- Department of Neurosurgery, Tokyo Women's Medical University Medical Center East, Tokyo, Japan
Correspondence Address:
Yasuhiro Kuroi
Department of Neurosurgery, Tokyo Women's Medical University Medical Center East, Tokyo, Japan
DOI:10.4103/sni.sni_42_17
Copyright: © 2017 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Yasuhiro Kuroi, Shigeru Tani, Hidenori Ohbuchi, Hidetoshi Kasuya. Microvascular decompression for hypoglossal nerve palsy secondary to vertebral artery compression: A case report and review of the literature. 10-May-2017;8:74
How to cite this URL: Yasuhiro Kuroi, Shigeru Tani, Hidenori Ohbuchi, Hidetoshi Kasuya. Microvascular decompression for hypoglossal nerve palsy secondary to vertebral artery compression: A case report and review of the literature. 10-May-2017;8:74. Available from: http://surgicalneurologyint.com/surgicalint-articles/microvascular-decompression-for-hypoglossal-nerve-palsy-secondary-to-vertebral-artery-compression-a-case-report-and-review-of-the-literature/
Abstract
Background:Neurovascular-compression syndrome (NCS) is described as a prominent pathological contact between cranial nerves and vessels. Trigeminal neuralgia, hemifacial spasm, and glossopharyngeal neuralgia are typical clinical entities associated with NCS. On the other hand, the hyoglossal nerve is rarely affected by NCS.
Case Description:We present a case of hypoglossal nerve palsy (HNP) secondary to vertebral artery (VA) compression. A 47-year-old man presented to our hospital with a 1-month history of dysarthria and dysphagia. Neurological examination revealed left HNP, with an intact swallowing reflex and no oropharyngeal or palatal weakness. Magnetic resonance imaging (constructive interference in steady state) revealed left hypoglossal nerve compression by the V4 segment of the left atherosclerotic VA. He underwent microvascular decompression (MVD) surgery. Intraoperatively, the VA was compressing the hypoglossal nerve. The left VA was moved and attached to the dura matter using a polytetrafluoroethylene (Teflon®) sheet and fibrin glue. Postoperatively, the patient exhibited gradual recovery of HNP in 3 months without dysfunction of lower cranial nerves.
Conclusion:In patients with isolated HNP, vascular compression should be considered as a cause of these symptoms, and subsequent MVD can lead to resolution.
Keywords: Hypoglossal nerve palsy, microvascular decompression, vertebral artery
INTRODUCTION
Neurovascular compression syndromes (NCS) occur when cranial nerves are compressed by intracranial vascular loops. Trigeminal neuralgia, hemifacial spasm, and glossopharyngeal neuralgia are typical clinical entities associated with NCS. These diseases usually occur when the root exit zone of the nerves is affected. Microvascular decompression (MVD) surgery is effective and usually results in immediate postoperative improvement of symptoms. The hyoglossal nerve is rarely affected by NCS, but we encountered a case of hypoglossal nerve palsy (HNP) secondary to vertebral artery (VA) compression.
