- Department of Orthopedics, Hospital Español, Mendoza, Argentina,
- Department of Orthopedic, Hospital Italiano de Buenos Aires, Buenos Aires, Argentina,
- Department of Neurosurgery, Hospital Clínico Regional de Concepción, Concepción, Chile,
- Department of Orthopedics, Axial Medical Group, Buenos Aires, Argentina,
- Department of Orthopedic, Hospital Israelita Albert Einstein, Sao Paulo, Brasil,
- Department of Neurosurgery, University of Passo Fundo, Passo Fundo, Brasil,
- Department of Neurosurgery, Clinica Portoazul, Barranquilla, Colombia,
- Department of Medicine, University of Caxias do Sul, Rio Grande do Sul, Brasil.
Correspondence Address:
Alfredo José Guiroy
Department of Orthopedics, Hospital Español, Mendoza, Argentina.
DOI:10.25259/SNI_600_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Alfredo José Guiroy1, Matias Pereira Duarte2, Juan Pablo Cabrera3, Nicolás Coombes4, Martin Gagliardi1, Alberto Gotfryd5, Charles Carazzo6, Nestor Taboada7, Asdrubal Falavigna8. Neurosurgery versus orthopedic surgery: Who has better access to minimally invasive spinal technology?. 11-Nov-2020;11:385
How to cite this URL: Alfredo José Guiroy1, Matias Pereira Duarte2, Juan Pablo Cabrera3, Nicolás Coombes4, Martin Gagliardi1, Alberto Gotfryd5, Charles Carazzo6, Nestor Taboada7, Asdrubal Falavigna8. Neurosurgery versus orthopedic surgery: Who has better access to minimally invasive spinal technology?. 11-Nov-2020;11:385. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=10388
Abstract
Background: Our aim was to evaluate differences in neurosurgeons versus orthopedists access to technologies needed to perform minimally invasive spine surgeries (MISS) in Latin America.
Methods: We sent a survey to members of AO Spine Latin America (January 2020), and assessed the following variables; nationality, level of hospital (primary, secondary, and tertiary), number of spinal operations performed per year, spinal pathologies addressed, the number of minimally invasive spine operations performed/year, and differences in access to MISS spinal technology between neurosurgeons and orthopedists.
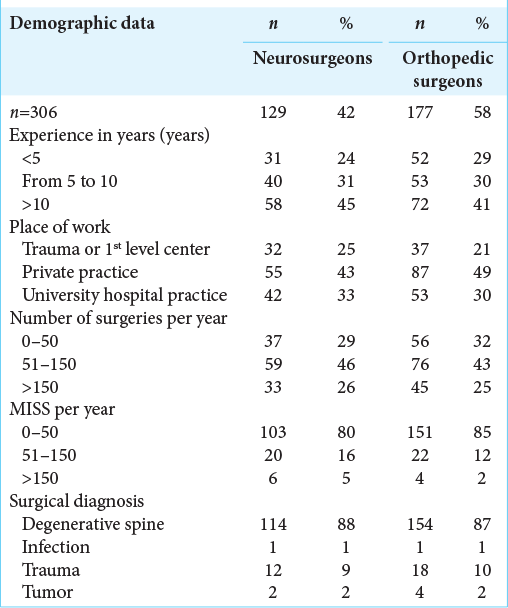
