- Department of Neurosurgery, University Medical Center Regensburg, Regensburg, Germany
Correspondence Address:
Julius Höhne
Department of Neurosurgery, University Medical Center Regensburg, Regensburg, Germany
DOI:10.4103/2152-7806.195234
Copyright: © 2016 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Julius Höhne, Alexander Brawanski, Karl-Michael Schebesch. Fluorescein sodium-guided surgery of a brain abscess: A case report. 05-Dec-2016;7:
How to cite this URL: Julius Höhne, Alexander Brawanski, Karl-Michael Schebesch. Fluorescein sodium-guided surgery of a brain abscess: A case report. 05-Dec-2016;7:. Available from: http://surgicalneurologyint.com/surgicalint_articles/fluorescein-sodium%e2%80%91guided-surgery-of-a-brain-abscess-a-case-report/
Abstract
Background:Up to now, the feasibility and benefit of using fluorescein sodium under a dedicated surgical microscope filter (YE560, YELLOW 560 nm filter, Carl Zeiss Meditec, Germany) has never been clinically evaluated in infectious disorders of the brain.
Case Description:Here, we report the case of a male patient with a brain abscess in the right parietal lobe that was removed under fluorescence-guidance (intravenous administration of fluorescein sodium 10%, 5 mg/kg bodyweight). The abscess capsule showed intensive yellow fluorescent staining, while − under white light − the cortex appeared normal.
Conclusion:This technique may improve the identification and surgical removal of brain abscesses.
Keywords: Blood–brain barrier, brain abscess, fluorescein sodium, fluorescence-guided surgery, YELLOW 560 nm filter
INTRODUCTION
Fluorescein sodium (FL) has been increasingly used in oncologic neurosurgery, and its benefit has been repeatedly confirmed for high grade gliomas, brain metastases, and cerebral lymphomas.[
However, to the best of our knowledge, the application of FL under the YE560 filter has never been evaluated for the visualization and removal of a brain abscess. Here, we report the rare case of a male patient with a brain abscess who was microsurgically treated with FL/YE560.
CASE REPORT
A 45-year-old Caucasian male patient presented at our emergency department with headache, visual deficiencies, and moderate disorientation. On the day of the admission, he experienced a convulsive seizure. His medical history was free of any severe infections, immunomodulatory diseases, severe traumas, malignancies, and recent surgical interventions. In the past years, he had not visited any tropical or subtropical areas.
Laboratory parameters on admission were not deranged and physical examination showed normothermia without meningeal irritation. In addition to the visual deficiencies and the mild mnestic impairment, no neurological deficits could be identified.
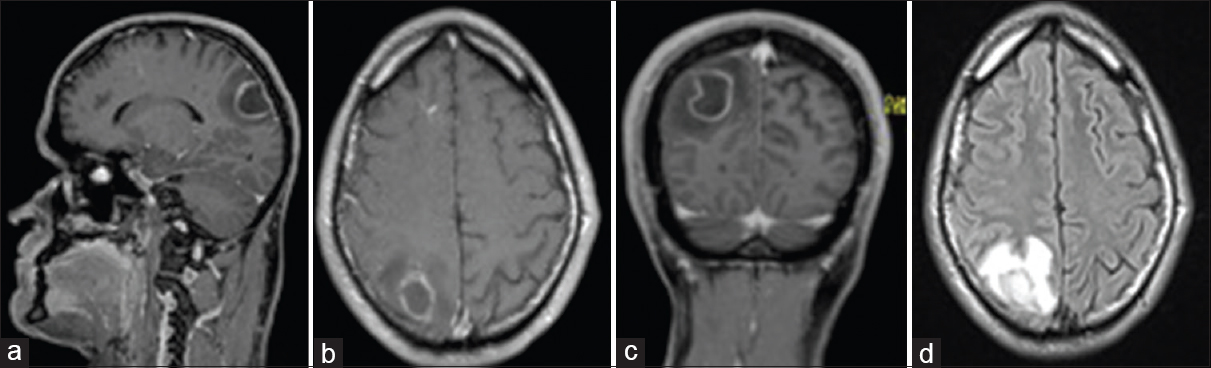
Immediate computed tomography (CT) scan showed a hypodense lesion in the right parietal region. On contrast-enhanced magnetic resonance imaging (MRI), a ring-shaped lesion in the right parietal lobe was noted [Figure
Calculated antibiotic treatment was initiated with amoxicillin/clavulanic acid and metronidazole. The patient was prepared for surgical intervention. The patient was informed regarding the off-label use of FL, and he provided written consent.
Approximately 30–45 minutes prior to skin incision, 5 mg/kg bodyweight of FL (Natrium Fluoreszein® 10%, ALCON, Germany) was administered via the central venous line during induction of anesthesia.
