- Department of Neurological Surgery, University of California, San Francisco, California, USA
- Department of Pathology, University of California, San Francisco, California, USA
- Department of Anesthesia and Perioperative Care, University of California, San Francisco, California, USA
Correspondence Address:
Line Jacques
Department of Neurological Surgery, University of California, San Francisco, California, USA
DOI:10.4103/sni.sni_80_17
Copyright: © 2017 Surgical Neurology International This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Derek G. Southwell, Joseph A. Osorio, Christopher S. Liverman, Lauren M. Friedman, Ramana K. Naidu, Lawrence R. Poree, Melanie M. Henry, Line Jacques. Intrathecal catheter-associated inflammatory mass in a neurofibromatosis type-1 patient receiving fentanyl and bupivacaine. 25-Jul-2017;8:159
How to cite this URL: Derek G. Southwell, Joseph A. Osorio, Christopher S. Liverman, Lauren M. Friedman, Ramana K. Naidu, Lawrence R. Poree, Melanie M. Henry, Line Jacques. Intrathecal catheter-associated inflammatory mass in a neurofibromatosis type-1 patient receiving fentanyl and bupivacaine. 25-Jul-2017;8:159. Available from: http://surgicalneurologyint.com/surgicalint-articles/intrathecal-catheter%e2%80%91associated-inflammatory-mass-in-a-neurofibromatosis-type%e2%80%911-patient-receiving-fentanyl-and-bupivacaine/
Abstract
Background:Catheter-associated inflammatory masses (CIMs) are a rare but serious complication of intrathecal drug delivery devices. CIM formation is influenced by local medication concentration, which is determined in part by flow dynamics at the catheter tip. Underlying spinal pathologies, such as neoplasms, may alter flow at the catheter tip, thereby contributing to CIM formation. Moreover, they may also complicate the clinical and radiologic diagnosis of a CIM.
Case Description:A 36-year-old man with neurofibromatosis type 1 presented to our emergency department with complaints of increased back pain and leg weakness. To treat pain secondary to his multiple spinal masses, he had previously undergone placement of an implantable drug delivery system, which infused a compounded drug of fentanyl and bupivacaine. Imaging studies depicted numerous masses consistent with neurofibromatosis, including a compressive mass located circumferentially at the porous catheter terminus and proximal to the catheter tip. Surgical removal of this mass was performed; pathologic findings were consistent with a catheter tip granuloma.
Conclusions:In the described case, CIM formation likely resulted from a combination of, 1) an unusually high fentanyl concentration, and, 2) altered infusate flow due to spinal neurofibromas. Consideration of underlying spinal pathologies, particularly mass lesions, is critical to the management of intrathecal drug delivery devices.
Keywords: Catheter-associated inflammatory mass, chronic pain, fentanyl pump, granuloma, intraspinal drug therapy, intrathecal catheter
INTRODUCTION
Catheter-associated inflammatory masses (CIMs), traditionally referred to as “catheter granulomas,” are a rare but potentially serious complication of intrathecal drug delivery devices. These masses, which typically occur near the tip of implanted drug catheters, and comprise a range of pathologically defined abnormalities, including intrathecal and intraparenchymal granulomas, epidural fibrosis, drug precipitates, and infectious collections.[
Here we describe a neurofibromatosis type-1 patient, who presented with a symptomatic spinal mass in the setting of an intrathecal fentanyl and bupivacaine pump. The mass, initially thought by referring physicians to be a nerve sheath tumor, was resected and found to be a catheter granuloma. In this case, the tip of the catheter was compressed by a neurofibroma, which caused the catheter to take on a concave shape, likely altering the dispersion of the intrathecal infusate. We believe this, along with excessively high medication dosages, resulted in the formation of the CIM. The patient received immediate surgical intervention to prevent permanent spinal cord injury and made good neurologic recovery.
