- Department of Neurosurgery, Toyama University Hospital, Sugitani, Toyama, Japan
- Department of Neurosurgery, University of Toyama, Sugitani, Toyama, Japan.
Correspondence Address:
Daina Kashiwazaki, Department of Neurosurgery, Toyama University Hospital, Sugitani, Toyama, Japan.
DOI:10.25259/SNI_224_2023
Copyright: © 2023 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Kunitaka Maruyama1, Daina Kashiwazaki1, Shusuke Yamamoto1, Naoki Akioka2, Emiko Hori2, Satoshi Kuroda2. Coil embolization for post-bypass aneurysm of middle meningeal artery for moyamoya disease – preservation of transdural anastomosis. 28-Apr-2023;14:157
How to cite this URL: Kunitaka Maruyama1, Daina Kashiwazaki1, Shusuke Yamamoto1, Naoki Akioka2, Emiko Hori2, Satoshi Kuroda2. Coil embolization for post-bypass aneurysm of middle meningeal artery for moyamoya disease – preservation of transdural anastomosis. 28-Apr-2023;14:157. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=12294
Abstract
Background: Middle meningeal artery (MMA) pseudoaneurysm following revascularization surgery for moyamoya disease (MMD) is rare.
Case Description: Here, a 29-year-old man presented with an MMA pseudoaneurysm after he underwent revascularization surgery (superficial temporal artery-to-middle cerebral artery bypass and encephalo-duro-myoarterio-pericranial synangiosis) for hemorrhagic MMD. At 3 months post-surgery, digital subtraction angiography showed a pseudoaneurysm in the right MMA. Transdural anastomosis to the parietal and occipital lobes was opacified at the distal MMA of the pseudoaneurysm. Intra-aneurysmal coil embolization was performed for preservation of transdural anastomosis. The postoperative course was uneventful. At 1 month post-embolization, angiography revealed an entirely occluded pseudoaneurysm.
Conclusion: An increase in blood flow in the MMA due to bypass surgery may accelerate aneurysm development by increasing the hemodynamic stress. This case suggested that intra-aneurysmal embolization may be a potential treatment.
Keywords: Endovascular treatment, Moyamoya disease, Pseudoaneurysm
INTRODUCTION
Moyamoya disease (MMD) is an uncommon cerebrovascular disorder characterized by progressive occlusion of the internal carotid artery and its main branches within the circle of Willis.[
CASE PRESENTATION
A 29-year-old man was referred to our hospital for MMD treatment. The patient had experienced transient left-sided hemiparesis when he was 11-years-old, and he was eventually diagnosed with MMD at 12 years of age. He was prescribed aspirin at a previous hospital. Sixteen years had passed uneventfully; however, at 28 years of age, he presented with a sudden headache. Computed tomography revealed right thalamic hemorrhage with ventricular hemorrhage [
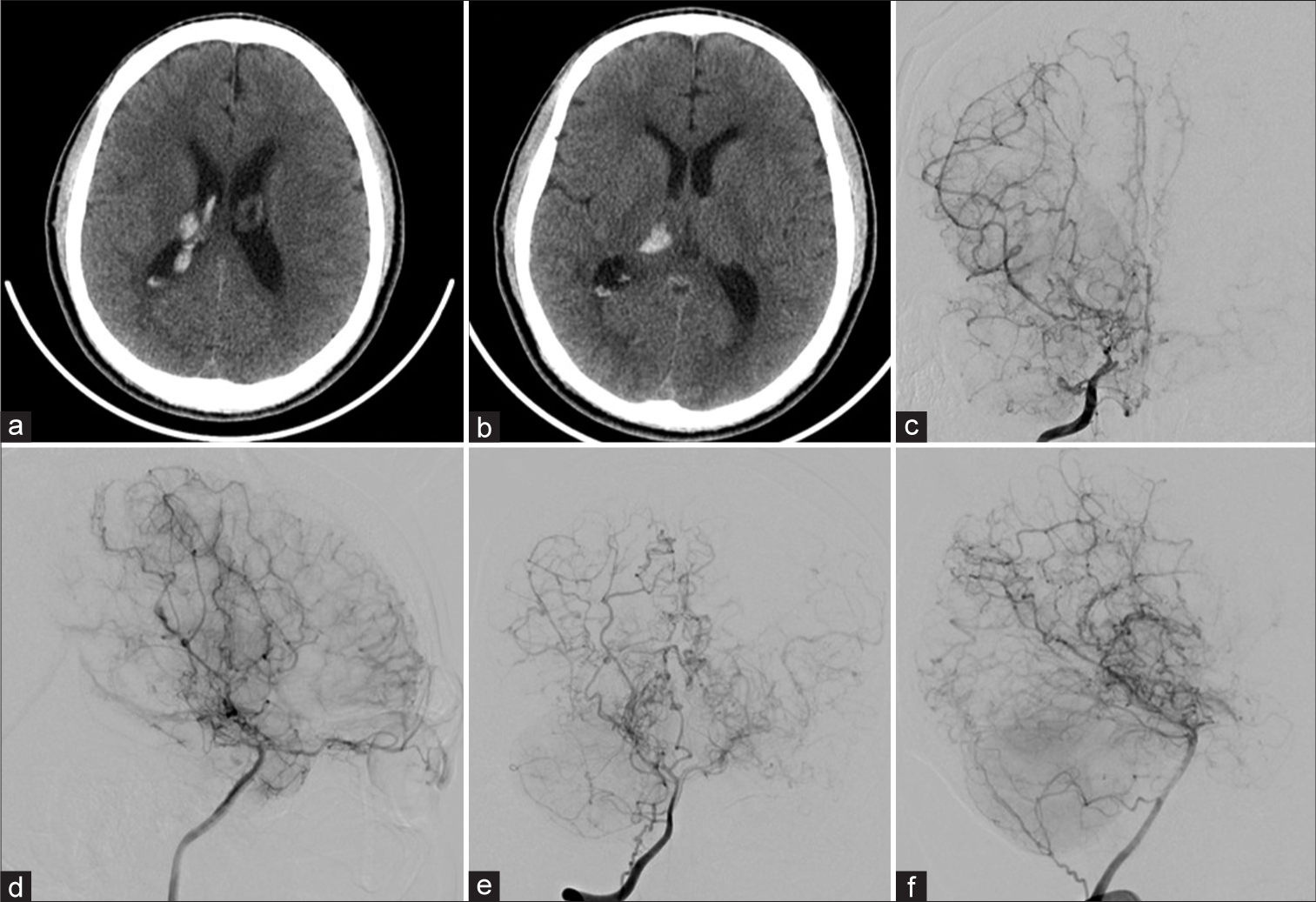
Figure 1:
