- Grant Medical Center, Department of Neurosurgery, Ohio Health, Columbus, Ohio, USA
Correspondence Address:
Jason Milton
Grant Medical Center, Department of Neurosurgery, Ohio Health, Columbus, Ohio, USA
DOI:10.4103/sni.sni_250_18
Copyright: © 2018 Surgical Neurology International This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.How to cite this article: Zubair Ahammad, Jason Milton, Kailash Narayan, Victor Awuor. Lateral position and utility of navigation for posterior fixation of unstable cervical fracture with ankylosing spondylitis. 02-Nov-2018;9:225
How to cite this URL: Zubair Ahammad, Jason Milton, Kailash Narayan, Victor Awuor. Lateral position and utility of navigation for posterior fixation of unstable cervical fracture with ankylosing spondylitis. 02-Nov-2018;9:225. Available from: http://surgicalneurologyint.com/surgicalint-articles/9061/
Abstract
Background:Ankylosing spondylitis (AS) is a seronegative spondyloarthropathy within the spectrum of rheumatologic diseases. The systemic inflammation that characterizes AS leads to bone resorption and reformation. Pathologic remodeling may include kyphosis, osteoporosis, and multi-segment auto-fusion. Cervical fractures account for 53–78% of spinal trauma seen with AS. Surgical planning is often challenging owing to spinal deformity, medical comorbidities, the cervicothoracic foci of injury, and gross instability of these fracture.
Case Description:A 55-year-old male with AS was presented with a three-column injury at the C6 level. The C6 vertebra was fractured, minimally displaced, and there was a focal kyphotic deformity. Attempted posterior fixation 2 days after presentation was aborted; the patient could not tolerate prone positioning, and there were further technical limitations to a posterior approach. Cervicothoracic fixation from C2 to T2 was then performed using the right lateral decubitus position employing the Mayfield head holder, a beanbag, and spinal neuronavigation.
Conclusion:In this study, we presented a unique approach to posterior fixation of an unstable cervicothoracic fracture in a patient with AS utilizing the lateral position and neural navigation under intraoperative physiological monitoring.
Keywords: Ankylosing spondylitis, cervical, navigation, spine, trauma