CASE DESCRIPTION
History and presentation
In August of 2015, a 36-year-old man with neurofibromatosis type 1, multiple peripheral nerve sheath tumors and chronic pain presented to our emergency department with complaints of worsening back pain and progressive right leg weakness. In 2010, he had undergone placement of an intrathecal catheter and drug infusion pump at an outside hospital. At the time of presentation, the pump was administering 8.9 mg/day of fentanyl and 22.2 mg/day of bupivacaine (fentanyl concentration, 14 mg/mL; bupivacaine concentration, 35 mg/mL). Ten days prior to presentation, the patient had undergone lumbar epidural steroid injection at an outside hospital for complaints of cramping in his bilateral quadriceps. Five days prior to presentation, he noted onset of paresthesias in his right foot, then, 3 days prior to presentation, he began to experience progressive right leg weakness resulting in an inability to ambulate. He denied any history of recent trauma.
Examination and initial treatment
Motor examination revealed full strength in the bilateral arms and left leg. The right leg was flaccid, with 2/5 right hip flexor strength, and 1/5 strength in all other muscle groups. Bilateral numbness was noted below the T8 level, and was more pronounced in the left leg. Reflex examination revealed diminished patellar reflexes; myoclonus was absent.
Spinal imaging was performed [
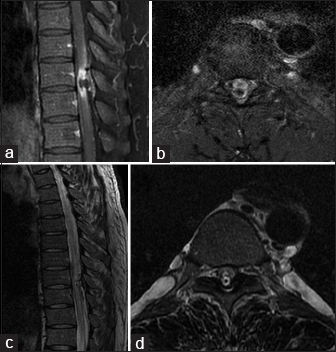
Figure 1
Gadolinium-enhanced T1-weighted sagittal (a) and axial (b) magnetic resonance images depicting the catheter-associated intrathecal granuloma. T2-weighted sagittal image (c) depicts extensive hyperintensity from the T4 level to the conus. T2-weighted axial image (d) depicts spinal cord compression from the dorsal intrathecal granuloma
Given the patient’s rapid neurologic decline, and radiologic evidence of thoracic spinal cord compression, the patient was admitted for surgical treatment. The intrathecal pump was set to the minimum infusion rate. The patient was given dexamethasone (4 mg every 6 h) for spinal cord inflammation, and he received systemic pain medications, including intravenous fentanyl and ketamine (200 μg/h and 2 μg/kg/min, respectively), transdermal clonidine (200 μg/day), and intravenous methadone (10 mg every 8 h). His outpatient oral medications were continued (baclofen 10 mg every 8 h and oxycodone 30–60 mg every 4 h as needed). A fiducial screw was percutaneously placed using computed tomography guidance at the right T9 lamina.
Operation and pathology findings
On the day after admission, the patient was taken to the operating room for thoracic spinal decompression. A T9-T10 laminectomy was performed to expose the thecal sac at the level of the lesion. At the T9-T10 left neuroforamen, a 1.1 cm × 0.4 cm × 0.2 cm mass was adhered to the exiting nerve root; this lesion was resected and later identified by pathological examination to be a neurofibroma. The exposed dura was incised, revealing an adherent, 1.2 cm × 0.6 cm × 0.5 cm, soft tissue mass just proximal to the terminus of the intrathecal catheter [
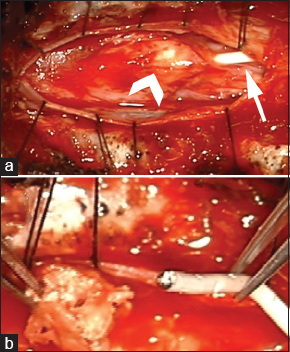
Figure 2
Microscope images obtained during resection of the intrathecal catheter-associated granuloma. (a) Prior to resection, the granuloma (chevron) surrounded the distal end catheter (arrowhead). (b) The granuloma (at left) was separated from the distal end of the catheter (right) and spinal cord. Image orientation, cephalad at left
The spinal segment of the catheter was then removed through a small incision over the lumbar region. The implanted drug pump and the abdominal portion of the catheter were left in place for potential future pain management. A needle was used to access the pump reservoir; the fentanyl-bupivacaine admixture was removed, and replaced with sterile saline. The pump was then confirmed to be in minimum rate to avoid damage to the internal pump mechanism and allow for future reactivation.
