- Department of Neurosurgery, Ibn Sina University Hospital, Rabat,
- Faculty of Medicine and Pharmacy, University of Mohammed V, Rabat, Morocco.
Correspondence Address:
Saad Moussa Elmi, Department of Neurosurgery, IBN SINA University Hospital, Rabat, Mohammed V University of Rabat, Morocco.
DOI:10.25259/SNI_92_2023
Copyright: © 2023 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, transform, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Saad Moussa Elmi1,2, Alngar Djimrabeye1,2, José Dimbi Makoso1,2, Rayhane Hamdaoui1,2. Spinal cord compression caused by a brown tumor secondary to primary hyperparathyroidism. 24-Mar-2023;14:108
How to cite this URL: Saad Moussa Elmi1,2, Alngar Djimrabeye1,2, José Dimbi Makoso1,2, Rayhane Hamdaoui1,2. Spinal cord compression caused by a brown tumor secondary to primary hyperparathyroidism. 24-Mar-2023;14:108. Available from: https://surgicalneurologyint.com/?post_type=surgicalint_articles&p=12205
Abstract
Background: Brown tumors (BTs) are rare non-neoplastic lesions that arise secondary to hyperparathyroidism largely involving mandible, ribs, pelvis, and large bones. Spinal involvement is extremely rare and may result in cord compression.
Case Description: A 72-year-old female with the primary hyperparathyroidism developed a thoracic spine BT causing T3–T5 spinal cord compression warranting operative decompression.
Conclusion: BTs should be included in the differential diagnosis in lytic-expansive lesions involving the spine. For those who develop neurological deficits, surgical decompression may be warranted followed by parathyroidectomy.
