- Department of Neurosurgery, Montefiore Medical Center, New York, USA
- Department of Neurology, Weill Cornell Medical College, New York Presbyterian Queens Hospital, New York, USA
Correspondence Address:
Adam Ammar
Department of Neurosurgery, Montefiore Medical Center, New York, USA
DOI:10.4103/sni.sni_482_17
Copyright: © 2018 Surgical Neurology International This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.How to cite this article: Adam Ammar, Reza Zarnegar, Reza Yassari, Merritt Kinon. Large central lumbar disc herniation causing acute cauda equina syndrome with loss of evoked potentials during prone positioning for surgery. 19-Mar-2018;9:66
How to cite this URL: Adam Ammar, Reza Zarnegar, Reza Yassari, Merritt Kinon. Large central lumbar disc herniation causing acute cauda equina syndrome with loss of evoked potentials during prone positioning for surgery. 19-Mar-2018;9:66. Available from: http://surgicalneurologyint.com/surgicalint-articles/large-central-lumbar-disc-herniation-causing-acute-cauda-equina-syndrome-with-loss-of-evoked-potentials-during-prone-positioning-for-surgery/
Abstract
Background:Few studies in the literature discuss operative positioning for lumbar surgery precipitating acute cauda equina syndromes (CES).
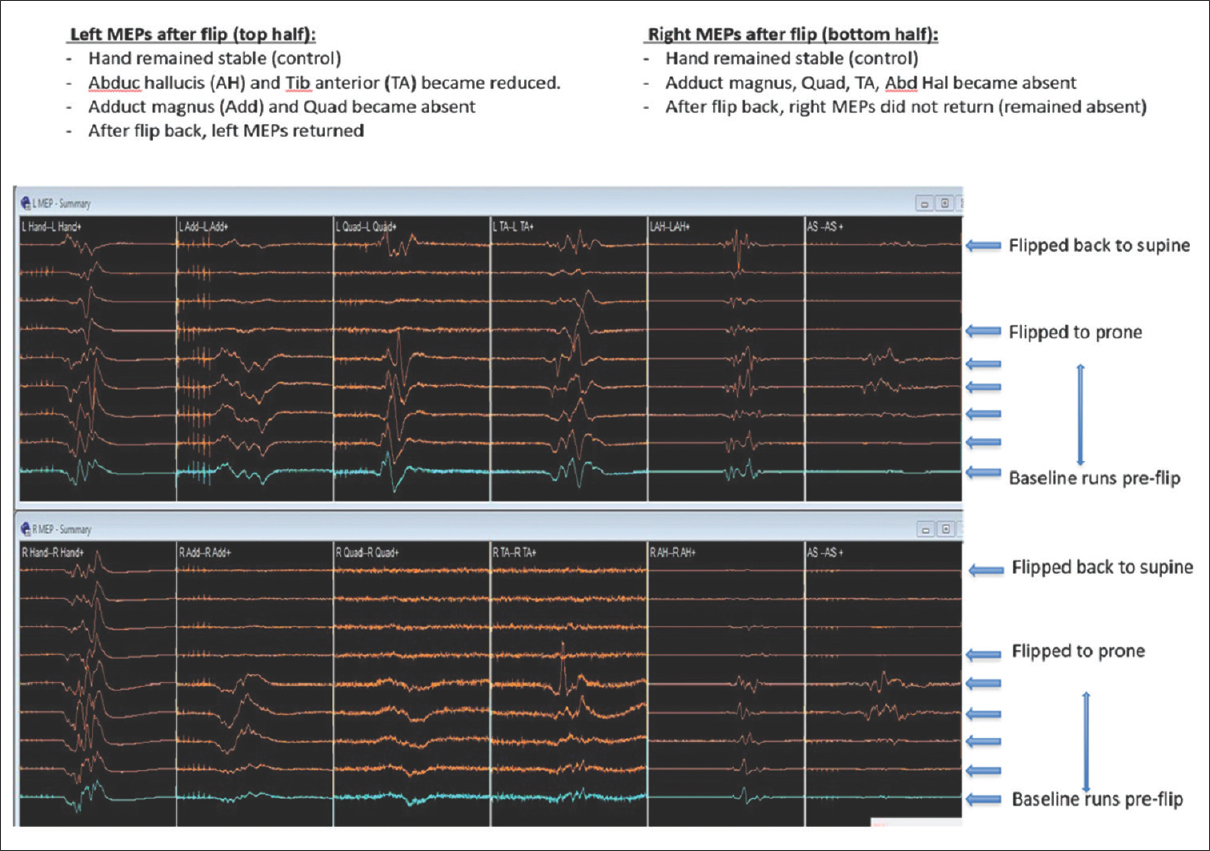
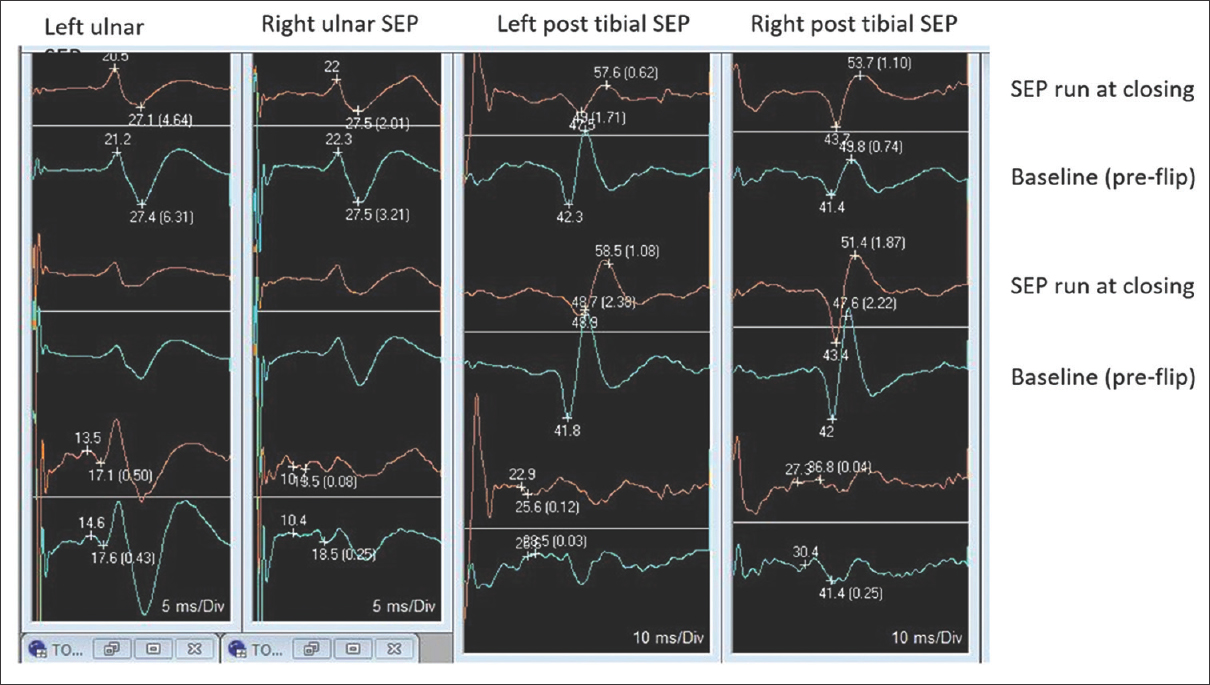
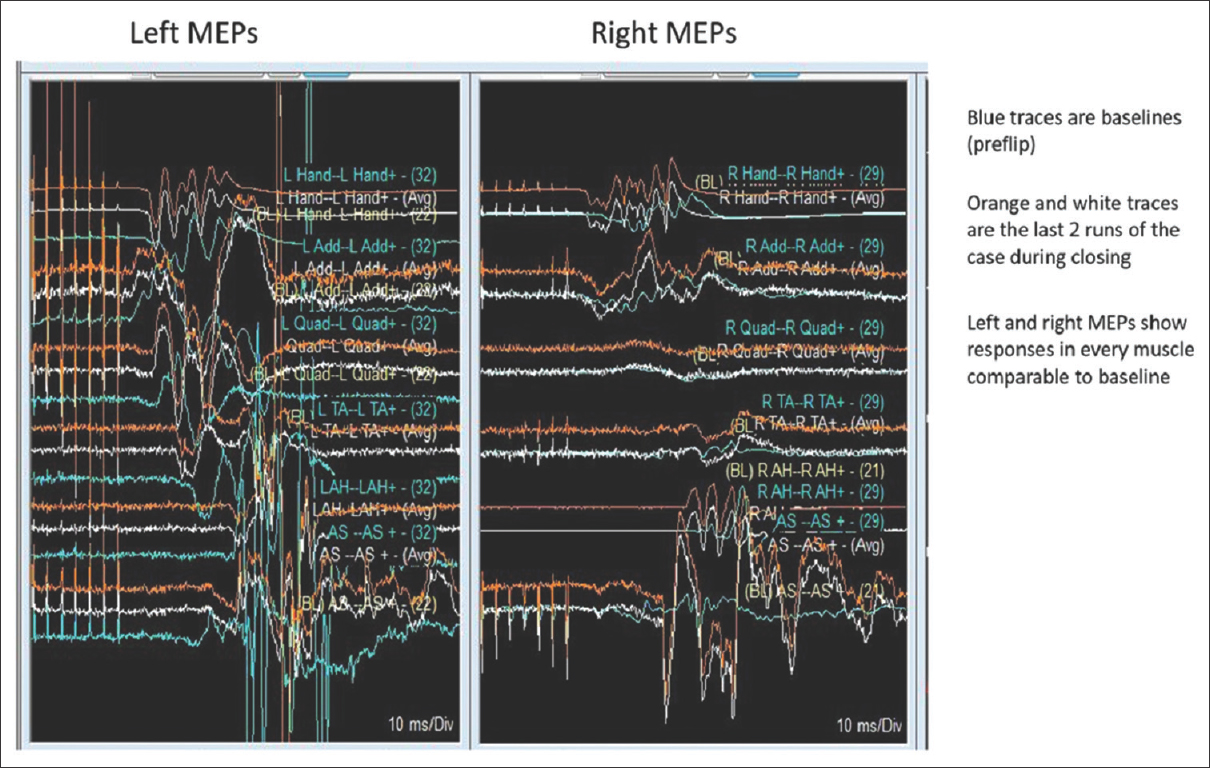
Case Description:A 56-year-old male with a large L2-3-disc herniation was placed prone on a Jackson table. He immediately lost all motor and sensory evoked potentials. Signals returned to the baseline when surgery was aborted, and he was returned to the supine position. However, potentials were again lost when he was repositioned prone, following which the surgeons proceeded with surgical decompression with a good outcome.
Conclusion:This case highlights the risk for patients with large acute lumbar disc herniation/stenosis and CES undergoing prone positioning for lumbar decompression. Here, despite the secondary