- Departamento de Neurocirurgia, Hospital Mater Dei, Belo Horizonte, Brazil
- Departamento de Neurocirurgia, Federal University of Minas Gerais, Belo Horizonte, Brazil
- Division of Neurological Surgery and Department of Neurosurgery Research, Barrow Neurological Institute, Phoenix, Arizona, USA
Correspondence Address:
Mark C. Preul
Division of Neurological Surgery and Department of Neurosurgery Research, Barrow Neurological Institute, Phoenix, Arizona, USA
DOI:10.4103/2152-7806.161241
Copyright: © 2015 Reis CVC. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.How to cite this article: C. Reis CV, Sebastião N. S. Gusmão, Elhadi AM, Dru A, Uédson Tazinaffo, Zabramski JM, Spetzler RF, Preul MC. Midline as a landmark for the position of the superior sagittal sinus on the cranial vault: An anatomical and imaging study. Surg Neurol Int 21-Jul-2015;6:121
How to cite this URL: C. Reis CV, Sebastião N. S. Gusmão, Elhadi AM, Dru A, Uédson Tazinaffo, Zabramski JM, Spetzler RF, Preul MC. Midline as a landmark for the position of the superior sagittal sinus on the cranial vault: An anatomical and imaging study. Surg Neurol Int 21-Jul-2015;6:121. Available from: http://surgicalneurologyint.com/surgicalint_articles/midline-as-a-landmark-for-the-position-of-the-superior-sagittal-sinus-on-the-cranial-vault-an-anatomical-and-imaging-study/
Abstract
Background:Craniotomies involving the midline are regular practice in neurosurgery, during which injury to the superior sagittal sinus (SSS), an uncommon yet devastating event, may occur. The midline tends to be the most common landmark used to identify the position of the SSS. In this study we examined the reliability of the midline as a landmark for the SSS.
Methods:We performed bilateral craniectomies on eight cadaveric heads, preserving the coronal, sagittal, and lambdoid sutures. The width of the SSS and its displacement from midline were measured on the cadaveric specimens and on 105 normal magnetic resonance images (MRIs) of the head at the following locations: halfway between nasion and bregma (NB), bregma (B), halfway between bregma and lambda (BL), lambda (L), and inion (I).
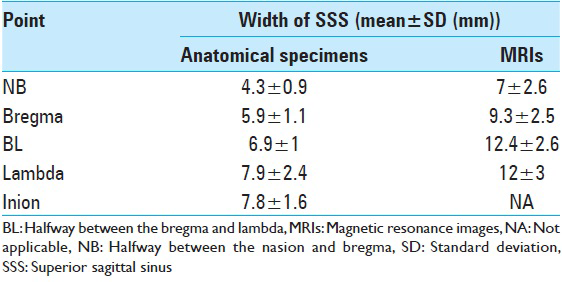
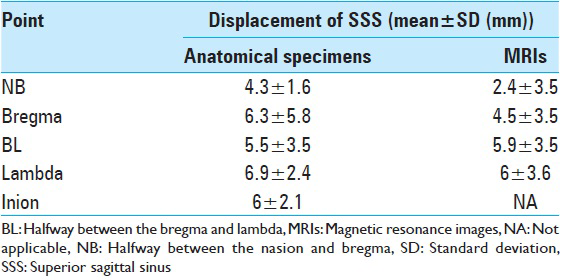
Results:In all cadaveric specimens, the SSS was partially or totally displaced toward one side of midline, usually to the right. It tended to be closer to midline in the frontal region and more displaced posteriorly. The SSS usually drained into the right-side transverse sinus. The mean width of the SSS was 4.3, 5.9, 6.9, 7.9, and 7.8 mm, and the average displacement from midline was 4.3, 6.3, 5.5, 6.9, and 6.0 mm for NB, B, BL, L, and I, respectively. These measurements were then compared with those obtained from the MRIs.
Conclusion:The SSS was consistently displaced on either side of midline. Thus, the midline is not reliable for identifying the SSS, and caution should be used within 6-10 mm on either side of midline.