INTRODUCTION
Ankylosing spondylitis (AS) is a seronegative spondyloarthropathy within the spectrum of rheumatologic diseases. There is a correlation with HLA-B27 and associated uveitis, inflammatory bowel disease, and sacroiliitis.[
Fracture risk of ankylosing spondylitis
With AS, there is a fourfold increased risk of spinal fracture even with minor trauma; this correlates with a greater than 20% risk of associated spinal cord injury.[
Surgical planning with cervical ankylosing spondylitis
Surgical planning is often challenging owing to AS spinal deformity, medical comorbidities, the cervicothoracic locus of injury, and gross instability. An increased propensity for iatrogenic displacement and resultant neurological decline has been reported, particularly involving worsening with operative positioning.[
CASE DESCRIPTION
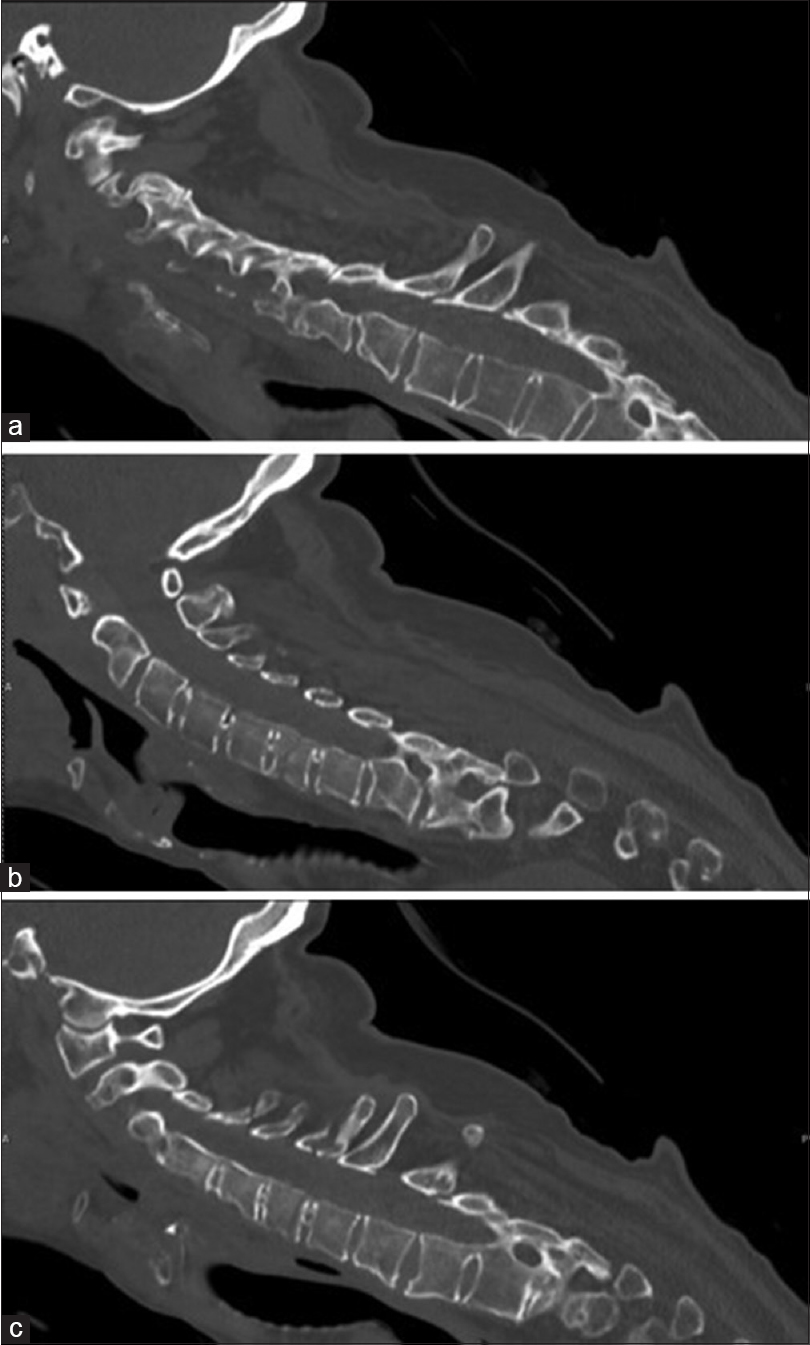
A 55-year-old male with AS was presented with neck pain after falling off from a table while incarcerated. The non-contrast cervical computed tomography (CT) revealed a transverse three column fracture of the C6 cervical vertebra with minimal displacement; there was a mild kyphotic deformity and attendant evidence of multilevel auto-fusion of the spine consistent with the diagnosis of AS [
Initial failed attempt at surgical positioning and treatment of C6 Vertebral fracture
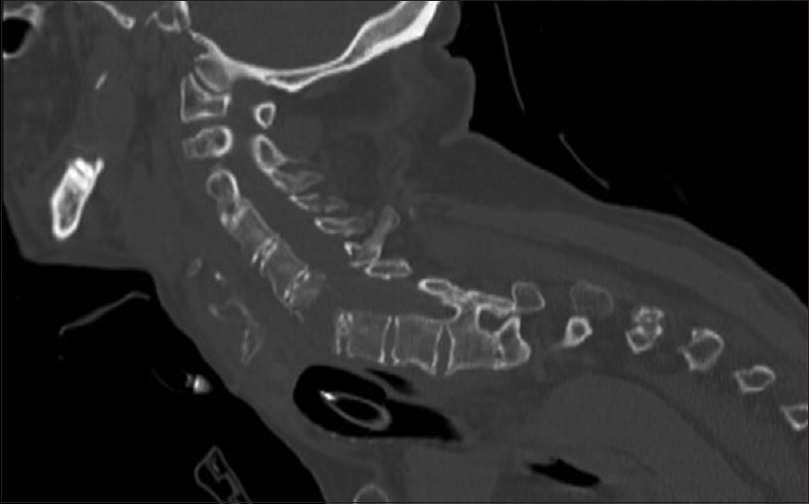
Originally, the patient was intubated, and posterior fixation was attempted but aborted 2 days after admission (e.g., elevated peek pressures, inability to ventilate, and severe kyphosis). Somatosensory evoked potentials (SSEP) and motor evoked potentials (MEP) prior to and after positioning remained unchanged from baseline. The CT of the cervical spine following this aborted procedure revealed significant new malalignment and distraction of the fracture margin [
Secondary lateral surgical positioning and treatment of C6 vertebral fracture
Further, a cervicothoracic fusion from C2 to T2 was performed in the right lateral decubitus position using the Mayfield head holder, a beanbag, and spinal neuronavigation. Throughout surgery, the SSEP and MEP signals were stable (e.g., before, after positioning, and postoperatively).
