- Department of Neurosurgery, Federal Center of Neurosurgery, Novosibirsk, Russian Federation
- Department of Neurosurgery, University of Illinois at Chicago, Chicago, United States.
Correspondence Address:
Konstantin V. Slavin, Department of Neurosurgery, University of Illinois at Chicago, Chicago, United States.
DOI:10.25259/SNI_539_2023
Copyright: © 2023 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Jamil A. Rzaev1, Romana V. Bahrii2, Konstantin V. Slavin2. Report of the third international Siberian neurosurgical conference (Sibneuro 22): Scientific and professional exchange in the heart of Siberia. 28-Jul-2023;14:264
How to cite this URL: Jamil A. Rzaev1, Romana V. Bahrii2, Konstantin V. Slavin2. Report of the third international Siberian neurosurgical conference (Sibneuro 22): Scientific and professional exchange in the heart of Siberia. 28-Jul-2023;14:264. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=12466
Abstract
We present a summary of the recently held Third International Siberian Neurosurgical Conference (Sibneuro 22). Professional education, scientific exchange, and social interactions are essential in neurosurgical practice. In addition to the main program of the Congress, there were two practical pre-meeting courses: on aneurysm clipping and on intraoperative neuromonitoring. In addition, there was a 1-day seminar focusing on a role of laboratory diagnostics in neurosurgical practice. Within the framework of the Siberian Congress, there was a session devoted to inventions in neurosurgery, a rare subject of discussion at neurosurgical events. Our educational event is very important for the Siberian neurosurgery. Neurosurgeons of Siberia are a part of the world neurosurgical family. We not only try providing high-quality neurosurgical care to patients but also maintaining the academic level of education and scientific activity. The next - fourth - Siberian Neurosurgical Congress will take place in July 2024 in Irkutsk.
INTRODUCTION
Very recently, due to a rather long lockdown related to a worldwide viral pandemic, a huge number of events of various formats in all areas of human activity, involving travel, meetings, and live communication between professionals, were canceled. Our specialty has also been deeply affected: For almost 2 years, both local events, such as practical courses (workshops, hands-on courses), as well as large international congresses, conferences, have been canceled. It was literally yesterday. It seemed that the online format had won on a global scale and this change was irreversible. There was a lot of talk that live gatherings would no longer be necessary, that there was no sense in going to the other side of the world, to meet colleagues in congress halls to discuss certain professional issues, when you can easily connect through your laptop in your office or living room and give a report, express your opinion in the discussion, etc.
However, once the COVID restrictions began getting lifted, people started organizing professional meetings again, regardless of the associated hassle, time, and expense. That is just the way we humans are built. We need live communication, which cannot be replaced by talking on the Zoom. You could probably say that, fortunately, this is the case, not the other way around. The Siberian Association of Neurosurgeons was established in Novosibirsk in 2014. The main reasons for its creation were the following: Excessive centralization of the national Russian Neurosurgical Association, remoteness of Siberia from the European part of Russia, and a large number of neurosurgical departments in the Siberian (Asian) part of the Russian Federation.
The territory of the Siberian Federal District (SFD), whose center is the city of Novosibirsk, is almost 4.5 million square kilometers (more than one-quarter of the entire territory of Russia!), where 17.5 million people live. At present, it includes ten regions: Three republics (Altai, Tyva, Khakassia), two territories (Altai, Krasnoyarsk), and five regions (Irkutsk, Kemerovo, Novosibirsk, Omsk, Tomsk).
Today, in Siberia, there are over 100 scientific institutes and research centers, many of which are leading in Russia in a number of important areas of modern science. The SFD has about 2000 medical institutions employing more than 100,000 doctors.