(a and b) Computed tomography revealing thalamic hemorrhage. (c) Anterior-posterior and (d) lateral angiography of the right internal carotid artery before bypass surgery showing Suzuki grade 4 moyamoya disease. (e) Anterior-posterior and (f) lateral angiography of the right vertebral artery demonstrating development of the thalamic channel.
Figure 2:
(a) Anterior-posterior angiography before revascularization surgery. (b) Lateral angiography of the right external carotid artery at 3 months after revascularization surgery. The angiogram shows a pseudoaneurysm (arrowheads, b) at the middle meningeal artery (arrows, a and b). The diameter of the middle meningeal artery at 6 months after the superficial temporal artery-to-middle cerebral artery (STAMCA) bypass and encephalo-duro-myo-arterio-pericranio-synangiosis (EDMAPS) was larger than that before surgery. (c) Fusion image of computed tomography and right external carotid artery angiography. The pseudoaneurysm is located at the edge of the craniotomy (black arrow). (d) Intraoperative photo of STA-MCA bypass and EDMAPS. The arrow is location of pseudoaneurysm hereafter.
Endovascular treatment for MMA pseudoaneurysm
We planned to perform the internal trapping under general anesthesia. After intravenous administration of 4000 U of heparin, the right external carotid artery was catheterized with a 4-Fr guiding sheath (ASAHI FUZBUKI, Asahi Intech, Japan). Subsequently, a distal access catheter (Guidepost, Tokai Medical Products, Japan) and microcatheter (Echelon-10, Medtronic, USA) were navigated into the right MMA. Microangiography of the posterior trunk of MMA revealed transdural anastomosis by indirect bypass [
Figure 3:
(a) Right middle meningeal artery (MMA) angiography shows the indirect bypass to the parietal and occipital lobe. The pseudoaneurysm is located at the posterior branch of the MMA (black arrow). (b) The working angle of coil embolization. The aneurysm size is 4.2 mm × 3.9 mm and neck length is 1.1 mm (black arrow) (c) Intra-aneurysmal embolization using platinum coils. (d) Post-embolization angiography of the MMA reveals patency of the posterior branch of the MMA. (e and f) Follow-up angiography at 1 month after pseudoaneurysm embolization. Complete occlusion of the aneurysm and patency of the middle meningeal artery is observed.
The microcatheter was navigated into the pseudoaneurysm, and the pseudoaneurysm was embolized using five platinum coils (Optima Coil System™, BALT, USA) [
DISCUSSION
In this study, we present a rare case of MMA pseudoaneurysm after STA-MCA bypass and EDMAPS for MMD. Endovascular coil embolization with preservation of transdural anastomosis was successfully performed for the treatment of the MMA pseudoaneurysm. We further discuss the mechanism of MMA pseudoaneurysm formation and its treatment strategy.
