- Department of Neurosurgery, Fundação Faculdade Regional de Medicina de São José do Rio Preto (FUNFARME), São José do Rio Preto, São Paulo, Brazil.
Correspondence Address:
Lucas Crociati Meguins, Department of Neurosurgery, Fundação Faculdade Regional de Medicina de São José do Rio Preto (FUNFARME), São José do Rio Preto, São Paulo, Brazil.
DOI:10.25259/SNI_514_2021
Copyright: © 2021 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Lucas Crociati Meguins, Andre Salotto Rocha, Matheus Rodrigo Laurenti, Dionei Freitas de Morais. Ventricular empyema associated with severe pyogenic meningitis in COVID-19 adult patient: Case report. 12-Jul-2021;12:346
How to cite this URL: Lucas Crociati Meguins, Andre Salotto Rocha, Matheus Rodrigo Laurenti, Dionei Freitas de Morais. Ventricular empyema associated with severe pyogenic meningitis in COVID-19 adult patient: Case report. 12-Jul-2021;12:346. Available from: https://surgicalneurologyint.com/surgicalint-articles/10962/
Abstract
Background: Coronavirus Disease 2019 (COVID-19) pandemic raised global attention especially due to the severe acute respiratory symptoms associated to it. However, almost one third of patients also develop neurological symptoms. The aim of the present study is to describe the case of a previously health adult that evolved cerebral ventricular empyema in the IV ventricle during COVID-19 infection treatment.
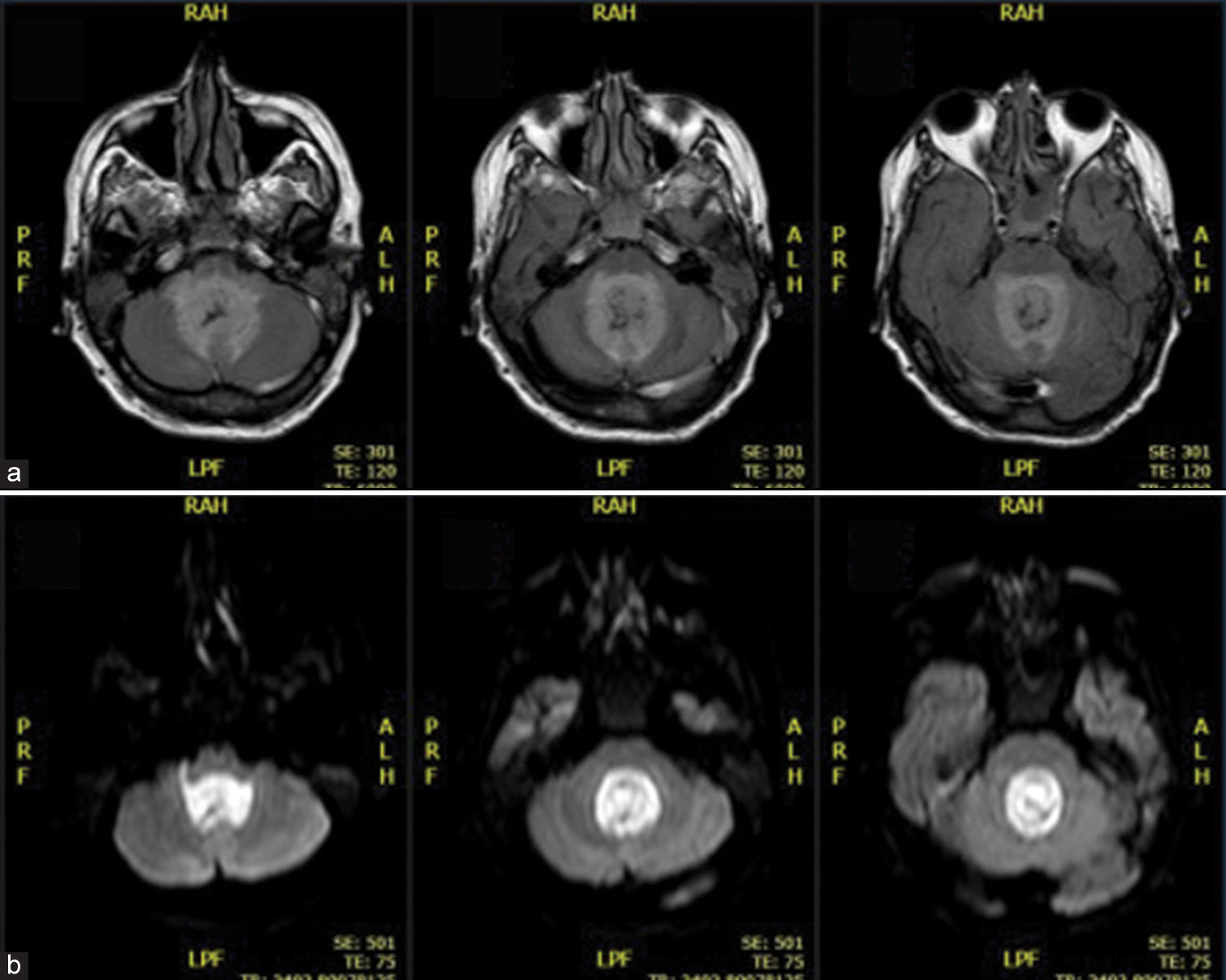
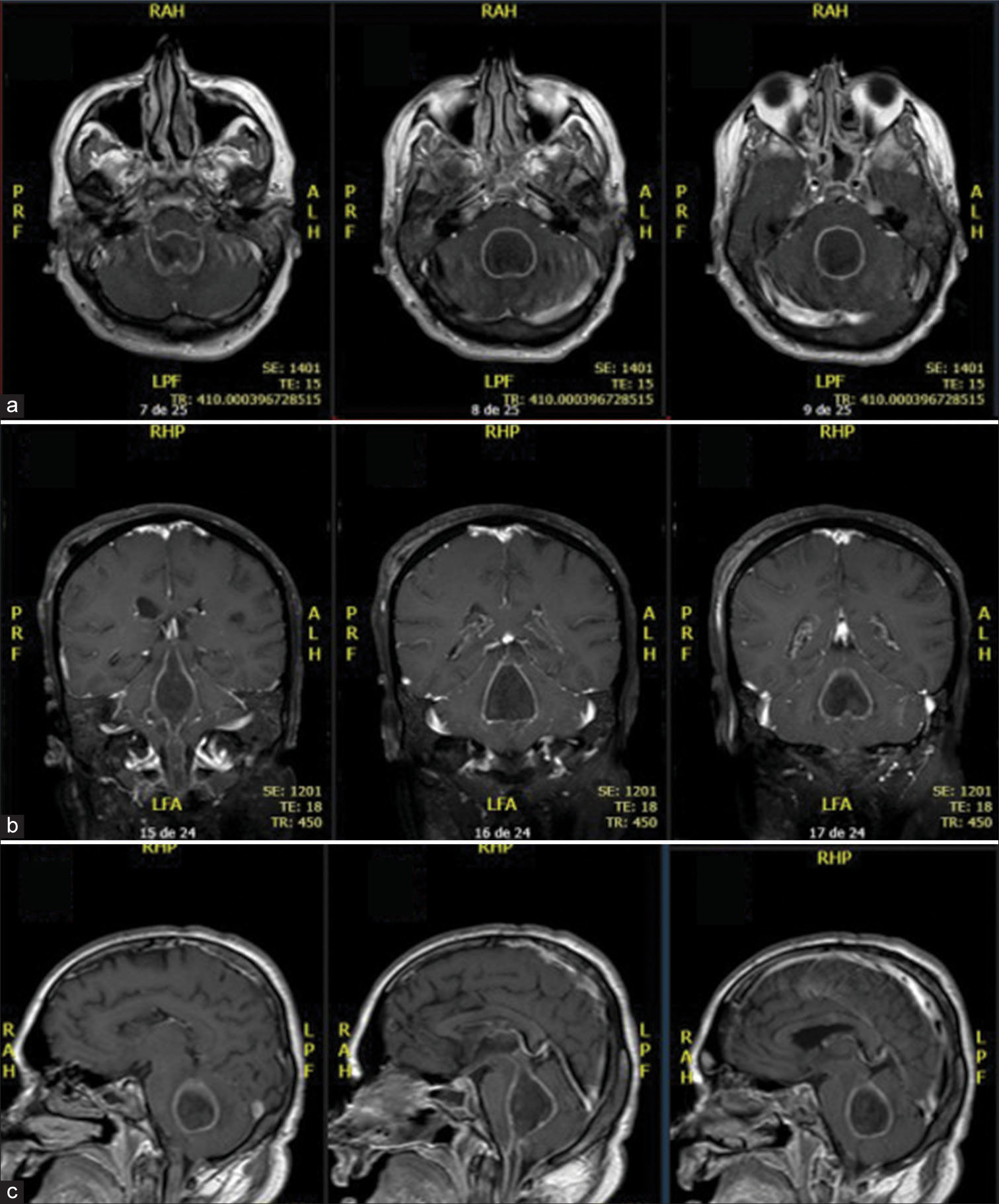
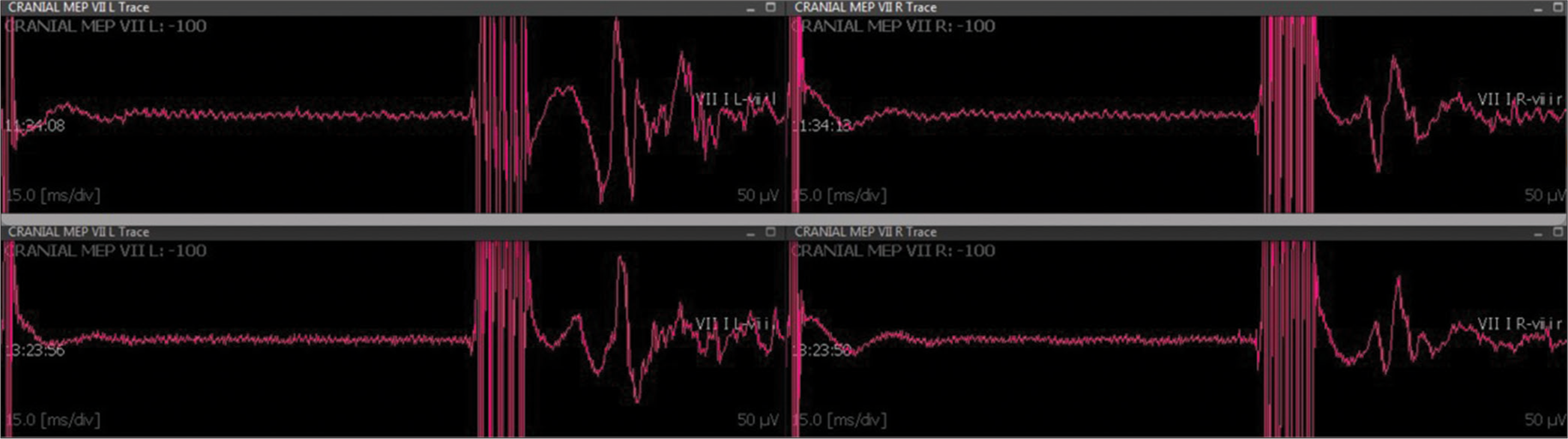
Case Description: A 49-year-old man with COVID-19 developed pneumonia caused by multidrug-resistant Acinetobacter baumannii. After treating adequate treatment, sedation was switched off without showing appropriate awakening. Brain CT was performed with evidence of communicating hydrocephalus. External ventricular shunt (EVD) was implant with intraoperative cerebrospinal fluid suggestive of meningitis with a positive culture for oxacillin-sensitive Staphylococcus hominis. Twenty days after EVD, meningitis treatment was finished and with 2 negative cultures, conversion to ventriculoperitoneal shunt was performed. In the following week, during the evaluation of the patient in intensive care, quadriplegia and absence of spontaneous respiratory movement were evidenced, just maintaining head movement. Brain MRI was performed with a diagnosis of ventriculitis associated with pus collections on the IV ventricle. The patient underwent microsurgical drainage removal of the shunt, with a positive intraventricular collection culture for Klebsiella pneumoniae carbapenemase and multidrug-resistant Pseudomonas aeruginosa, without improvement in the neurological condition. After 14 weeks of hospitalization, the patient died.