The goal of the Siberian Association of Neurosurgeons “SibNeuro” is the realization and development of the professional potential of the medical community in the interest of solving urgent problems in the field of neurosurgery of theoretical, practical, and scientific orientation. To achieve the main goal, we set ourselves the following tasks:
Protection of professional interests of medical workers – members of the association, in the specialty “neurosurgery” and related specialties Assistance in the advanced training of the members of the association in these specialties Assistance in the development of projects and programs aimed at solving problems in the field of neurosurgery and related disciplines Establishment and development of international relations in neurosurgery Promoting scientific research Protection of the rights of the association members in the provision of medical care Organization and conduct of exhibitions, congresses, seminars, forums, and other events Improvement of health and safety conditions for the members of the association.
In the process of creating the association, we heard from our colleagues in the neurosurgical community both approval and support, as well as sharply negative comments about the very idea of creating such an organization. The arguments were something like this: “Why do we need a regional organization when we have a national one?,” “Why do we need to disperse forces and spend resources on work outside the national Association?,” and other things of that nature. However, this has not stopped us from realizing our vision: We believe that the appearance of various professional associations only benefits the development of our common cause and increases the professionalism of all participants in these or other communities, whether they are neurosurgeons, neurologists, cardiologists, or any other specialties. We are always open to constructive communication and productive effective cooperation with our colleagues from all cities and countries.
There are 344 neurosurgeons in 42 neurosurgical departments in Siberia. The peculiarities of the neurosurgical service in Siberia are the very long distances between cities and towns and the low population density in the vast territory. Out of 42 neurosurgical departments, eight are university (academic) departments and the remaining 34 belong to the municipal healthcare system.
From the 1 day of its work, the Siberian Association of Neurosurgeons has actively cooperated with colleagues from Moscow and St. Petersburg, as well as actively developed international partnership and cooperation. During the 8 years of work, a large number of master classes, rallies, and practical courses have been held.
In 2016, the first Siberian Neurosurgical Congress was held, and the second Siberian Neurosurgical Congress took place in 2018. Initial plans to keep the biannual format for this event were altered for obvious reasons, and so the 3rd Siberian Neurosurgical Congress took place in Novosibirsk on July 11–16, 2022. From the very beginning, we planned to hold this event in the middle of the summer, as good weather is guaranteed in Siberia in July.
THE CONGRESS
