- Department of Neurosurgery, Hospital Privado de Rosario, Rosario, Argentina
- Department of Plastic and Reconstructive Surgery, Hospital Privado de Rosario, Rosario, Argentina
- Department of Neuroradiology, Hospital Privado de Rosario, Rosario, Argentina
Correspondence Address:
Ignacio J. Barrenechea, Department of Neurosurgery, Hospital Privado de Rosario, Rosario, Argentina.
DOI:10.25259/SNI_895_2024
Copyright: © 2025 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Ignacio J. Barrenechea1, Micaela Clerici2, César Cordero Ramírez2, Luis Márquez1, Sabrina C. Miralles3, Ernesto Adrian Moretti2. Anterior rotation of the temporalis muscle for prevention of temporal hollowing in cranial surgeries: Esthetic and patient-reported outcomes. 14-Mar-2025;16:90
How to cite this URL: Ignacio J. Barrenechea1, Micaela Clerici2, César Cordero Ramírez2, Luis Márquez1, Sabrina C. Miralles3, Ernesto Adrian Moretti2. Anterior rotation of the temporalis muscle for prevention of temporal hollowing in cranial surgeries: Esthetic and patient-reported outcomes. 14-Mar-2025;16:90. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=13438
Abstract
BackgroundTemporal hollowing is a common cosmetic complication following pterional craniotomies. To address this issue, we evaluated the efficacy of anterior rotation of the temporalis muscle at closure. Although this technique is not new and has been generally reported, no research studies have been conducted to evaluate its objective and patient-reported outcomes in the long term.
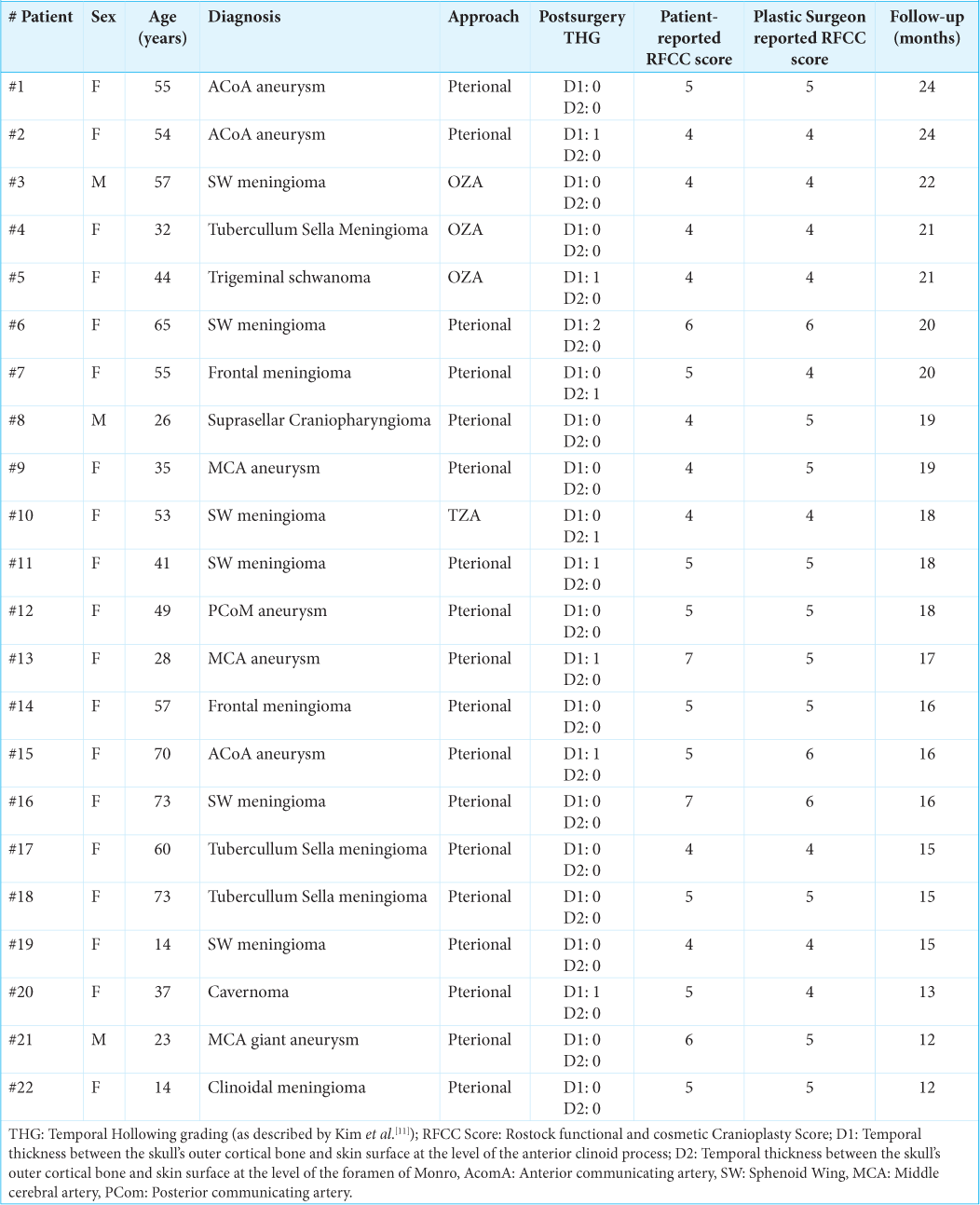
MethodsWe retrospectively reviewed 22 patients treated with pterional, fronto-orbitozygomatic, or frontotemporo-zygomatic craniotomies from March 2021 to 2023. A 12-month postoperative magnetic resonance imaging was used to evaluate the degree of temporal hollowing. To quantify temporal hollowing, we measured the distance of depression at the level of the temporal fossa. This distance, or “temporal thickness,” was defined as the widest distance