- Department of Neurosurgery, King Abdulaziz Medical City, National Guard Health Affairs, Jeddah, Saudi Arabia
- King Abdullah International Medical Research Center, Jeddah, Saudi Arabia
- College of Medicine, King Saud Bin Abdulaziz University for Health Sciences, Jeddah, Saudi Arabia
- Neurosurgery Department, King Abdullah Medical City in Holy Capital, Saudi Arabia.
Correspondence Address:
Abdulaziz M. Alghamdi, College of Medicine, King Saud Bin Abdulaziz University for Health Sciences, Jeddah, Saudi Arabia.
DOI:10.25259/SNI_226_2023
Copyright: © 2023 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Abdulhadi Y. Algahtani1,2,3, Abdulaziz M. Alghamdi2,3, Alaa Ashqar2,3, Abdulaziz Abdullah Basurrah4, Moajeb Alzahrani1,2,3. Idiopathic spontaneous bilateral subdural hematoma in a 28-year-old male: A comprehensive literature review and case report. 07-Apr-2023;14:130
How to cite this URL: Abdulhadi Y. Algahtani1,2,3, Abdulaziz M. Alghamdi2,3, Alaa Ashqar2,3, Abdulaziz Abdullah Basurrah4, Moajeb Alzahrani1,2,3. Idiopathic spontaneous bilateral subdural hematoma in a 28-year-old male: A comprehensive literature review and case report. 07-Apr-2023;14:130. Available from: https://surgicalneurologyint.com/surgicalint-articles/12239/
Abstract
Background: Subdural hematoma (SDH) is considered spontaneous in the absence of trauma history. It is a common presentation in the geriatric age group due to the many influential factors. Most cases have a known underlying etiology that explains the incidence, otherwise, they are considered idiopathic. We present a rare case report of idiopathic nontraumatic bilateral SDH with a literature review of similar cases.
