- Department of Ortho-Spine Surgery, New Delhi, India.
- Department of Pathology, Sir Ganga Ram Hospital, New Delhi, India.
Correspondence Address:
Nitin Adsul
Department of Pathology, Sir Ganga Ram Hospital, New Delhi, India.
DOI:10.25259/SNI-49-2019
Copyright: © 2019 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Nitin Adsul, K. L. Kalra, Nikhil Jain, Mukesh Haritwal, R. S. Chahal, Shankar Acharya, Sunila Jain. Thoracic cryptococcal osteomyelitis mimicking tuberculosis: A case report. 10-May-2019;10:81
How to cite this URL: Nitin Adsul, K. L. Kalra, Nikhil Jain, Mukesh Haritwal, R. S. Chahal, Shankar Acharya, Sunila Jain. Thoracic cryptococcal osteomyelitis mimicking tuberculosis: A case report. 10-May-2019;10:81. Available from: http://surgicalneurologyint.com/surgicalint-articles/9336/
Abstract
Background: Isolated cryptococcal osteomyelitis of the spine is extremely uncommon; there have been only seven cases identified in literature. The majority were originally misdiagnosed as tuberculosis. Here, we present a patient with cryptococcal osteomyelitis of the thoracic spine with associated fungal retinal deposits.
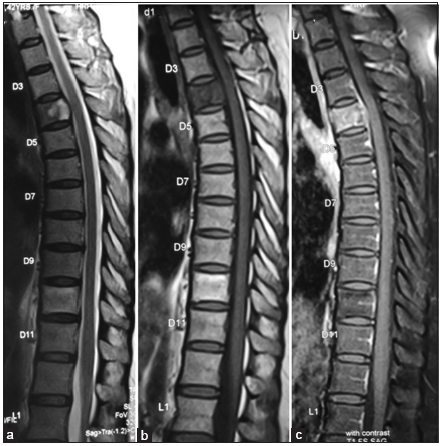
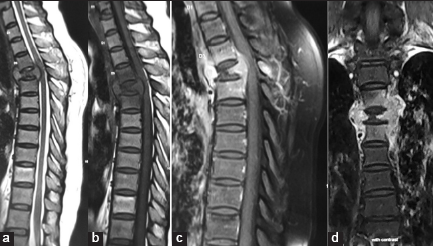
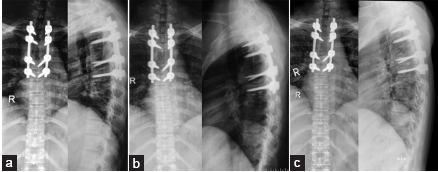
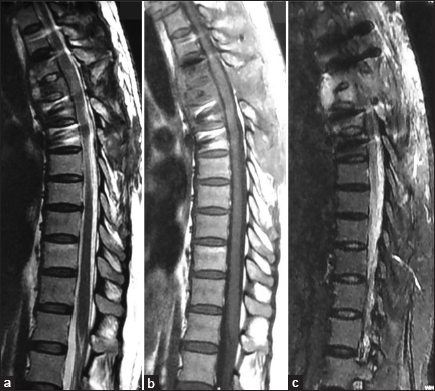
Case Description: A 45-year-old, type II diabetic female presented with a 5-month history of severe back pain. Her magnetic resonance imaging (MRI) revealed osteomyelitis involving the T4 vertebral body with epidural and prevertebral extension; notably, the intervertebral disc spaces were not involved. Although the fine-needle aspiration cytologic examination was inconclusive, the patient was empirically placed on antitubercular drug therapy. One month later, she became fully paraplegic. The MRI now demonstrated osteolytic lesions involving the T4 vertebral body with cord compression. She underwent biopsy of the T4 vertebral body and a transfacet T4 decompression with T2-T6 pedicle screw fixation. Culture and histopathological examinations both documented a cryptococcal infection, and she was placed on appropriate antifungal therapy. Notably, 3 weeks after surgery, she developed a sudden loss of vision loss due to retinal fungal endophthalmitis. She recovered vision in one eye after the administration of intravitreal voriconazole but lost vision in the other eye despite a vitrectomy. Over the next 8 months, she gradually recovered with motor function of 4/5 in both lower extremities without evidence of recurrent disease.
Conclusion: Cryptococcal infection should be among the differential diagnostic considerations for patients with vertebral osteomyelitis. Notably, diagnostic delay can lead to devastating neurological deficits and involvement of other organ systems.