between the skull’s outer cortical bone and skin surfaces at the level of the anterior clinoid process (D1) and foramen of Monro (D2). Furthermore, pre and postoperative cosmetic results were evaluated using the Rostock Functional and Cosmetic Cranioplasty (RFCC) Score. For reasons of objectivity, RFCC was tested by two independent plastic surgeons against the patient’s rating.
ResultsAfter a year or more follow-up, 54.5% of patients exhibited no hollowing, while 31.8% had mild or moderate hollowing. Moreover, 91% reported good esthetic outcomes. No cases of severe hollowing were observed. Importantly, temporomandibular joint dysfunction was not observed.
ConclusionThese results suggest that anterior rotation of the temporalis muscle is an effective primary strategy to mitigate cosmetic deformities without compromising masticatory function. Further studies with larger sample sizes are warranted to confirm these findings.
Keywords: Etiology, Magnetic resonance imaging clinical score, Prevention, Rostock functional and cosmetic cranioplasty, Temporal hollowing, Temporal muscle rotation, Temporal anatomy, Temporal fat pad
INTRODUCTION
Neurosurgical practice has understandably evolved over the past 20 years. These changes include a trend toward endovascular procedures for vascular lesions, an increasing number of metastatic or skull base tumors treated with stereotactic radiosurgery, or the application of minimally invasive tubular techniques to resect intraaxial tumors. Nevertheless, certain brain or skull base tumors still require “conventional approaches” (pterional, orbitozygomatic, etc.). However, the current trends and patient’s expectations require special attention to cosmetic results. Considering that these approaches sometimes require extensive temporalis muscle detachment to expose the temporal fossa, surgeons have developed various techniques to avoid temporal hollowing, a frequent cosmetic problem reported to occur in 87–100% of pterional craniotomies.[
