- School of Medicine, University of California, San Diego, CA, USA
- Department of Pathology, University of California, San Diego, CA, USA
- Department of Neurosurgery, University of California, San Diego, CA, USA
Correspondence Address:
Clark C. Chen
Department of Neurosurgery, University of California, San Diego, CA, USA
DOI:10.4103/2152-7806.159373
Copyright: © 2015 Lai G. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.How to cite this article: Lai G, Muller KA, Carter BS, Chen CC. Arteriovenous malformation within an isocitrate dehydrogenase 1 mutated anaplastic oligodendroglioma. Surg Neurol Int 25-Jun-2015;6:
How to cite this URL: Lai G, Muller KA, Carter BS, Chen CC. Arteriovenous malformation within an isocitrate dehydrogenase 1 mutated anaplastic oligodendroglioma. Surg Neurol Int 25-Jun-2015;6:. Available from: http://surgicalneurologyint.com/surgicalint_articles/arteriovenous-malformation-within-an-isocitrate-dehydrogenase-1-mutated-anaplastic-oligodendroglioma/
Abstract
Background:The co-occurrence of intracranial arteriovenous malformations (AVMs) and cerebral neoplasms is exceedingly rare but may harbor implications pertaining to the molecular medicine of brain cancer pathogenesis.
Case Description:Here, we present a case of de novo AVM within an isocitrate dehydrogenase 1 mutated anaplastic oligodendroglioma (WHO Grade III) and review the potential contribution of this mutation to aberrant angiogenesis as an interesting case study in molecular medicine.
Conclusion:The co-occurrence of an IDH1 mutated neoplasm and AVM supports the hypothesis that IDH1 mutations may contribute to aberrant angiogenesis and vascular malformation.
Keywords: Arteriovenous malformation, isocitrate dehydrogenase 1, oligodendroglioma
INTRODUCTION
The co-occurrence of cerebral neoplasms and arteriovenous malformations (AVMs) is a rare but documented phenomenon.[
In this context, we present a case of de novo AVM within an isocitrate dehydrogenase 1 (IDH1) mutated anaplastic oligodendroglioma (WHO Grade III). IDH1 encodes for a metabolic enzyme that catalyze the conversion of isocitrate to α-ketoglutarate, the first step of the citric acid cycle.[
CASE REPORT
History and examination
The patient is a 44-year-old woman who presented with a sub-acute neurocognitive decline over a several months period, such that she was no longer able to perform routine tasks required for daily activities. Past medical history is notable for Graves disease (diagnosed 2005, treated with methimazole) and endometrial adenocarcinoma s/p total abdominal hysterectomy-bilateral salpingo-oophorectomy and chemotherapy (carboplatin and paclitaxel) in 2009, in remission since. Neurological examination was notable for difficulties recalling the events prior to the presentation and disorganized speech. However, the patient re-oriented easily. Physical examination revealed bilateral and symmetric proptosis. Laboratory values were unremarkable. Computed tomography scan of the brain showed 6.1 cm × 4.8 cm × 4.9 cm mass centered over the anterior falx cerebri with moderate surrounding hypodensity and effacement of adjacent sulci [
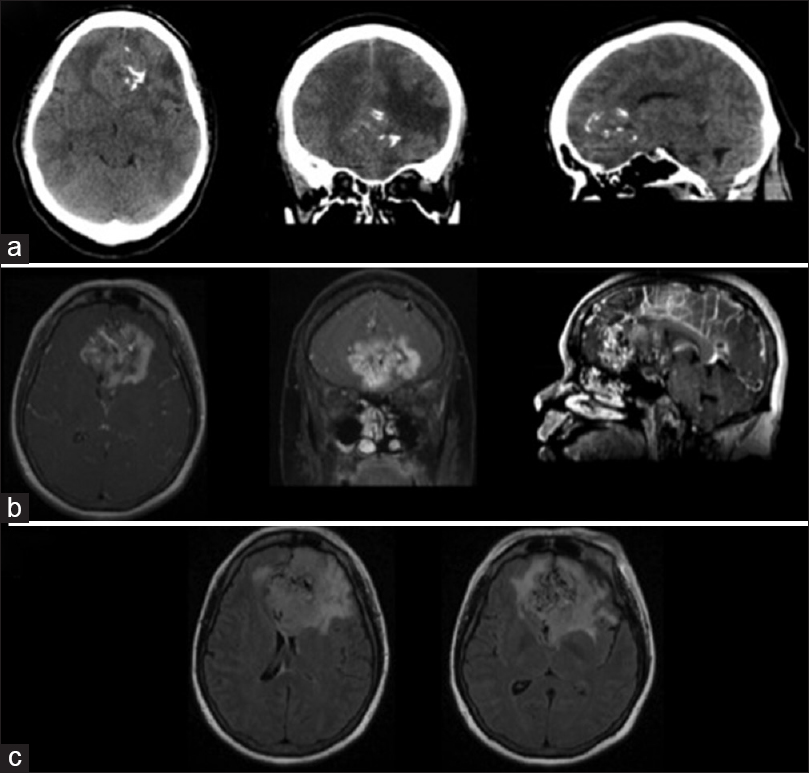
Figure 1
Pretreatment imaging: Computed tomography (a) T1 magnetic resonance postcontrast (b) and fluid attenuation inversion recovery (c) showing 6 cm × 5 cm × 5 cm bilateral frontal lobe mass with internal coarse calcifications, marked enhancement, and surrounding vasogenic edema with multiple flow voids and large draining veins. There is abnormal tissue interspersed between vascular elements and large areas of cystic changes and necrosis
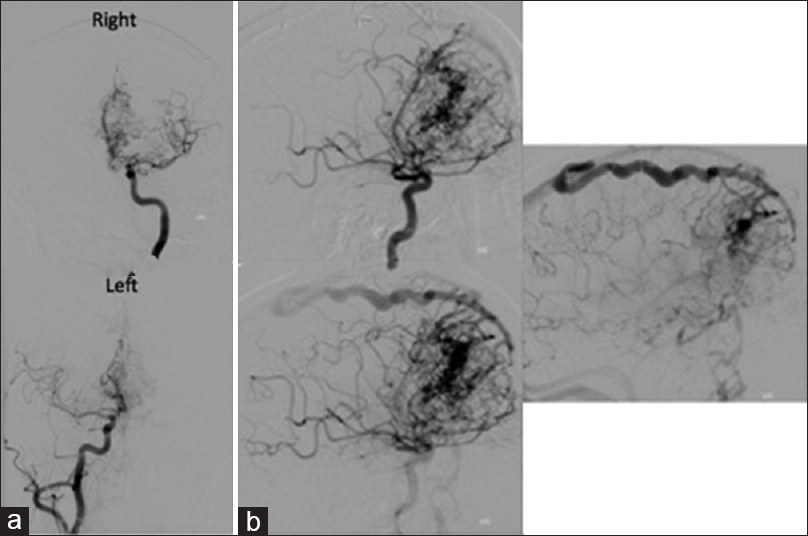
Figure 2
(a) Preembolization digital subtraction angiograms of the anterior circulation performed by injection of the left internal carotid artery and right internal carotid artery demonstrating vascular pedicles emerging from the right middle cerebral artery and right anterior communicating artery (ACA) (top), and pedicles emerging from the left ACA (bottom). (b) Mid to late phase angiogram demonstrate the arteriovenous malformation nidus and the venous outflow
Surgery
Staged embolizations were performed prior to surgical resection. The first stage involved Onyx embolization of four major pedicles arising from the right anterior cerebral artery. 3 days later, Onyx embolization of three major pedicles arising from the left ACA and two pedicles arising from the left MCA were performed. 3 days after the second embolization, the patient underwent resection of the mass through a bi-frontal craniotomy with frontal sinus exenteration. Under microscopic magnification, the plane along the inferior margin of the lesion was developed along the skull base to devascularize the dural pedicles. Branches of the ACA were identified and followed to isolate A1 and A2 branches. Under stereotactic guidance, corticectomy was made in the right middle frontal gyrus to allow a trajectory to the superior margin of the tumor. The tumor was debulked until the distal ACAs were identified. These vessels were carefully followed until continuity to the proximal ACA was established. Tumor fragments were then carefully micro-dissected free from the ACA. Closure was performed using standard methods.
