- Department of Neurosurgery, “Federico II” University, Naples, Italy
- Department of Neurosurgery, Anthea Hospital, Bari, Italy
Correspondence Address:
Rocco Severino
Department of Neurosurgery, Anthea Hospital, Bari, Italy
DOI:10.4103/sni.sni_257_17
Copyright: © 2017 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Rocco Severino, Paolo Severino. Cervical intramedullary spinal cord lipoma. 24-Oct-2017;8:255
How to cite this URL: Rocco Severino, Paolo Severino. Cervical intramedullary spinal cord lipoma. 24-Oct-2017;8:255. Available from: http://surgicalneurologyint.com/surgicalint-articles/cervical-intramedullary-spinal-cord-lipoma/
Abstract
Background:Intramedullary, nondysraphic, spinal cord lipomas are rare and account for less than 1% of all spinal cord lesions. Symptoms typically consist of a progressive myelopathy associated with increasing degrees of paralysis (e.g., quadriparesis/plegia, paraparesis/plegia).
Case Description:A 39-year-old male, without a history of spinal dysraphism, presented with a progressive spastic quadriparesis. This was attributed to magnetic resonance-documented large intramedullary cervical lipoma. Following partial intramedullary surgical debulking of the lesion, the patient neurologically improved.
Conclusion:Partial debulking of a cervical intramedullary lipoma in a patient who originally presented with a severe quadriparesis resulted in significant neurological improvement. Notably, utilization of intraoperative ultrasonography, CO2 laser, and both motor evoked and somatosensory evoked potentials can be helpful during the removal of such lipomas.
Keywords: Cervical spine lipoma, cervical spine tumors, intramedullary lipoma
INTRODUCTION
Spinal lipomas are usually extramedullary lesions, and are typically found in the lumbosacral spine with spinal dysraphism. Truly intramedullary spinal cord lipomas are rare, comprising less than 1% of all spinal cord lesions.[
Here, we report a 39-year-old male with a large cervical intramedullary lipoma who improved after partial surgical debulking.
CASE REPORT
Clinical presentation
A 39-year-old male presented with a 1-year history of cervical pain and progressive tetraparesis. His neurological complaints included hypoesthesia in all four extremities, accompanied by a progressive quadriparesis (e.g., inability to walk and left leg hyperreflexia).
Magnetic resonance imaging (MRI) showed an intradural, intramedullary mass extending from C5 to T2 (6.2 × 1.3 cm), causing a severe cord compression without spinal dysraphism [
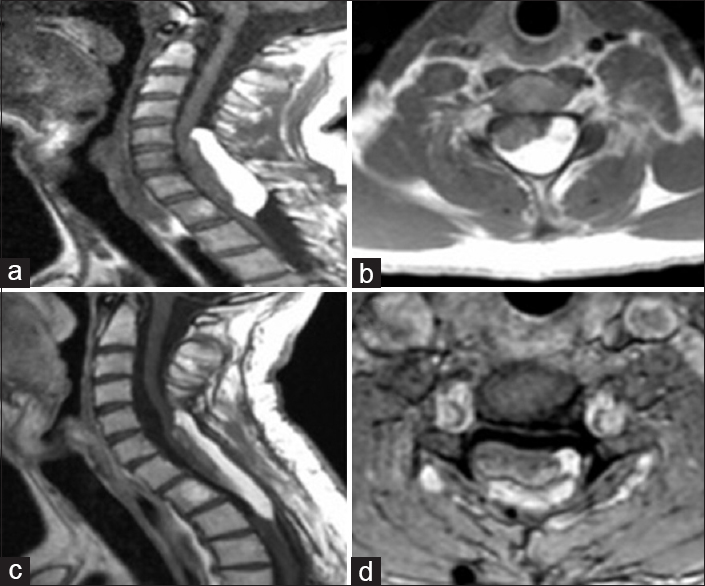
Figure 1
(a and b) preoperative T1-weighted MRI showing a hyperintense intramedullary mass extending from C5 to D2 with compression and dislocation of the spinal cord. (c and d) 4-year postoperative T1-weighted MRI showing the decompression of the spinal cord and a residual of the tumor where it was most adherent to the nervous tissue
The patient underwent a cervical laminectomy extending from C5 to D2 with a myelotomy performed at the thinnest area of the spinal cord overlying the mass. As there was no clear cleavage plane between the lipoma and the cord, an internal debulking of the mass was performed along with a duroplasty. The postoperative period was uneventful, and the patient was discharged on postoperative day 8. Following surgery, the patient's spasticity and the weakness improved and he was again able to ambulate. Four years later, MR showed only a mild growth of the residual tumor [
DISCUSSION
Spinal cord lipomas are rare lesions, representing less than 1% of all spinal cord tumors.[
Etiology/Embryogenesis
The few spinal cord lipoma cases reported in the literature are typically extramedullary lesions.[
Clinical presentation
The clinical presentation of cervical intramedullary lipomas includes ataxia, cervical axis pain, dysesthesias, and a progressive quadriparesis, as noted in this case. Adults often exhibit more subtle findings characterized by a slowly-progressive myelopathy. When compression is maximal, the patients finally develop increasing myelopathy.[
Early diagnosis and treatment
Early diagnosis and treatment are critical to avoid prolonged cervical cord compression with resultant irreversible neurological injury.[
MRI usually demonstrates a T1 hyperintense and T2 hypointense intramedullary mass with an inversion of intensity at short T1 inversion recovery sequences, supporting the adipose nature of the mass. The optimal treatment of these lesions is decompression from within the tumor margins to avoid further neurological deterioration as there is typically no clear plane of cleavage between the lesion and the spinal cord.[
Some surgeons advocate using the carbon-dioxide laser to vaporizes these lesions, avoiding direct manipulation of the spinal cord.[
CONCLUSIONS
Intramedullary cervical spinal cord intramedullary lipomas are rare. They typically present with a progressive spastic quadriparesis. Treatment usually requires debulking rather than gross total resection to avoid increasing the neurological deficit.[
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Bhatoe HS, Singh P, Chaturvedi A, Sahai K, Dutta V, Sahoo PK. Nondysraphic intramedullary spinal cord lipomas: A review. Neurosurg Focus. 2005. 18: ECP1-
2. Caram PC, Carton CA, Scarcella G. Intradural lipomas of the spinal cord; with particular emphasis on the intramedullary lipomas. J Neurosurg. 1957. 14: 28-42
3. Chagla AS, Balasubramaniam S, Goel AH. A massive cervicomedullary intramedullary spinal cord lipoma. J Clin Neurosci. 2008. 15: 817-20
4. Lee M, Rezai AR, Abbott R, Coelho DH, Epstein FJ. Intramedullary spinal cord lipomas. J Neurosurg. 1995. 82: 394-400
5. McCormick PC, Stein BM. Intramedullary tumors in adults. Neurosurg Clin N Am. 1990. 1: 609-30
6. Mori K, Kamimura Y, Uchida Y, Kurisaka M, Eguchi S. Large intramedullary lipoma of the cervical cord and posterior fossa. Case report. J Neurosurg. 1986. 64: 974-6
7. Naim Ur R, Salih MA, Jamjoom AH, Jamjoom ZA. Congenital intramedullary lipoma of the dorsocervical spinal cord with intracranial extension: Case report. Neurosurgery. 1994. 34: 1081-3
8. Rogers HM, Long DM, Chou SN, French LA. Lipomas of the spinal cord and cauda equina. J Neurosurg. 1971. 34: 349-54