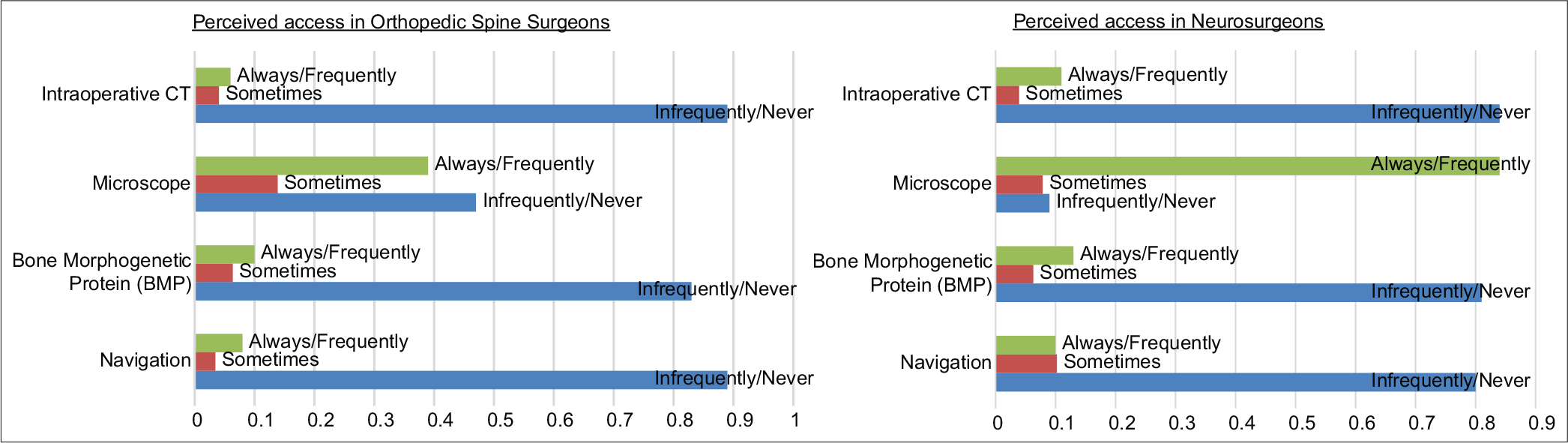
Results: Responses were returned from 306 (25.6) members of AO Spine Latin America representing 20 different countries; 57.8% of respondents were orthopedic surgeons and 42.4% had over 10 years of experience. Although both specialties reported a lack of access to most of the technologies, the main difference between the two was greater utilization/access of neurosurgeons to operating microscope (e.g., 84% of the neurosurgeons vs. 39% of orthopedic spine surgeons).
Conclusion: Although both specialties have limited access to MISS spinal technologies, orthopedic spine surgeons reported significantly lower access to operating microscopes versus neurosurgeons (P
Keywords: Microscope, Minimally invasive spine surgery, Neurosurgeons, Neurosurgery, Orthopedics, Technologies
INTRODUCTION
For Latin America, we evaluated the main obstacles spinal neurosurgeons and orthopedists have to performing minimally invasive spine surgeries (MISS). Variables studied included high MISS implant costs, and limited access to navigation technology, percutaneous screws, and to operating microscopes.[
MATERIALS AND METHODS
Study design
This cross-sectional study utilized a survey to evaluate accessibility to MISS technology in Latin America. Members of AO Spine Latin America received an email with an internet link to the survey.
MISS technology accessibility survey
Emails explaining the study objectives in Spanish and Portuguese were sent to 1192 spinal surgeons (neurosurgeons and orthopedists) in January 2020. All authors were blinded to the identity of the respondents. Once a response was accepted, it was immediately anonymized.
Survey data
In the survey, respondents were asked about their personal practice [
Statistical analysis
Statistical analysis was performed using the statistical software program SPSS (IBM version 25.0, Chicago, IL). Additional cross-tabulation methods were used to assess for any statistically-significant differences between the two surgical specialties, utilizing a Pearson Chi-square analysis. The a-priori criterion for statistical significance was set as P ≤ 0.05.
