of 10 cases. Neurochirurgie. 1989. 35: 242-5
25. Sakamoto S, Ohba S, Shibukawa M, Kiura Y, Okazaki T, Arita K. Characteristics of aneurysms of the internal carotid artery bifurcation. Acta Neurochir (Wien). 2006. 148: 139-43
26. Saleme S, Iosif C, Ponomarjova S, Mendes G, Camilleri Y, Caire F. Flow-diverting stents for intracranial bifurcation aneurysm treatment. Neurosurgery. 2014. 75: 623-31
27. Spiotta AM, Chaudry MI, Turk AS, Turner RD. Initial experience with the PulseRider for the treatment of bifurcation aneurysms: Report of first three cases in the USA. J Neurointerv Surg. 2016. 8: 186-9
28. van Rooij WJ, Sluzewski M, Beute GN. Internal carotid bifurcation aneurysms: Frequency, angiographic anatomy and results of coiling in 50 aneurysms. Neuroradiology. 2008. 50: 583-7
29. Yavuz K, Geyik S, Cekirge S, Saatci I. Double stent-assisted coil embolization treatment for bifurcation aneurysms: Immediate treatment results and long-term angiographic outcome. AJNR Am J Neuroradiol. 2013. 34: 1778-84