Similar to the first two meetings, where in addition to the main program of the Congress, there were practical pre- and post-congress courses, this congress also included two practical pre-meeting courses: on aneurysm clipping and intraoperative neuromonitoring (IONM). In addition, we had a 1-day seminar focusing on a role of laboratory diagnostics (coagulography and thromboelastography) in neurosurgical practice.
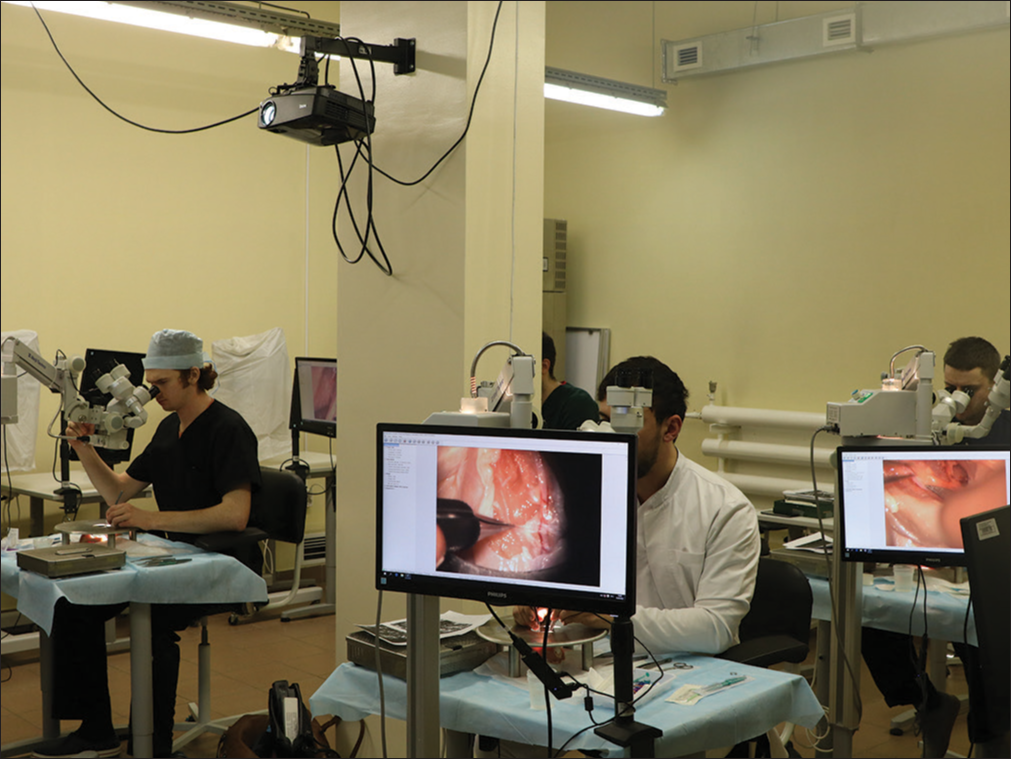
At the hands-on aneurysm clipping course, ten registered participants were divided into two groups of five. For 2 days, these participants practiced cadaveric dissection in the laboratory [
At the IONM course, 20 participants enjoyed lectures on all relevant neuromonitoring issues given by invited instructors. The lectures were short, 20–25 min each. And then, the trainees in each of three subgroups, accompanied by their instructor, worked together in the operating room. Joint practical work is very important in the sense of acquiring the necessary skills for placing and fixing electrodes, positioning the patient, discussing the type of anesthesia, and intraoperative dynamic control with the anesthesiologist. Three days of the course were divided as follows – 1 day of spinal surgery with monitoring of nerve roots, D-wave, motor, and sensory evoked potentials; the 2nd day was dedicated to cerebellopontine angle surgery; and the final 3rd day was devoted to awake surgery and cortical mapping.
The seminar on laboratory diagnostics in neurosurgical practice was devoted to the prevention of thrombosis and thromboembolic complications in the early postoperative period. More than 100 participants attended this seminar [
One of us (prof. K. Slavin, University of Illinois at Chicago, USA) was a guest speaker at the congress, giving lectures on microelectrode recording during deep brain stimulation (DBS) [
During the main 2 days of the congress, its scientific program consisted of three plenary and 18 breakout sessions. At this time, there were 350 physicians of different specialties, mainly neurosurgeons. The geography of the participants was not limited to Siberia and the Far East. Colleagues from all over Russia, practically from all Russian metropolitan areas, and international participants from the countries of Central Asia and Southern Caucasus came to Novosibirsk.
The plenary sessions of the Congress were devoted to the main problems of modern neurosurgery [
Dr. Vyacheslav Tkachev (Krasnodar) shared his 15-year experience in the surgical treatment of ruptured cerebral aneurysms at a regional vascular center. The unsolved problem remains the treatment of vasospasm after aneurysm rupture.
Prof. Ivan Savin (Moscow), neuroreanimatologist (neurointensivist), devoted his presentation to the diagnosis and treatment of elevated intracranial pressure (ICP) in the acute period of subarachnoid hemorrhage (SAH) in ruptured aneurysms. According to the literary data, intracranial hypertension (ICP >20 mmHg) is observed in more than half of the cases of SAH. The question of in whom and when to monitor ICP cannot be considered as solved. According to Prof. Savin, it is preferable to perform it through external ventricular drainage. One in three patients with SAH has delayed cerebral ischemia due to vasospasm. To combat it, “pharmacological angioplasty” – intra-arterial injection of vasoactive drugs – is practiced, but convincing evidence of its effectiveness has not yet been obtained. The report provoked a discussion. Academician V. Krylov urged to put an ICP measuring sensor in every patient in a coma.
