- Department of Neurosurgery, St. Marianna University School of Medicine, Yokohama, Kanagawa, Japan
- Department of Neurosurgery, Kawasaki Municipal Tama Hospital, Yokohama, Kanagawa, Japan
- Department of Neurosurgery, Yokohama Rosai Hospital, Yokohama, Kanagawa, Japan
Correspondence Address:
Hidemichi Ito
Department of Neurosurgery, St. Marianna University School of Medicine, Yokohama, Kanagawa, Japan
DOI:10.4103/2152-7806.157795
Copyright: © 2015 Ito H. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.How to cite this article: Ito H, Onodera H, Sase T, Uchida M, Morishima H, Oshio K, Shuto T, Tanaka Y. Percutaneous transluminal angioplasty in a patient with internal carotid artery stenosis following gamma knife radiosurgery for recurrent pituitary adenoma. Surg Neurol Int 28-May-2015;6:
How to cite this URL: Ito H, Onodera H, Sase T, Uchida M, Morishima H, Oshio K, Shuto T, Tanaka Y. Percutaneous transluminal angioplasty in a patient with internal carotid artery stenosis following gamma knife radiosurgery for recurrent pituitary adenoma. Surg Neurol Int 28-May-2015;6:. Available from: http://surgicalneurologyint.com/surgicalint_articles/percutaneous-transluminal-angioplasty-patient-internal/
Abstract
Background:Intracranial vascular complications following radiosurgery are extremely rare.
Case Description:We report a case of stenosis in the internal carotid artery 5 years after gamma knife radiosurgery for a recurrent pituitary adenoma. Percutaneous transluminal angioplasty was performed successfully with anatomical and functional improvement.
Conclusion:These results suggested the importance of monitoring for arterial stenosis in the long-term follow-up. Moreover, this is the first case of endovascular treatment as an effective therapy for intracranial arterial stenosis due to radiotherapy.
Keywords: Angioplasty, endovascular treatment, gamma knife radiosurgery, internal carotid artery stenosis, pituitary adenoma
INTRODUCTION
Gamma knife radiosurgery (GKS) has been considered as an effective and safe management strategy for recurrent pituitary adenoma.[
CASE REPORT
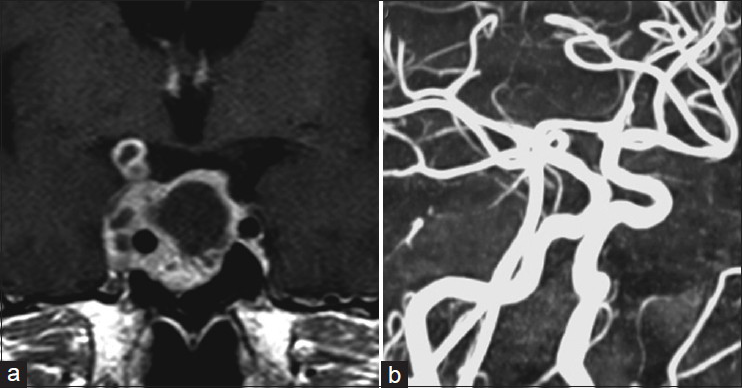
A 54-year-old male patient was admitted following a 3-month history of visual disturbance. He had no history of heart disease or metabolic disorder that could predispose to cerebrovascular complications. Neurological examination revealed a right homonymous hemianopia and decreased visual acuity. Magnetic resonance imaging (MRI) demonstrated a 5.0 × 5.3 cm pituitary tumor projecting toward the suprasellar region with encasement of both ICAs [
