- Department of Neurosurgery, Henry Ford Hospital, Detroit, Michigan, USA
Correspondence Address:
Thomas Noh
Department of Neurosurgery, Henry Ford Hospital, Detroit, Michigan, USA
DOI:10.4103/2152-7806.194519
Copyright: © 2016 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Thomas Noh, Mokbel K. Chedid. A novel technique to repair a transverse sacral fracture in a previously fused lumbosacral spondylolisthesis. 21-Nov-2016;7:
How to cite this URL: Thomas Noh, Mokbel K. Chedid. A novel technique to repair a transverse sacral fracture in a previously fused lumbosacral spondylolisthesis. 21-Nov-2016;7:. Available from: http://surgicalneurologyint.com/surgicalint_articles/a-novel-technique-to-repair-a-transverse-sacral-fracture-in-a-previously-fused-lumbosacral-spondylolisthesis/
Abstract
Background:Transverse fractures of the sacrum are rare, and surgical treatment for these fractures ranges from conservative to challenging. Transverse stress fractures of the sacrum after placement of lumbar-to-sacral instrumentation have been previously described. We report a new technique to repair a transverse Type-2 Roy-Camille fracture with spondylolisthesis of S1 over S2 in a previously fused instrumented high-grade L4-L5, L5-S1 spondylolisthesis.
Case Description:A 64-year-old female who previously had an L4-L5, L5-S1 fusion for spondylolisthesis presented with excruciating lower back pain and radiculopathy for over 6 months. She was found to have an S1-S2 transverse fracture caused by previous implantation of pedicle screws. She underwent repositioning of several failed right lumbar and sacral screws and then had bilateral S1-S2 screws placed directly across the fracture line. The patient had an unremarkable postoperative course. She discontinued most of her pain medications within 6 weeks postoperatively. In the months following surgery, she reported only minimal lower back pain and no radiculopathy with the last appointment 5 years postoperatively.
Conclusions:We describe a novel technique to reduce an iatrogenic transverse type-2 Roy-Camille fracture at S1-S2 in a previously instrumented high-grade L4-L5, L5-S1 spondylolisthesis. The patient's fracture achieved adequate reduction and fusion with symptomatic relief.
Keywords: High-transverse Type-2 Roy-Camille fracture, L4-L5 spondylolisthesis, L5-S1 spondylolisthesis
INTRODUCTION
Transverse fractures of the sacrum are a rare complication reported after multilevel lumbosacral fusion.[
Surgical intervention is often necessitated by failure of conservative measures leading to pseudoarthrosis, severe pain, and deformity. In this case report, we describe a simple solution to these fractures using direct S1-S2 screws.
CASE REPORT
History and examination