The plenary report by Dr. Aleksandr Semenov (Irkutsk) gave an overview of head injury surgery at the present stage. New scales for assessing its severity are appearing (Mayo scale, combined trauma index, etc.). Neuroimaging methods (computed tomography and magnetic resonance imaging [MRI]) often reveal structural changes in the brain without any clinical signs. There is a “dominance of digitalization over clinical signs.” Annually 18 thousand patients (i.e., 18 cases/100 thousand adults) are operated on for head injury in Russia. The speaker called for the creation of a new paradigm of “decision-making hierarchy in the surgery of head injury,” but it is not clear who and how will implement it.
A report on the epidemiology of spine and spinal cord injury was given by Prof. Andrey Grin (Moscow). In one-third of the cases, such injury was sustained under alcoholic intoxication. The surgical part of the report focused on endoscopic technologies.
A very interesting report on gunshot wounds to the spine and pelvis was presented by Dr. Maksim Kravtsov (St. Petersburg). As awful as it is, modern warfare is characterized by numerous shrapnel wounds. Wearing body armor has reduced their number. The wound channel is examined with an endoscope (transcutaneous endovulnoscopy). Surgical access through the entrance hole, capturing, and extracting a foreign body with an endoscope is feasible.
Being a neurosurgical conference, it was of interdisciplinary character. Neurologists, anesthesiologists, orthopedists, radiation diagnosticians, etc., took part in it. Dr. Igor Basankin (Krasnodar) called for an integrated view of the spine and spinal cord. Neurosurgical priority is decompression of the spinal cord, and orthopedic priority is stabilization of the spine. The main areas of spinal surgery are as follows: first, implantation of stabilizing systems, second, decompressive surgery, and third, pain management. Contrary to conventional wisdom, the spine is not viewed as a column but as a chain of vertebrae. In conclusion, the speaker called for thinking about the functionality of the spine and for greater use of 3D modeling.
Prof. Artem Gushcha (Moscow) spoke about endoscopic techniques in spinal surgery, as well as the diagnostics of the degree of cervical myelopathy using transcranial magnetic stimulation and evoked potentials. The surgeon’s task is to perform optimal decompression of the spinal cord, and Prof. Guscha focused in detail on laminoplasty, nucleoplasty, and intervertebral disc prosthetics.
Dr. Sergey Riabykh (Moscow) devoted his presentation to the surgical treatment of spinal deformities in children. A very important question is how the costly staged treatment of severe neuroparalytic deformities of scoliosis is funded. There is a hybridization of treatment modalities and their “evidence-based titration.” “The detailing of nosology has necessitated a unification of terminology,” the speaker noted. He also noted the role of 3D modeling, the increasing complexity of treatment planning, the importance of criteria for prognosis and restoration of spinal balance and growth control, value for money, and technological continuity.
Oncologist Dr. Aslan Valiev (Moscow) spoke about the tactics of surgical treatment of primary tumors of the spine. He spoke about osteoid osteomas, osteoblastomas, gigantocellular tumors, etc. These issues are not often discussed at neurosurgical conferences. The more interesting and valuable for neurosurgeons was Dr. Valiev’s report and the discussion that followed the report.
Several plenary lectures were devoted to neuro-oncology. Prof. Andrey Grigoriev (Moscow) spoke about the evolution of pituitary adenoma surgery. After Oscar Hirsch and other pioneers of transnasal neurosurgery developed transsphenoidal access to the sella, the surgery of the sellar region has incredibly evolved. Today, the postoperative mortality rate for transcranial access is 4.2%, and 1% for the transnasal approach. Particular attention was paid to the need for joint management of such patients with endocrinologists.
Despite more than a century of history of vestibular schwannoma surgery, many unresolved questions remain both in the choice of treatment tactics and in the technique of cerebellopontine angle surgery. The report of Dr. Sergey Ilyalov (Moscow) was devoted to stereotactic radiosurgery of vestibular schwannomas. The first gamma knife treatment was performed back in 1968; now, the number of radiosurgical procedures has exceeded 1 million, including more than 100,000 patients with vestibular schwannomas. Dr. Ilyalov discussed the advantages and disadvantages of radiosurgical treatment of vestibular schwannomas.