Conclusion: It is well known that COVID-19 has potential to directly attack and cause severe damage to the central nervous system; however, ventricular empyema is an extremely rare life-threatening complication.
Keywords: Coronavirus disease 2019, External ventricular shunt, Hydrocephalus, Motor Evoked Potentials, Ventricular empyema
INTRODUCTION
Coronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), emerged in Wuhan, China, and has become a global health threat.[
The aim of the present study is to describe the case of a previously health adult that evolved a voluminous ventricular empyema in the IV ventricle during COVID-19 infection treatment.
CASE DESCRIPTION
A 49-year-old, previously healthy patient, diagnosed with COVID-19 in December/2020 was hospitalized in an intensive care unit with respiratory symptoms and no neurological deficits, but confusion and lethargy. He developed pneumonia caused by multidrug-resistant Acinetobacter baumannii and sinusitis. After treating such infections with antibiotic therapy, the patient’s sedation was switched off without showing adequate awakening, then a brain CT was performed with evidence of communicating hydrocephalus with signs of cerebrospinal fluid transudation. The patient underwent an external ventricular shunt (EVD) implant with intraoperative cerebrospinal fluid suggestive of meningitis with a positive culture for oxacillin-sensitive Staphylococcus hominis. Twenty days after EVD, meningitis treatment was finished and with 2 negative cultures, conversion to ventriculoperitoneal shunt was performed. In the following week, during the evaluation of the patient in intensive care, quadriplegia and absence of spontaneous respiratory movement were evidenced, just maintaining head movement, characterizing lock-in syndrome. A brain MRI was performed with a diagnosis of ventriculitis associated with an empyema on the 4th ventricle [
DISCUSSION
COVID-19 is a novel respiratory disease caused by SARSCoV-2 and has become a global health threat.[
The mechanisms involved in the neurological affections resulting from SARS-CoV-2 infection are not completely understood. However, it has been proposed that the virus gains access to the CNS by systemic vascular dissemination or, more locally, across the cribriform plate of the ethmoid bone.[
COVID-19 patients may present central (CNS) and peripheric nervous system (PNS)-associated signs and symptoms. Several CNS-related manifestations have been reported and include headache, dizziness, impaired consciousness, acute cerebrovascular disease, epilepsy, ataxia, acute disseminated encephalomyelitis, and viral encephalitis.[
Talamonti et al. described six consecutive COVID-19 patients with primary spinal epidural abscess (SEA) that was managed surgically.[
CONCLUSION
It is well known that COVID-19 has potential to directly attack and cause severe damage to the CNS; however, intraventricular pus collection is an extremely rare life-threatening complication in COVID-19 patient. Further scientific investigations are necessary to understand whether the viral infection increases the risk of ventricular empyema.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Abobaker A, Raba AA, Alzwi A. Extrapulmonary and atypical clinical presentations of COVID-19. J Med Virol. 2020. 92: 2458-64