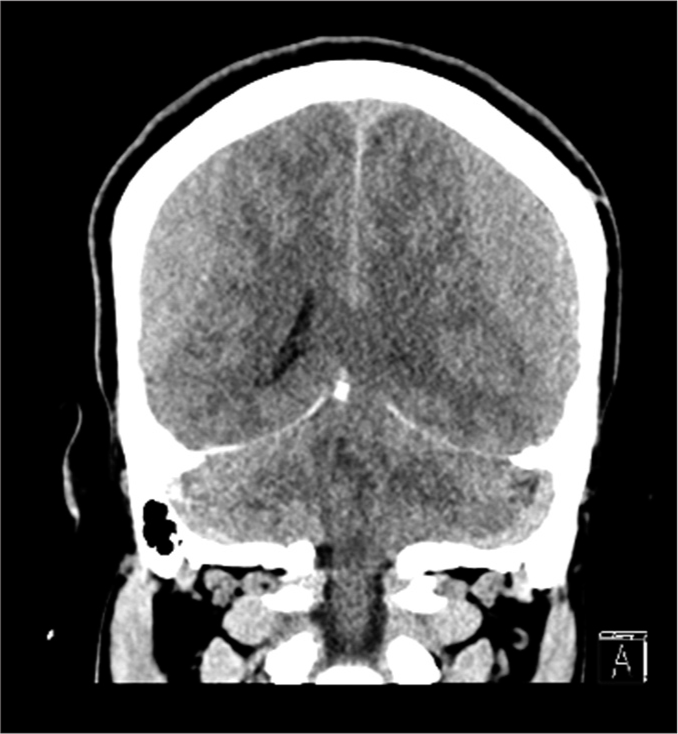
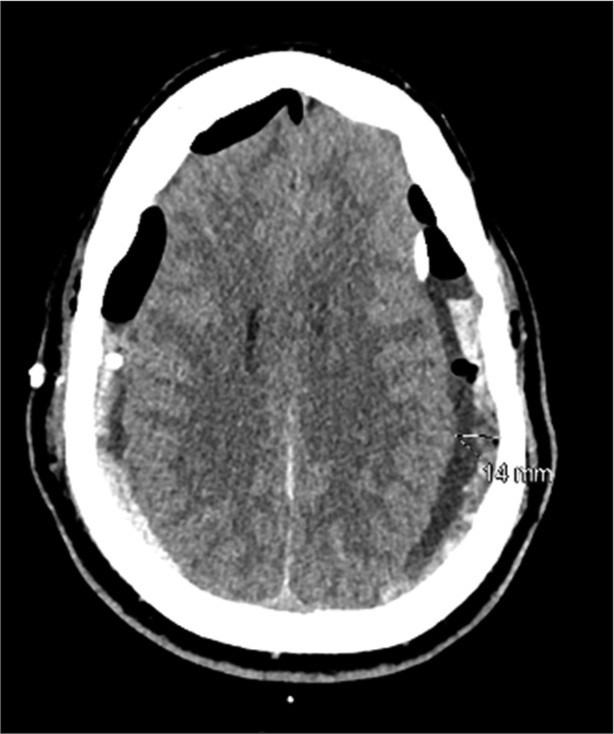
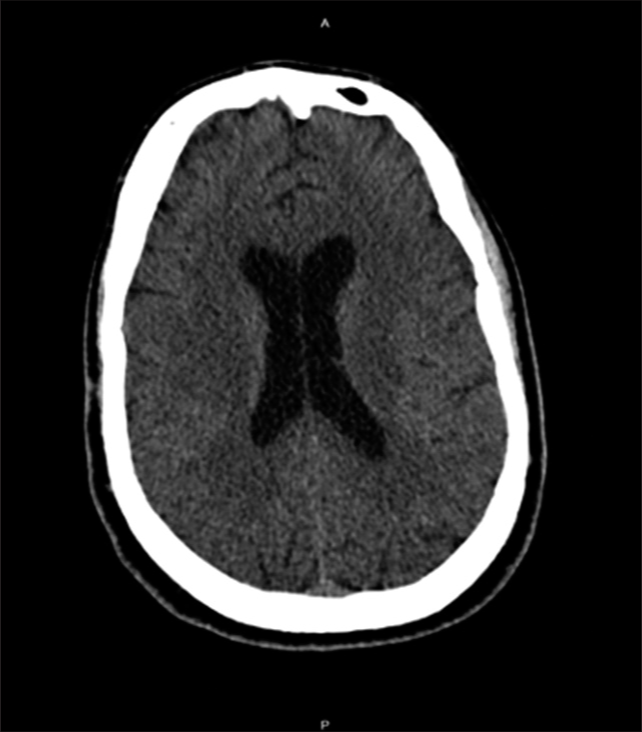
Case Description: A 28-year-old fit individual presented to the Emergency Department with a chronic history of severe headache and neck pain, associated with behavioral changes in the last 2 days. He reported that his symptoms started after lifting a heavy object 2 months ago; however, they became worse after a neck chiropractor therapy session. He is not on any chronic medications, and there was a negative history of trauma, seizure, hematological diseases, family history of neurological conditions, smoking, alcohol, or drug abuse with an unremarkable systemic review. A brain computerized tomography (CT) showed bilateral SDHs, for which he underwent bilateral mini craniotomies and drainage. The symptoms improved after surgery and the follow-up brain CT showed no recurrence.
Conclusion: Idiopathic spontaneous bilateral SDH in the adult age group is an extremely rare pathology and the literature review only revealed three similar cases. With the absence of any pathology that would explain the presentation after extensive investigations, we hypothesized that a sudden rise in vascular pressure was the underlying etiology, especially with the fact that the symptoms became unbearable after the neck chiropractor therapy session.