A 64-year-old female initially presented with excruciating lower back pain and radiculopathy for over six months. Her medical history included three previous back surgeries, the most recent involving lumbosacral instrumentation. The pain began following the third surgery.
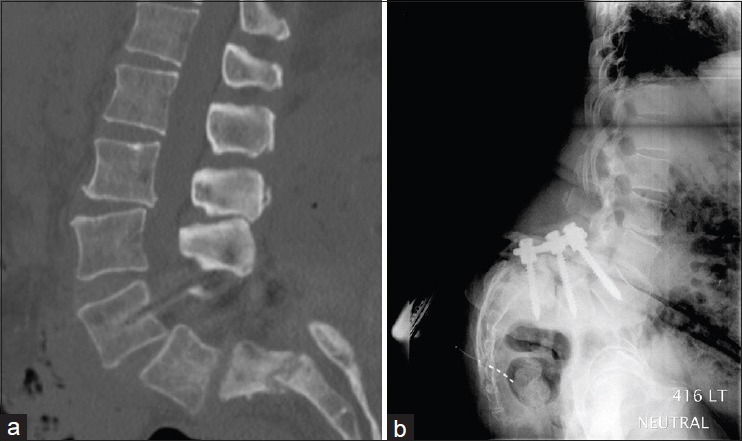
At initial examination on October 4, 2006, the patient showed no weakness, myelopathy, or muscular atrophy. She was able to ambulate slowly with a walker. Her lower back and sacroiliac area were tender to palpation. A positive bone scan, which included single-photon emission computerized tomography imaging, demonstrated abnormal activity along the sacral ala. Electromyography showed a mild left L5 radiculopathy. Her work-up also included a normal dual-energy X-ray absorptiometry (DEXA) scan, X-rays and a computed tomography (CT) scan with contrast and three-dimensional imaging. The scans revealed an S1-S2 transverse fracture caused by her previous sacral pedicle screws [Figure
Surgical technique
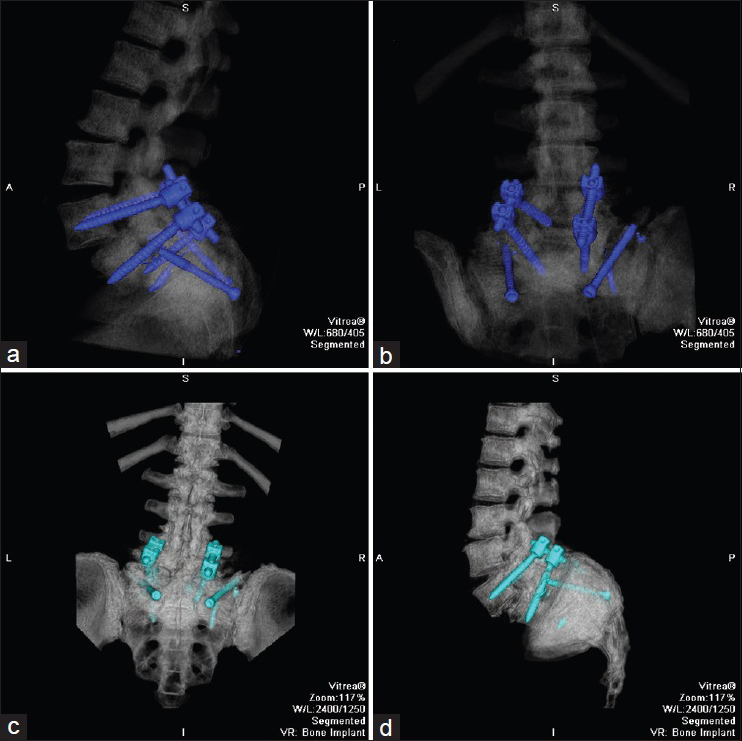
We began with a posterior approach and exposed the lumbosacral area, allowing us to identify the site where the pedicle screw had fractured the sacrum. After repositioning the right pedicle screws, two 50-mm lag screws (DePuy Spine, Raynham, MA) were used directly from S2 to S1 through the lateral sacral crest and across the fracture line (bilaterally). We then filled the fracture with cement (Kyphon, Memphis, TN). Anteroposterior (AP) and lateral C-arm images were used to confirm accurate placement of pins [Figure
DISCUSSION
Although many of these fractures are treated conservatively, operative treatment of these transverse type II fractures, when indicated, typically involves decompression and/or stabilization. Roy-Camille et al. advocated a medial posterior incision with sacral decompression, followed by reduction and fixation with lumboiliac plates, lumbosacral plates, or Harrington rod fixation [
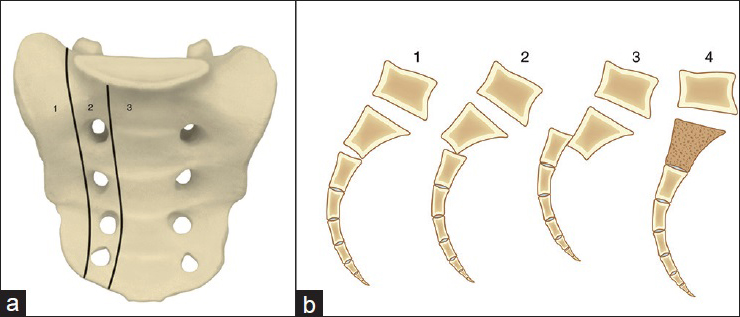
Figure 3
Denis zone classification of sacral fractures (a). Roy-Camille classification of sacral fractures (b). (Adapted from Herkowitz HN, Garfin SR, Eismont FJ, Bell GR, Balderston RA. Rothman-Simeone The Spine: Expert consultation. 6th ed. Saunders; 2011; and Roy-Camille R, Saillant G, Gagna G, Mazel C. Transverse fracture of the upper sacrum. Suicidal jumper's fracture. Spine (Phila Pa 1976) 1985;10:838-845)
Bose used a modified sacralization technique previously described by Benzel and Ball.[
Although the number of reports is limited, previous reports of post-fusion sacral fractures were in osteoporotic patients with larger fusions and longer moment-arms.[
CONCLUSION
