- Department of Orthopaedics, Seth G.S. Medical College and K.E.M Hospital, Mumbai, Maharashtra, India,
- Department of Spine Services, B. Toronto Western Hospital and Krembil Neuroscience Centre, Toronto, Ontario, Canada.
Correspondence Address:
Rishi Agarwal
Department of Spine Services, B. Toronto Western Hospital and Krembil Neuroscience Centre, Toronto, Ontario, Canada.
DOI:10.25259/SNI_772_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Sudhir Srivastava1, Aditya Raj1, Rishi Agarwal1, Sunil Bhosale1, Nandan Marathe2. Management dilemma of tuberculous paraplegia in pregnancy – A case report and review of literature. 29-Dec-2020;11:470
How to cite this URL: Sudhir Srivastava1, Aditya Raj1, Rishi Agarwal1, Sunil Bhosale1, Nandan Marathe2. Management dilemma of tuberculous paraplegia in pregnancy – A case report and review of literature. 29-Dec-2020;11:470. Available from: https://surgicalneurologyint.com/surgicalint-articles/10498/
Abstract
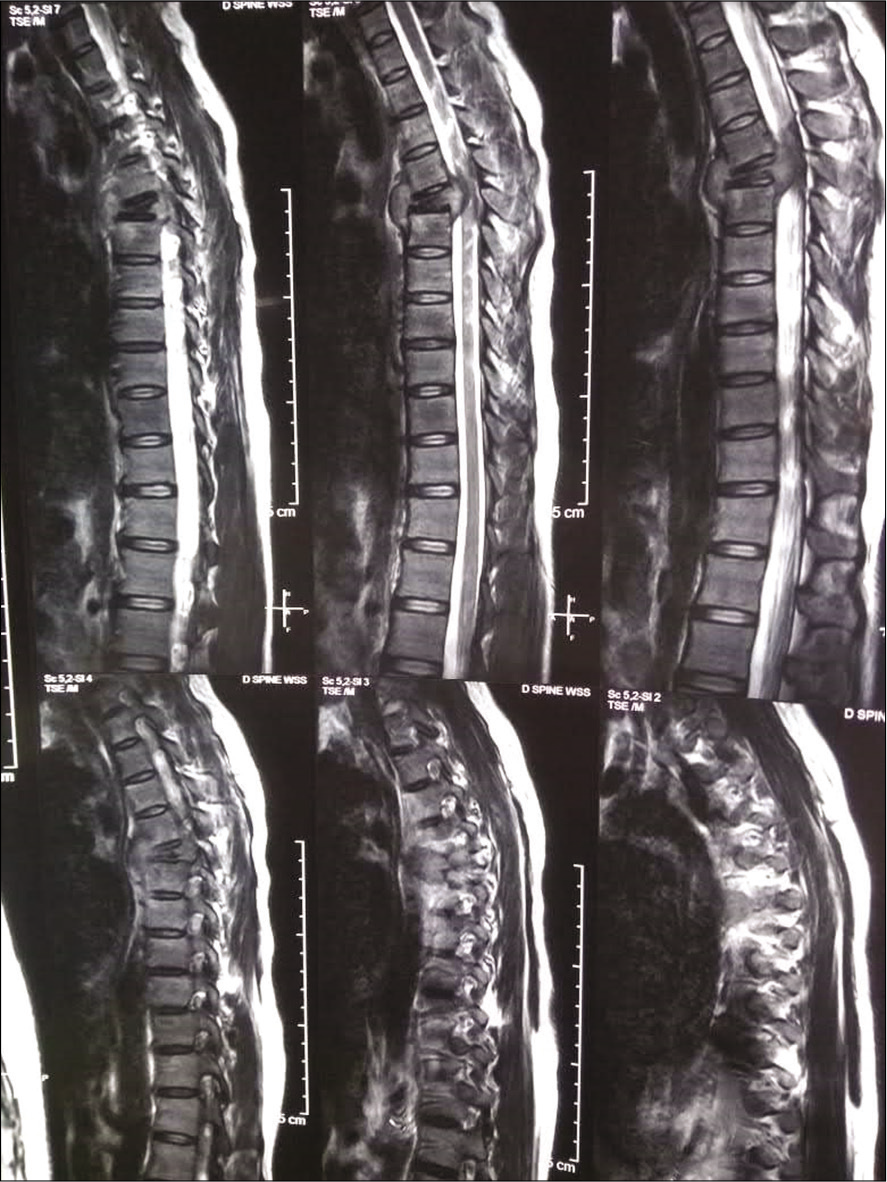
Background: Tuberculosis (TB)/tuberculous spondylodiscitis of the spine causing paraplegia in the 2nd trimester of pregnancy is rare and poses significant management dilemmas. Pregnancy, a relatively immunocompromised state with high hormonal levels, may prompt rapid TB destruction of a vertebral body resulting in an acute/ profound neurological deficit. Here, a pregnant paraplegic mother was diagnosed with spondylodiscitis that warranted immediate decompression/fusion to achieve neurological recovery.