Keywords: Bilateral subdural hematoma, Headache, Idiopathic, Nontraumatic
INTRODUCTION
Subdural hematoma (SDH) is one of the common pathologies in the field of neurosurgery, especially in the geriatric age group. Brain atrophy increases the space between the brain cortex and the skull, which causes the bridging veins to be stretched; therefore, it increases the probability of veins rupturing. Thus, the incidence of SDH is directly proportional to the space between the brain and the skull.[
CASE DESCRIPTION
A 28-year-old fit male soldier was brought by his family to Emergency Department (ED) with a history of severe headache, neck pain, nausea, and vomiting, which were associated with behavioral changes in the past 2 days. His symptoms started 2 months ago after lifting a heavy object when he developed neck pain associated with a severe headache that increased in severity over time. He has visited the ED twice before this time, and he was only investigated by a cervical spine X-ray with no brain images; then, he was discharged on analgesia and an outpatient department clinic appointment. As his symptoms did not improve with time, he went to an uncertified chiropractor for neck pain, asking for a neck therapy session, after which his symptoms increased in severity. As the headache became unbearable after the therapy session, he went to a hospital and did a brain computerized tomography (CT) which showed bilateral SDH [
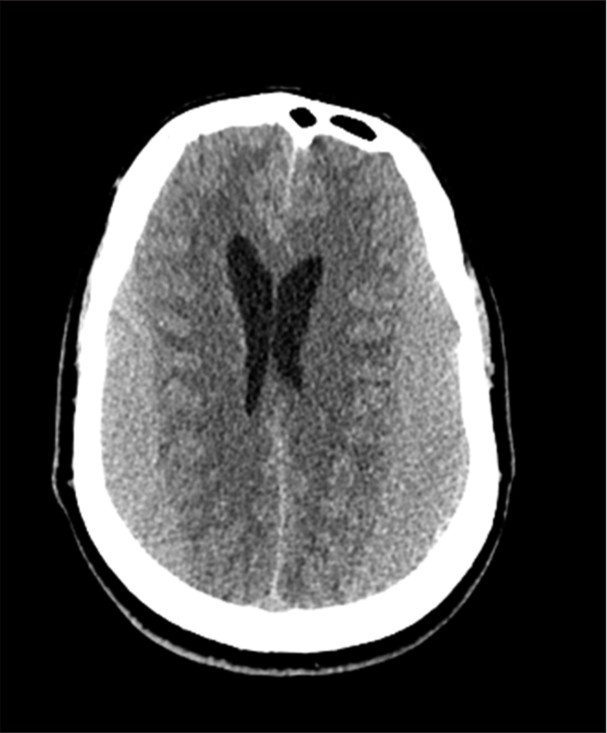
Factor VIII and XIII, and vWF cofactor and Antigen) were done and came within normal ranges. The psychiatry team was consulted, and he was diagnosed with major depressive disorder. Eventually, the patient was discharged home in stable condition and completely resolved symptoms on the 6th-day post-surgery. After 8 months, a follow-up brain CT scan was done, and it showed an interval resolution of the bilateral SDH with no signs of recurrence [
