- Department of Surgery, Santa Casa de Sao Paulo School of Medical Sciences, Rua Dr. Cesário Motta Júnior, São Paulo, Brazil.
DOI:10.25259/SNI_550_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Danilo Almeida Silva, Guilherme Brasileiro de Aguiar, Maurício Jory, Mario Luiz Marques Conti, José Carlos Esteves Veiga. “Whiplash” cervical trauma with fracture and migration of carotid stent fragments. 08-Oct-2020;11:329
How to cite this URL: Danilo Almeida Silva, Guilherme Brasileiro de Aguiar, Maurício Jory, Mario Luiz Marques Conti, José Carlos Esteves Veiga. “Whiplash” cervical trauma with fracture and migration of carotid stent fragments. 08-Oct-2020;11:329. Available from: https://surgicalneurologyint.com/surgicalint-articles/10316/
Abstract
Background: Angioplasty using a carotid stent is a treatment modality for carotid stenosis, with results similar to those obtained with endarterectomy, as demonstrated by important studies. The increasing use of this procedure has also led to a larger number of reports of complications, stent fractures among those. Stent fracture is a rare manifestation and hence needs further studying so that its actual prevalence can be determined, as well as its associated risk factors and proper clinical management. The current study reports the case of a patient who had previously undergone angioplasty with a carotid stent and, after an automobile accident, presented with a stent fracture and distal embolization of fragments thereof with neurological manifestation.
Case Description: A male patient, 40 years old, presented with a history of previously stent carotid angioplasty. He had been involved in an automobile accident and suffered a stent fracture with distal fragment migration. As he was an asymptomatic patient (NIHSS 0, Rankin zero), we opted for a conservative treatment with oral anticoagulant.
Conclusion: Angioplasty is an effective treatment for extracranial atherosclerosis and, albeit rare, stent fractures can result in the migration of fragments thereof. This occurrence should be suspected in patients who have sustained severe neck injuries due to sudden deceleration and may be associated with thromboembolism.
Keywords: Carotid artery injuries, Carotid stenosis, Cerebrovascular trauma, Intracranial embolism, Prostheses and implants, Stents
INTRODUCTION
Angioplasty coupled to carotid stent placement is a therapeutic option for the treatment of carotid stenosis having long- and medium-term results similar to those yielded by endarterectomy.[
Endovascular stent fractures are one of the possible complications and have been described in multiple topographies.[
CASE DESCRIPTION
Male patient, 40 years old, dyslipidemic, presented with a right carotid territory transient ischemic attack 7 months prior. At the time, he underwent diagnostic investigation during which there was found evidence of moderate stenosis (about 60%) in the right carotid bulb associated with an ulcerated plaque. Double antiplatelet aggregation therapy was then prescribed with aspirin and clopidogrel and the use of statins, in addition to angioplasty with a 7 × 40 mm carotid wall stent. He progressed without complications and was discharged after 3 days without sequelae.
The patient had been involved in an automobile accident (a collision between a car and a pole) and was referred to the emergency room, with no neurological deficit at the time of admission. Tomography and angiotomography scans of both the neck and skull were performed and revealed signs of thrombosis/occlusion of the bifurcation of the right internal carotid artery, close to the origin of the middle cerebral artery.
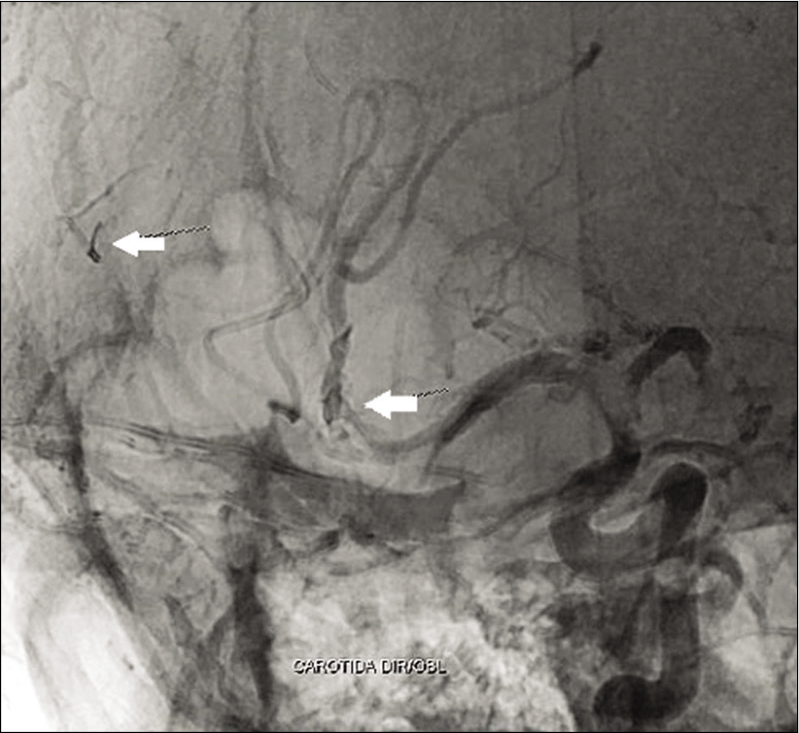
Subsequently, he underwent cerebral angiography that showed multiple fractures in the stent and a small metallic image in the topography of a branch of the right lingual artery, which is suggestive of a fragment thereof [
As he was an asymptomatic patient (NIHSS 0, Rankin zero), we opted for a conservative treatment with oral anticoagulant and a target international normalized ratio (INR) between 2.0 and 3.0.