Keywords: Brown tumor, Primary hyperparathyroidism, Spinal cord compression
INTRODUCTION
Brown tumors (BTs) are rare benign and non-neoplastic lesions that arise secondary to hyperparathyroidism (i.e., primary, or rarely secondary).[
CASE REPORT
Clinical presentation
A 72-year-old female presented with the upper back pain of 6 months’ with one month of acute worsening associated with the onset of paraparesis (i.e., 3/5 deficit). Laboratory studies showed; a serum calcium level of 144 mg/L (normal: 90–105 mg/L) and a slightly high parathyroid hormone level (pg/mL; normal is 10–53 pg/mL). A thyroid ultrasound proved negative, but the parathyroid scintigraphy with Tc-99 m showed focal activity in the inferior right thyroid lobe consistent with a parathyroid adenoma.
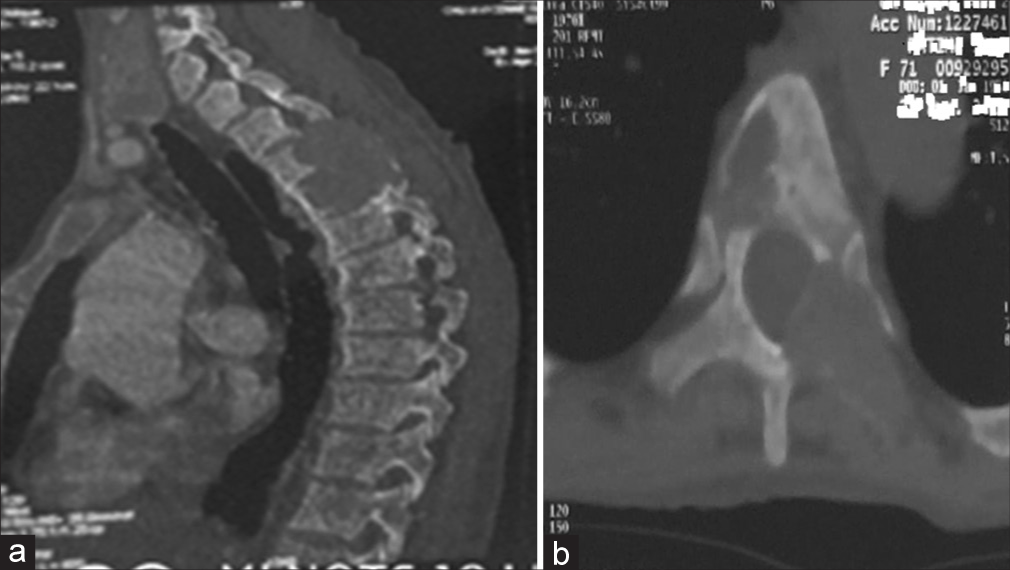
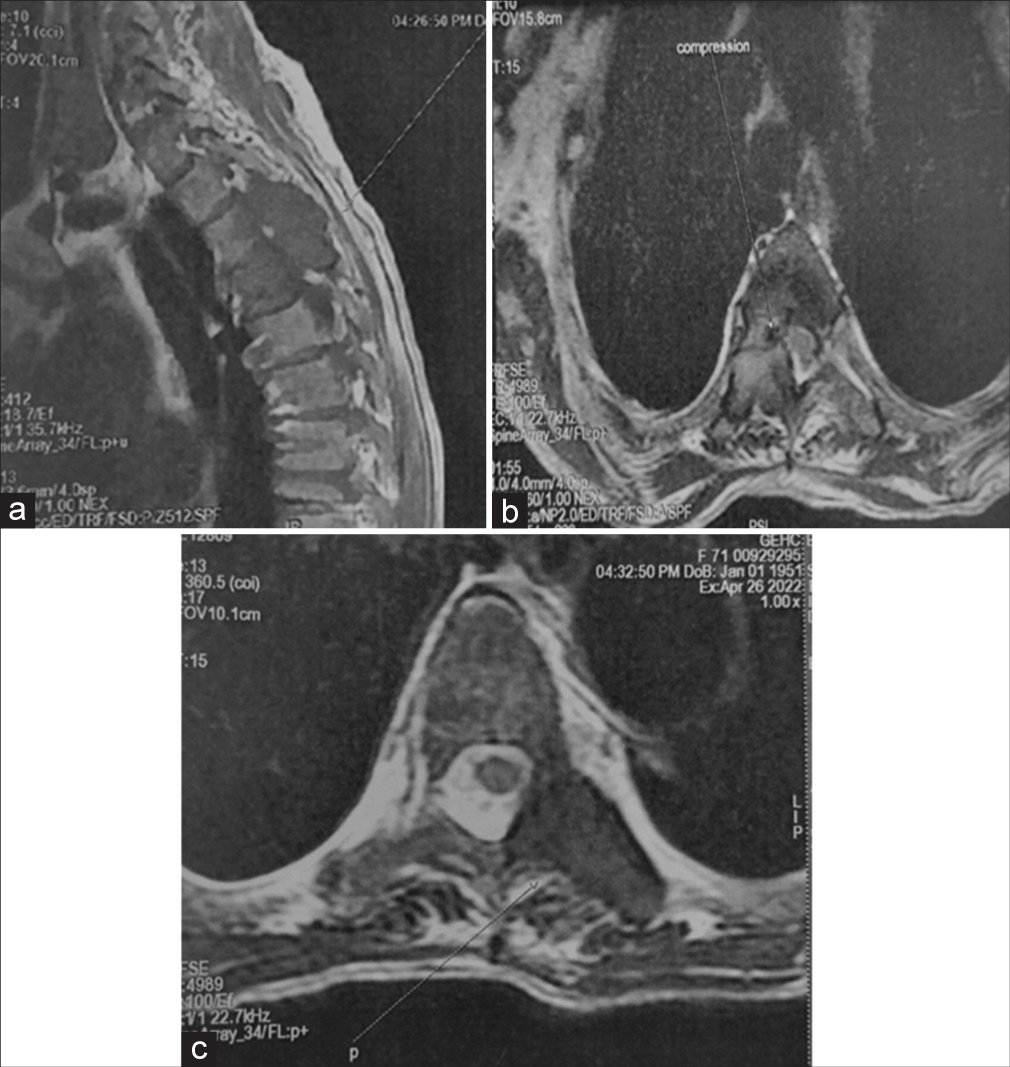
Spine computed tomography (CT) and magnetic resonance (MR) studies showing cord compression due to BT at T3–T5 levels
Both the CT and MR studies showed BTs compressing the cord from T3 to T5 secondary to hyperparathyroidism. The thoracic CT demonstrated multiple osteolytic lesions of the vertebral bodies and posterior elements from Th3 to Th5 level [
Surgery, pathology, and outcome
Following an emergent Th3-5 laminectomy, the extradural mass was totally excised, and the cord was adequately decompressed. The histopathological examination confirmed a BT secondary to hyperparathyroidism. Postoperatively, the patient’s symptoms resolved within 3 weeks. Subsequently, she was referred for a parathyroidectomy.