METHODS
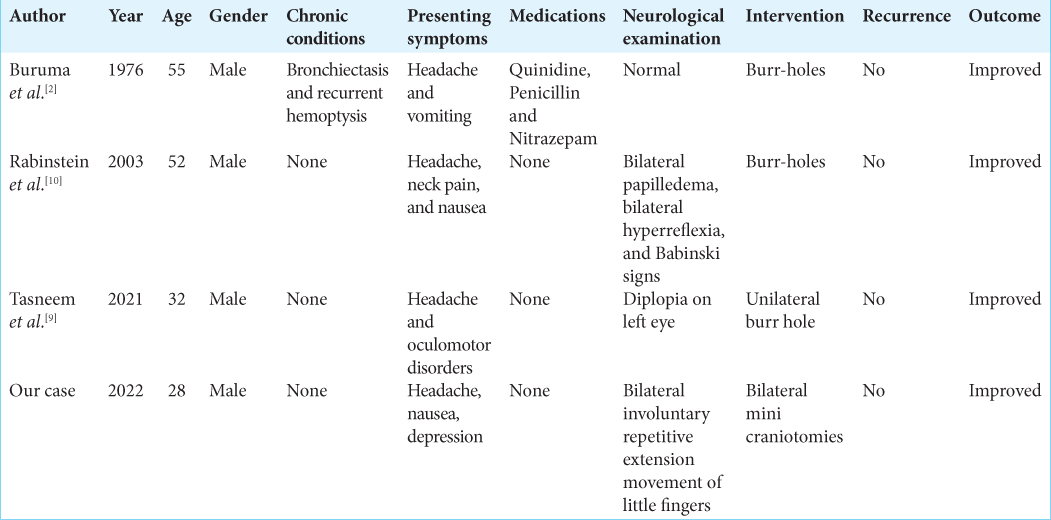
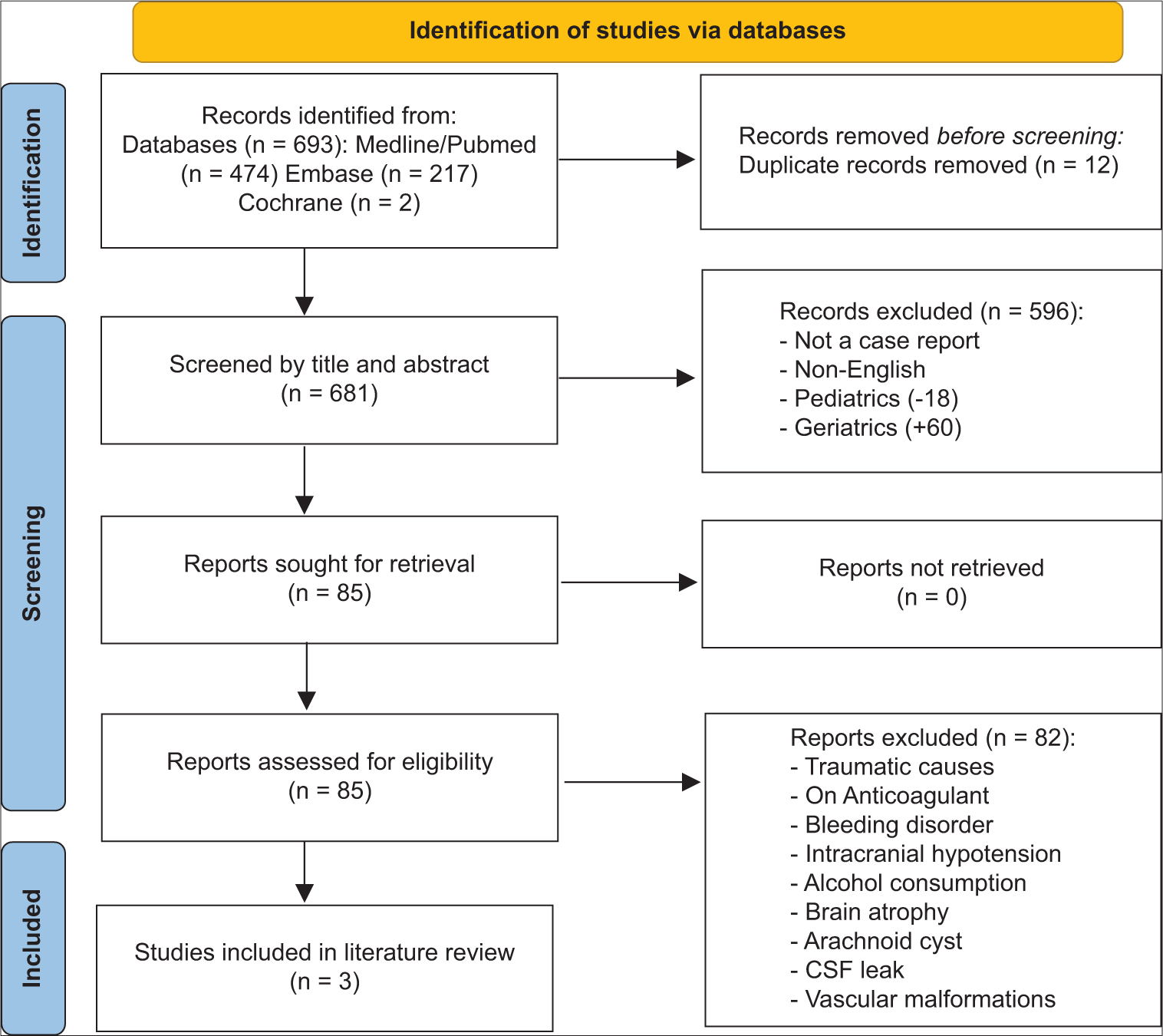
We performed a literature review of idiopathic spontaneous SDH case reports in the databases: PubMed/Medline, Embase, and Cochrane utilizing the keywords: (Bilateral SDH) and (case report) in July 2022. The following keywords: Traumatic and spinal have been used to exclude further the unwanted articles and the language of the included articles was restricted to only articles written in English. A thorough literature review of the enrolled articles by two independent reviewers in duplicate was conducted in two steps, the first step involved screening the titles and abstracts, and the second step involved screening the full texts, and conflicts, if any, were handled by a third independent reviewer. Only case reports of idiopathic spontaneous bilateral SDH in patients aged between 18 and 60 who underwent full investigations to rule out any identifiable causes were included in the study. The case reports of bilateral SDH with identifiable causes such as trauma, anticoagulant therapy, vascular malformation, bleeding disorders, cerebrospinal fluid leak, intracranial hypotension, alcohol consumption, or brain atrophy were excluded from the study. After the full-text screening was completed, two independent authors in duplicate further conducted the data extraction. The extracted data involved the following variables: Author name, year of publication, age, gender, chronic conditions, presenting symptoms, medications, neurological examination findings, intervention, recurrence, and outcome. The descriptive statistics such as frequencies and percentages were then analyzed using John’s Macintosh project software version 15.0.