Unfortunately, significant progress in the treatment of malignant brain tumors has not been achieved, as evidenced by the report of Prof. Leonid Kravets (Nizhnii Novhorod). The report was devoted to the reoperations of glioblastomas. According to the speaker, “reoperation creates new opportunities for local antitumor therapy.” For example, this may involve photodynamic therapy of the removed tumor bed. However, this claim has not yet been proven.
“Every surgeon sees surgery in his own way,” said Prof. Yuriy Kushel (Moscow). Therefore, he believes, it makes no sense to discuss the peculiarities of surgical technique with a surgical audience. It is better to consider the neurosurgical aspects of the new central nervous system (CNS) tumor classification. In 2016, the World Health Organization proposed a classification of these tumors that included genetic criteria. Five years later, this classification was revised. It describes about 100 CNS tumors in 584 pages. The diagnostic process now includes an addition of a mutation profile. However, due to the scarcity of reagents, modern diagnosis of tumors in Russia is not widely available. “An internationally integrated specialty cannot develop in a single room of a communal apartment,” the speaker summarized.
Over the past two decades, awake surgery has evolved from an exotic procedure performed in a small number of university clinics into a fairly routine surgical technique available in most neurosurgical departments. Prof. Andrey Zuev (Moscow) spoke about the multimodal approach in the surgery of tumors of the speech and motor areas. In his report, he noted the necessity of a thorough tractographic study and construction of a 3D model of the tumor. The problem is the variability of localization of the speech zones. Pre-, intra-, and postoperative neuropsychological and neurolinguistic studies are used. For this purpose, the Russian aphasiological test was developed jointly with the Laboratory of Neurolinguistics of the Higher School of Economics (Moscow). According to the reporter’s data, in 68% of cases, the tumor was completely removed in the speech areas, and the persistent neurological deficit (6 months after surgery) was observed in only 4%. All insular tumors in the dominant hemisphere were operated on with awake intraoperative testing.
The use of multimodal navigation techniques is also very important. A round table was organized at the Congress, where various types of modern navigation techniques in the surgery of benign and malignant gliomas were discussed for 3 h, from ultrasound to fluorescence.
The continuation of the plenary reports was sectional sessions. In the section on neuro-oncology, Dr. Anna Zolotova (Nizhnii Novhorod) spoke about the combination of multimodal MRI, neuronavigation, and awake craniotomy during the removal of tumors of the speech areas of the brain. On the material of 51 patients, it was shown that this approach allows to increase the volume of tumor resection and reduce the risk of persistent neurological deficit.
Dr. Anton Kalinovskii (Novosibirsk) shared his experience in minimally invasive surgery of isolated orbital tumors. For 10 years, 56 patients with primary orbital tumors have been operated on at the Novosibirsk Neurosurgery Center through trans-eyebrow access and lateral orbitotomy.
Prof. Armen Melikyan (Moscow) shared his experience with extensive disconnections in the surgery of pharmacoresistant epilepsy in 177 children in a plenary presentation. The advantage of such surgeries is a reduction in the volume of resection, less blood loss, and shorter operation time. In Prof. Melikyan’s series, different variants of disconnections prevailed – hemispherotomies (vertical, posterior quadrant, etc.) and different types of callosotomies.
At the sectional session on functional neurosurgery, Dr. Nikita Pediash (Moscow) spoke about disconnection (often hemispherotomy) in the surgical treatment of focal pharmacoresistant epilepsy in adults, and Dr. Fedor Efremov (Novosibirsk) shared his initial experience in the stimulation of anterior nuclei of the thalamus for seizure arrest in patients with epilepsy.