Case Description: A 26-year-old female was 23 weeks pregnant when she presented with an acute spastic paraplegia (complete motor, sensory deficit, and sphincter loss). Operative decompression utilized a Versatile Approach along with a “Hartshill rectangle” for fusion and sublaminar wiring. This procedure accomplished simultaneous anterior and posterior fixation with a single approach without the need for intraoperative radiologic imaging. Although the pregnancy was continued with an uneventful perioperative period, intra-uterine fetal demise was documented 1 month postoperatively. Within 18 postoperative months the patient was neurologically intact, and fusion was confirmed on a computed tomography scan.
Conclusion: A 23-week pregnant female acutely became paraplegic due to T5 tuberculous spondylitis confirmed on an X-ray (only source of radiation), and magnetic resonance imaging. Following a decompression/ instrumented fusion performed without fluoroscopic guidance, the patient regained full neurological function. However, 1 month postoperatively, the fetus spontaneously aborted.
Keywords: Paraplegia in pregnancy, Spinal decompression surgery in pregnancy, Tuberculous paraplegia
INTRODUCTION
Spinal tuberculosis (TB) in pregnancy is rare, and even more infrequent is the acute onset of paraplegia when it occurs in the late second trimester. Here, we reviewed the case of a 26-year-old female, 23 months pregnant, who only underwent a preoperative X-ray along with a magnetic resonance imaging (MRI), and subsequently had decompressive spinal surgery with fusion performed without fluoroscopic guidance. The pregnancy was complicated at presentation with severe intra-uterine growth restriction (IUGR), the fetus spontaneously aborted 1 month postoperatively.
Case A 26-year-old pregnant female G2P2L1 at 23 weeks of gestation developed over a 10 days period subacute onset paraplegia (Frankel A; complete motor, sensory T10 level) with bowel bladder incontinence. Plain radiographs obtained with abdominal shielding showed a collapse of the fifth thoracic vertebral body [
ADMINISTRATION OF ANTI-TB THERAPY
The patient was started on four drug anti-tubercular drug therapy: isoniazid, rifampicin, pyrazinamide, and ethambutol. Tissue diagnosis was avoided as it would involve additional X-ray exposure for obtaining a specimen by fluoroscopy/computed tomography (CT)-guided biopsy. In view of the classic radiologic picture, with widespread cases of TB in our country, plus her history of cervical tubercular lymphadenitis 1 year before presentation, anti-tubercular therapy was started empirically.
OBSTETRIC EVALUATION
An obstetric consult revealed that the fetus was viable but had severe IUGR, with Doppler studies revealing reduced flow in the umbilical artery.
SURGERY
A decompressive laminectomy with instrumented fusion was performed in the thoracic spine. In the left lateral position, the surgeons utilized a “Versatile approach”[
When 3 weeks of antitubercular drug therapy resulted in no neurological recovery, a decision for operative decompression was taken.
PATHOLOGY
The pathology was consistent with necrotizing granulomatous osteomyelitis. Nucleic acid based amplification tests detected the presence of Mycobacterium tuberculosis. On culture, there was growth of M. tuberculosis which was sensitive to all four first-line antitubercular drugs.
