- Department of Neurological Surgery, Albert Einstein College of Medicine, Montefiore Medical Center, New York, USA
Correspondence Address:
Merritt D. Kinon
Department of Neurological Surgery, Albert Einstein College of Medicine, Montefiore Medical Center, New York, USA
DOI:10.4103/sni.sni_35_17
Copyright: © 2017 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Merritt D. Kinon, Aleka Scoco, Joaquim M. Farinhas, Andrew Kobets, Karen M. Weidenheim, Reza Yassari, Patrick A. Lasala, Jerome Graber. Glioblastoma multiforme presenting with an open ring pattern of enhancement on MR imaging. 13-Jun-2017;8:106
How to cite this URL: Merritt D. Kinon, Aleka Scoco, Joaquim M. Farinhas, Andrew Kobets, Karen M. Weidenheim, Reza Yassari, Patrick A. Lasala, Jerome Graber. Glioblastoma multiforme presenting with an open ring pattern of enhancement on MR imaging. 13-Jun-2017;8:106. Available from: http://surgicalneurologyint.com/surgicalint-articles/glioblastoma-multiforme-presenting-with-an-open-ring-pattern-of-enhancement-on-mr-imaging/
Abstract
Background:Intracerebral ring enhancing lesions can be the presentation of a variety of pathologies, including neoplasia, inflammation, and autoimmune demyelination. Use of a precise diagnostic algorithm is imperative in correctly treating these lesions and minimizing potential adverse treatment effects.
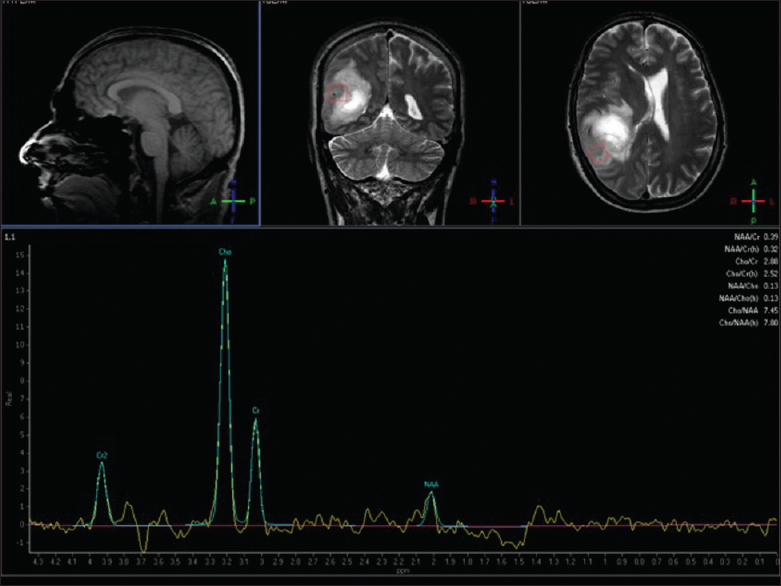
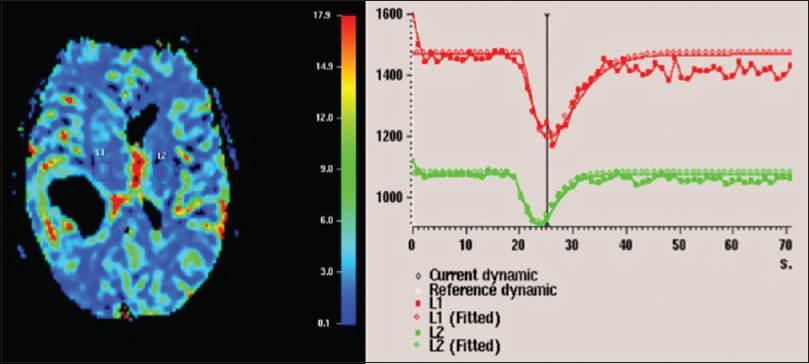
Case Description:A 55-year-old patient presented to the hospital with complaints of a post-concussive syndrome and a non-focal neurologic exam. Imaging revealed a lesion with an open ring enhancement pattern, minimal surrounding vasogenic edema, and minimal mass effect. Given the minimal mass effect, small size of the lesion, and nonfocal neurological exam, we elected to pursue a comprehensive noninvasive neurologic workup because our differential ranged from inflammatory/infectious to neoplasm. Over the next 8 weeks, the patient's condition worsened, and repeat imaging showed marked enlargement of the lesion with a now closed ring pattern of enhancement with satellite lesions and a magnetic resonance (MR) spectroscopy and perfusion signature suggestive of neoplasm. The patient was taken to surgery for biopsy and debulking of the lesion. Surgical neuropathology examination revealed glioblastoma multiforme.
Conclusion:The unique open ring enhancement pattern of this lesion on initial imaging is highly specific for a demyelinating process, however, high-grade glial neoplasms can also present with complex and irregular ring enhancement including an open ring sign. Therefore, other imaging modalities should be used, and close follow-up is warranted when the open ring sign is encountered.