RESULTS
Initially, 693 articles were identified from the previously mentioned databases. After the full-text screening, only three case reports fit our criteria and they were included in this literature review [
DISCUSSION
Spontaneous SDH is a common pathology in the geriatric age group, unlike in other age groups, where it is considered uncommon. There is enough data in the literature that suggests a relationship between some factors and the incidence of chronic SDH such as advanced age, high blood pressure, alcohol intake, use of blood thinners, and coagulopathies.[
Spontaneous SDH in the middle age group usually occurs unilaterally with one or more of the predisposing factors mentioned above.[
The underlying pathophysiology is still not clearly understood; however, the anatomical nature of the bridging veins makes them more susceptible to rupture, as they lack the presence of any supporting reinforcement from the arachnoid in addition to their structural lack of elastic or muscular layers.[
Some studies have proven that a sudden rise in vascular pressure leads to a defect in the blood-brain barrier, especially in the venules. An experimental study that was done by Mayhan and Heistad demonstrated a marked venules dilatation and blood–brain barrier disruption after acute arterial hypertension and superior vena cava occlusion.[
Limitations
This study has some limitations as the included literature evidence is only provided by case reports; therefore, it affects the quality of the study. However, considering how rare idiopathic spontaneous bilateral SDH in adults is, this study provides the best and latest evidence in the literature. Further studies to help understand the underlying causes and mechanisms of idiopathic spontaneous bilateral SDH in adults are recommended.
CONCLUSION
Spontaneous idiopathic bilateral SDH is an extremely rare pathology in the young age group. It is a diagnosis of exclusion with a favorable outcome. It must be included in the differential diagnosis for unexplained persistent neurological or psychiatric deterioration.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.
References
1. Alaraj AM, Chamoun RB, Dahdaleh NS, Haddad GF, Comair YG. Spontaneous subdural haematoma in anabolic steroids dependent weight lifters: Reports of two cases and review of literature. Acta Neurochir (Wien). 2005. 147: 85-7 discussion 87-8
2. Buruma OJ, Sande JJ. Bilateral acute spontaneous subdural hematoma. A case report. Clin Neurol Neurosurg. 1976. 79: 211-4
3. Coombs JB, Coombs BL, Chin EJ. Acute spontaneous subdural hematoma in a middle-aged adult: Case report and review of the literature. J Emerg Med. 2014. 47: e63-8
4. Erkulvrawatr S, Srinivasan G. Complete spontaneous resolution of bilateral subdural hematoma. South Med J. 1978. 71: 456-8
5. Farhat Neto J, Araujo JL, Ferraz VR, Haddad L, Veiga JC. Chronic subdural hematoma: Epidemiological and prognostic analysis of 176 cases. Rev Col Bras Cir. 2015. 42: 283-7
6. Kar SK, Kumar D, Singh P, Upadhyay PK. Psychiatric manifestation of chronic subdural hematoma: The unfolding of mystery in a homeless patient. Indian J Psychol Med. 2015. 37: 239-42
7. Kostić A, Kehayov I, Stojanović N, Nikolov V, Kitov B, Milošević P. Spontaneous chronic subdural hematoma in elderly people-Arterial hypertension and other risk factors. J Chin Med Assoc. 2018. 81: 781-6
8. Mayhan WG, Heistad DD. Role of veins and cerebral venous pressure in disruption of the blood-brain barrier. Circ Res. 1986. 59: 216-20
9. Mohamed T, Swed S, Al-Mouakeh A, Sawaf B. Nontraumatic bilateral subdural hematoma: Case report. Ann Med Surg (Lond). 2021. 71: 102907
10. Rabinstein AA, Pittock SJ, Miller GM, Schindler JJ, Wijdicks EF. Pseudosubarachnoid haemorrhage in subdural haematoma. J Neurol Neurosurg Psychiatry. 2003. 74: 1131-2
11. Scranton RA, Evans RW, Baskin DS. A motion simulator ride associated with headache and subdural hematoma: First case report. Headache. 2016. 56: 372-8
12. Sim YW, Min KS, Lee MS, Kim YG, Kim DH. Recent changes in risk factors of chronic subdural hematoma. J Korean Neurosurg Soc. 2012. 52: 234-9
13. Stubbs DJ, Vivian ME, Davies BM, Ercole A, Burnstein R, Joannides AJ. Incidence of chronic subdural haematoma: A single-centre exploration of the effects of an ageing population with a review of the literature. Acta Neurochir (Wien). 2021. 163: 2629-37
14. Yamashima T, Friede RL. Why do bridging veins rupture into the virtual subdural space?. J Neurol Neurosurg Psychiatry. 1984. 47: 121-7