- Department of Orthopedic Surgery, Western Reserve Hospital, Cuyahoga Falls, Ohio, USA
- Department of Neurosurgery, Cleveland Clinic Foundation, Cleveland, Ohio, USA
Correspondence Address:
Gordon Preston
Department of Neurosurgery, Cleveland Clinic Foundation, Cleveland, Ohio, USA
DOI:10.4103/sni.sni_209_17
Copyright: © 2017 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Gordon Preston, Toomas Anton. T2 vertebrectomy with combined anterior and posterior arthrodesis for treatment of a solitary plasmacytoma. 09-Aug-2017;8:173
How to cite this URL: Gordon Preston, Toomas Anton. T2 vertebrectomy with combined anterior and posterior arthrodesis for treatment of a solitary plasmacytoma. 09-Aug-2017;8:173. Available from: http://surgicalneurologyint.com/surgicalint-articles/t2-vertebrectomy-with-combined-anterior-and-posterior-arthrodesis-for-treatment-of-a-solitary-plasmacytoma/
Abstract
Background:Plasma cell neoplasmas are a heterogenous group of neoplastic tumor lesions occurring secondary to disordered proliferation of cells from a monocyte lineage. Plasmacytoma is a rare lesion that accounts for 5% of all plasma cell neoplasms. The current recommended treatment for solitary plasmacytoma is moderate dose radiation therapy. For patients who are suffering from axial back pain, spinal instability, radiculopathy, or bowel/bladder dysfunction secondary to spinal cord compression, surgical intervention with spinal decompression and stabilization can be used as an adjuvant to radiation therapy.
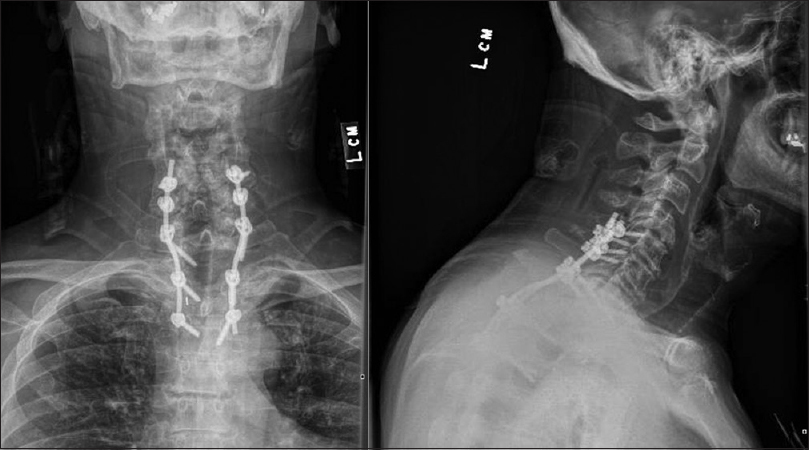
Case Description:We report a patient who presented with worsening axial and bilateral upper extremity pain. He was found to have a locally aggressive tumor involving the vertebral body of T2. After a repeat magnetic resonance imaging (MRI) and a computed tomography (CT)-guided biopsy, the diagnosis of a solitary plasmacytoma was confirmed. It destroyed over 90% of the T2 vertebral body, resulted in 22° of local kyphosis, and caused spinal cord compression. The tumor was treated with a T2 vertebrectomy, posterior arthrodesis from C5–T4, and anterior arthrodesis from T1–3.
Conclusions:Solitary plasmacytomas of the vertebral bodies are difficult lesions to treat secondary to their location and risk of neurologic compromise. Surgical intervention with tumor resection and adjuvant chemotherapy or radiation is the recommended treatment option.