Keywords: Glioblastoma, incomplete peripheral rim enhancement, open-ring sign, radiographic image enhancement, tumefactive demyelination, tumefactive demyelinating lesion
INTRODUCTION
Intracerebral ring enhancing lesions can be a presentation of neoplasia (including metastases, lymphoma, and gliomas), infections, or autoimmune demyelination mimicking neoplasia (tumefactive demyelination), thus posing a diagnostic and management dilemma.[
CASE HISTORY
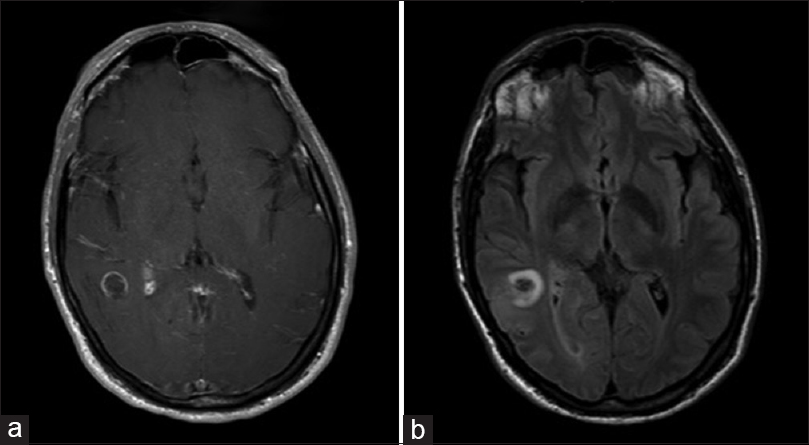
A 55-year-old man presented to an outside institution for treatment of a concussion which he sustained after a fall from a ladder while working in his yard. Initial neurologic examination and magnetic resonance imaging (MRI) of the brain were normal. The patient continued to have concussive symptoms and headache 4 months later. Neurologic exam was still normal, however, repeat MRI revealed a right posterior temporal cystic lesion measuring 1.5 × 1.5 cm with incomplete peripheral enhancement characteristic of an open ring sign [
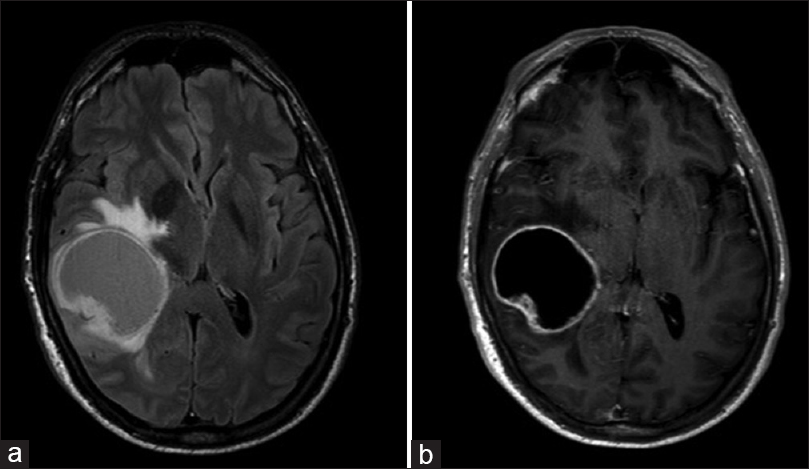
Figure 2
Axial cut MR showing increased size of lesion, measuring 5.3 × 4.2 cm with significant mass effect and surrounding vasogenic edema on T2 FLAIR (a) and a now closed ring pattern of peripheral enhancement on T1 contrast-enchanced image (b). Central cystic component now well-defined and satellite lesions are visible along posterior aspect
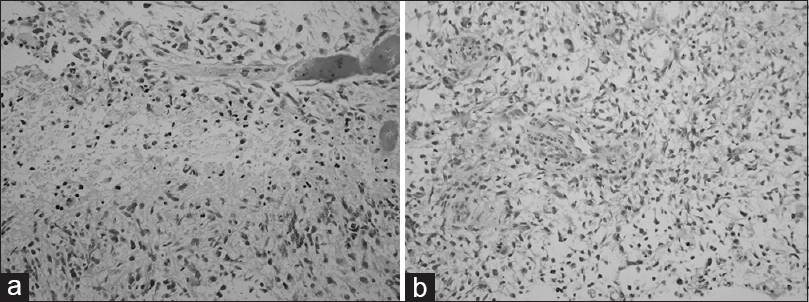
The patient was taken to surgery for a right-sided temporal craniotomy for resection of the mass. Intraoperatively, the lesion was noted to be hemorrhagic with areas of necrosis and thrombosed vessels suggestive of a malignant glial neoplasm. Surgical neuropathology examination showed the lesion to be an infiltrating glial neoplasm with a fibrillary background. Tumor cells had elongated, pleomorphic, vesicular nuclei with scant cytoplasm [Figure
The patient began treatment with standard radiation and temozolomide and was well at the last follow-up 3 months after his diagnosis.