RESULTS
We received 306 responses (25.6% response rate) from spinal surgeons; 177 were orthopedists (58%) and 129 were neurosurgeons (42%). Notably, 42.4% of all spinal surgeons reported more than 10 years of surgical experience, and performed fewer than 50 MISS procedures per year [
Obstacles to MISS technology
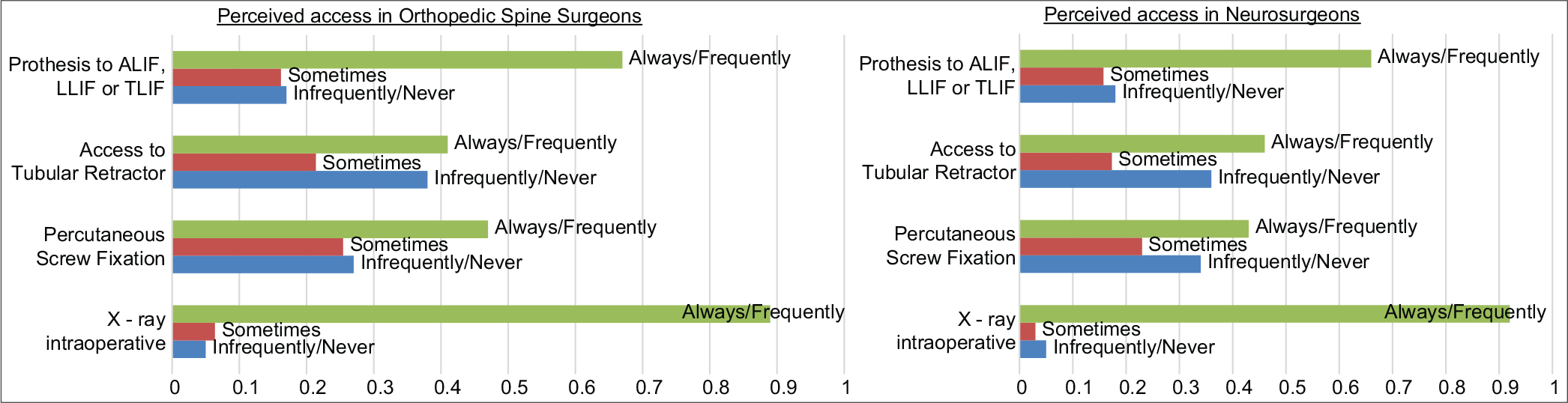
Both neurosurgeons and orthopedic spine surgeons reported limited access to intraoperative CT, bone morphogenetic protein, neuronavigation technology, interbody cages, tubular retractors, intraoperative X-rays, and percutaneous screws [
DISCUSSION
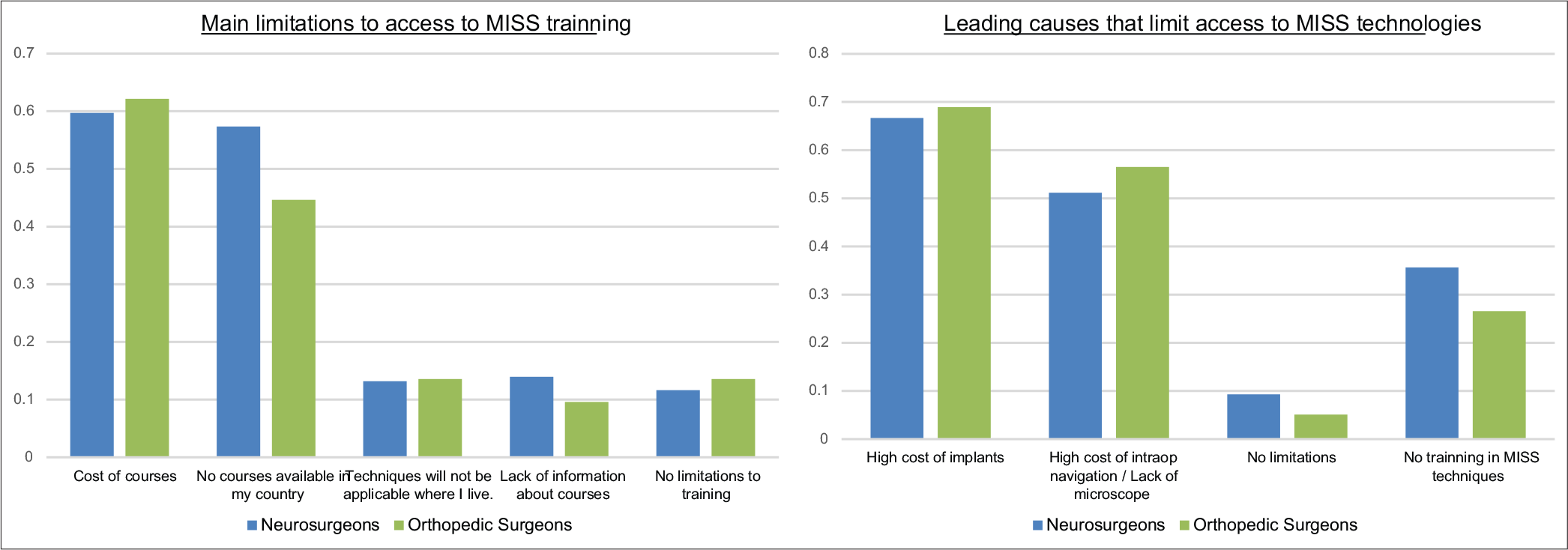
Latin American spinal surgeons have limited access to perform MISS spine surgery due to the; high cost, lack of availability of implants/hardware, and the high cost of neuronavigation. Further, we found that neurosurgeons have more access (84%) to operating microscopes versus orthopedists (39%).[
Of interest, Avellanal et al. determined that neurosurgeons may have greater need for utilizing operating microscope, as they perform 2-times more neural decompressions while orthopedists performed 2.5 times more fusions (instrumented and non-instrumented).[
Further, Pejrona et al. found that neurosurgeons felt more competent dealing with certain cervical pathologies (e.g., spinal tumors) warranting an operating microscope versus orthopedists spinal surgeons who were more frequently treating spinal deformities/pelvic trauma.[
MISS
MISS have inherently greater risks to neural/vertebral structures, as they typically provide more limited/insufficient exposures, restrictive maneuverability, and restrictive operative corridors.[
