- Departments of Neurosurgery, Brigham and Women’s Hospital, Boston, Massachusetts, United States,
- Neurology, Brigham and Women’s Hospital, Boston, Massachusetts, United States.
Correspondence Address:
Melissa Ming Jie Chua, Department of Neurosurgery, Brigham and Women’s Hospital, Boston, Massachusetts, United States.
DOI:10.25259/SNI_4_2022
Copyright: © 2022 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Melissa Ming Jie Chua1, Michael T. Hayes2, Rees Cosgrove1. Parsonage-Turner syndrome following COVID-19 vaccination and review of the literature. 15-Apr-2022;13:152
How to cite this URL: Melissa Ming Jie Chua1, Michael T. Hayes2, Rees Cosgrove1. Parsonage-Turner syndrome following COVID-19 vaccination and review of the literature. 15-Apr-2022;13:152. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=11531
Abstract
Background: Parsonage-Turner syndrome (PTS) is a rare brachial plexopathy characterized by self-limiting shoulder girdle and upper arm pain followed by the upper extremity weakness and sensory changes. While the etiology is not well-understood, the most common cause of PTS is thought to be postviral. There are at least nine reports, to the best of our knowledge, of PTS associated with COVID-19 infection and nine reports associated with COVID-19 vaccination.
Case Description: Here, we present a case of PTS after COVID-19 vaccination in a 64-year-old male and a review of the current literature.
Conclusion: PTS can occur post-COVID-19 vaccination and should be on the differential diagnosis when patient continues to experience shoulder pain and develops weakness or sensory changes in the extremity.
Keywords: COVID-19, Idiopathic brachial neuritis, Parsonage-Turner syndrome, SARS-CoV-2, Vaccine
INTRODUCTION
Parsonage-Turner syndrome (PTS) is a rare upper extremity disorder with an incidence of 1.64/100,000 people. Furthermore, it is known as idiopathic acute brachial neuritis or neuralgic amyotrophy, the syndrome typically involves the upper and middle brachial plexus trunks.[
CASE DESCRIPTION
A 64-year-old previously healthy right-handed senior neurosurgeon with a medical history of hypertension and hyperlipidemia received his first dose of COVID-19 vaccine (mRNA-1273; ModernaTX, Inc.; Cambridge, Massachusetts) without any clinically significant side effects other than transient malaise and fatigue. After his scheduled second COVID-19 vaccine dose administered again into the left deltoid, he experienced mild shoulder soreness and transient rigors in the first 12–24 h. However, 2 weeks postvaccination, he developed intense, unremitting left shoulder girdle pain with associated muscle tenderness that was not relieved with conservative measures such as stretching, heat, or anti-inflammatories (ibuprofen 800 mg Q.I.D.). A week thereafter, he noticed decreased strength and dexterity in the left hand with difficulty opening bottle caps and manipulating small instruments. Within the next few days, he also noted sensory loss with paresthesia and hypoesthesia in the left fourth and fifth digits, as well as on the ulnar aspect of the forearm. His neurologic examination was notable for decreased strength in the left finger extensors (4+/5), particularly in the left fourth and fifth digits, and thenar eminence (4+/5). Reflexes were normal. Sensation was impaired to light touch distally in the left fourth and fifth digits and to a lesser extent in the third digit. Brachial plexitis was suspected and he was started on a steroid taper treatment with prednisone (80 mg/day for 3 days followed by a rapid taper of 20 mg decrease per day to off).
