- Department of Neurosurgery, Houston Methodist Neurological Institute, Houston Methodist Hospital, Houston, Texas, United States.
DOI:10.25259/SNI_38_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Virendra Rajendrakumar Desai, Saeed Sam Sadrameli, Amanda V. Jenson, Samuel K. Asante, Bradley Daniels, Todd W. Trask, Gavin Britz. Ventriculoperitoneal shunt complications in an adult population: A comparison of various shunt designs to prevent overdrainage. 05-Sep-2020;11:269
How to cite this URL: Virendra Rajendrakumar Desai, Saeed Sam Sadrameli, Amanda V. Jenson, Samuel K. Asante, Bradley Daniels, Todd W. Trask, Gavin Britz. Ventriculoperitoneal shunt complications in an adult population: A comparison of various shunt designs to prevent overdrainage. 05-Sep-2020;11:269. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=10248
Abstract
Background: Overdrainage after cerebrospinal fluid diversion remains a significant morbidity. The hydrostatic, gravitational force in the upright position can aggravate this. Siphon control (SC) mechanisms, as well as programmable and flow regulating devices, were developed to counteract this. However, limited studies have evaluated their safety and efficacy. In this study, direct comparisons of the complication rates between siphon control (SC) and non-SC (NSC), fixed versus programmable, and flow- versus pressure regulating valves are undertaken.
Methods: A retrospective chart review was performed over all shunt implantations from January 2011 to December 2016 within the Houston Methodist Hospital system. Complication rates within 6 months of the operative date, including infection, subdural hematoma, malfunction, and any other shunt-related complication, were analyzed via Fisher’s exact test, with P
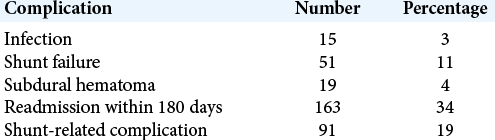
Results: The overall shunt-related complication rate in this study was 19%. Overall rates of infection, shunt failure, and readmission within 180 days were 3%, 11%, and 34%, respectively. No difference was seen between SC and NSC groups in any complication rate overall or on subgroup analyses. When comparing fixed versus programmable and flow- versus pressure-regulating valves, the latter in each analysis had significantly lower malfunction and total complication rates.
Conclusions: Programmable and pressure regulating devices may lead to lower shunt malfunction and total complication rates. Proper patient selection should guide valve choice. Future prospective studies may further elucidate the difference in complication rates between these various shunt designs.
Keywords: Fixed, Flow regulating, Programmable, Siphon control, Ventriculoperitoneal shunt
INTRODUCTION
Cerebrospinal fluid (CSF) diversion through ventriculoperitoneal shunt placement is one of the oldest and most common neurosurgical operations.[
Excessive CSF drainage may occur in the upright position, increasing the hydrostatic, gravitational pressure of the shunt system, and thereby leading to headaches, nausea, vomiting, impaired cognition, multiple hospitalizations, and repeated surgeries.[
In more severe cases, as CSF drains through the shunt, bridging veins can be stretched and subsequently tear, causing subdural effusions or hematomas, with incidences ranging from 3 to 33%.[
Variables influencing CSF flow through a shunt include intracranial pressure, intra-abdominal pressure, hydrostatic pressure (“siphon effect”), as well as shunt system factors such as valve setting and tubing patency.[
MATERIALS AND METHODS
After obtaining Institutional Review Board approval, a retrospective study through chart review was performed for all adult ventriculoperitoneal shunts placed at any hospital within the Houston Methodist System from January 2011 to December 2016. Cases were included only if a new valve was placed during surgery either coupled with an initial, entirely new shunt system or with a revision of a prior shunt involving a valve replacement. Ventriculoatrial and ventriculopleural shunts were excluded, due to their rarity within our hospital system.
As most adult shunt-related complications reported in the literature occur in the first 6 months, chart reviews were performed to identify complications occurring within 6 months of the operative date, including infection, shunt malfunction (proximal catheter, valve, or distal catheter), subdural hematoma formation, and any other shunt-related issue.[
The cases were organized and analyzed in the following groups: SC versus NSC; flow versus pressure-control; and fixed versus programmable. Mean age between the SC and NSC groups was compared through student’s t-test. Demographics and complications rates were analyzed through Fisher’s exact test to compare SC versus NSC, flow versus pressure regulating valves, and fixed versus programmable valves. Statistical analyses were performed through Microsoft Excel (Microsoft Office 365 MSO, Microsoft Corporation, Redmond, Washington) with P < 0.05 regarded as significant.