Reduction of the fracture was achieved predominately by positioning the patient in the Mayfield head rest. Segmental instrumentation with cervical lateral mass screws and thoracic pedicle screws was performed uneventfully. This was followed by posterolateral arthrodesis with allograft.
Outcome
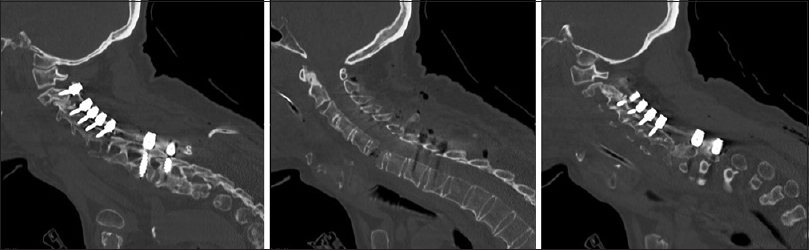
Three weeks later, the patient remained neurologically intact and the wound healed. The postoperative CT confirmed adequate alignment, intact instrumentation, and a good reduction of the injury [
DISCUSSION
Multiple factors increase the complexity and risk of surgical stabilization in patients with AS. Preoperative considerations often include greater medical comorbidities, such as severe hypoventilation due to hyperkyphosis.[
Failure of conservative treatment for ankylosing spondylitis
Conservative measures including bracing, traction, and halo fixation have significant complications that include pseudoarthrosis, progression of kyphosis, neurologic deterioration, and skin breakdown.[
More success with surgery for ankylosing spondylitis
Surgical management improves survival and functional outcomes for AS.[
Lateral operative approach to ankylosing spondylitis
Isolated posterior long-segment fixation has correlated with favorable radiographic and clinical outcomes.[
CONCLUSION
This case of AS uniquely demonstrates that an unstable cervicothoracic fracture (centered at C6) can be treated surgically utilizing the lateral position with neuronavigation. Circumvention of positioning difficulties allows for posterior long-segment fixation in the setting of severe anatomic abnormalities.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Choi D. Fractures in Ankylosing Disorders of the Spine: Easy to Miss and High Risk of Deterioration. World Neurosurg. 2015. 83: 1029-1031
2. El Tecle NE, Abode-Iyamah KO, Hitchon PW, Dahdaleh NS. Management of spinal fractures in patients with ankylosing spondylitis. Clin Neurol Neurosurg. 2015. 139: 177-182
3. Kouyoumdjian P, Guerin P, Schaelderle C, Asencio G, Gille O. Fracture of the lower cervical spine in patients with ankylosing spondylitis: Retrospective study of 19 cases. Orthop Traumatol Surg Res. 2012. 98: 543-551
4. Lazennec JY, d'Astorg H, Rousseau MA. Cervical spine surgery in ankylosing spondylitis: Review and current concept. Orthop Traumatol Surg Res. 2015. 101: 507-513
5. Leone A, Marino M, Dell'Atti C, Zecchi V, Magarelli N, Colosimo C. Spinal fractures in patients with ankylosing spondylitis. Rheumatol Int. 2016. 36: 1335-1346
6. Lukasiewicz AM, Bohl DD, Varthi AG, Basques BA, Webb ML, Samuel AM. Spinal Fracture in Patients With Ankylosing Spondylitis: Cohort Definition, Distribution of Injuries, and Hospital Outcomes. Spine (Phila Pa 1976). 2016. 41: 191-196
7. Ma J, Wang C, Zhou X, Zhou S, Jia L. Surgical Therapy of Cervical Spine Fracture in Patients With Ankylosing Spondylitis. Medicine. 2015. 94: e1663-
8. Mahajan R, Chhabra HS, Srivastava A, Venkatesh R, Kanagaraju V, Kaul R. Retrospective analysis of spinal trauma in patients with ankylosing spondylitis: A descriptive study in Indian population. Spinal Cord. 2015. 53: 353-357
9. Robinson Y, Robinson AL, Olerud C. Complications and survival after long posterior instrumentation of cervical and cervicothoracic fractures related to ankylosing spondylitis or diffuse idiopathic skeletal hyperostosis. Spine. 2015. 40: E227-233
10. Schiefer TK, Milligan BD, Bracken CD, Jacob JT, Krauss WE, Pichelmann MA. In-hospital neurologic deterioration following fractures of the ankylosed spine: a single-institution experience. World Neurosurg. 2015. 83: 775-783