Three weeks after his initial symptom onset, he underwent an electromyogram (EMG) and nerve conduction study (NCS). The right median and right radial sensory nerve action potentials (SNAPs) (unaffected side) had low amplitude, but these were felt to be incidental and related to known prior trauma to that hand. The left median SNAPs were normal, including the lateral and medial antebrachial cutaneous sensory nerves. The left median abductor pollicis brevis compound motor action potentials (CMAPs) were normal as well. The left ulnar SNAP and left ulnar-abductor digiti minimi CMAPs had borderline low amplitude. The left median and ulnar F waves were unremarkable. Needle EMG demonstrated a reduced recruitment pattern in the left extensor indices and left flexor digitorum profundus to digit IV, with increased spontaneous activity in the left first dorsal interosseus. These findings were felt to reflect a mild, patchy, and acute-to-subacute lower trunk brachial plexopathy [
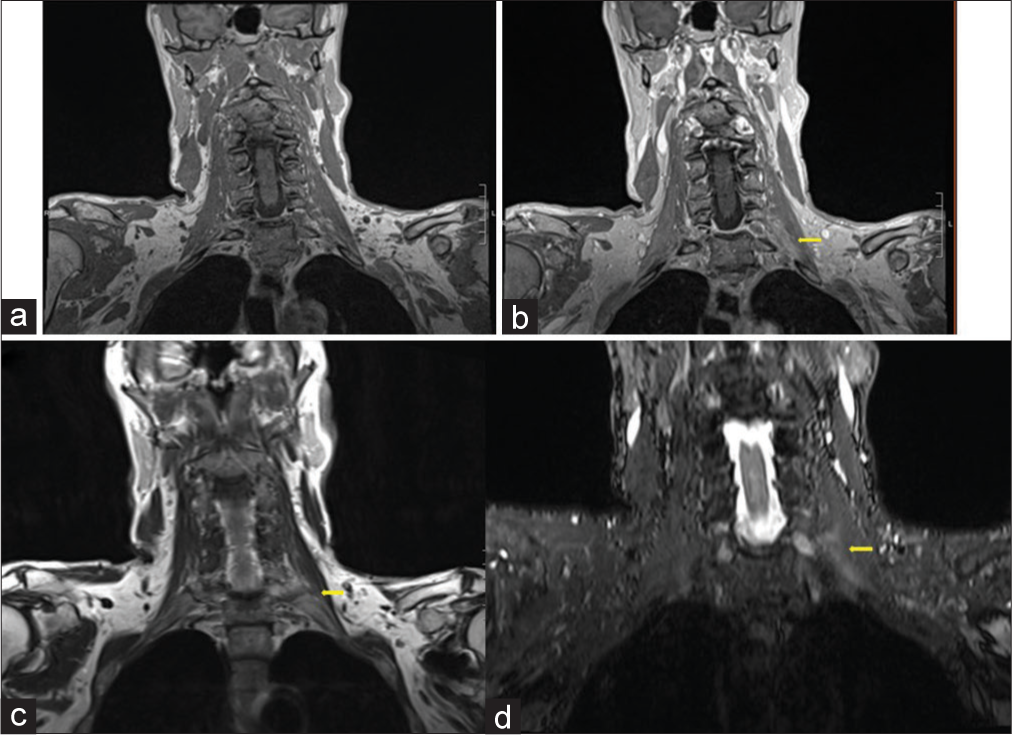
Figure 1:
(a-d) Magnetic resonance imaging of the brachial plexus. T1 precontrast (a), T1 postcontrast (b), T2 (c), and STIR (d) demonstrating increased STIR signal, T2-weighted signal, and mild T1 postcontrast enhancement of the medial left scalene muscles along the inferior brachial plexus consistent with inflammatory changes and intramuscular edema (yellow arrows).
Over the course of the next month, there was gradual improvement in finger sensation and strength with near complete resolution by 4 months.