In addition, subgroup analyses were performed to compare complication rates between SC and NSC valves in each diagnosis category – normal pressure hydrocephalus (NPH), pseudotumor cerebri (PTC), and hydrocephalus (HCP) – with statistical analysis performed through Fisher’s exact test. The HCP group comprised all patients with diagnoses other than NPH or PTC; this included those with communicating or obstructive HCP related to subarachnoid hemorrhage, tumor-related, aqueductal stenosis, congenital HCP, and more.
RESULTS
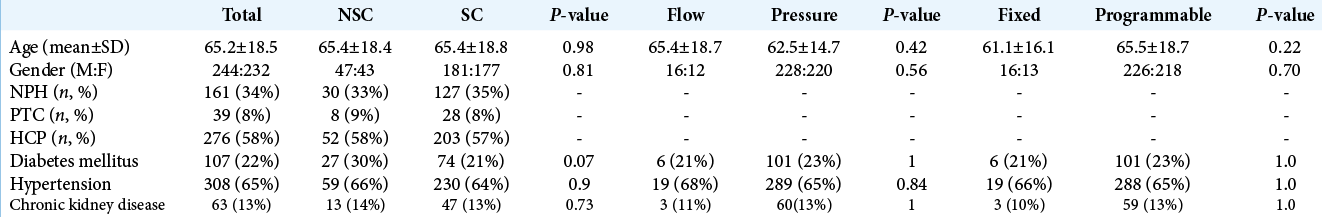
A total of 476 patients met the inclusion criteria. Demographic information is shown in [
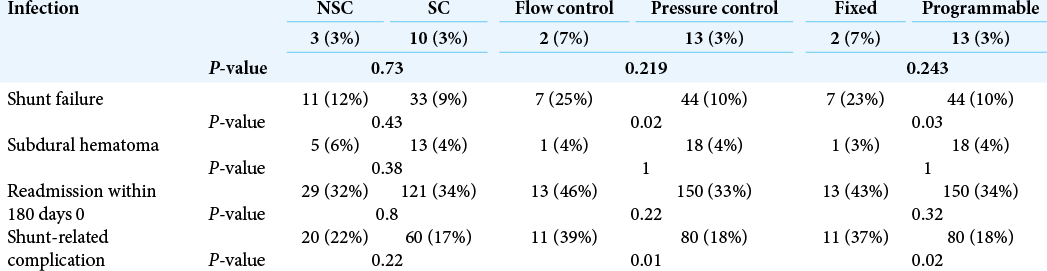
The various complication rates for the different groups are shown in [
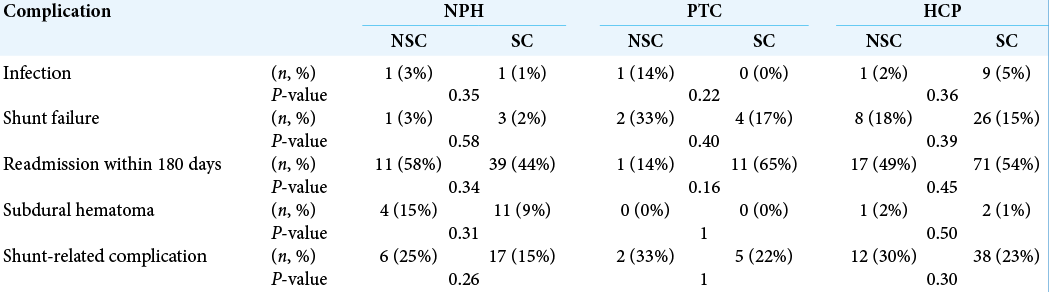
On subgroup analysis for each diagnosis category as shown in [
DISCUSSION
The total complication rate in this study of ventriculoperitoneal shunt surgeries in adults was 19%. The rates of infection, shunt failure, and readmission within 180 days for any reason were 3%, 11%, and 34%, respectively, with no significant difference in any of these variables between SC and NSC. The overall rate of SDH was 4%, and although this rate trended slightly higher in the NSC group relative to SC, this difference was not statistically significant.