Keywords: Confluence of sinuses, superior sagittal sinus, sagittal suture, torcular Herophili
INTRODUCTION
Understanding the anatomy of the superior sagittal sinus (SSS) and its position in relation to the midline has been problematic and is poorly understood in the literature.[
Damage to the SSS is a potential complication of any paramedian midline cranial vault approach. Inadvertent injury of the sinus, usually during craniotomy, can lead to severe bleeding. Such injuries are difficult to repair and can result in devastating consequences. To avoid such complications, neurosurgeons typically use the midline, which is the line on the surface of the skull connecting the nasion and the inion, as a reference to estimate the position of the SSS. Correlation between the SSS and the sagittal suture was previously described in the literature;[
In this study, we used anatomical specimens and magnetic resonance images (MRIs) of the head to evaluate the reliability of using the midline as an anatomical reference for the position of the SSS. The results can be used to avoid injuring the SSS during paramedian and midline cranial approaches, especially when intraoperative image guidance is unavailable.
METHODS
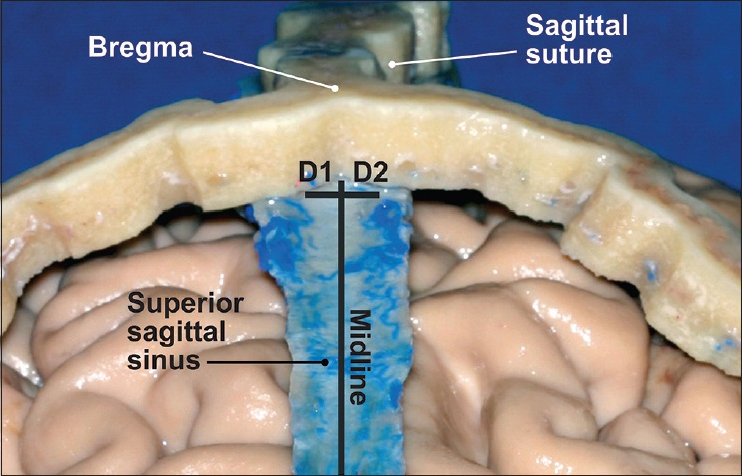
Eight silicone-injected/formalin-fixed Caucasian cadaveric heads were used. All heads were normal in structure, that is, without disease processes of the face, scalp, cranium, or cranial contents. None of the specimens had signs of craniosynostosis or hyperostosis. Major vessels of these specimens were identified and injected with colored silicone to trace the intracranial and extracranial vessels and dural venous sinuses. After reflection of all soft tissue of the scalp, the midline was identified and marked on the skull from the nasion to the inion. A bilateral craniectomy was performed that preserved the coronal, sagittal, and lambdoid sutures. Through a small gap in the sagittal suture, the SSS was exposed completely at five points: (i) Halfway between the nasion and bregma (NB), (ii) bregma (B), (iii) halfway between bregma and lambda (BL), (iv) lambda (L), and (v) inion (I). The roof of the sagittal sinus was opened, and the width of the sinus and any displacement from midline [
We randomly chose 105 normal MRIs of the head from the archives of the Department of Radiology at the Madre Teresa Hospital in Belo Horizonte, Brazil. The sample consisted of 63 women and 42 males, with a mean age of 42.4 years (range, 7–87 years; all patients Caucasian). Studies with intra- and extracranial pathology were excluded. MRIs (postcontrast T1-weighted sequence) were ordered by physicians for other medical reasons and were performed with a Siemens Magnetom Vision 1.5 T scanner (Siemens Corporation, Washington, DC). No special sequences were performed for the purpose of this study that would interfere with the T1-weighted sequence image results.
The landmark used to identify the midline on the images was the longitudinal fissure of the brain. The width of the SSS and its displacement from midline were measured using Voxar 3D (Toshiba Medical Visualization Systems Europe, Ltd., Edinburgh, United Kingdom) software at NB, B, BL, and L. This software enables advanced analysis of the uploaded image sequences in any plane and in large volumetric datasets. This means that image quality and technical tilt of the scan can be eliminated as variables affecting measurement and interpretation.