The effectiveness of the interventional therapy of facial pain under ultrasound guidance was evaluated in a report by Galina Moisak, MD, Ph.D. (Novosibirsk). For 10 months, 35 patients with facial pain (including trigeminal neuralgia and trigeminal neuropathy) were observed. The patients underwent blockades of the second and third branches of the trigeminal nerve (5–6 blocks/course) under ultrasound guidance. Facial pain was reduced in 78% of cases, and reversible adverse effects were observed in 9.2%.
The choice of target for DBS in Parkinson’s disease is debatable. Some neurosurgeons prefer to stimulate the STN and others – the globus pallidus internus (GPi). Dr. Aleksey Tomskii (Moscow) has implanted DBS system in GPi in 32 patients and in STN in 25 patients during 3 years. The results are comparable between these two targets.
Dr. Chingiz Shashkin (Kazakhstan) reported the results of microvascular decompression of the facial nerve in 34 patients. This disease is more common in the oriental population; there are many such patients in Kazakhstan, and Dr. Shashkin began to operate actively in his country on this pathology and analyze long-term (up to several years) results.
Dr. Vidzhai Dzhafarov (Moscow) shared with the audience the first experience of applying MRI-guided transcranial focused ultrasound to treat essential tremor, Parkinson’s disease tremor, and torsion dystonia. The duration of the procedure is about 40 min. The target (Ventral intermediate nucleus (VIM) nucleus of contralateral thalamus in case of tremor, in case of torsion dystonia – Ventro-oral nucleus (VO) nucleus) was lesioned by heating with focused ultrasound to 55 degrees. Ultrasound was applied for 10-45 s under the control of MRI thermography. Since November 2021, 21 patients were treated. This method is so far comparable to radiofrequency thalamotomy in effectiveness, but the long-term results have yet to be analyzed.
A plenary report by Dr. Pavel Shniakin (Krasnoyarsk) was devoted to complications in neurosurgery. The problem is in the definition of the term “complication.” How does a complication differ from a consequence of surgery or a medical error? The complication is suggested to be an unexpected negative event, related to the surgery, and the consequence is any predictable unfavorable outcome. A tactic-oriented classification of complications is proposed. In practice, the boundary between complications and medical errors is often blurred.
Within the framework of the Siberian Congress, there was a sectional session devoted to inventions in neurosurgery, a rare subject of discussion at neurosurgical events. The session “Inventions in Neurosurgery” was moderated by the young resident physician Oleg Titov (Moscow). As a medical student, Dr. Titov became interested in clinical neuroscience already in his 1 year of studies. He has been actively involved in inventions since his 3rd (out of 6) school year. He has ten patents, received two grants, and published four articles. At the Congress, he gave a lecture on the invention process. The reasons can be external (for example, a patent is equated by the High Attestation Commission to a peer-reviewed article to fill a complement needed to proceed with PhD thesis defense) and internal (prevention of burnout, feeling of one’s own worth). Invention is a multi-stage process: generation of an idea, patenting, production, and financing. It is recommended to write down or sketch the idea you came up with. Then, it should be checked for novelty in databases (Google patents and the national patent database). There is an algorithm for working through an idea. Then, it can get patented. There are three types of patents in Russia: invention, utility model, and design. The criteria for an invention are as follows: Novelty, industrial applicability, and inventive step. The duration of a patent in these cases is different (20, 10, and 5 years, respectively). There is a program of the Foundation for Assistance to Innovations called UMNIK (“a smarty”). During the Congress, the 1st Russian Exhibition of Neurosurgical Inventions took place, presenting 27 inventions (21 devices and 6 methods) and 4 utility models [
SUMMARY
Our educational event is very important for the Siberian neurosurgery. Neurosurgeons of Siberia are a part of the world neurosurgical family. We not only try providing high-quality neurosurgical care to patients but also maintaining the academic level of education and scientific activity.
The next – already the fourth – Siberian Neurosurgical Congress will take place in July 2024 in Irkutsk.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.