Literature overdrainage complication rates range from 3 to 50%.[
Programmable valves represent an alternate development initially geared toward reducing overdrainage complications.[
While several studies suggest a decreased risk of overdrainage with programmable valve, this was not seen in our study possibly due to the low frequency of fixed valve usage.[
Notably, in this study, complications were designated as such not only if they required re-operation but also if they required hospitalization with shunt adjustment only, whether from subdural hygroma development or increased ventricular size. These cases were included as complications as many cases of subdural hematoma development were managed conservatively, but the mere fact that this SDH was symptomatic and required hospitalization merited inclusion as a complication in our view.
No difference was seen between SC and NSC valves in our adult population in terms of infections, malfunctions, subdural hematomas, readmissions within 180 days, or total complications. Higher malfunction and total complication rates were seen with flow- versus pressure-regulating valves and fixed versus programmable valves, with no difference in rates of infection, subdural hematoma, or readmission within 180 days.
The retrospective nature of this review limited a thorough assessment of patients’ clinical responses to CSF diversion and may have missed a number of subdural hygromas managed conservatively in the outpatient setting through adjustment of programmable valve setting. In addition, the true causative factors for SDH development – whether over-shunting versus traumatic – are unknown. Finally, multiple surgeons within a single city-wide hospital system performed the shunt operations; given that each surgeon may favor a certain valve type over others, this may present a confounding factor in the analysis.
CONCLUSIONS
The overall complication rate in this study was 19%. No difference was seen in complication rates between SC and NSC valves. Increased malfunction and total shunt-related complication rates were seen when comparing flow- versus pressure-regulated valves and fixed versus programmable valves. Proper patient selection should guide valve choice to minimize rates of under- and over-drainage. Future prospective studies may further elucidate the difference in complication rates between SC and NSC valves.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgments
The authors would like to thank Chika Ezeana, Shenyi Chen, and Mamta Puppala for data collection and organization.
References
1. Agarwal N, Kashkoush A, McDowell MM, Lariviere WR, Ismail N, Friedlander RM. Comparative durability and costs analysis of ventricular shunts. J Neurosurg. 2018. p. 1-8
2. Freimann FB, Vajkoczy P, Sprung C. Patients benefit from low-pressure settings enabled by gravitational valves in normal pressure hydrocephalus. Clin Neurol Neurosurg. 2013. 115: 1982-6
3. Kaestner S, Kruschat T, Nitzsche N, Deinsberger W. Gravitational shunt units may cause under-drainage in bedridden patients. Acta Neurochir (Wien). 2009. 151: 217-21
4. Kiefer M, Eymann R, Meier U. Five years experience with gravitational shunts in chronic hydrocephalus of adults. Acta Neurochir (Wien). 2002. 144: 755-67
5. Kondageski C, Thompson D, Reynolds M, Hayward RD. Experience with the Strata valve in the management of shunt overdrainage. J Neurosurg. 2007. 106: 95-102
6. Korinek AM, Fulla-Oller L, Boch AL, Golmard JL, Hadiji B, Puybasset L. Morbidity of ventricular cerebrospinal fluid shunt surgery in adults: An 8-year study. Neurosurgery. 2011. 68: 985-94
7. Kurtom KH, Magram G. Siphon regulatory devices: Their role in the treatment of hydrocephalus. Neurosurg Focus. 2007. 22: E5
8. Lee L, King NK, Kumar D, Ng YP, Rao J, Ng H. Use of programmable versus nonprogrammable shunts in the management of hydrocephalus secondary to aneurysmal subarachnoid hemorrhage: A retrospective study with cost-benefit analysis. J Neurosurg. 2014. 121: 899-903
9. Lemcke J, Meier U, Muller C, Fritsch MJ, Kehler U, Langer N. Safety and efficacy of gravitational shunt valves in patients with idiopathic normal pressure hydrocephalus: A pragmatic, randomised, open label, multicentre trial (SVASONA). J Neurol Neurosurg Psychiatry. 2013. 84: 850-7