We also observed which transverse sinus drained the SSS (dominant transverse sinus). The four points of interest were first identified on sagittal MRIs. The measurements were then taken from coronal and/or axial MRIs of the head.
RESULTS
[
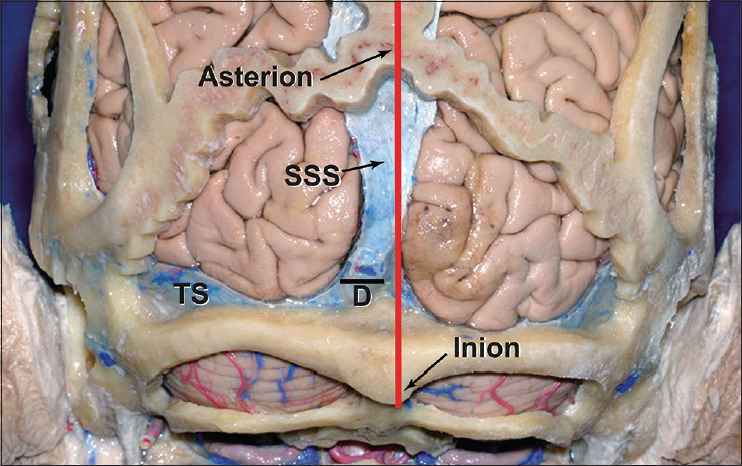
In all specimens, the SSS was a single structure. In one specimen the sagittal suture was deviated to the left of midline. Despite the ectopic sagittal suture, the SSS was related to midline. The lateral displacement of the SSS from midline followed a similar pattern. The lateral displacement of the torcular Herophili to the inion was a mean of 6.0 ± 2.1 mm [
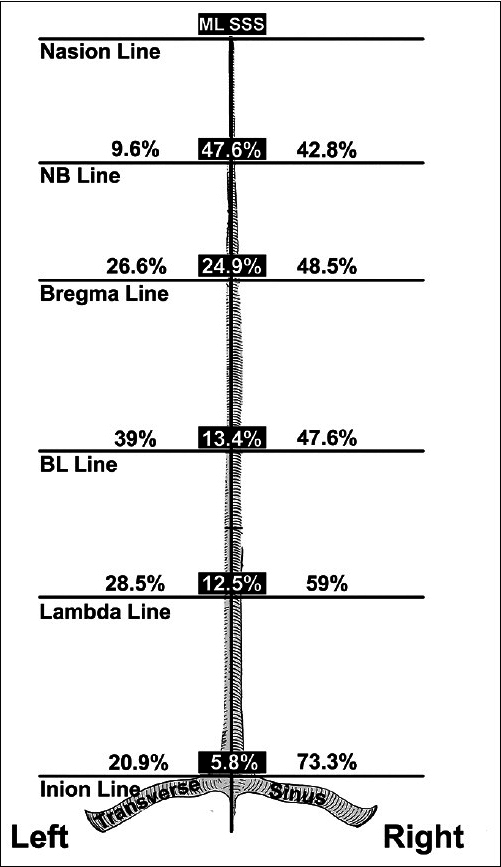
Figure 3
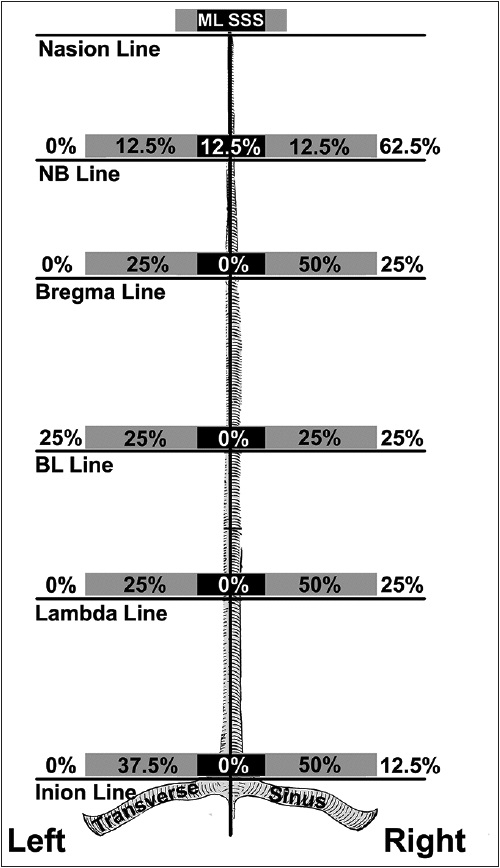
Schematic representation of the displacement of the superior sagittal sinus (SSS) from midline in the anatomical specimens. The frequencies of the SSS exactly at midline are represented in the black shaded areas. Sinuses partially displaced to the left or right are in the gray shaded areas. Sinuses completely displaced toward one side are outside the shaded areas. The midline is represented by the black longitudinal line. NB, halfway between the nasion and bregma; BL, halfway between bregma (B) and lambda (L); ML, midline. Used with permission from Barrow Neurological Institute, Phoenix, Arizona.