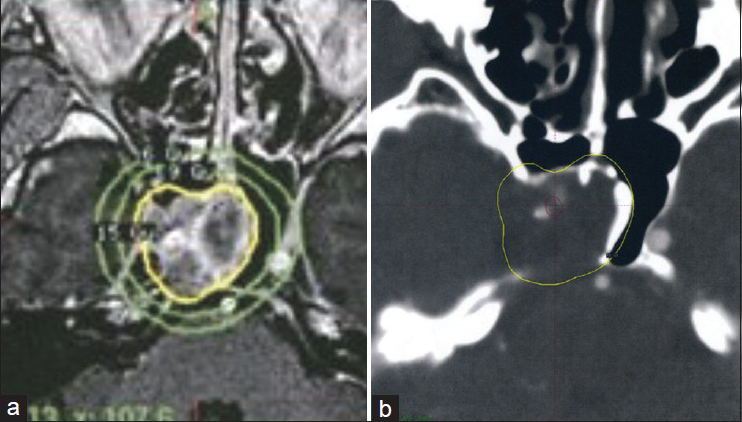
Figure 2
(a) Dosimetry of the GKS procedure. The marginal dose to the tumor margin was 15 Gy at the 50% isodose curve. (b) Isodose lines on the dosimetry planning showing the dose received by the intracavernous segment of the ICA, retrospectively (red line = 20-22 Gy isodose line, yellow line = 15 Gy isodose line)
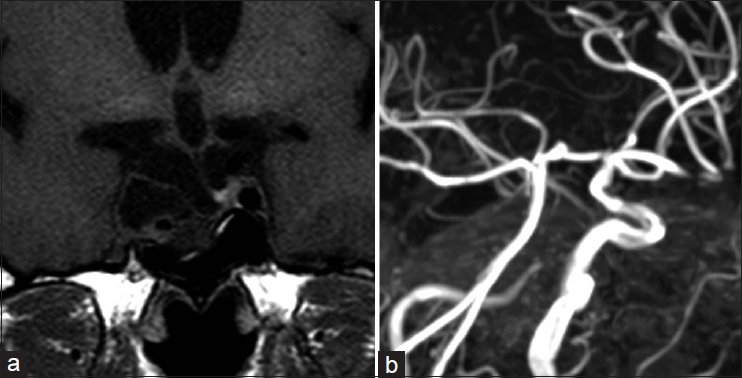
Five years after the GKS, the MRA demonstrated severe stenosis of the cavernous segment of the right ICA with a remarkable reduction of the residual pituitary adenoma [
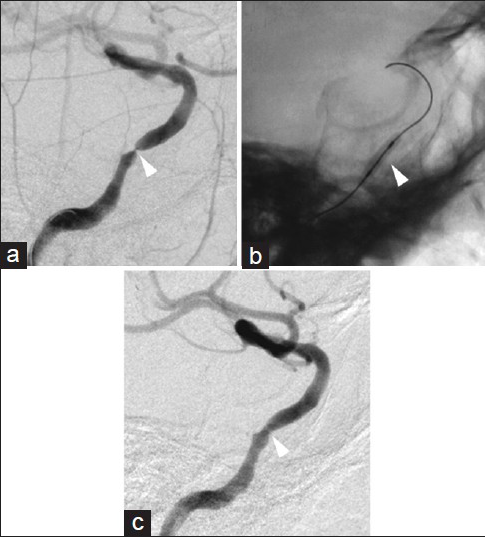
Figure 4
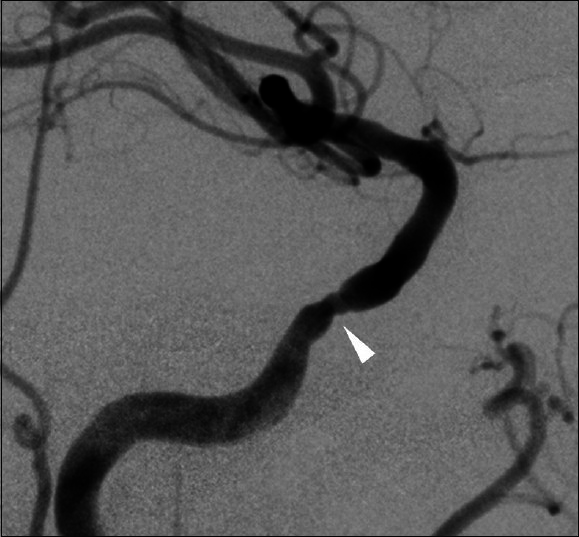
Pretreatment and posttreatment right ICA angiograms. The pretreatment angiogram indicating severe stenosis in the cavernous segment of the ICA (a, arrowhead). A microguidewire was advanced through the stenotic lesion and into the supraclinoid segment of the ICA. Inflation of a contrast-filled gateway PTA balloon (b, arrowhead) within the stenotic cavernous segment of the ICA dilated the vessel lumen, improving flow (c, arrowhead)
DISCUSSION
Several therapeutic options are recommended for the management of pituitary adenomas, for example, medical treatment, surgery, or radiotherapy.[
Accelerated atherosclerosis in the extracranial ICA is a well-recognized complication of irradiation for head and neck diseases.[
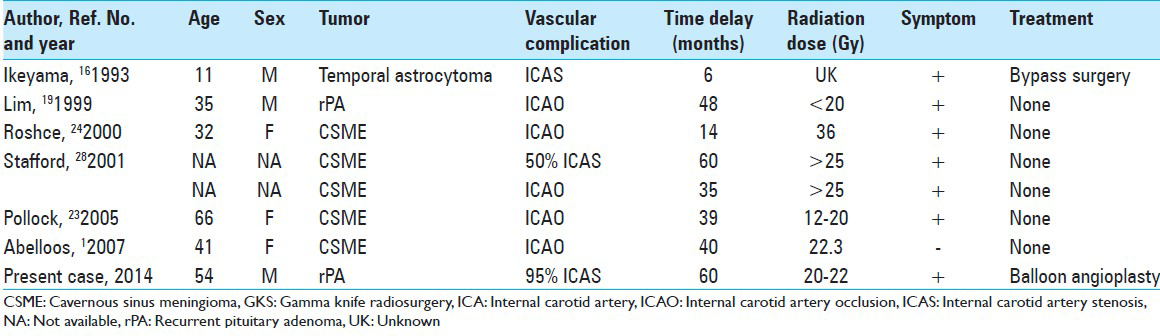
Intracranial vascular complications following radiosurgery seem to be extremely rare. The first case report of ICA stenosis after GKS was published by Ikeyama et al.[
Extracranial carotid artery angioplasty and stenting have clear advantages in treating patients with radiation-induced extracranial carotid artery stenosis.[
The resteonsis rate of a stenting for symptomatic intracranial stenosis has been reported to be from 7.5% to 30%,[
CONCLUSION
We reported a rare case of ICA stenosis 5 years after GKS for a recurrent pituitary adenoma. The irradiated vessels could be affected with stenosis in a delayed fashion; therefore, surveillance imaging should be performed even if the patient is asymptomaic up until that time. Endovascular angioplasty may most likely be the treatment of choice for steno-occlusive arteries following GKS.