DISCUSSION
Ring-enhancing lesions are usually subcortical or deep. When presenting with associated vasogenic edema and mass effect, these lesions usually favor primary central nervous system neoplasm or abscess. However, demyelinating lesions seen in multiple sclerosis or tumefactive demyelination during the “active phase” of inflammation can also enhance, though the enhancement pattern of these lesions can be faint, with minimal perilesional vasogenic edema, and the enhancing rim may be incomplete.[
This case is a rare example of an open-ring enhancing lesion which evolved from initial presentation to a complete ring-enhancing lesion, which was later confirmed to be glioblastoma multiforme. When trying to identify MR and CT features that distinguish TDLs from glioma or lymphoma, Kim et al. found 4 out of the 13 tumor patients exhibiting focal rim enhancement to have incomplete rings on MR.[
When presented with open-ring enhancing lesions, there is necessity to correlate with other features suggestive of TDL to rule out neoplasm. Such features include T2-weighted iso- and hyperintensity of enhanced regions, absence of mass effect, low relative perfusion, absence of cortical involvement, and CT hypoattenuation of MR enhanced regions.[
CONCLUSION
Open-ring pattern of enhancement is reported to be highly specific for demyelinating lesions, rather than neoplasia. However, high grade glial neoplasms can also present with complex and irregular ring enhancement including an open ring sign. Therefore, other imaging modalities should be used and close follow-up is warranted when the open ring sign is encountered.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Faehndrich J, Weidauer S, Pilatus U, Oszvald A, Zanella FE, Hattingen E. Neuroradiological viewpoint on the diagnostics of space-occupying brain lesions. Clin Neuroradiol. 2011. 21: 123-39
2. Fallah A, Banglawa S, Ebrahim S, Paulseth JE, Jha NK. Tumefactive demyelinating lesions: A diagnostic challenge. Can J Surg. 2010. 53: 69-70
3. Given CA, Stevens BS, Lee C. The MRI Appearance of Tumefactive Demyelinating Lesions. Am J Roentgenol. 2004. 182: 1959-
4. Javalkar V, Manix M, Wilson J, Nanda A. Open ring enhancement in atypical brain demyelination. J Clin Neurosci. 2012. 19: 910-2
5. Kim DS, Na DG, Kim KH, Kim JH, Kim E. Distinguishing tumefactive demyelinating lesions from glioma or central nervous system lymphoma: Added value of unenhanced CT compared with conventional contrast-enhanced MR imaging. Radiology. 2009. 251: 467-75
6. Kimura N, Kumamoto T, Hanaoka T, Hasama Y, Nakamura K, Okazaki T. Monofocal large inflammatory demyelinating lesion, mimicking brain glioma. Clin Neurol Neurosurg. 2009. 111: 296-9
7. Masdeu JC, Quinto C, Olivera C, Tenner M, Leslie D, Visintainer P. Open-ring imaging sign: Highly specific for atypical brain demyelination. Neurology. 2000. 54: 1427-33
8. McAdam LC, Blaser SI, Banwell BL. Pediatric tumefactive demyelination: Case series and review of the literature. Pediatr Neurol. 2002. 26: 18-25
9. Medeiros FC de, Albuquerque LAF de, Pittella JEH, Souza RB de, Gomes Neto AP, Christo PP. Open-Ring Enhancement in Pseudotumoral Multiple Sclerosis: Important Radiological Aspect. Case Rep Neurol Med 2014. 2014. p. 1-5
10. Report C, Akimoto J, Fukuhara H, Suda T, Nagai K, Hashimoto R. Disseminated cerebellar hemangioblastoma in two patients without von Hippel – Lindau disease. Surg Neurol Int. 2014. 5: 145-
11. Riva D, Chiapparini L, Pollo B, Balestrini MR, Massimino M, Milani N. A Case of Child Neurology A Case of Pediatric Tumefactive. J Child Neurol. 2008. 23: 944-7
12. Saindane AM, Cha S, Law M, Xue X, Knopp EA, Zagzag D. Proton MR spectroscopy of tumefactive demyelinating lesions. Am. J. Neuroradiol. 2002. 23: 1378-86
13. Siddiqui A, Sahni A, Khadilkar S. The open-ring sign. Neurol India. 2005. 53: 253-4
14. Sinha M, Garg R, Bhatt M, Chandra A. Tumefactive demyelinating lesion: Experience with two unusual patients. J Postgrad Med. 2010. 56: 146-
15. Zhang D, Hu LB, Henning TD, Ravarani EM, Zou LG, Feng XY. MRI Findings of Primary CNS Lymphoma in 26 Immunocompetent Patients. Korean J Radiol. 2010. 11: 269-