The positions of the SSS in relation to the midline in the MRIs are summarized in [
Figure 4
Schematic representation of the displacement of the superior sagittal sinus (SSS) from midline on magnetic resonance images. The frequencies of the SSS exactly at midline are represented in the black shaded areas. The sinuses displaced to the left or right are listed outside the black shaded areas. The midline is represented by the solid black longitudinal line. NB, halfway between the nasion and bregma; BL, halfway between bregma and lambda; ML, midline. Used with permission from Barrow Neurological Institute, Phoenix, Arizona.
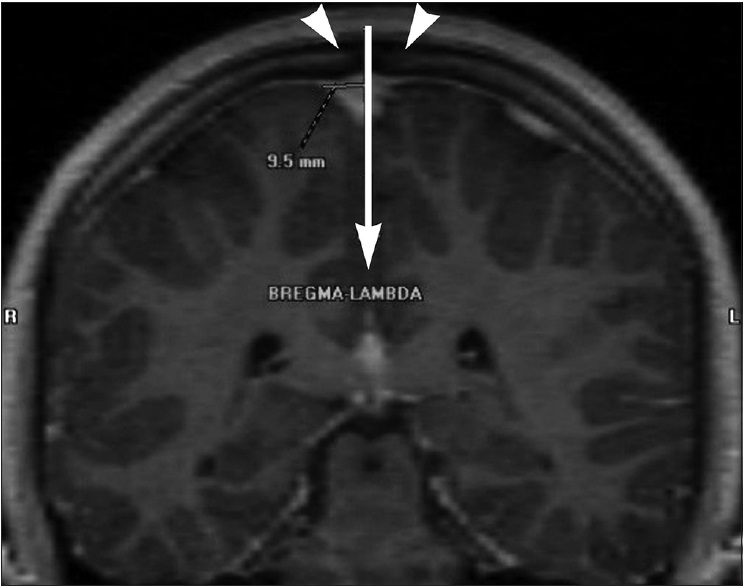
Figure 5
Coronal magnetic resonance image shows the displacement of the superior sagittal sinus toward the right at halfway between bregma and lambda. The sagittal suture is the hypointense gap at the top of the head (arrowheads). Used with permission from Barrow Neurological Institute, Phoenix, Arizona.
