- Department of Neurosurgery, Hospital Quironsalud Zaragoza, Zaragoza, Aragon, Spain.
DOI:10.25259/SNI_880_2020
Copyright: © 2020 Surgical Neurology International This is an open-access article distributed under the terms of the Creative Commons Attribution-Non Commercial-Share Alike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.How to cite this article: Pablo Barbero-Aznarez, Carlos Bucheli-Peñafiel, Eduardo Olmos-Francisco, Asís Lorente-Muñoz, Severiano Cortés-Franco. Broken surgical blade retrieval following lumbar discectomy through paravertebral/lateral transpsoas approach: A case report. 20-Jan-2021;12:25
How to cite this URL: Pablo Barbero-Aznarez, Carlos Bucheli-Peñafiel, Eduardo Olmos-Francisco, Asís Lorente-Muñoz, Severiano Cortés-Franco. Broken surgical blade retrieval following lumbar discectomy through paravertebral/lateral transpsoas approach: A case report. 20-Jan-2021;12:25. Available from: https://surgicalneurologyint.com/surgicalint-articles/10534/
Abstract
Background: There are rare reports of broken surgical blades occurring during lumbar discectomy, and even fewer that discuss their retrieval.
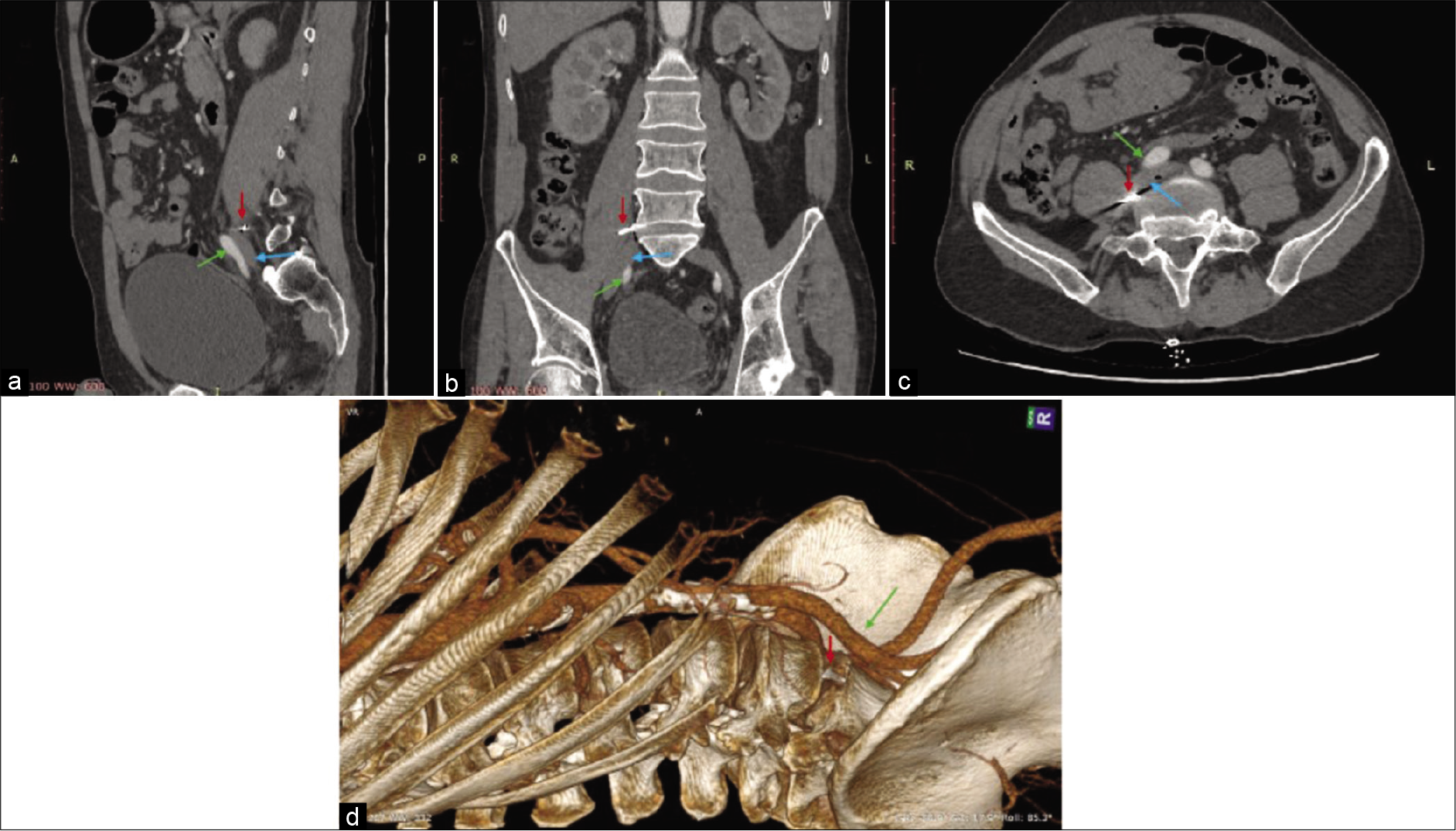
Case Description: While a 54-year-old male was undergoing a lumbar discectomy, the knife blade was broken. As it was difficult to retrieve the fragment through the original incision, the patient was closed, and a postoperative angio-computerized tomography (CT) was obtained. When the CT angiogram (CTA) documented the retained fragment had become lodged near the iliac vein within the psoas muscle, a second operation for blade retrieval, consisting of a paravertebral, lateral transpsoas approach, was successfully performed.