loss of both sensory and motor evoked potentials, the patient successfully underwent lumbar decompressive surgery/discectomy performed on a Jackson table, resulting in full postoperative neurological recovery.
Keywords: Acute cauda equina syndrome, lumbar disc, motor evoked potentials, positional, somatosensory evoked potentials, stenosis
INTRODUCTION
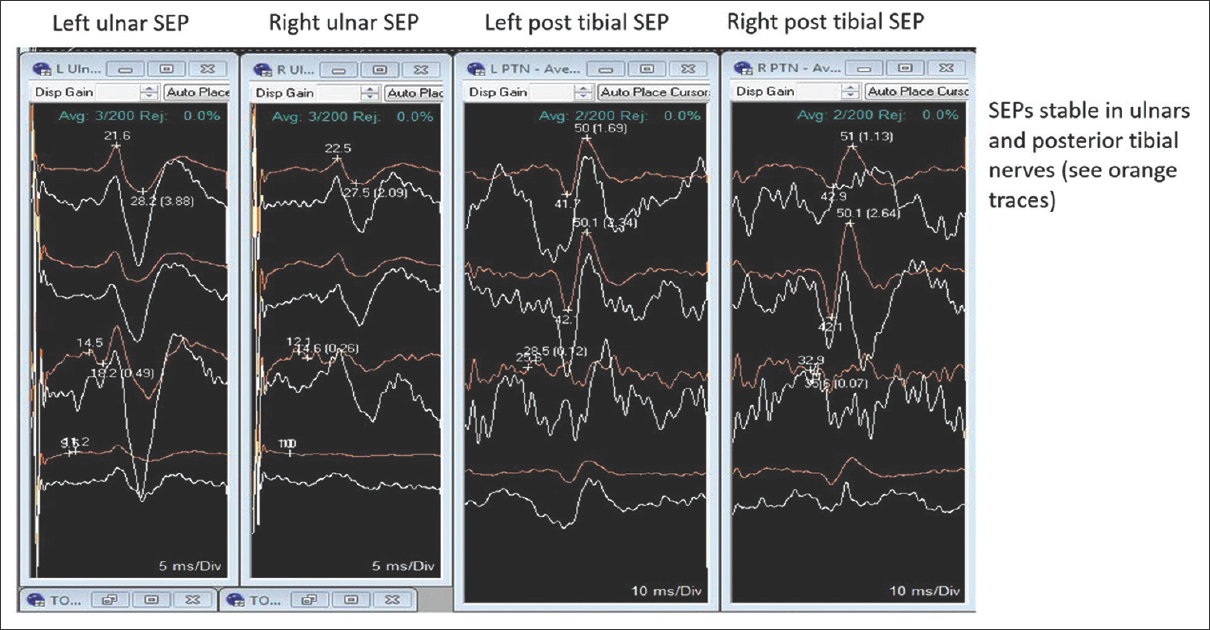
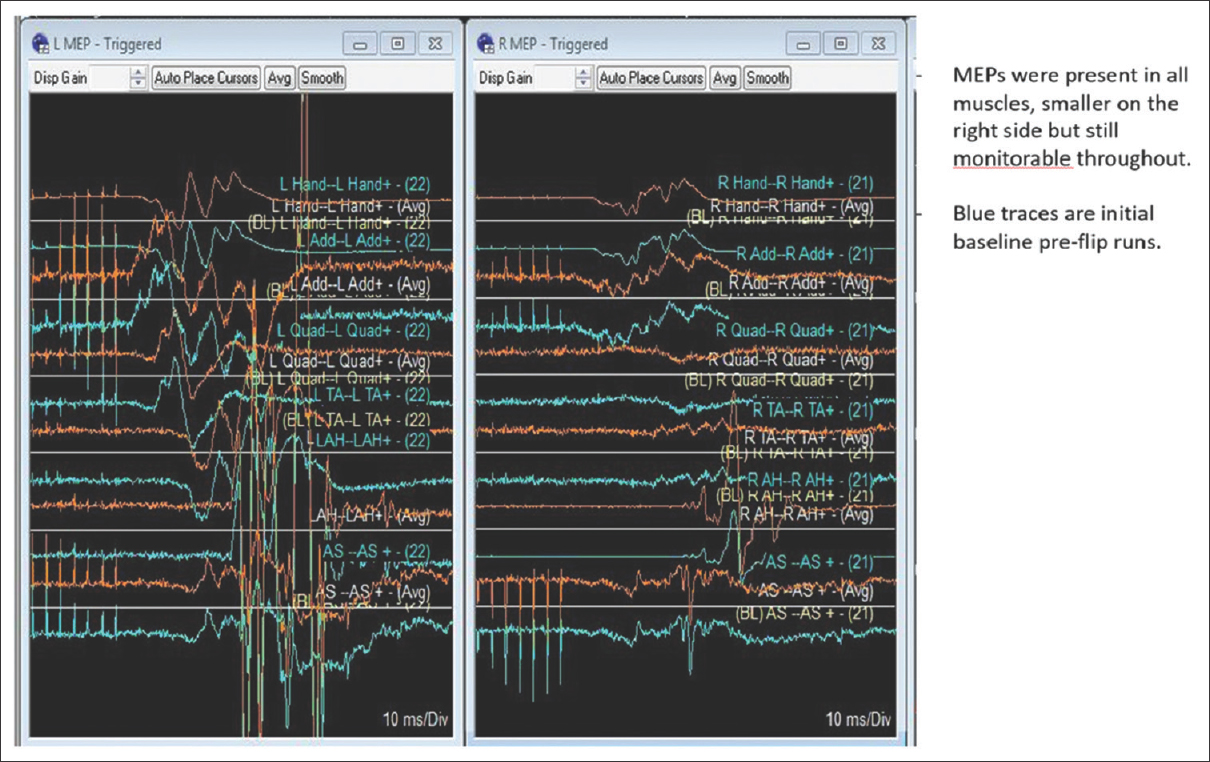
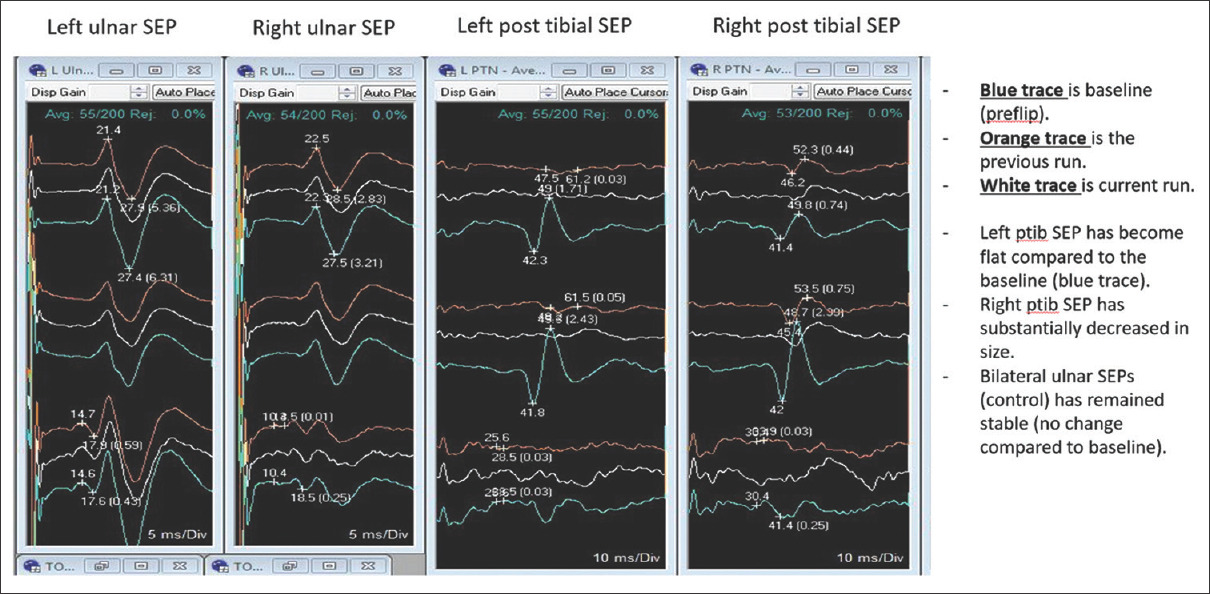
When patients with severe lumbar stenosis/acute lumbar disc herniation are placed prone for spinal surgery, they rarely exhibit acute loss of both sensory/motor evoked potentials (SEP/MEP). Here, we present a patient who twice exhibited the complete and immediate loss of SEP/MEP when placed prone on a Jackson table for excision of a large L2-L3-disc herniation with stenosis.[
CASE HISTORY
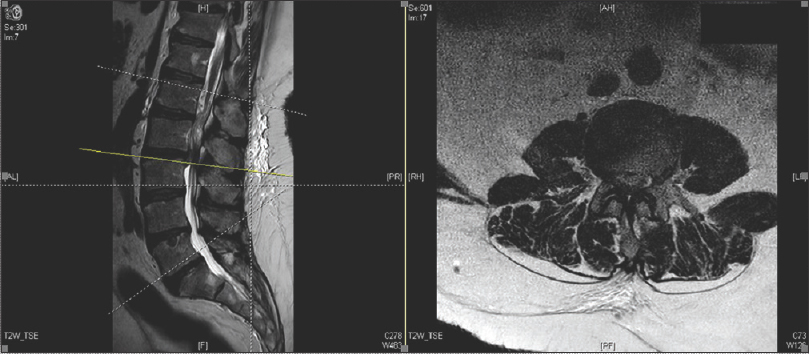
