- Department of Neurology, Yale School of Medicine, New Haven, Connecticut, United States.
Correspondence Address:
Adeel Shakil Zubair, Department of Neurology, Yale School of Medicine, New Haven, Connecticut, United States.
DOI:10.25259/SNI_543_2023
Copyright: © 2023 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Adeel Shakil Zubair. “Hot nose” sign in brain death. 11-Aug-2023;14:282
How to cite this URL: Adeel Shakil Zubair. “Hot nose” sign in brain death. 11-Aug-2023;14:282. Available from: https://surgicalneurologyint.com/surgicalint-articles/12498/
Abstract
Background: Brain death testing is a rigorous process in which meticulous examination is crucial. In certain cases, ancillary testing is required.
Case Description: A 30-year-old male presented to the emergency room after a motor vehicle accident and was found to have subarachnoid hemorrhage and subdural hematoma. The examination was notable for the absence of brainstem responses. A nuclear medicine brain scan was completed which showed carotid arterial activity up to the level of the skull base with no intracranial arterial activity above with a “hot nose” sign consistent with brain death.
Conclusion: The “hot nose” sign has been described in brain-dead patients and is postulated to occur due to increased flow to the nose through the external carotid artery.
Keywords: Brain death, Hot nose, Neurocritical care, Perfusion imaging
A 30-year-old male presented to the hospital following a motor vehicle accident as a trauma code. He was evaluated in the emergency room and found to have a Glasgow coma scale of three and was emergently intubated. A computed tomography scan of the head was completed which demonstrated a left subdural hematoma as well as subarachnoid hemorrhage. At the time of the initial examination, the patient had preserved brainstem reflexes and was admitted to the surgical intensive care unit for further treatment.
His hospital course was notable for hemodynamic instability. He was noted to have a loss of pupillary responses and other core brainstem reflexes. Nuclear medicine (NM) testing was ordered and the NM brain scan showed carotid arterial activity up to the level of the skull base with no intracranial arterial activity above; increased blood flow was seen on delayed imaging to the external carotid artery circulation with a “hot nose” sign consistent with brain death [
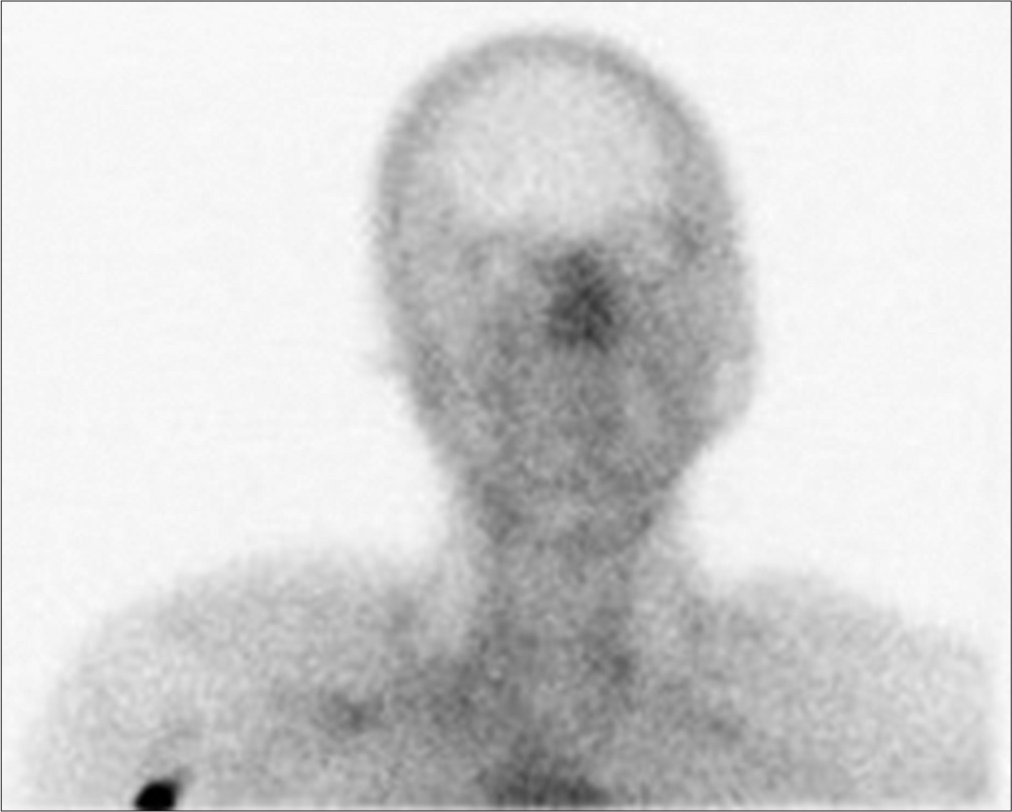
Figure 1:
Nuclear medicine brain imaging showing carotid arterial activity up to the level of the skull base with no intracranial arterial activity above. Increased blood flow was seen on delayed imaging of the external carotid artery circulation. A “hot nose” sign is visible, consistent with brain death.
The “hot nose” sign has been described in the literature in patients who are brain-dead.[
Declaration of patient consent
Patient’s consent not required as patient’s identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.
References
1. Appelt EA, Song WS, Phillips WT, Metter DF, Salman UA, Blumhardt R. The “hot nose” sign on brain death nuclear scintigraphy: Where does the flow really go?. Clin Nucl Med. 2008. 33: 55-7
2. Baron M, Brasfield J. A 37-year-old man with severe head trauma, and a “hot nose” sign on brain flow study. Chest. 1999. 116: 1468-70
3. Huang AH. The hot nose sign. Radiology. 2005. 235: 216-7
4. Kalra SS, Chizinga M, Ataya A. The ‘hot nose’ sign in brain death. QJM. 2020. 113: 365-6
5. Orrison WW, Champlin AM, Kesterson OL, Hartshorne MF, King JN. MR ‘hot nose sign’ and ‘intravascular enhancement sign’ in brain death. AJNR Am J Neuroradiol. 1994. 15: 913-6