ACKNOWLEDGMENTS
The authors thank Robert E. Brandt, Founder, CEO, and CME, of MedEd Japan, for editing the manuscript.
References
1. Abeloos L, Levivier M, Devriendt D, Massager N. Internal carotid occlusion following gamma knife radiosurgery for cavernous sinus meningioma. Stereotact Funct Neurosurg. 2007. 85: 303-6
2. Al-Ali F, Cree T, Hall S, Louis S, Major K, Smoker S. Predictors of unfavorable outcome in intracranial angioplasty and stenting in a single-center comparison: Results from the Borgess Medical Center-Intracranial Revascularization Registry. AJNR Am J Neuroradiol. 2011. 32: 1221-6
3. Andrews DW. Pituitary adenomas. Curr Opin Oncol. 1994. 6: 53-9
4. Barami K, Grow A, Brem S, Dagnew E, Sloan AE. Vascular complications after radiosurgery for menigiomas. Neurosurg Focus. 2007. 22: E9-
5. Bose A, Hartmann M, Henkes H, Liu HM, Teng MM, Szikora I. A novel, self-expanding, nitinol stent in medically refractory intracranial atherosclerotic stenosis: The Wingspan study. Stroke. 2007. 38: 1531-7
6. Bowen J, Paulsen CA. Stroke after pituitary irradiation. Stroke. 1992. 23: 908-11
7. Cheng SW, Ting AC, Lam LK, Wei WI. Carotid stenosis after radiotherapy for nasopharyngeal carcinoma. Arch Otolaryngol Head Neck Surg. 2000. 126: 517-21
8. Connors JJ, Wojak JC. Percutaneous transluminal angioplasty for intracranial atherosclerotic lesions: Evolution of technique and short-term results. J Neurosurg. 1999. 91: 415-23
9. Conomy JP, Kellermeyer RW. Delayed cerebrovascular consequences of therapeutic radiation. A clinicopathologic study of a stroke associated with radiation-related carotid arteriopathy. Cancer. 1975. 36: 1702-8
10. Elerding SC, Fernandez RN, Grotta JC, Lindberg RD, Causay LC, McMurtrey MJ. Carotid artery disease following external cervical irradiation. Ann Surg. 1981. 194: 609-15
11. Flickinger JC, Nelson PB, Martinez AJ, Deutsch M, Taylor F. Radiotherapy of nonfunctional adenomas of the pituitary gland. Results with long-term follow-up. Cancer. 1989. 63: 2409-14
12. Flickinger JC, Nelson PB, Taylor FH, Robinson A. Incidence of cerebral infarction after radiotherapy for pituitary adenoma. Cancer. 1989. 63: 2404-8
13. Groschel K, Schnaudigel S, Pilgram SM, Wasser K, Kastrup A. A systematic review on outcome after stenting for intracranial atherosclerosis. Stroke. 2009. p.