POSTOPERATIVE COURSE
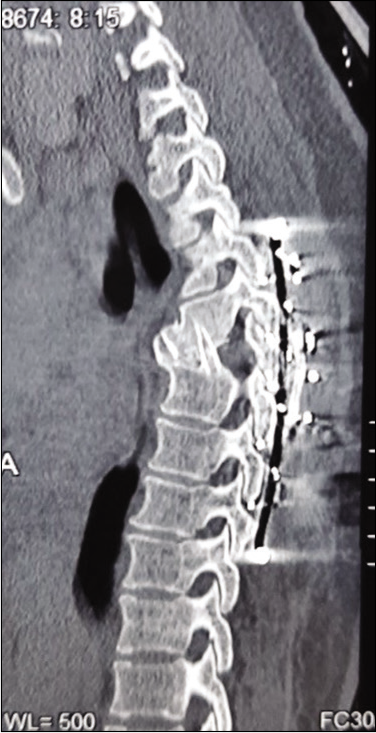
The postoperative course was uneventful. She regained partial power in the lower extremities within the 1st postoperative week. Although spasticity persisted for 14 months, motor recovery was complete at 3 postoperative months, and she additionally regained normal bowel and bladder function. At 18 months, a CT scan documented fusion [
SPONTANEOUS FOETAL ABORTION
Postoperative obstetric ultrasonography showed a single live intrauterine pregnancy with IUGR. However, the 4-week post surgery ultrasound showed reversal of end diastolic flow in the umbilical artery, and eventually confirmed intrauterine fetal demise. Despite the failure to save the fetus in this case, the authors concluded that surgical decompression/fusion for acute paraplegia due to TB of the spine remains a viable option for pregnant patients with significant TB-related neurological deficits.
DISCUSSION
A third to half of the cases of skeletal TB involves the vertebral column, and TB of the spine accounts for about 2% of all cases of TB. There are no well-defined protocols for the management of pregnancy complicated by tuberculous spondylitis with paraplegia in the second trimester of pregnancy. Pregnancy, with high serum steroid levels and a relative immunocompromised state, may enable skeletal TB to become potentially aggressive leading to rapid/profound vertebral destruction and neurological deterioration.[
The first-line drugs rifampicin, isoniazid, and ethambutol are not shown to have any significant adverse maternal-fetal effects or requirement of dose adjustment during pregnancy and in the postpartum period.[
CONCLUSION
Neurological defecit resulting from TB of the spine has a good prognosis if early decompression and stabilization are performed under the cover of antitubercular drug therapy Here, the surgery included a “versatile” approach, which allowed for simultaneous anterior/posterior access to the vertebral column and decompression/fusion. All possible precautions were taken to prevent maternal hypotension, hypothermia, and hypoxia during surgery.
Although the pregnancy resulted in fetal demise in this case, for others maintaining the pregnancy may be a viable option in conjunction with decompression/fusion to reverse major acute neurological deficits associated with TB spondylodiscitis.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Publication of this article was made possible by the James I. and Carolyn R. Ausman Educational Foundation.
Conflicts of interest
There are no conflicts of interest.
References
1. Cunningham F, Grant NF, Loreno KJ, Norman F, Kenneth J, Hauth J.editors. Infections. Williams Obstetrics. New York: McGraw-Hill; 2001. p. 146
2. Guyton AC, Hall JE.editors. Pregnancy and lactation. Textbook of Medical Physiology. Philadelphia, PA: W. B. Saunders Company; 1996. p. 1039
3. Mathad JS, Gupta A. Tuberculosis in pregnant and postpartum women: Epidemiology, management, and research gaps. Clin Infect Dis. 2012. 55: 1532-49
4. Srivastava SK, Aggarwal RA, Bhosale SK, Roy K, Nemade PS. The versatile approach: A novel single incision combined with anterior and posterior approaches for decompression and instrumented fusion to treat tuberculosis of the thoracic spine. Asian Spine J. 2017. 11: 294-304