Development of MMA pseudoaneurysm following revascularization surgery for MMD
Surgical revascularization for MMD is a widely accepted treatment due to the extremely high rate of recurrent stroke associated with MMD.[
Treatment for MMA pseudoaneurysm
In the current case, the treatment of the MMA pseudoaneurysm was prioritized due to the high risk of rupture, which can be fatal. Seo et al.[
Several treatment options are available for pseudoaneurysms of the MMA, such as surgical trapping and endovascular treatment. Park et al.[
CONCLUSION
Pseudoaneurysm formation after revascularization surgery for MMD is an infrequent but possible complication. The mechanism of pseudoaneurysm formation in such cases may be related to the increased blood flow resulting from transdural anastomosis. Intra-aneurysmal embolization with preservation of transdural anastomosis may be a possible treatment strategy for MMA pseudoaneurysm occurrence following revascularization surgery for MMD.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.
References
1. Bruneau M, Gustin T, Zekhnini K, Gilliard C. Traumatic false aneurysm of the middle meningeal artery causing an intracerebral hemorrhage: Case report and literature review. Surg Neurol. 2002. 57: 174-8 discussion 178
2. Fujimura M, Kaneta T, Mugikura S, Shimizu H, Tominaga T. Temporary neurologic deterioration due to cerebral hyperperfusion after superficial temporal artery-middle cerebral artery anastomosis in patients with adult-onset moyamoya disease. Surg Neurol. 2007. 67: 273-82
3. Funaki T, Takahashi JC, Houkin K, Kuroda S, Fujimura M, Tomata Y. Effect of choroidal collateral vessels on de novo hemorrhage in moyamoya disease: Analysis of nonhemorrhagic hemispheres in the Japan Adult Moyamoya Trial. J Neurosurg. 2019. 132: 408-14
4. Hori S, Kashiwazaki D, Akioka N, Hayashi T, Hori E, Umemura K. Surgical anatomy and preservation of the middle meningeal artery during bypass surgery for moyamoya disease. Acta Neurochir (Wien). 2015. 157: 29-36
5. Ishikawa T, Kamiyama H, Kuroda S, Yasuda H, Nakayama N, Takizawa K. Simultaneous superficial temporal artery to middle cerebral or anterior cerebral artery bypass with pan-synangiosis for Moyamoya disease covering both anterior and middle cerebral artery territories. Neurol Med Chir (Tokyo). 2006. 46: 462-8
6. Karasawa J, Kikuchi H, Furuse S, Kawamura J, Sakaki T. Treatment of moyamoya disease with STA-MCA anastomosis. J Neurosurg. 1978. 49: 679-88
7. Karasawa J, Kikuchi H, Furuse S, Sakaki T, Yoshida Y. A surgical treatment of “moyamoya” disease “encephalo-myo synangiosis”. Neurol Med Chir (Tokyo). 1977. 17: 29-37
8. Khattar NK, White AC, Fortuny EM, Hruska RT, James RF. Management of unruptured traumatic middle meningeal artery pseudoaneurysms through onyx embolization. Cureus. 2017. 9: e1794
9. Kuroda S, Houkin K. Moyamoya disease: Current concepts and future perspectives. Lancet Neurol. 2008. 7: 1056-66
10. Kuroda S, Houkin K, Ishikawa T, Nakayama N, Iwasaki Y. Novel bypass surgery for moyamoya disease using pericranial flap: Its impacts on cerebral hemodynamics and long-term outcome. Neurosurgery. 2010. 66: 1093-101 discussion 101
11. Marvin E, Laws LH, Coppens JR. Ruptured pseudoaneurysm of the middle meningeal artery presenting with a temporal lobe hematoma and a contralateral subdural hematoma. Surg Neurol Int. 2016. 7: S23-7
12. Matsushima Y, Fukai N, Tanaka K, Tsuruoka S, Inaba Y, Aoyagi M. A new surgical treatment of moyamoya disease in children: A preliminary report. Surg Neurol. 1981. 15: 313-20
13. Miyamoto S, Yoshimoto T, Hashimoto N, Okada Y, Tsuji I, Tominaga T. Effects of extracranial-intracranial bypass for patients with hemorrhagic moyamoya disease: Results of the Japan Adult Moyamoya Trial. Stroke. 2014. 45: 1415-21
14. Park YS, Suk JS, Kwon JT. Repeated rupture of a middle meningeal artery aneurysm in moyamoya disease. Case report. J Neurosurg. 2010. 113: 749-52
15. Seo D, Yoon BH, Byun J, Park W, Park JC, Ahn JS. Pseudoaneurysm formation or dural arteriovenous fistula formation at the middle meningeal artery following revascularization surgery in Moyamoya disease. J Cerebrovasc Endovasc Neurosurg. 2023. 25: 87-92
16. Suzuki J, Takaku A. “moyamoya” disease. Disease showing abnormal net-like vessels in base of brain. Arch Neurol. 1969. 20: 288-99