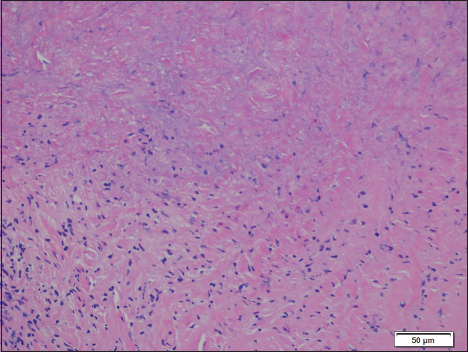
On histologic examination, the catheter-associated mass was found to contain dense fibrous tissue with necrotic debris and chronic inflammation, consistent with granuloma [
Postoperative course
Following surgery, the patient’s right leg strength began to improve, and his lower body sensation returned. Five days after surgery, at the time of discharge, he exhibited full strength throughout his left lower extremity, and 4/5 strength throughout his right lower extremity. The patient did not experience withdrawals from cessation of intrathecal therapy; his pain was managed with fentanyl infusion, methadone, transdermal clonidine, and a low-dose ketamine infusion. Sensation was intact in his left leg, and it had improved in his right leg. The patient was able to ambulate with a walker, and reported pain equal to his baseline, presurgical level.
The patient’s discharge pain medication regimen consisted of transdermal fentanyl (200 μg/h), transdermal clonidine (200 μg/day), oral methadone (10 mg every 8 h), oral baclofen (10 mg every 8 h), and oral oxycodone (30–60 mg every 4 h, as needed).
DISCUSSION
The patient described here presented with complaints typical of CIM, namely, increasing medication infusion requirements and a severe, new neurological deficit. However, this case is unique in that: 1) Preoperative identification of the CIM was complicated by his spinal neurofibromatosis, 2) The catheter tip abutted a spinal tumor, caused a deflection in the catheter which likely impaired the flow of cerebrospinal fluid and intrathecal medication, and 3) The patient received a compound formulation of fentanyl and bupivacaine that contained a rather high concentration of fentanyl (14 mg/mL).
The formation of an intrathecal CIM typically manifests as a slow reduction in pain control, which may then be followed by new, progressive neurologic deficit.[
Other case reports have described catheter tip masses that mimicked other pathologic entities, such as epidural hematoma or spinal cord neoplasm.[
CIM formation has been described in cases involving opioids such as morphine, hydromorphone, diamorphine, sufentanil, and tramadol, as well as non-opioids such as baclofen.[
To our knowledge, this is only the second description of a CIM in a patient receiving intrathecal fentanyl.[
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Allen JW, Horais KA, Tozier NA, Yaksh TL. Opiate pharmacology of intrathecal granulomas. Anesthesiology. 2006. 105: 590-8
2. Andres J, Tatay Vivo J, Palmisani S, Villanueva Perez VL, Minguez A. Intrathecal granuloma formation in a patient receiving long-term spinal infusion of tramadol. Pain Med. 2010. 11: 1059-62
3. Coffey RJ, Burchiel K. Inflammatory mass lesions associated with intrathecal drug infusion catheters: Report and observations on 41 patients. Neurosurgery. 2002. 50: 78-86
4. Deer T, Krames ES, Hassenbusch S, Burton A, Caraway D, Dupen S. Management of intrathecal catheter-tip inflammatory masses: An updated 2007 consensus statement from an expert panel. Neuromodulation. 2008. 11: 77-91
5. Deer TR, Pope JE, Hayek S, Lamer TJ, Veizi IE, Erdek M. The Polyanalgesic Consensus Conference (PACC): Recommendations for Intrathecal Drug Delivery: Guidance for Improving Safety and Mitigating Risks. Neuromodulation. 2017. p.