DISCUSSION
Historical considerations
The first modern neurosurgical attempt to systematically divide the SSS and illustrate its course was by Harvey Cushing and Louise Eisenhardt in 1938. Initially, Cushing sketched a two-dimensional rendering of the SSS with origin from the crista galli and termination from the torcular Herophili. When he superimposed the approximate location and size of 51 cases of parasagittal global tumors on the drawing, he astutely observed that the SSS could be divided into three regions based on the symptomatology and shared tumor characteristics. The ‘central’ third of the SSS housed 32 of the 51 tumors and consistently had the smallest tumors of the series. In addition, 30 of the 32 cases were associated with convulsive seizures with Jacksonian progression. The ‘frontal’ third of the SSS included 13 of the 51 tumors, and the ‘occipital’ third of the SSS included 6 of the 51 tumors. Tumors in these regions were consistently larger than those found in the central region. According to Cushing, presenting symptoms of tumors in the frontal and occipital zones were identical, with headache and failing vision secondary to optic atrophy in all of the frontal tumor cases and in five of the six occipital cases.[
More recently, angiography of the SSS has led to describing the its sections according to relative quantity of bridging veins (BVs) and direction of drainage of the veins.”[
Anatomical considerations
The SSS is the longest cranial dural venous sinus and extends posteriorly from the crista galli to the sinus confluence at the internal cranial surface. Its mean length ranges from 23 to 30 cm, which makes the dural sinus the most vulnerable to injury.[
The embryology of the SSS is complex. Its position on the cranial vault seems to depend on embryological signals from the falx cerebri between the cerebral hemispheres rather than on signal from the bone at the midline.[
Tubbs et al.[
Unlike these previous studies, we used the midline, which extends backward from the nasion to the inion, as a reference for the position of the SSS. This landmark was chosen for several reasons. First, it is different from the sagittal suture, which can be used only between B and L. In contrast, the midline can be used to estimate the position of the entire length of the SSS, including the segment covered by the suture. Second, the midline is visible on MRI and computed tomography images. Consequently, it is a relevant landmark for estimating the position of the SSS before surgery, especially when image guidance is unavailable. Finally, from an embryological perspective, the position of the SSS seems to be more closely related to the midline than to the sagittal suture.[
Our findings reinforce and expand upon the conclusions of Tubbs et al.[
Traditionally, the inion has been used to estimate the position of the torcular Herophili on the cranial vault. The torcular Herophili is found at one side of the external occipital protuberance, typically on the right side, where the transverse sinus is more developed.[
Surgical considerations
Median and paramedian cranial vault approaches always risk injuring the SSS. Such injuries usually occur during the craniotomy, when the Gigli saw or the bit of the high-speed drill lacerates the walls of the sinus. Even before Cushing's advances, surgeons were fearful of causing such damage and therefore habitually cut bone flaps 2 cm lateral to midline.[
The medial margin of a unilateral frontal craniotomy tends to be in close proximity of the midline. Therefore, the segment of the SSS halfway between the nasion and B can be exposed, especially if the craniotomy is placed on the right side. When the SSS is severely injured during a craniotomy, the sinus can be treated by ligation if the involved segment is near the nasion. We strongly recommend repairing the sinus if it is injured beyond the NB point. Ligation distal to this point is likely to lead to venous infarction.[
The bone flap of the anterior transcallosal approach is usually planned so that two-thirds extend anterior and one-third extends posterior to the coronal suture. Therefore, the SSS is at risk of damage at two of the craniometric points used in this study: NB and B. Depending on the objective, the surgeon can plan the bone flap to expose the entire width of the SSS or only its border. In our study, the incidence of the SSS displaced to the right of midline at both of these points was high, but the exact location of the SSS is best identified on coronal MRIs before surgery. When MRI is unavailable, burr holes should be placed at least 1 cm lateral of midline on the left side and 2 cm lateral of midline on the right side to avoid injuring the SSS.
Parasagittal tumors of the rolandic region can be exposed through a median interhemispheric approach. Typically, the craniotomy reaches or crosses midline. The SSS is partially or completely exposed at the segment related to the midpoint between B and L.[
The posterior transcallosal approach exposes about half of the course of the SSS anterior to L. The borders of the craniotomy can expose the margin or the entire width of the SSS at BL and L. Because the SSS is usually displaced toward the right in this region, we recommend applying the same surgical principles described for reaching rolandic parasagittal lesions through a posterior transcallosal approach.
