- Department of Surgery, Division of Plastic Surgery, Brigham and Women's Hospital, Boston, MA 02115, USA
- Department of Surgery, Center for Surgery and Public Health, Brigham and Women's Hospital, Boston, MA 02115, USA
- Departmant of Neurosurgery, Brigham and Women's Hospital, Boston, MA 02115, USA
Correspondence Address:
Edward J. Caterson
Department of Surgery, Division of Plastic Surgery, Brigham and Women's Hospital, Boston, MA 02115, USA
DOI:10.4103/2152-7806.161409
Copyright: © 2015 Singh M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.How to cite this article: Singh M, Rios Diaz AJ, Golby AJ, Caterson EJ. “Countersinking” of reservoir in an irradiated patients can decrease tension on scalp closure. Surg Neurol Int 23-Jul-2015;6:
How to cite this URL: Singh M, Rios Diaz AJ, Golby AJ, Caterson EJ. “Countersinking” of reservoir in an irradiated patients can decrease tension on scalp closure. Surg Neurol Int 23-Jul-2015;6:. Available from: http://surgicalneurologyint.com/surgicalint_articles/countersinking-of-reservoir-in-an-irradiated-patients-can-decrease-tension-on-scalp-closure/
Abstract
Background:Subcutaneous reservoirs are used to provide therapy by establishing access to cerebrospinal fluid. However, it is associated with complications such as hemorrhage, infection, malfunction, and malpositioning. In an irradiated field with thin skin, use of reservoir can result in wound dehiscence, wound infection, and device extrusion.
Case Description:We introduced a “countersinking” technique for the reservoir placement which involves the creation of bony recess in the skull to effectively accommodate the reservoir and decrease the protrusion. “Countersinking” of the reservoir can result in tension-free closure of the scalp and allow durable coverage of the reservoir. In the representative case, the incisional wound healed completely without any concern for wound dehiscence and the countersink technique may have contributed to effective healing of the radiated scalp.
Conclusion:Countersinking of the reservoir can be a strategy to prevent complications such as wound dehiscence, and device extrusion in any patient, but in irradiated patients with very thin skin it also enables tension-free closure of the wound.
Keywords: Countersinking, ommaya reservoir, wound dehiscence
INTRODUCTION
Subcutaneous reservoirs such as ommaya reservoir are used to administer intraventricular antibiotics for chronic meningitis, intrathecal chemotherapy for central nervous system lymphoma, and aspirate fluids from cystic tumors.[
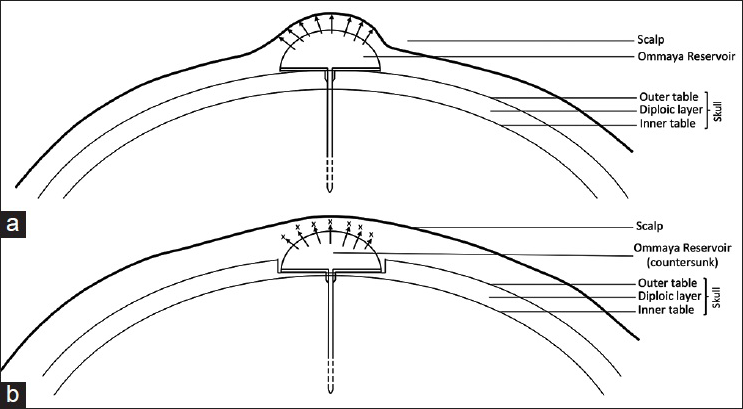
Figure 1
Protrusion of the reservoir increases the tension on the overlying wound (a) while countersinking of the reservoir between the outer and inner table of the skin bone (b) promotes tension-free wound closure. This technique facilitates wound healing prevents complications such as wound dehiscence
CASE REPORT
The patient was a 46-year-old woman who underwent right frontal craniotomy in1998 for tumor resection. Pathology was consistent with astrocytoma requiring adjuvant chemoradiation therapy. Her follow-up magnetic resonance imaging in 2012 showed interval cyst enlargement in the right frontal lobe. A plan was made to proceed with aspiration of the cyst contents and then leave a catheter into the cavity which would then be connected to a reservoir for access in case the cyst reaccumulates.