Several techniques have been proposed to address this problem, such as split myofascial bone flap, interfascial pterional craniotomy, or avoidance of dissection beneath the superficial layer of deep temporal fascia or through the temporal fat pad. To overcome this issue, the authors have been utilizing anterior rotation of the temporalis muscle at closure to counterbalance the unavoidable muscle atrophy. Although this technique is not new and has been generally reported elsewhere,[
MATERIALS AND METHODS
This retrospective case series study has been reported in line with the PROCESS guidelines.[
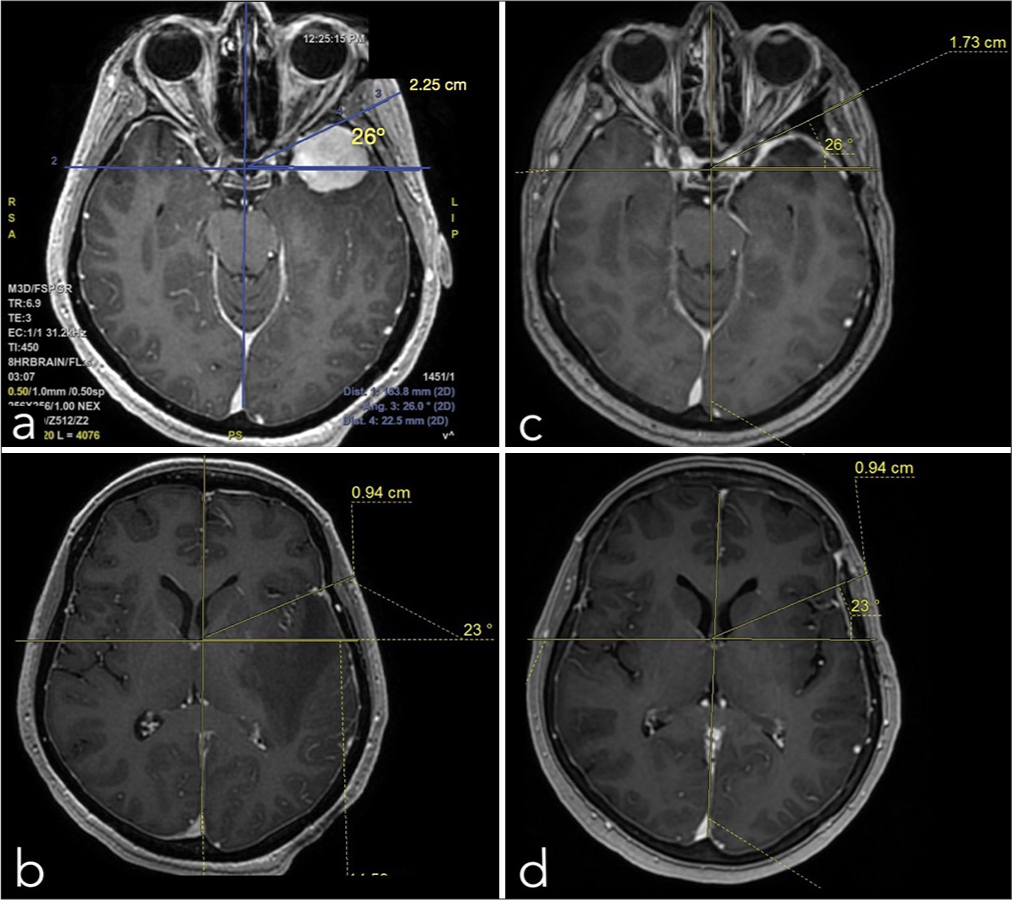
Figure 1:
Pre (a;b) and postoperative (c;d) temporal thickness magnetic resonance imaging measurements (example case # 11). This distance was defined as the widest distance between the skull’s outer cortical bone and skin surfaces at the level of the anterior clinoid process (D1) and at the level of the foramen of Monro (D2). To avoid errors between pre and postoperative measurements, we used the same angle drawn from the intersection of the midline and a horizontal line (in the x plane) crossing the sella turcica in D1. In D2, the center of the angle was the intersection of the midline and a horizontal line (in the x plane) crossing the foramina of Monro.
Surgical technique
After general anesthesia was induced, the patient was placed in a supine position, with their head rotated and secured in a Mayfield head holder. The skin incision began 1.0–1.5 cm anterior to the ear at the level of the zygomatic arch, extending superiorly across the temporal region. Afterward, it curved anteriorly (posterior to the hairline) to end at the midline or the contralateral pupillary line, depending on the required exposure. Preservation of the frontotemporal branch of the facial nerve was achieved through an interfascial dissection technique, as described by Yasargil et al.[
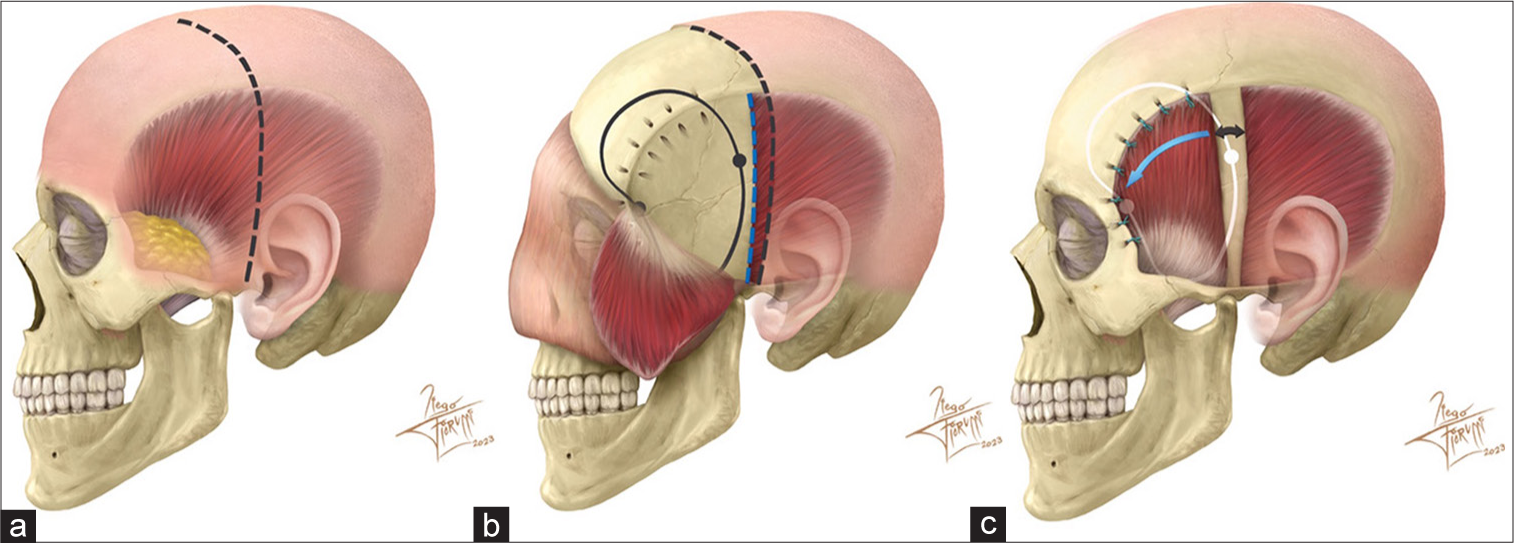
Figure 2:
Original artistic drawing of the reported technique. (a) Classic left pterional approach incision. (b) Flap and temporalis muscle reflection. Note the v-shaped tunnels drilled in the outer cortex along the superior temporal line. (c) Final temporalis muscle position. The muscle is rotated anteriorly (blue arrow), leaving a gap behind (double head black arrow). Several 2-0 Ethibond stitches are placed through the v-shaped tunnels to anchor the muscle back to the superior temporal line. Bone cement is used in burr holes and bone gaps to avoid long-term cosmetic scalp defects.
RESULTS
Twenty-two patients were operated using this cosmetic technique at closure. The patient group consisted of 19 female and 3 male patients with an average age of 46.1 ± 3.2 years (±Enhanced Surveillance Measures) and a median follow-up of 18 months (range 12–24 months). Details of the cohort are detailed in
At the last follow-up, among 22 patients, 54.5% (12 patients) showed grade 0 for both D1 and D2 measures. In addition, 7 patients (31.8%) exhibited grades 1 and 2 for D1 measures (6 with “mild hollowing” and 1 with “moderate hollowing”), while their D2 measures were classified as grade 0 (““no hollowing”). Only 3 patients (13.6%) displayed grade 2 (“moderate hollowing”) for D2, which was worse than their D1 distance indicating no hollowing; 19/22 patients (86.4%) were classified as “no hollowing” at D2 measure, and no cases of “severe hollowing” were registered neither at D1 or D2 measures; Kappa index: −0.222/1.0 (95% confidence interval [CI]: −0.782 to 0.337). The inclusion of a 0 value within the 95% CI suggested no relationship [
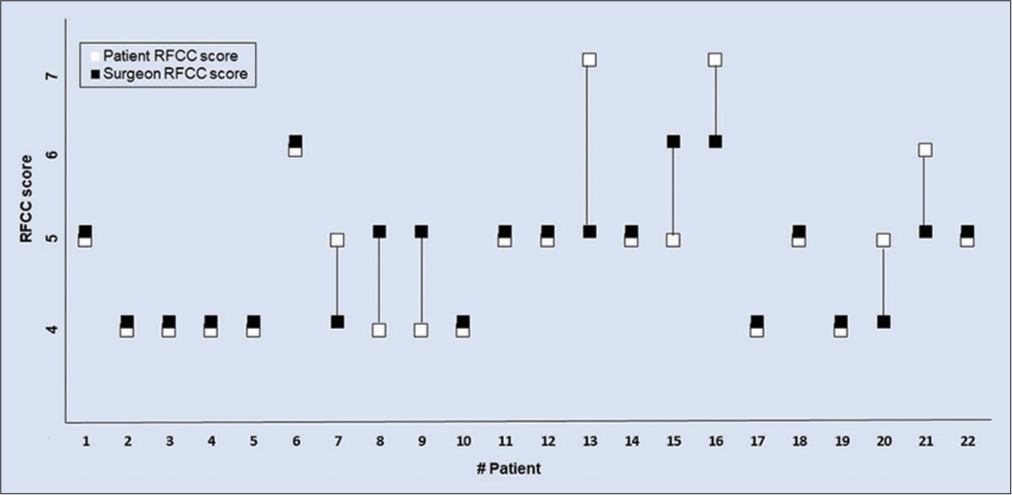
The surgeons and patient RFCC scores were measured; 20/22 (91%) patient scores and 20/22 (91%) plastic surgeon scores stated as “good postoperative results” in terms of appearance; in only 2/22 (9%) cases and plastic surgeon qualified as “acceptable results.” Specifically,
In all cases, the operated temporalis fossa showed a discrete bulging for several months (compared to the nonoperated side). After that time, both sides remained nearly even. Of note, no external defects were seen at the muscle gap level [