Keywords: Arthrodesis, solitary plasmacytoma, thoracic spine
INTRODUCTION
The most common primary tumor of the axial skeleton is a plasmacytoma. It comprises proliferation of monoclonal plasma cells derived from B cells in the bone marrow.[
CASE DESCRIPTION
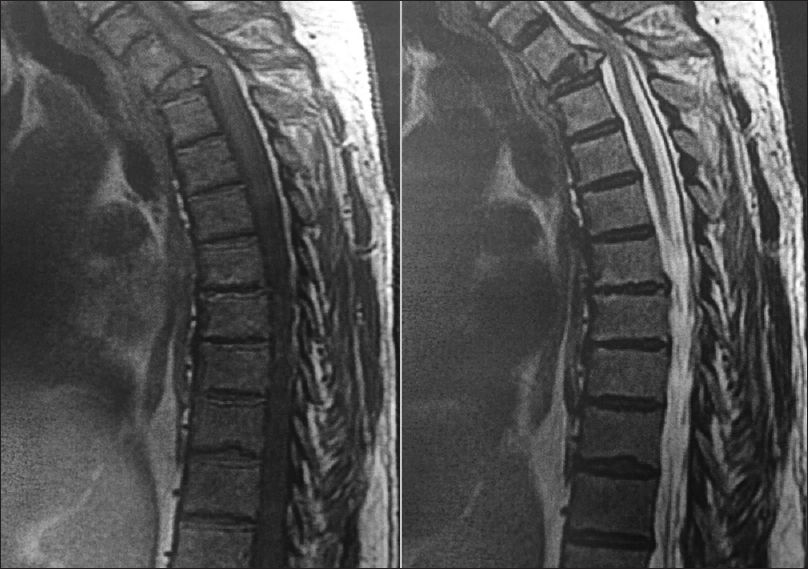
The patient is a 68-year-old male who presented with 6 months of progressively worsening interscapular back pain and bilateral arm pain. A CT-guided biopsy was negative for multiple myeloma. The patient's urine Serum Protein Electrophoresis (SPEP) displayed an M-spike of 0.4, however, free kappa and lambda light chains were normal. The patient did not display any signs of renal insufficiency or anemia. The magnetic resonance imaging (MRI) of the thoracic spine displayed a T2 pathologic fracture with 90% height loss, 22° of local kyphosis, and spinal cord compression. The fracture appeared to have high signal intensity on the T2-weighted image and low signal intensity on the T1-weighted image, consistent with an active tumor, most likely a plasmacytoma [
The final pathology displaying sheets of small plasma cells overrunning normal tissues that were positive for CD138 which had aberrant expression of CD56, indicating plasma cells. The patient continued to have improvement of his symptoms at 3-month follow-up.
DISCUSSION
Solitary plasmacytoma is a rare tumor that typically occurs in the thoracic spine. Patients can present without symptoms or with complaints of back pain, with or without signs of spinal cord compression.[
Spinal surgery can be an effective adjuvant to radiation therapy, but it is not always indicated as part of the treatment regimen. In asymptomatic patients who have no signs of spinal instability, radiation therapy alone can be effective. Dimopoulos et al. revealed that surgery with radiation therapy vs radiation therapy alone had no significant difference in 10-year probability of local control in multiple myeloma patients.[
CONCLUSION
Overall, spinal surgeries are not indicated for patients suffering from solitary plasmacytoma unless the disease has progressed to cause axial back pain, spinal instability, radiculopathy, or signs of spinal cord compression. Our patient, however, was a good surgical candidate as he met multiple operative indications. Postoperatively the patient had significant resolution of axial back pain, which continued to improve at 3-month follow up.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Brenner H, Gondos A, Pulte D. Expected long-term survival of patients diagnosed with multiple myeloma in 2006-2010. Haematologica. 2009. 94: 270-5
2. Dimopoulos MA, Moulopoulos LA, Maniatis A, Alexanian R. Solitary plasmacytoma of bone and asymptomatic multiple myeloma. Blood. 2000. 96: 2037-44
3. Ghodke K, Shet T, Epari S, Sengar M, Menon H, Gujral S. A retrospective study of correlation of morphologic patterns, MIB1 proliferation index, and survival analysis in 134 cases of plasmacytoma. Ann Diagn Pathol. 2015. 19: 117-23
4. Hong B, Hermann EJ, Reuter C, Brandis A, Krauss JK. Outcome of surgical decompression of spinal mass lesions in non-Hodgkin's lymphoma and plasmacytoma. Clin Neurol Neurosurg. 2013. 115: 2476-81
5. Knobel D, Zouhair A, Tsang RW, Poortmans P, Belkacémi Y, Bolla M. Prognostic factors in solitary plasmacytoma of the bone: A multicenter Rare Cancer Network study. BMC Cancer. 2006. 6: 118-
6. Mirzashahi B, Mazoochy H, Jamnani RK, Farzan A. Contribution of surgery in solitary plasmacytoma of spine; a case report. Arch Bone Jt Surg. 2014. 2: 121-5
7. Terada T. Solitary plasmacytoma of the thoracic vertebra presenting with sudden paraplegia and back pain: A pathologic case report. Pathol Oncol Res. 2011. 17: 167-9
8. Yang JS, Cho YJ, Kang SH, Choi HJ. Rapid progression of solitary plasmacytoma to multiple myeloma in lumbar vertebra. J Korean Neurosurg Soc. 2013. 54: 426-30






Ali Fahir Ozer
Posted September 2, 2017, 1:43 am
This surgery can be performed only posterior approach. Plasmacytoma is a soft tumour and it is easily evacuated including midline mass removing facet joints and pedicles on one side or both sides. Anterior approach can be difficult because of increasing AP diameter of chest cavity. There is no absolute indication of bone graft. Bone cement can be a good choice instead of bone graft because the patient will get radiotherapy soon. It can be placed following posterior decompression. Morbidity risk can become high with anterior approach. Plus anterior approach is not wrong but over treatment.