Here, we report a new technique utilizing a direct S1-S2 screw to repair an iatrogenic transverse sacral fracture, which provided adequate reduction and symptomatic relief.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Bederman SS, Hassan JM, Shah KN, Keister PD, Bhatia NN, Zamorano DP. Fixation techniques for complex traumatic transverse sacral fractures: A systematic review. Spine. 2013. 38: E1028-40
2. Bellabarba C, Schildhauer TA, Chapman JR, Quinones-Hinojosa A.editors. Management of sacral fractures. Schmidek & Sweet Operative Neurosurgical Techniques. Philadelphia, PA: W.B. Saunders; 2012. p. 2035-45
3. Benzel EC, Ball PA. Management of low lumbar farctures by dorsal decompression, fusion, and lumbosacral laminar distraction fixation. J Neurosurg. 2000. 92: 142-8
4. Bose B. Fracture of S1-2 after L4-S1 decompression and fusion. Case report and review of the literature. J Neurosurg Spine. 2003. 99: 310-2
5. Elias WJ, Shaffrey ME, Whitehill R. Sacral stress fracture following lumbosacral arthrodesis. Case illustration. J Neurosurg. 2002. 96: 135-
6. Fourney DR, Prabhu SS, Cohen ZR, Gokaslan ZL, Rhines LD. Early sacral stress fracture after reduction of spondylolisthesis and lumbosacral fixation: Case report. Neurosurgery. 2002. 51: 1507-
7. Fuentes S, Metellus P, Adetchessi T, Dufour H, Grisoli F. Operative treatment of complex lombosacral fracture dislocation: L5 chance fracture with trans S1-S2 dislocation [in French]. Neurochirurgie. 2006. 52: 376-80
8. Gibbons KJ, Soloniuk DS, Razack N. Neurological injury and patterns of sacral fractures. J Neurosurg. 1990. 72: 889-93
9. Herkowitz HN, Garfin SR, Eismont FJ, Bell GR, Balderston RA.editorsRothman-Simeone The Spine: Expert consultation. Saunders; 2011. p.
10. Mathews V, McCance SE, O’Leary PF. Early fracture of the sacrum or pelvis: An unusual complication after multilevel instrumented lumbosacral fusion. Spine. 2001. 26: E571-5
11. Phelan ST, Jones DA, Bishay M. Conservative management of transverse fractures of the sacrum with neurological features. A report of four cases. J Bone Joint Surg Br. 1991. 73: 969-71
12. Roy-Camille R, Saillant G, Gagna G, Mazel C. Transverse fracture of the upper sacrum. Suicidal jumper's fracture. Spine. 1985. 10: 838-45
13. Sapkas GS, Mavrogenis AF, Papagelopoulos PJ. Transverse sacral fractures with anterior displacement. Eur Spine J. 208;. 7: 342-7
14. Schizas C, Theumann N. An unusual natural history of a L5-S1 spondylolisthesis presenting with a sacral insufficiency fracture. Eur Spine J. 2006. 15: 506-9
15. Suzuki K, Mochida J. Operative treatment of a transverse fracture-dislocation at the S1-S2 Level. J Orthop Trauma. 2001. 15: 363-7
16. Vavken P, Krepler P. Sacral fractures after multi-segmental lumbosacral fusion: A series of four cases and systematic review of literature. Eur Spine J. 2008. 17: S285-90
17. Wilde GE, Miller TT, Schneider R, Girardi FP. Sacral fractures after lumbosacral fusion: A characteristic fracture pattern. AJR Am J Roentgenol. 2011. 197: 184-8