14. Hashimoto N, Handa H, Yamashita J, Yamagami T. Long-term follow-up of large or invasive pituitary adenomas. Surg Neurol. 1986. 25: 49-54
15. Hyodo A, Matsumaru Y, Anno I, Sato H, Kato N, Nakai Y. Percutaneous transluminal angioplasty for atherosclerotic stenosis of the intracranial cerebral arteries. Special reference to the device for reducing the complications drawn from the analysis of our complicated cases. Interv Neuroradiol. 1998. 4: S57-62
16. Ikeyama Y, Abiko S, Kurokawa Y, Okamura T, Watanabe K, Inoue S. Radiation-induced cerebrovasculopathy: A case report and review of the literature (in Japanese). No Shinkei Geka. 1993. 21: 751-7
17. Jahan R, Solberg TD, Lee D, Medin P, Tateshima S, Sayre J. Stereotactic radiosurgery of the rete mirabile in swine: A longitudinal study of histopathological changes. Neurosurgery. 2006. 58: 551-8
18. Kong DS, Lee JI, Lim do H, Kim KW, Shin HJ, Nam DH. The efficacy of fractionated radiotherapy and stereotactic radiosurgery for pituitary adenomas: Long-term results of 125 consecutive patients treated in a single institution. Cancer. 2007. 110: 854-60
19. Lim YJ, Leem W, Park JT, Kim TS, Rhee BA, Kim GK. Cerebral infarction with ICA occlusion after Gamma Knife radiosurgery for pituitary adenoma: A case report. Stereotact Funct Neurosurg. 1999. 72: S132-9
20. Marks LB. Conventional fractionated radiation therapy vs. radiosurgery for selected benign intracranial lesions (arteriovenous malformations, pituitary adenomas, and acoustic neuromas). J Neurooncol. 1993. 17: 223-30
21. Mazighi M, Yadav JS, Abou-Chebl A. Durability of endovascular therapy for symptomatic intracranial atherosclerosis. Stroke. 2008. 39: 1766-9
22. Murros KE, Toole JF. The effect of radiation on carotid arteries. A review article. Arch Neurol. 1989. 46: 449-55
23. Pollock BE, Stafford SL. Results of stereotactic radiosurgery for patients with imaging defined cavernous sinus meningiomas. Int J Radiat Oncol Biol Phys. 2005. 62: 1427-31
24. Roche PH, Regis J, Dufour H, Fournier HD, Delsanti C, Pellet W. Gamma knife radiosurgery in the management of cavernous sinus meningiomas. J Neurusurg. 2000. 93: S68-73
25. Sheehan JP, Starke RM, Mathieu D, Young B, Sneed PK, Chiang VL. Gamma Knife radiosurgery for the management of nonfunctioning pituitary adenomas: A multicenter study. J Neurosurg. 2013. 119: 446-56
26. Siddiq F, Vazquez G, Memon MZ, Suri MF, Taylor RA, Wojak JC. Comparison of primary angioplasty with stent placement for treating symptomatic intracranial atherosclerotic diseases: A multicenter study. Stroke. 2008. 39: 2505-10
27. . SSYLVIA Study Investigators. Stenting of symptomatic atherosclerotic lesions in the vertebral or intracranial arteries (SSYLVIA): Study results. Stroke. 2004. 35: 1388-92
28. Stafford SL, Pollock BE, Foote RL, Link MJ, Gorman DA, Schomberg PJ. Meningioma radiosurgery: Tumor control, outcomes, and complications among 190 consecutive patients. Neurosurgery. 2001. 49: 1029-37
29. Tallarita T, Oderich GS, Lanzino G, Cloft H, Kallmes D, Bower TC. Outcomes of carotid artery stenting versus historical surgical controls for radiation-induced carotid stenosis. J Vasc Surg. 2011. 53: 629-36
30. Tran LM, Blount L, Horton D, Sadeghi A, Parker RG. Radiation therapy of pituitary tumors: Results in 95 cases. Am J Clin Oncol. 1991. 14: 25-9