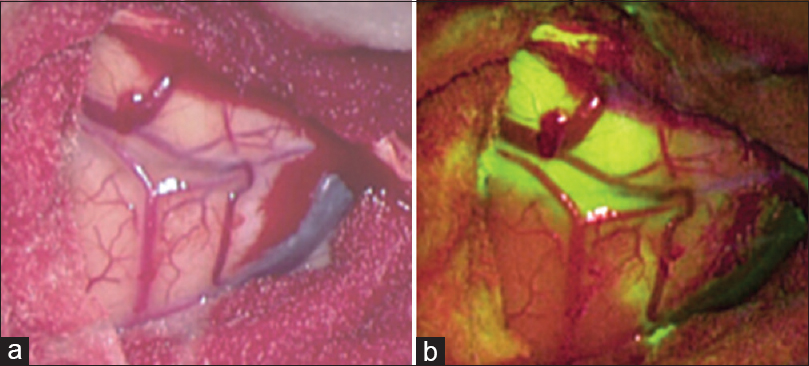
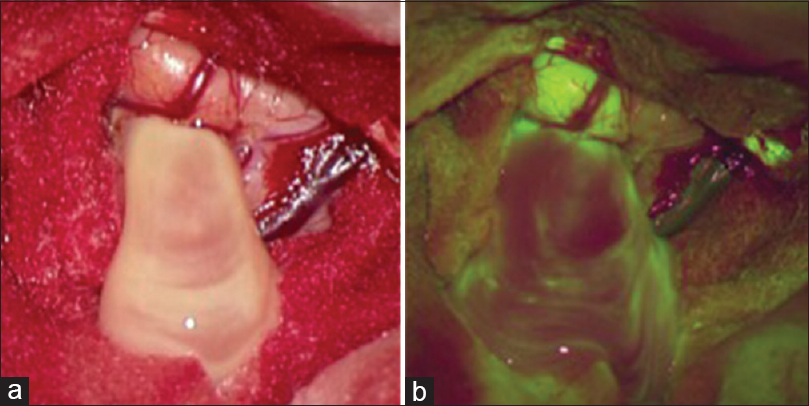
Craniotomy was planned with neuronavigation. After durotomy, the PENTERO 900 surgical microscope was applied. The lesion could not be detected under white light, however, showed intensive fluorescent staining under the YE560 nm filter [Figure
The postoperative course was uneventful. Because no microbiological specimen could be identified, calculated antibiotic treatment was continued. The visual deficiencies and the mnestic impairment completely resolved, and the patient was discharged after 5 weeks.
DISCUSSION
Many literature reports have described the feasibility and benefit of FL under the YE560 or in confocal laser-endomicroscopy in malignant brain tumors.[
In high-grade gliomas and cerebral metastases, the BBB is severely disrupted.[
The American surgeon George E. Moore pioneered FL-guided surgery.[
Many authors assumed that lesions with contrast-enhancement in the T1-weighted MR sequence excellently correspond to intraoperative fluorescence, irrespective of the biological and histological etiology of the lesion. For brain abscesses, however, this finding has only been confirmed experimentally but not clinically.
CONCLUSION
To the best of our knowledge, this is the first report evaluating the effect of FL under a dedicated microscope filter in a patient with a solid infectious lesion of the brain. In future, this technique can help identify subcortical or deeply located abscess formations and may be beneficial in increasing the rate of complete resection of abscess capsules. It is noteworthy that perilesional edema, to some degree is also stained yellow and must not be resected.
Financial support and sponsorship
Nil.
Conflicts of interest
Alexander Brawanski and Karl-Michael Schebesch have received speaker's fees from Carl Zeiss Meditec, Oberkochen, Germany.
References
1. Lo WD, McNeely DL, Boesel CW. Blood-brain barrier permeability in an experimental model of bacterial cerebritis. Neurosurgery. 1991. 29: 888-92
2. Martirosyan NL, Eschbacher JM, Kalani MY, Turner JD, Belykh E, Spetzler RF. Prospective evaluation of the utility of intraoperative confocal laser endomicroscopy in patients with brain neoplasms using fluorescein sodium: Experience with 74 cases. Neurosurg Focus. 2016. 40: E11-
3. Moore GE. Fluorescein as an Agent in the Differentiation of Normal and Malignant Tissues. Science. 1947. 106: 130-1
4. Moore GE, Peyton WT, French LA, Walker WW. The clinical use of fluorescein in neurosurgery; the localization of brain tumors. J Neurosurg. 1948. 5: 392-8
5. Nakagawa Y, Shinno K, Okajima K, Matsumoto K. Perifocal brain oedema in experimental brain abscess in rats. Acta Neurochir Suppl. 1990. 51: 381-2
6. Nduom EK, Yang C, Merrill MJ, Zhuang Z, Lonser RR. Characterization of the blood-brain barrier of metastatic and primary malignant neoplasms. J Neurosurg. 2013. 119: 427-33
7. Schebesch KM, Brawanski A, Hohenberger C, Hohne J. Fluorescein Sodium-Guided Surgery of Malignant Brain Tumors: History, Current Concepts, and Future Project. Turk Neurosurg. 2016. 26: 185-94