A 56-year-old obese male presented with 7 days of low back pain radiating down both lower extremities accompanied by a mild 4/5 right foot drop. The lumbar magnetic resonance imaging (MRI) demonstrated a large L2-3 central disc herniation/stenosis resulting in marked thecal sac/nerve root compression [
DISCUSSION
Intraoperative neurophysiologic monitoring is useful in predicting neurologic compromise in patients with significant compressive spinal pathologies.[
Although SEP/MEPs were lost both times the patient was placed prone on the Jackson table prior to surgery, the second time it was elected to proceed with an immediate decompression. Potentials likely dropped due to prone positioning on the Jackson table – the position probably acutely increased the lumbar lordosis, exacerbated the stenosis, and increased the epidural pressure.[
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Chau AM, Xu LL, Pelzer NR, Gragnaniello C. Timing of surgical intervention in cauda equina syndrome: A systematic critical review. World Neurosurg. 2014. 81: 640-50
2. Chung SS, Lee CS, Kim SH, Chung MW, Ahn JM. Effect of low back posture on the morphology of the spinal canal. Skeletal Radiol. 2000. 29: 217-23
3. Gardner A, Gardner E, Morley T. Cauda equina syndrome: A review of the current clinical and medico-legal position. Eur Spine J. 2011. 20: 690-7
4. Lavy C, James A, Wilson-Macdonald J, Fairbank J. Cauda equina syndrome. BMJ. 2009. 338: b936-
5. Ofiram E, Lonstein JE, Skinner S, Perra JH. “The disappearing evoked potentials”: A special problem of positioning patients with skeletal dysplasia: Case report. Spine. 2006. 31: E464-70
6. Pease M, Gandhoke GS, Kaur J, Thirumala P, Balzer J, Crammond D. Predictive Value of Intraoperative Neurophysiological Monitoring During Spine Surgery: A Prospective Analysis of 4489 Consecutive Patients. Neurosurgery. 2016. 63: 192-3
7. Raynor BL, Bright JD, Lenke LG, Rahman RK, Bridwell KH, Riew KD. Significant change or loss of intraoperative monitoring data: A 25-year experience in 12,375 spinal surgeries. Spine. 2013. 38: E101-8