Due to the history of radiation and very thin skin, there was a significant concern for wound breakdown and a modified technique was used for reservoir placement. A U-shaped incision was made adjacent to the previous incision outside the borders of the radiated skin and a pericranial flap was then raised. The skull bone was drilled through the outer table and the diploic layer to the level of the inner table to provide a tailored bony recess for countersinking the reservoir in the skull so that it would not protrude. The BrainLab navigation system was used to establish the oblique trajectory of the catheter. The dura was opened and the catheter was passed into the cyst. About 20 ml of yellowish thick fluid was aspirated and sent to cytology. The catheter was then secured to the reservoir which was effectively countersunk in the bony recess. The patient had no complications from the reservoir placement at 2 months follow-up appointment.
CONCLUSION
Subcutaneous reservoirs provide an effective way of establishing external access to cerebrospinal fluid (CSF) and other intracranial fluid spaces.[
In our patient, there was a high risk of wound dehiscence and reservoir extrusion given the thin irradiated skin. Countersinking of the reservoir into the bone decreases the protuberance and by doing so, minimizes the stretching of the overlying skin [
Since a large number of brain tumor patients require chemoradiation and these patients often have significant other co-morbidities resulting in poor wound healing, the “countersinking” of the reservoir can potentially prevent the risk wound dehiscence and device extrusion in these patients and enable tension free intra-operative closure of the wound.
References
1. Barnett GC, West CM, Dunning AM, Elliott RM, Coles CE, Pharoah PD. Normal tissue reactions to radiotherapy: Towards tailoring treatment dose by genotype. Nat Rev Cancer. 2009. 9: 134-42
2. Bernardi RJ, Bomgaars L, Fox E, Balis FM, Egorin MJ, Lagattuta TF. Phase I clinical trial of intrathecal gemcitabine in patients with neoplastic meningitis. Cancer Chemother Pharmacol. 2008. 62: 355-61
3. Dinndorf PA, Bleyer WA. Management of infectious complications of intraventricular reservoirs in cancer patients: Low incidence and successful treatment without reservoir removal. Cancer Drug Deliv. 1987. 4: 105-17
4. Hom DB, Adams GL, Monyak D. Irradiated soft tissue and its management. Otolaryngol Clin North Am. 1995. 28: 1003-19
5. Jiang PF, Yu HM, Zhou BL, Gao F, Shen SX, Xia ZZ. The role of an Ommaya reservoir in the management of children with cryptococcal meningitis. Clin Neurol Neurosurg. 2010. 112: 157-9
6. Kulkarni S, Ghosh SP, Hauer-Jensen M, Kumar KS. Hematological targets of radiation damage. Curr Drug Targets. 2010. 11: 1375-85
7. Lishner M, Perrin RG, Feld R, Messner HA, Tuffnell PG, Elhakim T. Complications associated with Ommaya reservoirs in patients with cancer. The Princess Margaret Hospital experience and a review of the literature. Arch Intern Med. 1990. 150: 173-6
8. Obbens EA, Leavens ME, Beal JW, Lee YY. Ommaya reservoirs in 387 cancer patients: A 15-year experience. Neurology. 1985. 35: 1274-8
9. Ratcheson RA, Ommaya AK. Experience with the subcutaneous cerebrospinal-fluid reservoir. Preliminary report of 60 cases. N Engl J Med. 1968. 279: 1025-31
10. Rubenstein JL, Fridlyand J, Abrey L, Shen A, Karch J, Wang E. Phase I study of intraventricular administration of rituximab in patients with recurrent CNS and intraocular lymphoma. J Clin Oncol. 2007. 25: 1350-6
11. Sandberg DI, Bilsky MH, Souweidane MM, Bzdil J, Gutin PH. Ommaya reservoirs for the treatment of leptomeningeal metastases. Neurosurgery. 2000. 47: 49-54
12. Shapiro WR, Posner JB, Ushio Y, Chemik NL, Young DF. Treatment of meningeal neoplasms. Cancer Treat Rep. 1977. 61: 733-43
13. Witorsch P, Williams TW Jr, Ommaya AK, Utz JP. Intraventricular administration of amphotericin B. Use of subcutaneous reservoir in four patients with mycotic meningitis. JAMA. 1965. 194: 699-702
14. Yang S, Dai J, Zhang X, Jin Y. Intracerebral arachnoid cyst treated with Ommaya reservoir implantation in a patient younger than two years. J Craniofac Surg. 2014. 25: e378-80