10. Lemcke J, Meier U. Improved outcome in shunted iNPH with a combination of a Codman Hakim programmable valve and an aesculap-miethke shunt assistant. Cent Eur Neurosurg. 2010. 71: 113-6
11. McDowell MM, Chiang MC, Agarwal N, Friedlander RM, Wecht DA. Exclusive use of fixed pressure valves for cerebrospinal fluid diversion in a modern adult cohort. Heliyon. 2018. 4: e01099
12. Merkler AE, Ch’ang J, Parker WE, Murthy SB, Kamel H. The rate of complications after ventriculoperitoneal shunt surgery. World Neurosurg. 2017. 98: 654-8
13. Miyake H. Shunt devices for the treatment of adult hydrocephalus: Recent progress and characteristics. Neurol Med Chir (Tokyo). 2016. 56: 274-83
14. Mpakopoulou M, Brotis AG, Gatos H, Paterakis K, Fountas KN. Ten years of clinical experience in the use of fixed-pressure versus programmable valves: A retrospective study of 159 patients. Acta Neurochir Suppl. 2012. 113: 25-8
15. O’Kelly CJ, Kulkarni AV, Austin PC, Urbach D, Wallace MC. Shunt-dependent hydrocephalus after aneurysmal subarachnoid hemorrhage: Incidence, predictors, and revision rates. Clinical article. J Neurosurg. 2009. 111: 1029-35
16. Pereira RM, Suguimoto MT, Oliveira MF, Tornai JB, Amaral RA, Teixeira MJ. Performance of the fixed pressure valve with antisiphon device SPHERA® in the treatment of normal pressure hydrocephalus and prevention of overdrainage. Arq Neuropsiquiatr. 2016. 74: 55-61
17. Pinto FC, Pereira RM, Saad F, Teixeira MJ. Performance of fixed-pressure valve with antisiphon device SPHERA(®) in hydrocephalus treatment and overdrainage prevention. Arq Neuropsiquiatr. 2012. 70: 704-9
18. Portnoy HD, Schulte RR, Fox JL, Croissant PD, Tripp L. Anti-siphon and reversible occlusion valves for shunting in hydrocephalus and preventing post-shunt subdural hematomas. J Neurosurg. 1973. 38: 729-38
19. Puca A, Anile C, Maira G, Rossi G. Cerebrospinal fluid shunting for hydrocephalus in the adult: Factors related to shunt revision. Neurosurgery. 1991. 29: 822-6
20. Reddy GK, Bollam P, Caldito G. Long-term outcomes of ventriculoperitoneal shunt surgery in patients with hydrocephalus. World Neurosurg. 2014. 81: 404-10
21. Reddy GK, Bollam P, Shi R, Guthikonda B, Nanda A. Management of adult hydrocephalus with ventriculoperitoneal shunts: Long-term single-institution experience. Neurosurgery. 2011. 69: 774-80
22. Reddy GK. Ventriculoperitoneal shunt surgery and the incidence of shunt revision in adult patients with hemorrhage-related hydrocephalus. Clin Neurol Neurosurg. 2012. 114: 1211-6
23. Reinprecht A, Czech T, Dietrich W. Clinical experience with a new pressure-adjustable shunt valve. Acta Neurochir (Wien). 1995. 134: 119-24
24. Ringel F, Schramm J, Meyer B. Comparison of programmable shunt valves vs standard valves for communicating hydrocephalus of adults: A retrospective analysis of 407 patients. Surg Neurol. 2005. 63: 36-41
25. Saehle T, Farahmand D, Eide PK, Tisell M, Wikkelso C. A randomized controlled dual-center trial on shunt complications in idiopathic normal-pressure hydrocephalus treated with gradually reduced or fixed pressure valve settings. J Neurosurg. 2014. 121: 1257-63
26. Serarslan Y, Yilmaz A, Cakir M, Guzel E, Akakin A, Guzel A. Use of programmable versus nonprogrammable shunts in the management of normal pressure hydrocephalus: A multicenter retrospective study with cost-benefit analysis in Turkey. Medicine (Baltimore). 2017. 96: e8185
27. Sindou M, Guyotat-Pelissou I, Chidiac A, Goutelle A. Transcutaneous pressure adjustable valve for the treatment of hydrocephalus and arachnoid cysts in adults. Experiences with 75 Cases. Acta Neurochir (Wien). 1993. 121: 135-9
28. Trinh VT, Duckworth EA. Revision to an adjustable non-siphon control valve in low pressure hydrocephalus: Therapeutic siphoning and a new perspective on NPH: Series of 3 cases and review of the literature. Clin Neurol Neurosurg. 2013. 115: 175-8
29. Wu Y, Green NL, Wrensch MR, Zhao S, Gupta N. Ventriculoperitoneal shunt complications in California: 1990 to 2000. Neurosurgery. 2007. 61: 557-62
30. Zemack G, Romner B. Adjustable valves in normal-pressure hydrocephalus: A retrospective study of 218 patients. Neurosurgery. 2008. 62: 677-87
31. Zemack G, Romner B. Seven years of clinical experience with the programmable Codman Hakim valve: A retrospective study of 583 patients. J Neurosurg. 2000. 92: 941-8