DISCUSSION
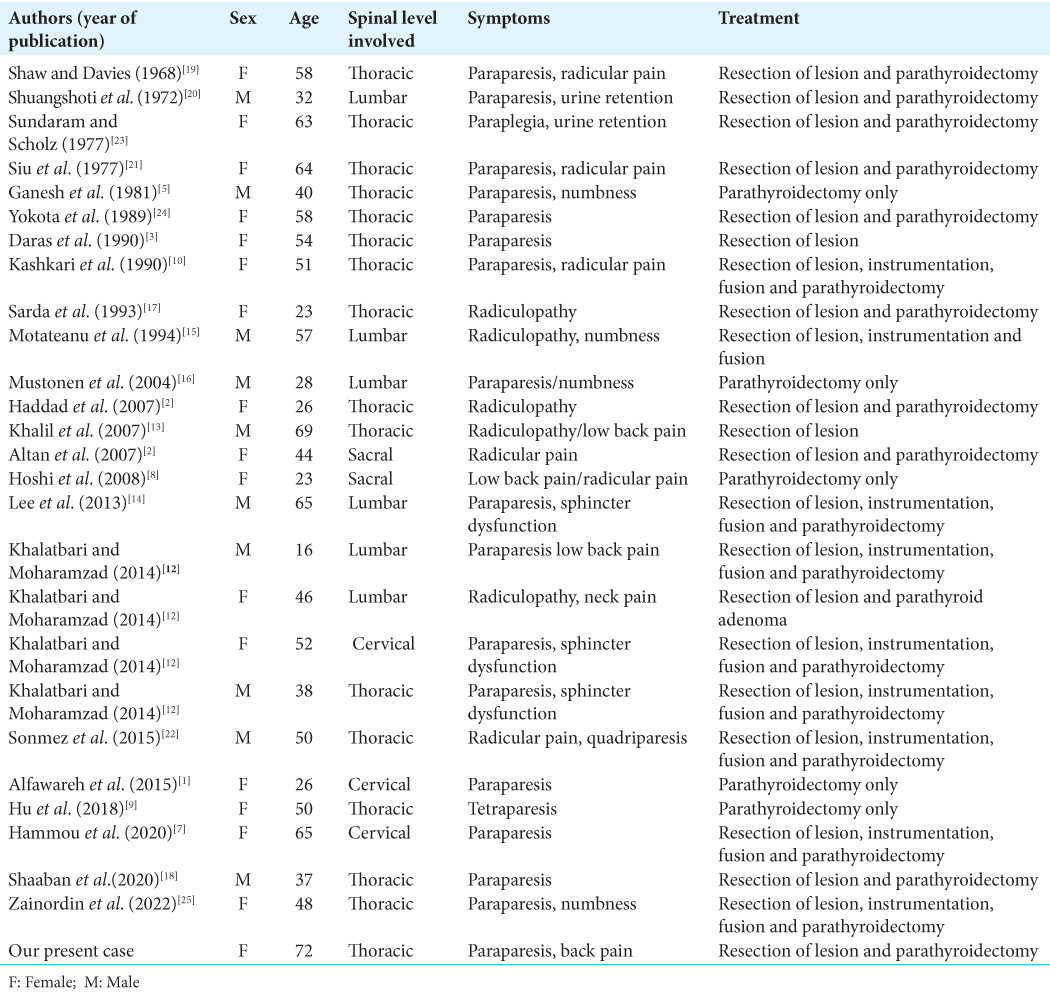
We identified 25 similar cases of BTs attributed primary hyperparathyroidism impacting the spine (since 1968 to present) [
The gold standard for the treatment for BTs due to primary hyperparathyroidism remains gross total removal of the spine lesion (i.e., biopsy, decompression with/without fusion for those with neurological deficits) followed by parathyroidectomy.[
CONCLUSION
BTs should be included in the differential diagnosis of spinal lytic-expansive lesions with or without neurological deficits. The standard treatment is gross spinal total tumor excision followed by parathyroidectomy.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Publication of this article was made possible by the James I. and Carolyn R. Ausman Educational Foundation.
Conflicts of interest
There are no conflicts of interest.
Disclaimer
The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Journal or its management. The information contained in this article should not be considered to be medical advice; patients should consult their own physicians for advice as to their specific medical needs.