DISCUSSION
Endovascular stent fractures can occur in different topographies, but they usually occur in areas having arteries with great flexibility and exposed to repetitive movements.[
According to Vos et al.,[
Stent fractures are still a poorly studied event. The occurrence rate ranges from 0% to 29%,[
The asymptomatic carotid trial (ACT-1) carried out by Weinberg et al.[
The presence of thick and irregular calcification plaques makes it difficult to place the stent, as these prevent the device from fully expanding. The irregularity of the calcified plaque causes tension points on the stent’s external wall, and this tension can be exacerbated by neck movements.[
In their review article published in 2010, Sfyroeras et al.[
We present herein the case of a patient who had a stent fracture that was detected following severe trauma (i.e ., after being a victim in an automobile x pole collision). The sudden deceleration (“whiplash”) may have triggered the fracture accompanied by migration of small fragments thereof. To date, there is little information in the literature about the management of patients with carotid stent fractures. Despite having no reports of stent fractures associated to degenerative cervical spine disease, degenerative deformities of cervical spine, like spondylosis, might contribute to increase external forces against carotid wall and then could enhance chances of stent fractures after a trauma. Further studies are needed to evaluate cervical spine degenerative disorders and its association with carotid stent fractures.
Carotid Doppler ultrasonography is the test used for the clinical follow-up of patients who have undergone stent angioplasty. When in-stent restenosis is suspected, it is important to request imaging tests that visualize the stent’s structure, given that restenosis may be associated with fractures.[
The limited information regarding management of carotid stent fractures[
In cases of fractures associated with in-stent restenosis in asymptomatic patients, it is likely that the clinical follow-up alone will suffice.[
In situations where the fracture is associated with thrombus formation, the placement of a new stent should be avoided due to the risk of distal embolization.[
In the case herein presented, the placement of another stent and mechanical thrombectomy was not indicated due to the risk that new fragments could migrate. Anticoagulant treatment was chosen because the patient was asymptomatic, and thrombi were distally present.
CONCLUSION
Most studies on angioplasty accompanied by the placement of a carotid stent do not aim to assess the structural behavior of stents overtime. Angioplasty is an effective treatment for extracranial atherosclerosis and, albeit rare, stent fractures can result in the migration of fragments thereof. This occurrence should be suspected in patients who have sustained severe neck injuries due to sudden deceleration and may be associated with thromboembolism.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Boehm G, Gschwendtner M, Schillinger M. Carotid stent fracture: Diagnosis and management. Catheter Cardiovasc Interv. 2009. 74: 273-7
2. Brott TG, Hobson RW, Howard G, Roubin GS, Clark WM, Brooks W. Stenting versus endarterectomy for treatment of carotid-artery stenosis. N Engl J Med. 2010. 363: 11-23
3. Brott TG, Howard G, Roubin GS, Meschia JF, Mackey A, Brooks W. Long-term results of stenting versus endarterectomy for carotid-artery stenosis. N Engl J Med. 2016. 374: 1021-31
4. Chang CK, Huded CP, Nolan BW, Powel RJ. Prevalence and clinical significance of stent fracture and deformation following carotid artery stenting. J Vasc Surg. 2011. 54: 685-90
5. Garcia-Toca M, Rodriguez HE, Naughton PA, Keeling A, Phade SV, Morasch MD. Are carotid stent fractures clinically significant?. Cardiovasc Intervent Radiol. 2012. 35: 263-7
6. Ling AJ, Mwipatayi P, Gandhi T, Sieunarine K. Stenting for carotid artery stenosis: Fractures, proposed etiology and the need for surveillance. J Vasc Surg. 2008. 47: 1220-6
7. Nazzal M, Abbas J, Nazzal M, Afridi S, Ritter M. Fractured internal carotid artery stent. Vascular. 2008. 16: 179-82
8. Sfyroeras GS, Koutsiaris A, Karathanos C, Giannakopoulos A, Giannoukas AD. Clinical relevance and treatment of carotid stent fractures. J Vasc Surg. 2010. 51: 1280-5
9. Valibhoy AR, Mwipatayi BP, Sieunarine K. Fracture of a carotid stent: An unexpected complication. J Vasc Surg. 2007. 45: 603-6
10. Vos JA, Vos AW, Linsen MA, Marcus JT, Overtoom TT, van den Berg JC. Impact of head movements on morphology and flow in the internal carotid artery after carotid angioplasty and stenting versus endarterectomy. J Vasc Surg. 2005. 41: 469-75
11. Weinberg I, Beckman JA, Matsumura JS, Rosenfield K, Ansel GM, Chaturvedi S. Carotid stent fractures are not associated with adverse events: Results from the ACT-1 multicenter randomized trial (carotid angioplasty and stenting versus endarterectomy in asymptomatic subjects who are at standard risk for carotid endarterectomy with significant extracranial carotid stenotic disease). Circulation. 2018. 137: 49-56