Pathological findings
An intraoperative frozen section was consistent with high-grade glioma. Subsequent hematoxylin and eosin-stained permanent sections revealed an intimate admixture of anaplastic oligodendroglioma (WHO Grade III) and AVM. The anaplastic oligodendroglioma exhibited archetypal histopathologic features including uniform cellularity with uniformly round nuclei set in perinuclear halos [
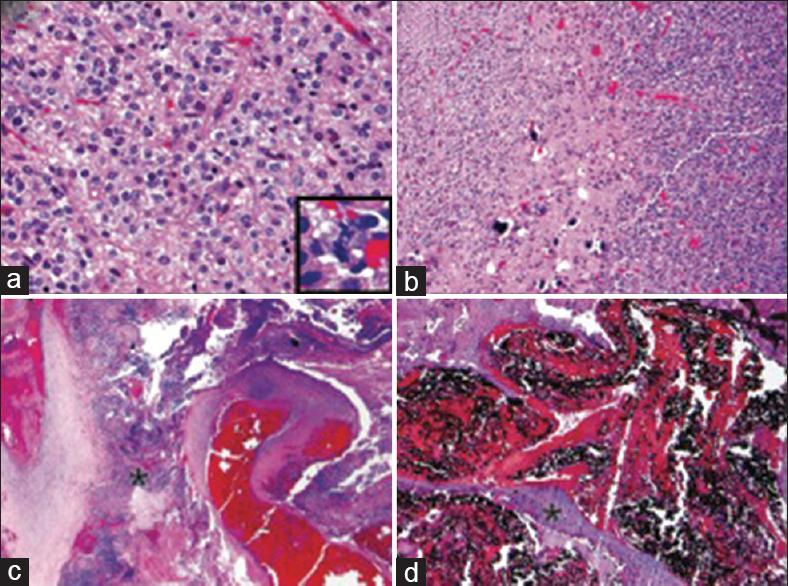
Figure 3
Photomicrographs of anaplastic oligodendroglioma and arteriovenous malformation (AVM) histology (a) anaplastic oligodendroglioma showing uniform cellularity, uniformly round nuclei, and perinuclear halos. This section shows classic delicate microvasculature, although microvascular proliferation was seen in other areas. Inset highlights an atypical mitotic figure of which many were identified (H and E; original magnification, ×200). (b) Secondary features of oligodendroglioma include scattered microcalcifications (center of the image) and clonal nodules of heightened cellularity (right side of image) (H and E original magnification, ×100). (c) Irregular large vessels of the AVM with intervening cellular oligodendroglioma (*) (H and E original magnification, ×20). (d) Irregularly contoured vessels of the AVM filled with black granular embolization material. An intimal cushion is identified in one of the fibrotic vessel walls (*) (H and E original magnification, ×50)
The AVM was set within a background of anaplastic oligodendroglioma and consisted of multiple irregularly contoured vascular lumens of varying diameters including both thick-walled muscular arteries and large thin-walled veins with variable amounts of intervening parenchyma including oligodendroglioma [
Postoperative course
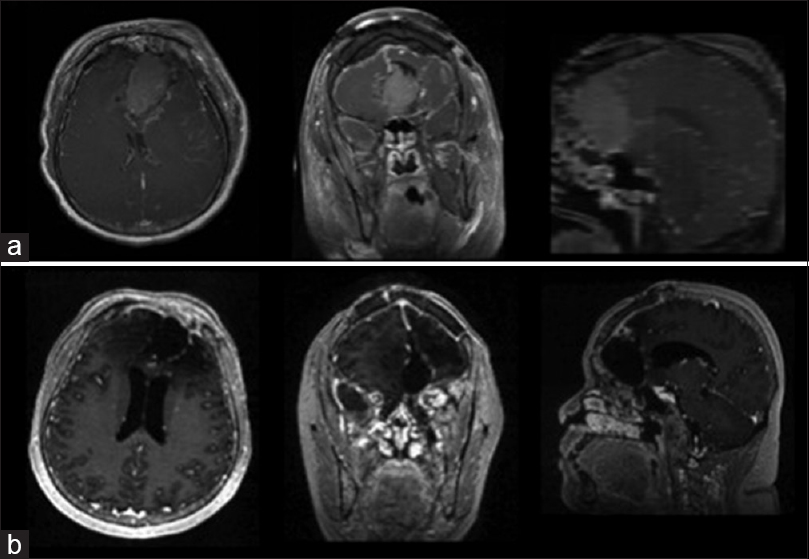
Postoperative MRI revealed a gross total resection of the lesion. The patient remained neurologically non-focal postoperatively. Due to cognitive dysfunction, the patient was discharged to rehabilitation. At the 1-month follow-up, the patient was oriented but had little recollection of the hospitalization. She subsequently underwent a 6-week course of radiation and temozolomide followed by a 1 year course of temozolomide. At the 2 years follow-up, she had her driver's license re-instated and resumed independent living. MRI at this time [
DISCUSSION
Isocitrate dehydrogenase 1 mutation in an anaplastic oligodendroglioma/AVM is of significant interest. The current literature suggests that vascular malformation can be induced by focal expression of vascular endothelial growth factor (VEGF)[
Surgical management of tumors harboring AVMs also warrants discussion. During surgical consideration, tumor vasculature should be deliberately and meticulously scrutinized. Any potential indication of aberrant structures should be further characterized by dedicated vascular studies. Although there are no guidelines for the management of these rare cases, preoperative endovascular embolization is recommended.[