CONCLUSION
Although both neurosurgeons and orthopedic spine surgeons in Latin America have limited accessing to the technologies for performing MISS, neurosurgeons are better able to utilize operating microscopes versus their orthopedic spinal surgeons’ counterparts.
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgments
This study was organized by the AO Spine Latin America Minimally Invasive Surgery Spine Study Group.
References
1. Avellanal M, Martin-Corvillo M, Barrigon L, Espi MV, Escolar CM. A 1-year cost analysis of spinal surgical procedures in Spain: Neurosurgeons versus orthopedic surgeons. Neurospine. 2019. 16: 354-9
2. Epstein NE. Extreme lateral lumbar interbody fusion: Do the cons outweigh the pros?. Surg Neurol Int. 2016. 7: S692-700
3. Gorek JE, Rolfe KW, Idler C. Minimally invasive surgery of the spine: Less is more. Semin Spine Surg. 2011. 23: 2-8
4. Guiroy A, Gagliardi M, Cabrera JP, Coombes N, Arruda A, Taboada N. Access to technology and education for the development of minimally invasive spine surgery techniques in Latin America. World Neurosurg. 2020. 142: e203-9
5. Pejrona M, Ristori G, Villafañe JH, Pregliasco FE, Berjano P. Does specialty matter? A survey on 176 Italian neurosurgeons and orthopedic spine surgeons confirms similar competency for common spinal conditions and supports multidisciplinary teams in comprehensive and complex spinal care. Spine J. 2018. 18: 1498-503
6. Weiss H, Garcia RM, Hopkins B, Shlobin N, Dahdaleh NS. A systematic review of complications following minimally invasive spine surgery including transforaminal lumbar interbody fusion. Curr Rev Musculoskelet Med. 2019. 12: 328-39