DISCUSSION
PTS is a rare brachial plexopathy famously described by Parsonage and Turner in 1948, but was first reported by Dreschfeld in 1886.[
EMG, NCS, and MRI can help confirm the diagnosis of PTS.[
There is no consensus on the treatment of PTS, but generally involves conservative measures including analgesia, corticosteroid treatment, and physical therapy.[
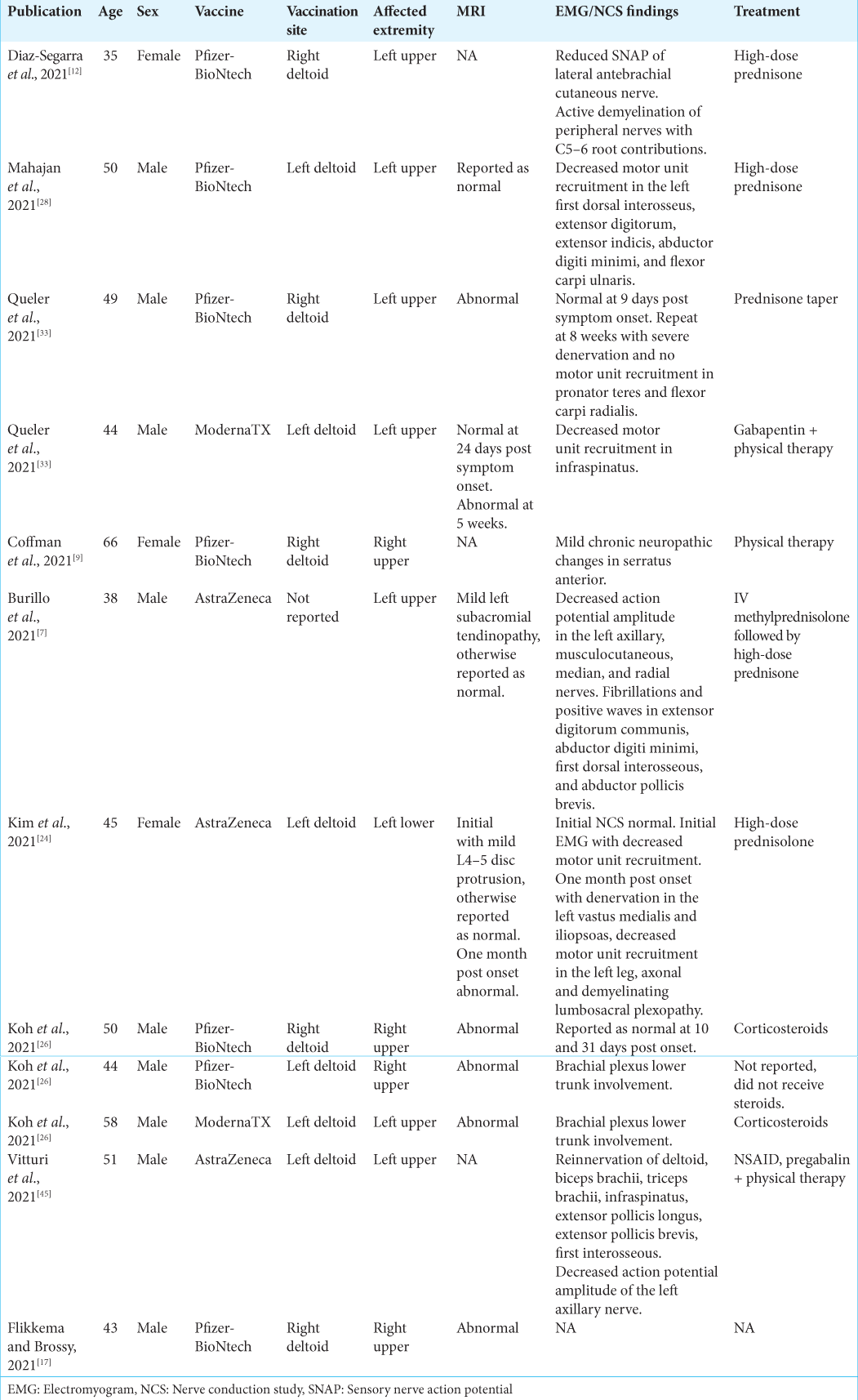
At the time of writing, there are only nine other published case reports of PTS post-COVID vaccination [
CONCLUSION
We present a case of post-COVID-19 vaccination PTS which improved following a corticosteroid taper and conservative measures. This is important as short-term shoulder soreness is a common post-COVID-19 vaccination, however, PTS should be in the differential if a patient continues to experience shoulder pain and develops weakness or sensory changes in the extremity.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Allan SG, Towla HM, Smith CC, Downie AW, Clark JC. Painful brachial plexopathy: An unusual presentation of polyarteritis nodosa. Postgrad Med J. 1982. 58: 311-3
2. Alvarado M, Lin-Miao Y, Carrillo-Arolas M. Parsonage-Turner syndrome post-infection by SARS-CoV-2: A case report. Neurologia (Engl Ed). 2021. 36: 568-71
3. Alvarez A, Amirianfar E, Mason MC, Huang L, Jose J, Tiu T. Extended neuralgic amyotrophy syndrome in a confirmed COVID-19 patient after intensive care unit and inpatient rehabilitation stay. Am J Phys Med Rehabil. 2021. 100: 733-6
4. Bloch SL, Jarrett MP, Swerdlow M, Grayzel AI. Brachial plexus neuropathy as the initial presentation of systemic lupus erythematosus. Neurology. 1979. 29: 1633-4
5. Bredella MA, Tirman PF, Fritz RC, Wischer TK, Stork A, Genant HK. Denervation syndromes of the shoulder girdle: MR imaging with electrophysiologic correlation. Skeletal Radiol. 1999. 28: 567-72
6. Brown R, O’Callaghan J, Peter N. Parsonage Turner syndrome caused by Staphylococcus aureus spondylodiscitis. BMJ Case Rep. 2020. 13: e233073
7. Burillo JA, Martínez CL, Arguedas CG, Pueyo FJ. Amyotrophic neuralgia secondary to Vaxzevri (AstraZeneca) COVID-19 vaccine. Neurologia (Engl Ed). 2021. 36: 571-2
8. Cacciavillani M, Salvalaggio A, Briani C. Pure sensory neuralgic amyotrophy in COVID-19 infection. Muscle Nerve. 2021. 63: E7-8
9. Coffman JR, Randolph AC, Somerson JS. Parsonage-Turner syndrome after SARS-CoV-2 BNT162b2 vaccine: A case report. JBJS Case Connect. 2021. 11: e21.00370
10. Coll C, Tessier M, Vandendries C, Seror P. Neuralgic amyotrophy and COVID-19 infection: 2 cases of spinal accessory nerve palsy. Joint Bone Spine. 2021. 88: 105196