Figure 4:
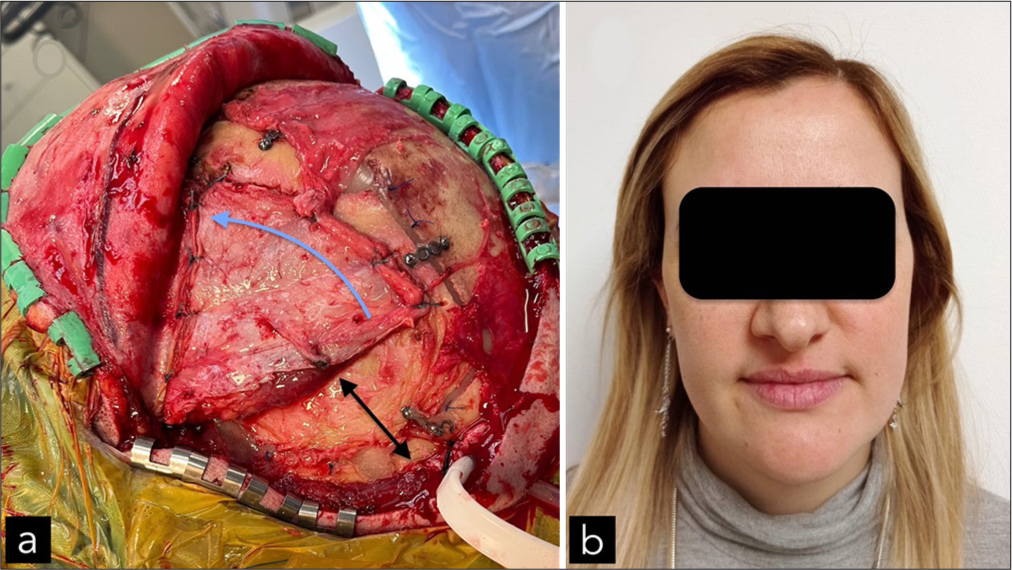
Case # 9. (a) Intraoperative picture of the final reconstruction before scalp closure. The muscle is thoroughly sutured to the superior temporal line. In this case, the zygoma was not exposed. However, the anterior cut over the temporalis fascia was closed with Ethibon. The muscle is rotated anteriorly (blue arrow), leaving a gap behind (double head black arrow). (b) At the 19-month follow-up, the patient was satisfied with the temporal contours.
DISCUSSION
Pterional or orbitozygomatic craniotomies are commonly used surgical procedures to access the intracranial compartment and treat various conditions, such as tumors, aneurysms, and arteriovenous malformations. One of the main complications of these procedures is temporal hollowing, which occurs due to retraction, denervation, or devascularization of the temporalis muscle during the surgery. Besides, injury to the superficial temporal fat pad (a quadrangular fan-shaped structure) contributes to this problem.[
Although the temporalis muscle is anchored back in a different position, no patient reported temporomandibular pain and/or functional jaw limitations. This finding further emphasizes the utility of this technique since some authors reported these symptoms after pterional approaches.[
CONCLUSION
In this initial series, 91% of patients reported good postoperative results, with no cases of severe hollowing registered. We conclude, therefore, that anterior rotation of the temporalis muscle at closure remains a useful primary prevention strategy for mitigating temporal hollowing following pterional, OZA, or TZC approaches. However, it would be important to extend the follow-up period for these patients and proceed with the development of case series studies involving larger sample sizes. Subsequently, comparative studies with other established techniques should be undertaken for a comprehensive evaluation.