Keywords: Cryptococcosis, Differential diagnosis, Endophthalmitis, Osteomyelitis, Spine infection, Thoracic vertebra
INTRODUCTION
Cryptococcus neoformans is an encapsulated fungal organism, which is abundant in topsoil, decayed food, and bird droppings (e.g., particularly pigeon fecal matter). Inhalation of C. neoformans primarily results in lung infections although, through hematogenous spread, it may also involve the meninges and other organ systems. Although meningitis is most frequently seen in immunocompromised hosts, 10–40% of cryptococcosis infections occur in those without a major primary illness or immunodeficiency. Isolated cryptococcal osteomyelitis of the spine is extremely uncommon, with only seven cases reported in literature.[
CASE REPORT
Clinical presentation and surgery
A 45-year-old female with type II diabetes presented with a 5-month history of severe back pain. She was a homemaker who kept pigeons as pets. Her laboratory investigations revealed an erythrocyte sedimentation rate (ESR) of 38 mm/1st h and a C-reactive protein (CRP) of 18 mg/l. The magnetic resonance imaging (MRI) demonstrated T4 osteomyelitis with relatively well-preserved intervertebral disc spaces [
Cultures, histology, and further treatment
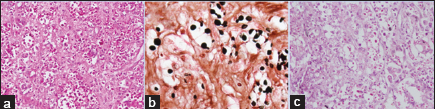
The culture and histopathological examinations revealed a cryptococcal fungal infection that was sensitive to amphotericin B; this was administered intravenously (150 mg/day) for the next 3 months [
Follow-up
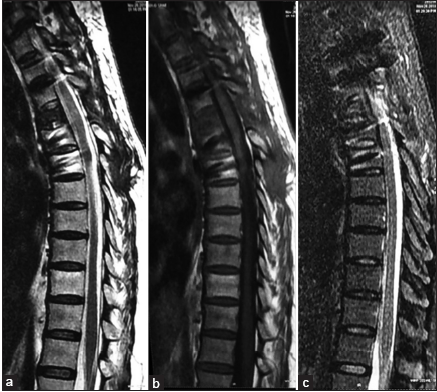
Three months following the spinal surgery, she regained 4/5 function in both lower extremities. Although the MRI still showed some prevertebral collection compared with the preoperative MRI, there was resolution of the T4 cord compression [
DISCUSSION
Vertebral involvement with cryptococcosis is very rare, typically involves the immunocompetent population, and is usually associated with both a raised ESR and CRP (sensitivity 80% and 100%, respectively) levels.[
Surgery and histopathological confirmation of spinal cryptococcosis
It is important to differentiate cryptococcosis from malignant spine tumors and TB.[
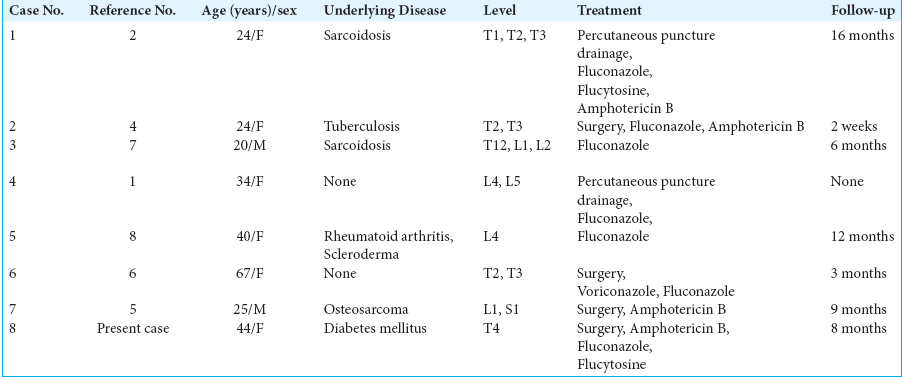
Literature review – eight cases of spinal cryptococcosis
In 1955, Eisen et al.[
This case summary
Our patient was initially misdiagnosed and treated for tuberculosis. The T4 biopsy, however, obtained during decompression/fusion confirmed the diagnosis of a cryptococcal fungal infection. She was then placed on amphotericin B and later required the addition of fluconazole/flucytosine.
CONCLUSION
Cryptococcal spinal infections must be considered among the differential diagnoses for patients presenting with vertebral osteomyelitis. Biopsy/histological/surgical confirmation of the diagnosis is critical to avoid undue delay, risking further hematogenous spread of infection to other organ systems.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patients have given their consent for their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgment
We would like to thank Dr. Chand Sahai, Senior Anesthesiologist, as part of our surgical team and for correcting grammatical mistakes in manuscript.
References
1. Al-Tawfiq JA, Ghandour J. Cryptococcus neoformans abscess and osteomyelitis in an immunocompetent patient with tuberculous lymphadenitis. Infection. 2007. 35: 377-82
2. Cook PP. Successful treatment of cryptococcal osteomyelitis and paraspinous abscess with fluconazole and flucytosine. South Med J. 2001. 94: 936-8
3. Eisen D, Shapiro I, Fischer JB. A case of cryptococcosis with involvement of lungs and spine. Can Med Assoc J. 1955. 72: 33-5
4. Gupta SK, Chhabra R, Sharma BS, Das A, Khosla VK. Vertebral cryptococcosis simulating tuberculosis. Br J Neurosurg. 2003. 17: 556-9
5. Lai Q, Liu Y, Yu X, Lv X, Wang Q, Zhou Y. Diagnosis and treatment of nonadjacent cryptococcal infections at the L1 and S1 vertebrae. Orthopade. 2017. 46: 85-9
6. Wang C, Jia N, Zhang L, Liu K, Liu H, Yu H. Imaging findings of cryptococcal infection of the thoracic spine. Int J Infect Dis. 2014. 29: 162-5
7. Wildstein MS, Martin SM, Glaser JA. Cryptococcal osteomyelitis in a 20-year-old male with sarcoidosis. Spine J. 2005. 5: 467-70
8. Zhou HX, Ning GZ, Feng SQ, Jia HW, Liu Y, Feng HY. Cryptococcosis of lumbar vertebra in a patient with rheumatoid arthritis and scleroderma: Case report and literature review. BMC Infect Dis. 2013. 13: 128-