11. Díaz C, Contreras JJ, Muñoz M, Osorio M, Quiroz M, Pizarro R. Parsonage-Turner syndrome association with SARS-CoV-2 infection. JSES Rev Rep Tech. 2021. 1: 252-6
12. Diaz-Segarra N, Edmond A, Gilbert C, Mckay O, Kloepping C, Yonclas P. Painless idiopathic neuralgic amyotrophy after COVID-19 vaccination: A case report. PM R. 2021. p. 1-3
13. Dreschfeld J. On some of the rarer forms of muscular atrophies. Brain. 1886. 9: 178-95
14. Feinberg JH, Nguyen ET, Boachie-Adjei K, Gribbin C, Lee SK, Daluiski A. The electrodiagnostic natural history of parsonage-turner syndrome. Muscle Nerve. 2017. 56: 737-43
15. Feinberg JH, Radecki J. Parsonage-turner syndrome. HSS J. 2010. 6: 199-205
16. Fibuch EE, Mertz J, Geller B. Postoperative onset of idiopathic brachial neuritis. Anesthesiology. 1996. 84: 455-8
17. Flikkema K, Brossy K. Parsonage-Turner syndrome after COVID-19 vaccination: A case report. JBJS Case Connect. 2021. 11: e21.00577
18. Fransz DP, Schönhuth CP, Postma TJ, van Royen BJ. Parsonage-Turner syndrome following post-exposure prophylaxis. BMC Musculoskelet Disord. 2014. 15: 265
19. Gonzalez-Alegre P, Recober A, Kelkar P. Idiopathic brachial neuritis. Iowa Orthop J. 2002. 22: 81-5
20. Helms CA, Martinez S, Speer KP. Acute brachial neuritis (Parsonage-Turner syndrome): MR imaging appearance--report of three cases. Radiology. 1998. 207: 255-9
21. Ismail II, Abdelnabi EA, Al-Hashel JY, Alroughani R, Ahmed SF. Neuralgic amyotrophy associated with COVID-19 infection: A case report and review of the literature. Neurol Sci. 2021. 42: 2161-5
22. Jacob JC, Andermann F, Robb JP. Heredofamilial neuritis with brachial predilection. Neurology. 1961. 11: 1025-33
23. James JL, Miles DW. Neuralgic amyotrophy: A clinical and electromyographic study. Br Med J. 1966. 2: 1042-3
24. Kim SI, Seok HY, Yi J, Cho JH. Leg paralysis after AstraZeneca COVID-19 vaccination diagnosed as neuralgic amyotrophy of the lumbosacral plexus: A case report. J Int Med Res. 2021. 49: 3000605211056783
25. Kim TU, Chang MC. Neuralgic amyotrophy: An underrecognized entity. J Int Med Res. 2021. 49: 3000605211006542
26. Koh JS, Goh Y, Tan BY, Hui AC, Hoe RH, Makmur A. Neuralgic amyotrophy following COVID-19 mRNA vaccination. QJM. 2021. 114: 503-5
27. Magee KR, Dejong RN. Paralytic brachial neuritis. Discussion of clinical features with review of 23 cases. JAMA. 1960. 174: 1258-62
28. Mahajan S, Zhang F, Mahajan A, Zimnowodzki S. Parsonage Turner syndrome after COVID-19 vaccination. Muscle Nerve. 2021. 14: 58-67
29. Martin WA, Kraft GH. Shoulder girdle neuritis: A clinical and electrophysiological evaluation. Mil Med. 1974. 139: 21-5