Ethical approval
The research/study was approved by the Institutional Review Board at Comité de Ética de Grupo Gamma, number 1/0151, dated July 10, 2024.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.
References
1. Agha RA, Sohrabi C, Mathew G, Franchi T, Kerwan A, O’Neill N. The PROCESS 2020 guideline: Updating consensus preferred reporting of CasESeries in surgery (PROCESS) guidelines. Int J Surg. 2020. 84: 231-5
2. Barone CM, Jimenez DF, Boschert MT. Temporalis muscle resuspension using titanium miniplates and screws: Technical note. Neurosurgery. 2001. 48: 450-1
3. Camarata JC, Wang PT. Hair sparing techniques and scalp flap design. Neurosurg Clin N Am. 2002. 13: 411-9
4. Chang LS, Kim YH, Kim SW. Correction of temporal hollowing deformity using serratus anterior muscle flap. Biomed Res Int. 2022. 2022: 9523629
5. Choudhry OJ, Christiano LD, Arnaout O, Adel JG, Liu JK. Reconstruction of pterional defects after frontotemporal and orbitozygomatic craniotomy using Medpor Titan implant: Cosmetic results in 98 patients. Clin Neurol Neurosurg. 2013. 115: 1716-20
6. De Andrade Júnior FC, de Andrade FC, de Araujo Filho CM, Carcagnolo Filho J. Dysfunction of the temporalis muscle after pterional craniotomy for intracranial aneurysms. Comparative, prospective and randomized study of one flap versus two flaps dieresis. Arq Neuropsiquiatr. 1998. 56: 200-5
7. Henker C, Hoppmann MC, Sherman MU, Glass A, Piek J. Validation of a novel clinical score: The rostock functional and cosmetic cranioplasty score. J Neurotrauma. 2018. 35: 1030-6
8. Hönig JF. V-tunnel drill system in craniofacial surgery: A new technique for anchoring the detached temporalis muscle. J Craniofac Surg. 1996. 7: 168-9
9. Kadri PA, Al-Mefty O. The anatomical basis for surgical preservation of temporal muscle. J Neurosurg. 2004. 100: 517-22
10. Kim E, Delashaw JB. Osteoplastic pterional craniotomy revisited. Neurosurgery. 2011. 68: 125-9 discussion 129
11. Kim JH, Lee R, Shin CH, Kim HK, Han YS. Temporal augmentation with calvarial onlay graft during pterional craniotomy for prevention of temporal hollowing. Arch Craniofac Surg. 2018. 19: 94-101
12. Kim S, Matic DB. The anatomy of temporal hollowing: The superficial temporal fat pad. J Craniofac Surg. 2005. 16: 760-3
13. Mericli AF, Gampper TJ. Treatment of postsurgical temporal hollowing with high-density porous polyethylene. J Craniofac Surg. 2014. 25: 563-7
14. Oikawa S, Mizuno M, Muraoka S, Kobayashi S. Retrograde dissection of the temporalis muscle preventing muscle atrophy for pterional craniotomy. Technical note. J Neurosurg. 1996. 84: 297-9
15. Park J, Hamm IS. Cortical osteotomy technique for mobilizing the temporal muscle in pterional craniotomies. Technical note. J Neurosurg. 2005. 102: 174-8
16. Rocha-Filho PA, Fujarra FJ, Gherpelli JL, Rabello GD, de Siqueira JT. The long-term effect of craniotomy on temporalis muscle function. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007. 104: e17-21
17. Santiago GF, Terner J, Wolff A, Teixeira J, Brem H, Huang J. Post-neurosurgical temporal deformities: Various techniques for correction and associated complications. J Craniofac Surg. 2018. 29: 1723-9
18. Spetzler RF, Lee KS. Reconstruction of the temporalis muscle for the pterional craniotomy. Technical note. J Neurosurg. 1990. 73: 636-7
19. Vaca EE, Purnell CA, Gosain AK, Alghoul MS. Postoperative temporal hollowing: Is there a surgical approach that prevents this complication? A systematic review and anatomic illustration. J Plast Reconstr Aesthet Surg. 2017. 70: 401-15
20. Yasargil MG, Reichman MV, Kubik S. Preservation of the frontotemporal branch of the facial nerve using the interfascial temporalis flap for pterional craniotomy. Technical article. J Neurosurg. 1987. 67: 463-6
21. Zager EL, DelVecchio DA, Bartlett SP. Temporal muscle microfixation in pterional craniotomies. Technical note. J Neurosurg. 1993. 79: 946-7