References
1. Aucourt J, Jissendi P, Kerdraon O, Baroncini M. Neuroimaging features and pathology of mixed glioblastoma – AVM complex: A case report. J Neuroradiol. 2012. 39: 258-62
2. Bruno CA Jr, Meyers PM. Endovascular management of arteriovenous malformations of the brain. Interv Neurol. 2013. 1: 109-23
3. Carmeliet P, Jain RK. Principles and mechanisms of vessel normalization for cancer and other angiogenic diseases. Nat Rev Drug Discov. 2011. 10: 417-27
4. Crowell RM, DeGirolami U, Sweet WH. Arteriovenous malformation and oligodendroglioma. Case report. J Neurosurg. 1975. 43: 108-11
5. Dang L, White DW, Gross S, Bennett BD, Bittinger MA, Driggers EM. Cancer-associated IDH1 mutations produce 2-hydroxyglutarate. Nature. 2009. 462: 739-44
6. Forsythe JA, Jiang BH, Iyer NV, Agani F, Leung SW, Koos RD. Activation of vascular endothelial growth factor gene transcription by hypoxia-inducible factor 1. Mol Cell Biol. 1996. 16: 4604-13
7. Gmeiner M, Sonnberger M, Wurm G, Weis S. Glioblastoma with the appearance of arteriovenous malformation: Pitfalls in diagnosis. Clin Neurol Neurosurg. 2013. 115: 501-6
8. Goodkin R, Zaias B, Michelsen WJ. Arteriovenous malformation and glioma: Coexistent or sequential?Case report. J Neurosurg. 1990. 72: 798-805
9. Han C, Choe SW, Kim YH, Acharya AP, Keselowsky BG, Sorg BS. VEGF neutralization can prevent and normalize arteriovenous malformations in an animal model for hereditary hemorrhagic telangiectasia 2. Angiogenesis. 2014. 17: 823-30
10. Harris OA, Chang SD, Harris BT, Adler JR. Acquired cerebral arteriovenous malformation induced by an anaplastic astrocytoma: An interesting case. Neurol Res. 2000. 22: 473-7
11. Koivunen P, Lee S, Duncan CG, Lopez G, Lu G, Ramkissoon S. Transformation by the (R)-enantiomer of 2-hydroxyglutarate linked to EGLN activation. Nature. 2012. 483: 484-8
12. Kroh H, Bidzinski J, Majchrowski A. Supratentorial astrocytoma associated with arteriovenous malformation. Case report. Folia Neuropathol. 1994. 32: 167-9
13. Lee TT, Landy HJ, Bruce JH. Arteriovenous malformation associated with pleomorphic xanthoastrocytoma. Acta Neurochir (Wien). 1996. 138: 590-1
14. Lombardi D, Scheithauer BW, Piepgras D, Meyer FB, Forbes GS. “Angioglioma” and the arteriovenous malformation-glioma association. J Neurosurg. 1991. 75: 589-66
15. Malcolm GP, Symon L, Tan LC, Pires M. Astrocytoma and associated arteriovenous malformation. Surg Neurol. 1991. 36: 59-62
16. McKinney JS, Steineke T, Nochlin D, Brisman JL. de novo formation of large arteriovenous shunting and a vascular nidus mimicking an arteriovenous malformation within an anaplastic oligodendroglioma: Treatment with embolization and resection. J Neurosurg. 2008. 109: 1098-102
17. Naganska E, Matyja E, Pucko E, Zabek M. The coexistence of pleomorphic xanthoastrocytoma and arteriovenous malformation. A case report. Folia Neuropathol. 2013. 51: 269-74