30. Mitry MA, Collins LK, Kazam JJ, Kaicker S, Kovanlikaya A. Parsonage-turner syndrome associated with SARS-CoV2 (COVID-19) infection. Clin Imaging. 2021. 72: 8-10
31. Parsonage MJ, Turner JW. Neuralgic amyotrophy; the shoulder-girdle syndrome. Lancet. 1948. 1: 973-8
32. Pellegrino JE, Rebbeck TR, Brown MJ, Bird TD, Chance PF. Mapping of hereditary neuralgic amyotrophy (familial brachial plexus neuropathy) to distal chromosome 17q. Neurology. 1996. 46: 1128-32
33. Queler SC, Towbin AJ, Milani C, Whang J, Sneag DB. Parsonage-Turner syndrome following COVID-19 vaccination: MR Neurography. Radiology. 2022. 302: 84-7
34. Scalf RE, Wenger DE, Frick MA, Mandrekar JN, Adkins MC. MRI findings of 26 patients with Parsonage-Turner syndrome. AJR Am J Roentgenol. 2007. 189: W39-44
35. Schmitt M, Daubail B, Bohm A. Parsonage-Turner syndrome secondary to Lyme disease. Joint Bone Spine. 2018. 85: 387-8
36. Shaikh MF, Baqai TJ, Tahir H. Acute brachial neuritis following influenza vaccination. BMJ Case Rep. 2012. 2012: bcr2012007673
37. Siepmann T, Kitzler HH, Lueck C, Platzek I, Reichmann H, Barlinn K. Neuralgic amyotrophy following infection with SARS-CoV-2. Muscle Nerve. 2020. 62: E68-70
38. Sneag DB, Rancy SK, Wolfe SW, Lee SC, Kalia V, Lee SK. Brachial plexitis or neuritis? MRI features of lesion distribution in Parsonage-Turner syndrome. Muscle Nerve. 2018. 58: 359-66
39. Stek CJ, van Eijk JJ, Jacobs BC, Enting RH, Sprenger HG, van Alfen N. Neuralgic amyotrophy associated with Bartonella henselae infection. J Neurol Neurosurg Psychiatry. 2011. 82: 707-8
40. Taylor RA. Heredofamilial mononeuritis multiplex with brachial predilection. Brain. 1960. 83: 113-37
41. Tsairis P, Dyck PJ, Mulder DW. Natural history of brachial plexus neuropathy. Report on 99 patients. Arch Neurol. 1972. 27: 109-17
42. van Alfen N, van Engelen BG, Hughes RA. Treatment for idiopathic and hereditary neuralgic amyotrophy (brachial neuritis). Cochrane Database Syst Rev. 2009. 2009: CD006976
43. van Alfen N. Clinical and pathophysiological concepts of neuralgic amyotrophy. Nat Rev Neurol. 2011. 7: 315-22
44. Viatgé T, Noel-Savina E, Prévot G, Faviez G, Plat G, De Boissezon X. Parsonage-Turner syndrome following severe SARS-CoV-2 infection. Rev Mal Respir. 2021. 38: 853-8
45. Vitturi BK, Grandis M, Beltramini S, Orsi A, Schenone A, Icardi G. Parsonage-Turner syndrome following coronavirus disease 2019 immunization with ChAdOx1-S vaccine: A case report and review of the literature. J Med Case Rep. 2021. 15: 589
46. Wendling D, Sevrin P, Bouchaud-Chabot A, Chabroux A, Toussirot E, Bardin T. Parsonage-Turner syndrome revealing Lyme borreliosis. Joint Bone Spine. 2009. 76: 202-4