CASE REPORT
History and examination
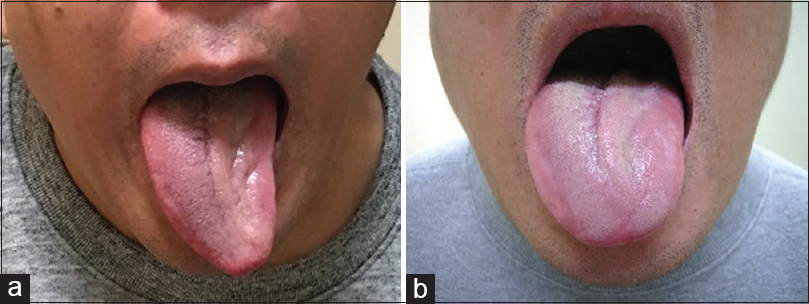
A 47-year-old man presented to our hospital with a 1-month history of dysarthria and dysphagia. He did not show swallowing difficulty, but had subtle difficulty in moving his tongue so that he frequently unintendedly bit his tongue. He had a past history of multiple cerebral aneurysms and had a checkup by angiography 6-months prior to the onset. He consumed alcohol occasionally, and had never smoked cigarettes. Neurological examination revealed isolated left HNP [
Imaging studies
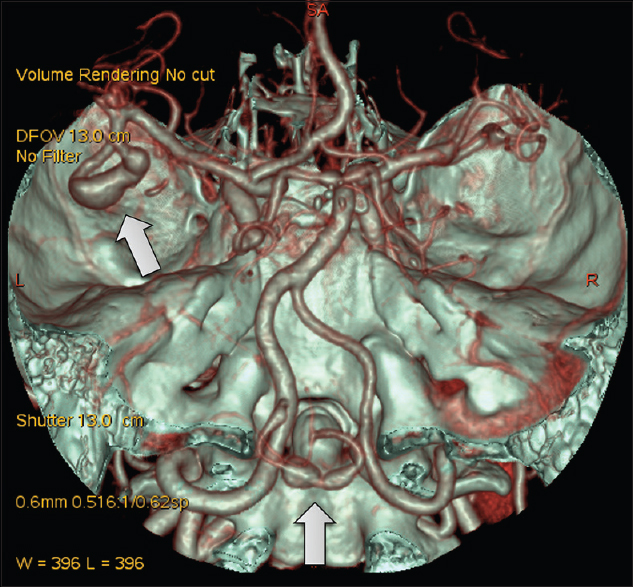
Magnetic resonance imaging (MRI) (CISS, constructive interference in steady state) revealed left hypoglossal nerve compression by the V4 segment of the left atherosclerotic VA [
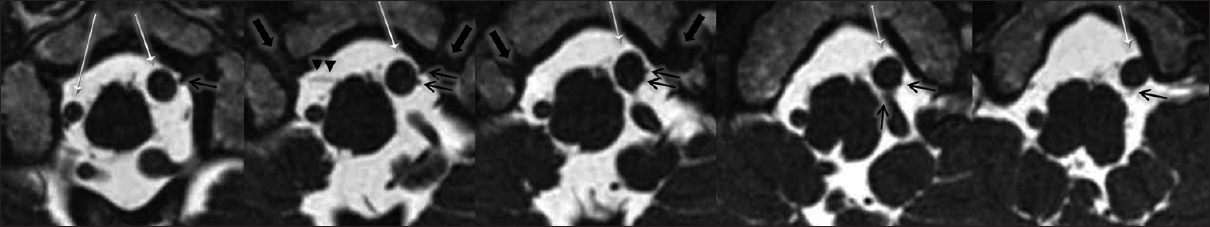
Figure 2
MRI (CISS, constructive interference in steady state) images of the present case. Left hypoglossal nerves (black thin arrows) originated from the ventral side of the medulla oblongata, which is composed of two bundles, and ran into the hypoglossal canal (black thick arrows) beyond the left VA (white thin arrow). It is easy to detect when compared with the contralateral side (arrow head)
Surgical procedure
On the basis of the above diagnosis, he underwent MVD of the left hypoglossal nerve. In a park-bench position, retrosigmoid lateral suboccipital craniotomy enabled us to visualize the glossopharyngeal, vagal, accessory, and hypoglossal nerve together with the VA. Intraoperatively, the VA was compressing the hypoglossal nerve. The hypoglossal nerve was stretched and was extremely thin. The left VA was moved toward the deep side of the surgical field and attached to the dura matter with a polytetrafluoroethylene (Teflon®) sheet and fibrin glue. The left hypoglossal nerve became free from compression after the procedure [Figure
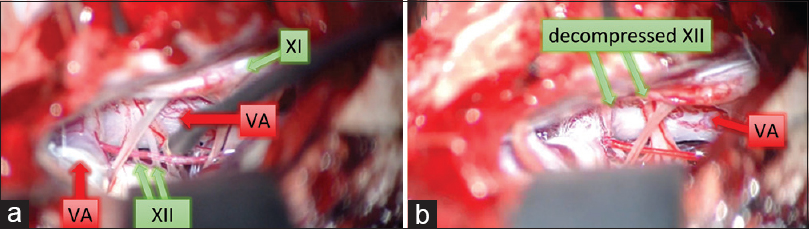
Figure 4
The left vertebral artery compressed the hypoglossal nerve from the deep side of the surgical field to the superficial side. Hypoglossal nerves were stretched by the left VA and became extremely thin (a). The left VA was moved anteriorly and attached to dura using a polytetrafluoroethylene (Teflon®) sheet and fibrin glue. Hypoglossal nerves were released (b)
Postoperative course
He was discharged 7 days after the operation without any obvious complication. At a 3-month postoperative follow-up, he exhibited improvement of hypoglossal nerve palsy without lower cranial nerve dysfunction [
DISCUSSION
Stino et al.[
This pathophysiology was first described in English by Rollnik et al.[
In reviewing previous MRI findings, most of the patients who had conservative therapy show atherosclerotic or ectatic changes of the VA, which was similar to our case study. Thus, we believe atherosclerotic changes to the VA caused hypoglossal nerve compression, finally resulting in HNP in these patients. The fact that their symptoms appeared gradually supports the theory that slowly ongoing atherosclerotic changes caused hypoglossal nerve compression. In those patients, prognosis is good when treated with MVD surgery. Two cases of MVD surgery, including ours, have shown good recovery of tongue deviation after 3 months.[