18. Nazek M, Mandybur TI, Kashiwagi S. Oligodendroglial proliferative abnormality associated with arteriovenous malformation: Report of three cases with review of the literature. Neurosurgery. 1988. 23: 781-5
19. Pallud J, Belaid H, Guillevin R, Vallee JN, Capelle L. Management of associated glioma and arteriovenous malformation – The priority is the glioma. Br J Neurosurg. 2009. 23: 197-8
20. Qureshi AI. Endovascular treatment of cerebrovascular diseases and intracranial neoplasms. Lancet. 2004. 363: 804-13
21. Rey S, Semenza GL. Hypoxia-inducible factor-1-dependent mechanisms of vascularization and vascular remodelling. Cardiovasc Res. 2010. 86: 236-42
22. Soltanolkotabi M, Schoeneman SE, Dipatri AJ, Hurley MC, Ansari SA, Rajaram V. Juvenile pilocytic astrocytoma in association with arteriovenous malformation. Interv Neuroradiol. 2012. 18: 140-7
23. Walker EJ, Su H, Shen F, Choi EJ, Oh SP, Chen G. Arteriovenous malformation in the adult mouse brain resembling the human disease. Ann Neurol. 2011. 69: 954-62
24. Ward PS, Cross JR, Lu C, Weigert O, Abel-Wahab O, Levine RL. Identification of additional IDH mutations associated with oncometabolite R(-)-2-hydroxyglutarate production. Oncogene. 2012. 31: 2491-8
25. White JB, Piepgras DG, Scheithauer BW, Parisi JE. Rate of spontaneous hemorrhage in histologically proven cases of pilocytic astrocytoma. J Neurosurg. 2008. 108: 223-6
26. Williams SC, Karajannis MA, Chiriboga L, Golfinos JG, von Deimling A, Zagzag D. R132H-mutation of isocitrate dehydrogenase-1 is not sufficient for HIF-1alpha upregulation in adult glioma. Acta Neuropathol. 2011. 121: 279-81
27. Xu M, Xu H, Qin Z, Zhang J, Yang X, Xu F. Increased expression of angiogenic factors in cultured human brain arteriovenous malformation endothelial cells. Cell Biochem Biophys. 2014. 70: 443-7
28. Yan H, Bigner DD, Velculescu V, Parsons DW. Mutant metabolic enzymes are at the origin of gliomas. Cancer Res. 2009. 69: 9157-9
29. Yan H, Parsons DW, Jin G, McLendon R, Rasheed BA, Yuan W. IDH1 and IDH2 mutations in gliomas. N Engl J Med. 2009. 360: 765-73
30. Zagzag D, Zhong H, Scalzitti JM, Laughner E, Simons JW, Semenza GL. Expression of hypoxia-inducible factor 1alpha in brain tumors: Association with angiogenesis, invasion, and progression. Cancer. 2000. 88: 2606-18
31. Zhao S, Lin Y, Xu W, Jiang W, Zha Z, Wang P. Glioma-derived mutations in IDH1 dominantly inhibit IDH1 catalytic activity and induce HIF-1alpha. Science. 2009. 324: 261-5
32. Ziyal IM, Ece K, Bilginer B, Tezel GG, Ozcan OE. A glioma with an arteriovenous malformation: An association or a different entity?. Acta Neurochir (Wien). 2004. 146: 83-6
33. Zuccarello M, Giordano R, Scanarini M, Mingrino S. Malignant astrocytoma associated with arteriovenous malformation. Case report. Acta Neurochir (Wien). 1979. 50: 305-9