- Department of Neurosurgery, Hospital São José-Santa Casa de Misericórdia de Porto Alegre, Porto Alegre, Brazil.
- Department of Teaching and Research, Universidade Federal de Pelotas, Pelotas, Rio Grande do Sul, Brazil.
Correspondence Address:
Rodrigo Ness, Department of Teaching and Reaserch, Universidade Federal de Pelotas, Pelotas, Brazil.
DOI:10.25259/SNI_1019_2022
Copyright: © 2023 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Guilherme Gago1, Guilherme Ludwig1, Rodrigo Ness2, Albert Brasil1. Use of Wiltse approach in lumbar plexus schwannoma: A technical note. 31-Mar-2023;14:118
How to cite this URL: Guilherme Gago1, Guilherme Ludwig1, Rodrigo Ness2, Albert Brasil1. Use of Wiltse approach in lumbar plexus schwannoma: A technical note. 31-Mar-2023;14:118. Available from: https://surgicalneurologyint.com/surgicalint-articles/12224/
Abstract
Background: Lumbar plexus schwannomas are a rare occurrence in neurosurgery, with few reported cases and no standard surgical approach. This study describes a successful surgical resection with no complications using the Wiltse approach.
Methods: Patient presented with an intra-psoas tumor suggesting schwannoma. We described the surgical technique involved step by step.
Results: The patient recovered from the surgery with no complications. The anatomopathological examination confirmed the schwannoma diagnosis. The post operatory magnetic resonance imaging showed complete resection.
Conclusion: This study shows that the use of Wiltse approach, mainly used for classical herniated disc extraforaminal, can be used successfully on Lumbar plexus schwannomas.
Keywords: Lumbar plexus schwannomas, Wiltse approach, Intra-psoas schwannomas
INTRODUCTION
Schwannomas are a benign and slow-growth type of tumor that originated from Schwann cells derived from the neural crest of any myelinated nerve.[
CASE AND TECHNICAL DESCRIPTION
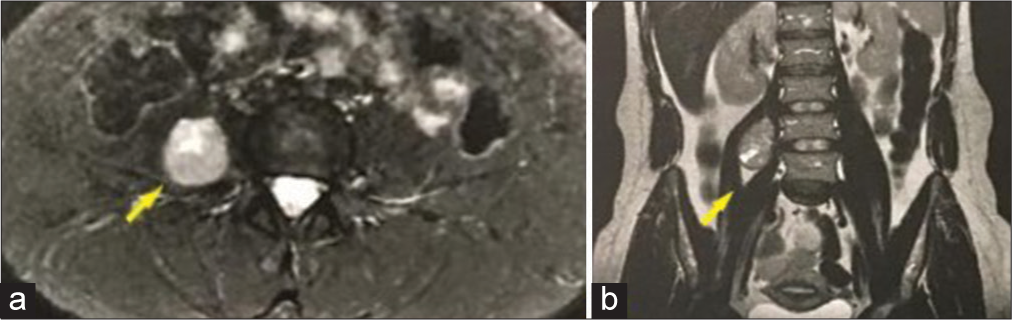
Patient, 34-year-old female, with a history of the right thigh paresthesia and pain which limited right leg movement, presented herself to the neurosurgery team. For investigation, a lumbar magnetic resonance imaging (MRI) was requested, revealing a right intra-iliopsoas well defined heterogeneous solid lesion in the plane of L4-L5 measuring 5.0 × 3.0 cm in the coronal plane [
Under general anesthesia, the neurophysiological monitoring system was installed, tested, and functional. The patient was placed in a prone position, with the testing of neurophysiological potentials going without complications. After the antisepsis and allocation of surgical fields, the lumbar level L3-L4-L5 was marked with intraoperative X-ray. Local anesthesia with lidocaine 2% and bupivacaine 0.5%. The incision was made 3 cm lateral to the midline, at the right side, with radioscopic confirmation on the L4 level.