6. Deer TR, Prager J, Levy R, Rathmell J, Buchser E, Burton A. Polyanalgesic Consensus Conference-2012: Consensus on diagnosis, detection, and treatment of catheter-tip granulomas (inflammatory masses). Neuromodulation. 2012. 15: 483-96
7. Duarte R V, Raphael JH, Southall JL, Baker C, Ashford RL. Intrathecal granuloma formation as result of opioid delivery: Systematic literature review of case reports and analysis against a control group. Clin Neurol Neurosurg. 2012. 114: 577-84
8. Fernandez J, Madison-Michael L, Feler C. Catheter Tip Granuloma Associated with Sacral Region Intrathecal Drug Administration. Neuromodulation. 2003. 6: 225-8
9. Gupta A, Martindale T, Christo PJ. Intrathecal catheter granuloma associated with continuous sufentanil infusion. Pain Med. 2010. 11: 847-52
10. Hassenbusch S, Burchiel K, Coffey RJ, Pen S Du, Follett KA, Krames E. Management of Intrathecal Catheter-Tip Inflammatory Masses. Pain Med. 2002. 3: 313-24
11. Jhas S, Tuli S. Intrathecal catheter-tip inflammatory masses: An intraparenchymal granuloma. J. Neurosurg Spine. 2008. 9: 196-9
12. McMillan MR, Doud T, Nugent W. Catheter-associated masses in patients receiving intrathecal analgesic therapy. Anesth Analg. 2003. 96: 186-90
13. Medel R, Pouratian N, Elias WJ. Catheter-tip mass mimicking a spinal epidural hematoma. J Neurosurg Spine. 2010. 12: 66-71
14. Murphy PM, Skouvaklis DE, Amadeo RJJ, Haberman C, Brazier DH, Cousins MJ. Intrathecal catheter granuloma associated with isolated baclofen infusion. Anesth Analg. 2006. 102: 848-52
15. Mutagi H, Chavan S, Kapur S, Raphael J SJ. First report of diamorphine associated intrathecal catheter-tip granuloma. Reg Anesth Pain Med. 2007. 32: 67-
16. North RB, Cutchis PN, Epstein JA, Long DM. Spinal cord compression complicating subarachnoid infusion of morphine: Case report and laboratory experience. Neurosurgery. 1991. 29: 778-84
17. Osborn AG.editorsDiagnostic Neuroradiology. St Louis: Mosby; 1993. p.
18. Perren F, Buchser E, Chédel D, Hirt L, Maeder P, Vingerhoets F. Spinal cord lesion after long-term intrathecal clonidine and bupivacaine treatment for the management of intractable pain. Pain. 2004. 109: 189-94
19. Wadhwa RK, Shaya MR, Nanda A. Spinal cord compression in a patient with a pain pump for failed back syndrome: A chalk-like precipitate mimicking a spinal cord neoplasm: Case report. Neurosurgery. 2006. 58: E387-
20. Yaksh TL, Hassenbusch S, Burchiel K, Hildebrand KR, Page LM, Coffey RJ. Inflammatory masses associated with intrathecal drug infusion: A review of preclinical evidence and human data. Pain. 2002. 3: 300-12
21. Zacest A, Carlson J, Nemecek A, Burchiel K. Surgical Management of Spinal Catheter Granulomas: Operative Nuances and Review of the Surgical Literature. Neurosurgery. 2009. 65: 1161-5






Joe Ordia, MD
Posted August 6, 2017, 9:21 am
I congratulate the authors for making a prompt diagnosis, performing excellent surgical decompression and excision, and a gratifying surgical outcome.
One consideration would have been to replace the intrathecal catheter and position the tip at about T11 (away from the CIM excision). This would likely have obviated the need for such high doses of opioid at discharge, calculated to be over 1000 daily Morphine Milligram Equivalent.