2. Ahmad I, Rathore FA. Neurological manifestations and complications of COVID-19: A literature review. J Clin Neurosci. 2020. 77: 8-12
3. Baig AM, Khaleeq A, Ali U, Syeda H. Evidence of the COVID-19 virus targeting the CNS: Tissue distribution, host-virus interaction, and proposed neurotropic mechanisms. ACS Chem Neurosci. 2020. 11: 995-8
4. Baig AM. Neurological manifestations in COVID-19 caused by SARS-CoV-2. CNS Neurosci Ther. 2020. 26: 499-501
5. Behzad S, Aghaghazvini L, Radmard AR, Gholamrezanezhad A. Extrapulmonary manifestations of COVID-19: Radiologic and clinical overview. Clin Imaging. 2020. 66: 35-41
6. Berger JR. COVID-19 and the nervous system. J Neurovirol. 2020. 26: 143-8
7. Bourgonje AR, Abdulle AE, Timens W, Hillebrands JL, Navis GJ, Gordijn SJ. Angiotensin-converting enzyme 2 (ACE2), SARS-CoV-2 and the pathophysiology of Coronavirus disease 2019 (COVID-19). J Pathol. 2020. 251: 228-48
8. Chau CH, Strope JD, Figg WD. COVID-19 clinical diagnostics and testing technology. Pharmacotherapy. 2020. 40: 857-68
9. Deletis V, Fernández-Conejero I. Intraoperative monitoring and mapping of the functional integrity of the brainstem. J Clin Neurol. 2016. 12: 262-73
10. Ge H, Wang X, Yuan X, Xiao G, Wang C, Deng T. The epidemiology and clinical information about COVID-19. Eur J Clin Microbiol Infect Dis. 2020. 39: 1011-9
11. Gupta A, Madhavan MV, Sehgal K, Nair N, Mahajan S, Sehrawat TS. Extrapulmonary manifestations of COVID-19. Nat Med. 2020. 26: 1017-32
12. Huang X, Wei F, Hu L, Wen L, Chen K. Epidemiology and clinical characteristics of COVID-19. Arch Iran Med. 2020. 23: 268-71
13. Iadecola C, Anrather J, Kamel H. Effects of COVID-19 on the nervous system. Cell. 2020. 183: 16-27e1
14. Liu X, Liu C, Liu G, Luo W, Xia N. COVID-19: Progress in diagnostics, therapy and vaccination. Theranostics. 2020. 10: 7821-35
15. Niazkar HR, Zibaee B, Nasimi A, Bahri N. The neurological manifestations of COVID-19: A review article. Neurol Sci. 2020. 41: 1667-71
16. Pathangey G, Fadadu PP, Hospodar AR, Abbas AE. Angiotensin-converting enzyme 2 and COVID-19: Patients, comorbidities, and therapies. Am J Physiol Lung Cell Mol Physiol. 2021. 320: L301-30
17. Samudrala PK, Kumar P, Choudhary K, Thakur N, Wadekar GS, Dayaramani R. Virology, pathogenesis, diagnosis and in-line treatment of COVID-19. Eur J Pharmacol. 2020. 883: 173375
18. Sarkesh A, Daei Sorkhabi A, Sheykhsaran E, Alinezhad F, Mohammadzadeh N, Hemmat N. Extrapulmonary clinical manifestations in COVID-19 patients. Am J Trop Med Hyg. 2020. 103: 1783-96
19. Talamonti G, Colistra D, Crisà F, Cenzato M, Giorgi P, D’Aliberti G. Spinal epidural abscess in COVID-19 patients. J Neurol. 2021. 268: 2320-6
20. Wan DY, Luo XY, Dong W, Zhang ZW. Current practice and potential strategy in diagnosing COVID-19. Eur Rev Med Pharmacol Sci. 2020. 24: 4548-53
21. Whittaker A, Anson M, Harky A. Neurological manifestations of COVID-19: A systematic review and current update. Acta Neurol Scand. 2020. 142: 14-22
22. Wu Y, Xu X, Chen Z, Duan J, Hashimoto K, Yang L. Nervous system involvement after infection with COVID-19 and other coronaviruses. Brain Behav Immun. 2020. 87: 18-22
23. Zhou M, Zhang X, Qu J. Coronavirus disease 2019 (COVID-19): A clinical update. Front Med. 2020. 14: 126-35