References
1. Alfawareh MD, Halawani MM, Attia WI, Almusrea KN. Brown tumor of the cervical spines: A case report with literature review. Asian Spine J. 2015. 9: 110-20
2. Altan L, Kurtŏglu Z, Yalçınkaya U, Aydınlı U, Ertürk E. Brown tumor of the sacral spine in a patient with low-back pain. Rheumatol Int. 2007. 28: 77-81
3. Daras M, Georgakopoulos T, Avdelidis D, Gravani A, Tuchman AJ. Spinal cord compression in primary hyperparathyroidism: Report of a case and review of the literature. Spine Phila Pa. 1990. 15: 238-40
4. Fargen KM, Lin CS, Jeung JA, Yachnis AT, Jacob RP, Velat GJ. Vertebral brown tumors causing neurologic compromise. World Neurosurg. 2013. 79: 208.e1-6
5. Ganesh A, Kuriant S, John L. Complete recovery of spinal cord compression following parathyroidectomy. Postgrad Med. 1981. 57: 652-3
6. Haddad FH, Malkawi OM, Sharbaji AA, Jbara IF, Rihani HR. Primary hyperparathyroidism. A rare cause of spinal cord compression. Saudi Med J. 2007. 28: 783-6
7. Hammou O, Azzouzi H, Ichchou L. Spinal cord compression secondary to brown tumor as first manifestation of primary hyperparathyroidism. World Neurosurg. 2020. 137: 384-8
8. Hoshi M, Takami M, Kajikawa M, Teramura K, Okamoto T, Yanagida I. A case of multiple skeletal lesions of brown tumors mimicking carcinoma metastases. Arch Orthop Trauma Surg. 2008. 128: 149-54
9. Hu J, He S, Yang J, Ye C, Yang X, Xiao J. Management of brown tumor of spine with primary hyperparathyroidism: A case report and literature review. Medicine (Baltimore). 2019. 98: e15007
10. Kashkari S, Kelly TR, Bethem D, Pepe RG. Osteitis fibrosa cystica (brown tumor) of the spine with cord compression: Report of a case with needle aspiration biopsy findings. Diagn Cytopathol. 1990. 6: 349-53
11. Kaya RA, Çavuşoğlu H, Tanik C, Kahyaoglu O, Dilbaz S, Tuncer C. Spinal cord compression caused by a brown tumor at the cervicothoracic junction. Spine J. 2007. 7: 728-32
12. Khalatbari MR, Moharamzad Y. Brown tumor of the spine in patients with primary hyperparathyroidism. Spine (Phila Pa 1976). 2014. 39: E1073-9
13. Khalil PN, Heining SM, Huss R, Ihrler S, Siebeck M, Hallfeldt K. Natural history and surgical treatment of brown tumor lesions at various sites in refractory primary hyperparathyroidism. Eur J Med Res. 2007. 12: 222-30
14. Lee JH, Chung SM, Kim HS. Osteitis fibrosa cystica mistaken for malignant disease. Clin Exp Otorhinolaryngol. 2013. 6: 110-3
15. Motateanu M, D´eruaz JP, Fankhauser H. Spinal tumour due to primary hyperparathyroidism causing sciatica: Case report. Neuroradiology. 1994. 36: 134-6
16. Mustonen AO, Kiuru MJ, Stahls A, Bohling T, Kivioja A, Koskinen SK. Radicular lower extremity pain as the first symptom of primary hyperparathyroidism. Skeletal Radiol. 2004. 33: 467-72
17. Sarda AK, Arunabh , Vijayaraghavan M, Kapur M. Paraplegia due to osteitis fibrosa secondary to primary hyperparathyroidism: Report of a case. Surg Today. 1993. 23: 1003-5
18. Shaaban AT, Ibrahem M, Saleh A, Haider A, Alyafai A. Brown tumor due to primary hyperparathyroidism resulting in acute paraparesis: Case report and literature review. Surg Neurol Int. 2020. 11: 355
19. Shaw MT, Davies M. Primary hyperparathyroidism presenting as spinal cord compression. Br Med J. 1968. 4: 230-31
20. Shuangshoti S, Hongsaprabhas C, Chandraprasert S, Rajatapiti B. Parathyroid adenoma, brown tumor and cauda equina compression. J Med Assoc Thai. 1972. 55: 251-8
21. Siu K, Sundaram M, Schultz C, Kirwan L. Primary hyperparathyroidism presenting as spinal cord compression: Report of a case. Aust N Z J Surg. 1977. 47: 668-72
22. Sonmez E, Tezcaner T, Coven I, Terzi A. Brown tumor of the thoracic spine: First manifestation of primary hyperparathyroidism. J Korean Neurosurg Soc. 2015. 58: 389-92
23. Sundaram M, Scholz C. Primary hyperparathyroidism presenting with acute paraplegia. AJR Am J Roentgenol. 1977. 128: 674-6
24. Yokota N, Kuribayashi T, Nagamine M, Tanaka M, Matsukura S, Wakisaka S. Paraplegia caused by brown tumor in primary hyperparathyroidism: Case report. J Neurosurg. 1989. 71: 446-8
25. Zainordin NA, Azraai AM, Shah FZ, Ghani RA. Primary hyperparathyroidism presenting with sudden onset paraplegia. SAGE Open Med Case Rep. 2022. 10: 2050313-X221089759