We also found other interesting case reports with similar pathophysiology. Mahadevappa et al.[
CONCLUSION
To our knowledge, NCS of the hypoglossal nerve is a rare condition. In patients with isolated HNP, vascular compression should be considered as a cause of the symptoms, and subsequent MVD can lead to resolution of the symptoms. We should carefully differentiate HNP due to VA dissection, which can cause similar symptoms, but does not require surgical intervention. As far as we know, this is the first case report with a thorough literature review of hypoglossal nerve palsy by VA compression.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgement
We thank Dr. Benjamin Lo for his excellent advice on the preparation of this manuscript.
References
1. Aladdin Y, Siddiqi ZA, Khan K. Hypoglossal-vertebral entrapment syndrome. Neurology. 2008. 71: 461-
2. Cheong JH, Kim JM, Yang MS, Kim CH. Resolution of isolated unilateral hypoglossal nerve palsy following microvascular decompression of the intracranial vertebral artery. J Korean Neurosurg. 2011. 49: 167-70
3. Graham RM, Thomson EF, Baldwin AJ. Isolated hypoglossal nerve palsy due to a vascular anomaly. Int J Oral Maxillofac Surg. 2007. 36: 759-61
4. Keane JR. Twelfth-nerve palsy. Analysis of 100 cases. Arch Neurol. 1996. 53: 561-6
5. Mahadevappa K, Chacko T, Nair AK. Isolated unilateral hypoglossal nerve palsy due to vertebral artery dissection. Clin Med Res. 2012. 10: 127-30
6. Mckeon A, Murphy S, McNamara B, Ryder DQ, Galvin RJ. Isolated hypoglossal nerve palsy due to compression by a dissecting vertebral artery. Eur Neurol. 2005. 53: 162-4
7. Mokri B, Silbert PL, Schievink WI. Cranial nerve palsy in spontaneous dissection of the extracranial internal carotid artery. Neurology. 1996. 46: 356-9
8. Morini A, Rozza L, Manera V, Buganza M, Tranquillini E, Orrico D. Isolated hypoglossal nerve palsy due to an anomalous vertebral artery course: Report of two cases. Ital J Neurol Sci. 1998. 19: 379-82
9. Rollnik JD, Sindern E, Mosler F, Spring B, Malin JP. Isolated peripheral hypoglossal palsy caused by a kinking of the left vertebral artery (hypoglossal vertebral entrapment syndrome). Eur Neurol. 1996. 36: 324-5
10. Salvi F, Mascalchi M, Plasmati R, Tugnoli V, De Grandis D. Hypoglossal vertebral entrapment syndrome. Muscle Nerve. 1999. 22: 288-9
11. Stino AM, Smith BE, Temkit M, Nagi Reddy S. Hypoglossal nerve palsy: 245 cases. Muscle Nerve. 2016. 54: 1050-4
12. Straube A, Linn J. Unilateral headache attacks and ipsilateral atrophy of the tongue due to neurovascular compression of the hypoglossal nerve. Cephalagia. 2008. 28: 996-8
13. Yamamoto M, Suzuki K, Takekawa H, Hirata K. Isolated hypoglossal nerve palsy caused by neurovascular compression. Intern Med. 2001. 50: 2701-2