The torcular Herophili, transverse sinus, and segment of SSS between the inion and L can be exposed during an occipital craniotomy. The SSS is widest in this area, and damage to the sinus or torcular can lead to catastrophic bleeding. Therefore, the craniotomy must be planned and performed carefully to avoid injuring the SSS. Because of the trajectory of the SSS toward the dominant right transverse sinus, the sinus is usually displaced (often completely) toward the right side in this region.[
CONCLUSIONS
The midline is not an accurate landmark for determining the course of the entire SSS across the cranial vault. In most cases, the sinus is partially and sometimes completely displaced from midline, usually toward the right side. The position of the SSS is easily observed on MRIs. We therefore recommend obtaining this study, when possible, to avoid damaging the SSS when performing surgical approaches in the vicinity of midline.
References
1. Alvernia JE, Lanzino G, Melgar M, Sindou MP, Mertens P. Is exposure of the superior sagittal sinus necessary in the interhemispheric approach?. Neurosurgery. 2009. 65: 962-4
2. Bisaria KK. Anatomic variations of venous sinuses in the region of the torcular Herophili. J Neurosurg. 1985. 62: 90-5
3. Brockmann C, Kunze S, Scharf J. Computed tomographic angiography of the superior sagittal sinus and bridging veins. Surg Radiol Anat. 2011. 33: 129-34
4. Browder J, Browder A, Kaplan HA. The venous sinuses of the cerebral dura mater. I. Anatomical structures within the superior sagittal sinus. Arch Neurol. 1972. 26: 175-80
5. Crosby EC, Humphrey T, Lauer EW.editors. Correlative Anatomy of the Nervous Aystem. New York: The MacMillan Company; 1962. p.
6. Cushing H, Eisenhardt L.editors. Meningiomas, Their Classification, Regional Behavior, Life History, and Surgical End Results. Springfield, IL: Charles C. Thomas; 2007. p.
7. Elhadi AM, Kalb S, Perez-Orribo L, Little AS, Spetzler RF, Preul MC. The journey of discovering skull base anatomy in ancient Egypt and the special influence of Alexandria. Neurosurg Focus. 2012. 33: E2-
8. Han H, Tao W, Zhang M. The dural entrance of cerebral bridging veins into the superior sagittal sinus: An anatomical comparison between cadavers and digital subtraction angiography. Neuroradiology. 2007. 49: 169-75
9. Heimer L. The Human Brain and Spinal Cord: Functional Neuroanatomy and Dissection Guide: Springer. 1983. p.
10. Lasjaunias P, Kwok R, Goh P, Yeong KY, Lim W, Chng SM. A developmental theory of the superior sagittal sinus(es) in craniopagus twins. Childs Nerv Syst. 2004. 20: 526-37
11. Samadian M, Nazparvar B, Haddadian K, Rezaei O, Khormaee F. The anatomical relation between the superior sagittal sinus and the sagittal suture with surgical considerations. Clin Neurol Neurosurg. 2011. 113: 89-91
12. Shao Y, Sun JL, Yang Y, Cui QK, Zhang QL. Endoscopic and microscopic anatomy of the superior sagittal sinus and torcular herophili. J Clin Neurosci. 2009. 16: 421-4
13. Sindou M, Auque J, Jouanneau E. Neurosurgery and the intracranial venous system. Acta Neurochir Suppl. 2005. 94: 167-75
14. Streeter GI. The development of the venous sinuses of the dura mater in the human embryo. Am J Anat. 1915. 18: 145-78
15. Teplick SK, Van Heertum RL, Clark RE, Carter AP. Pseudoparasagittal masses caused by displacement of the falx and superior sagittal sinus. J Nucl Med. 1974. 15: 1047-9
16. Tubbs RS, Salter G, Elton S, Grabb PA, Oakes WJ. Sagittal suture as an external landmark for the superior sagittal sinus. J Neurosurg. 2001. 94: 985-7
17. Tubbs RS, Salter G, Oakes WJ. Superficial surgical landmarks for the transverse sinus and torcular herophili. J Neurosurg. 2000. 93: 279-81
18. Woodhall B. Variations of the cranial venous sinuses in the region of the torcular helophili. Arch Surg. 1936. p. 297-314
19. Ziyal IM, Ozgen T. Landmarks for the transverse sinus and torcular herophili. J Neurosurg. 2001. 94: 686-7