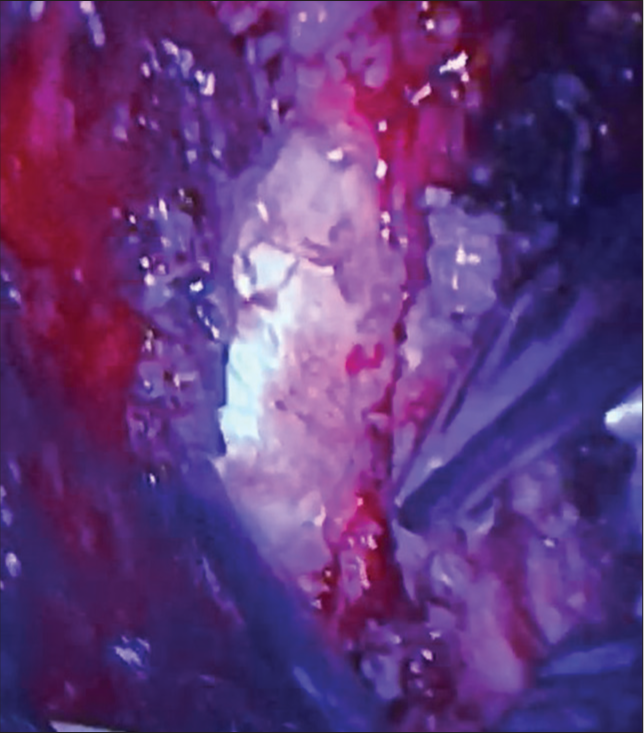
The multifidus and longissimus muscles were separated, progressing with blunt dissection until the exposition of the transverse process of L3-L5. Confirmation was made with intraoperative X-ray. The right transverse processes of L4 and L5 were both resected for better access to the tumor. A surgical microscope was set in the surgical field for visualization of the tumor lesion, which was seen in the interior of the right psoas muscle, with well-defined borders and a cleavage plane [
RESULTS
The patient was admitted to the recovery room, with a good post anesthesia recovery. She woke up without any neurological deficits. The recovery from the surgery was quick, with hospital discharge 2 days after the surgery, without pain or neurological deficits. During the medical appointment 2 weeks later, she was already completely recovered. The postoperative magnetic resonance imaging showed no residual tumor [
DISCUSSION
Lumbar plexus schwannomas are a rare type of tumor, with limited reported cases worldwide.[
CONCLUSION
The Wiltse approach proved to be useful for the treatment of lumbar plexus schwannoma in the case presented. Due to the rarity of such disease, more reports have to be done for a consensus to be made regarding the best surgical approach in this condition.
Declaration of patient consent
Patient’s consent not required as patient’s identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.
References
1. AlQahtani A, AlAli MN, Allehiani S, AlShammari S, Al-Sakkaf H, Arafah MA. Laparoscopic resection of retroperitoneal intra-psoas muscle schwannoma: A case report and extensive literature review. Int J Surg Case Rep. 2020. 74: 1-9
2. Guiroy A, Sícoli A, Masanés NG, Ciancio AM, Gagliardi M, Falavigna A. How to perform the Wiltse posterolateral spinal approach: technical note. Surg Neurol Int. 2018. 9: 38
3. Lee SE, Jahng TA, Kim HJ. Different surgical approaches for spinal schwannoma: A single surgeon’s experience with 49 consecutive cases. World Neurosurg. 2015. 84: 1894-902
4. Mukai Y, Takenaka S, Hosono N, Miwa T, Fuji T. Intramuscular pressure of the multifidus muscle and low-back pain after posterior lumbar interbody fusion: Comparison of mini-open and conventional approaches. J Neurosurg Spine. 2013. 19: 651-7
5. Rabelo NN, Da Silva BN, Filho LJ, Dos Passos GS, Pereira VH, Junior LA. Paraspinal lumbar spine approach-wiltse access. Braz Neurosurg. 2017. 36: 167-71
6. Sakurai K, Asamoto S, Nakamura S, Ishihara S, Ishikawa M, Nishiyama M. Surgical technique for lumbar spinal extraforaminal schwannoma. No Shinkei Geka. 2018. 46: 5-9
7. Seppälä MT, Haltia MJ, Sankila RJ, Jääskeläinen JE, Heiskanen O. Long-term outcome after removal of spinal schwannoma: A clinicopathological study of 187 cases. J Neurosurg. 1995. 83: 621-6
8. Sheikh MM, De Jesus O, editors. Schwannoma. StatPearls. Treasure Island, FL: StatPearls Publishing; 2022. p. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562312 [Last accessed on 2022 Aug 19]
9. Shimoda Y, Morimoto D, Isu T, Hamauchi S, Matsumoto R, Isobe M. Schwannoma developing in the psoas major muscle: A case report. No Shinkei Geka. 2011. 39: 51-7
10. Srinath SR, Divya D, Lileswar K. Incidental detection of retroperitoneal schwannoma: A case report. J Clin Case Rep. 2017. 7: 4
11. Tsutsumimoto T, Shimogata M, Ohta H, Misawa H. Mini-open versus conventional open posterior lumbar interbody fusion for the treatment of lumbar degenerative spondylolisthesis: Comparison of paraspinal muscle damage and slip reduction. Spine. 2009. 34: 1923-8