Conclusion: In some cases, it is difficult to retrieve a broken scalpel blade during the index surgery. When this occurs, we would recommend closing the patient, and obtaining a CTA to better document the location of the retained foreign body. Based upon these findings, a safer second stage procedure may be performed (e.g., as in this case using a paravertebral lateral transpsoas approach) to avoid undue sequelae/morbidity.
Keywords: Broken surgical blade, Complication, Lateral transpsoas approach, Lumbar discectomy
INTRODUCTION
There are few guidelines as to how retrieve potentially dangerous fractured surgical blades during index spinal surgical procedures (e.g., endoscopically, transforaminally, robot-assisted laparoscopy, paravertebral lateral transpsoas approach, and other).
Zheng emphasized that in such circumstances, a knife may migrate to a potentially dangerous location,[
Here, following a lumbar discectomy, we utilized a postoperative computerized tomography angiogram (CTA) to identify a retained/migrated knife blade and removed it secondarily through a paravertebral, lateral transpsoas approach.
CASE DESCRIPTION
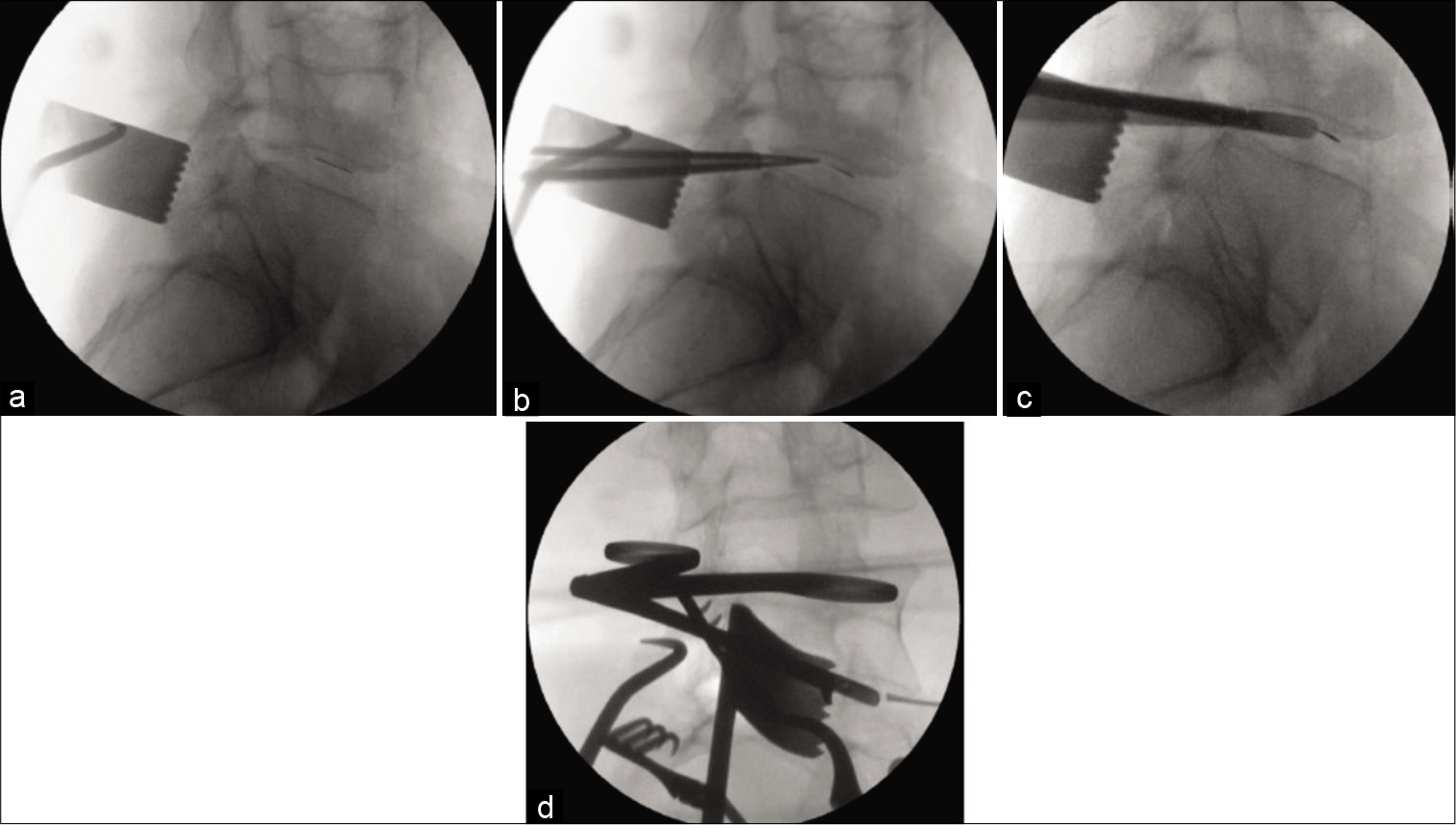
A 54-year-old male underwent a standard L4-L5 discectomy during which the knife blade suddenly broke off. After numerous failed attempts to retrieve the blade under fluoroscopy, the patient was closed, and a CTA was ordered [
DISCUSSION
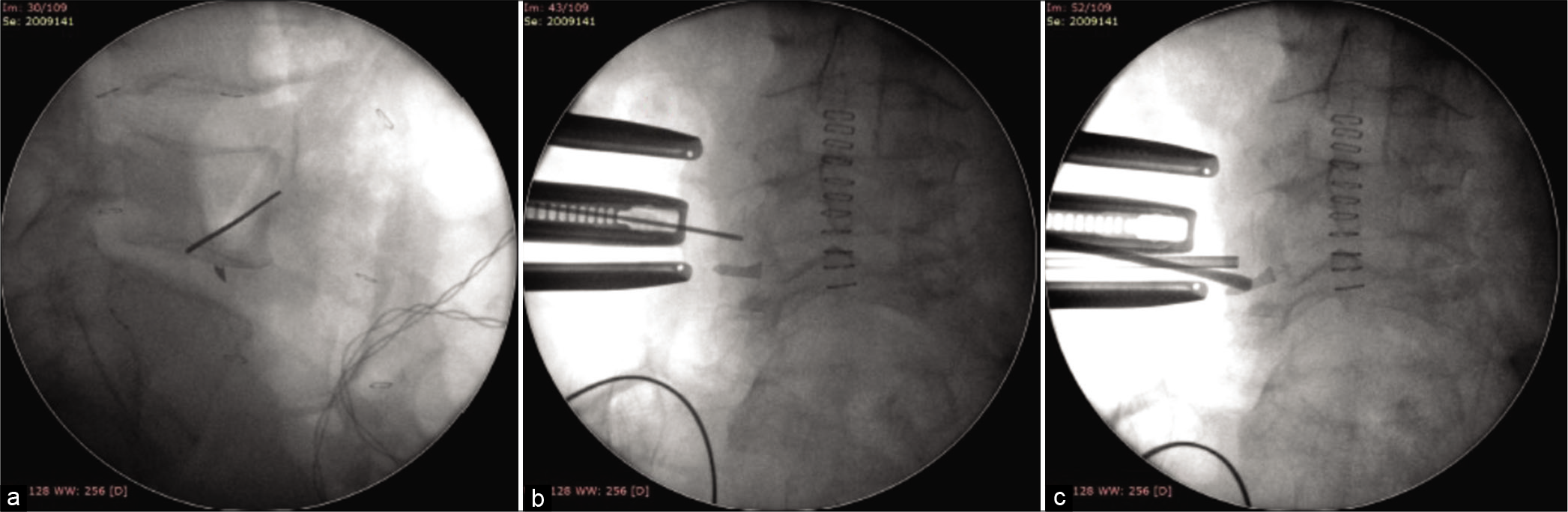
Here, we report a case in which a surgical blade broke off during a L4-L5 discectomy. After obtaining a postoperative CTA, the retained foreign body was safely approached utilizing a secondary paravertebral, lateral transpsoas approach. There are other approaches for retrieving a broken blade in the spine like the transforaminal approach, described by Rahimizadeh et al., not applicable to our particular case [
CONCLUSION
A surgical scalpel broke and significantly migrated during a lumbar discectomy making it impossible to remove at the index procedure. Utilizing a postoperative CTA to document the fragment location (i.e., close to the iliac vein), the patient underwent a secondary paravertebral lateral transpsoas approach for safe scalpel blade excision.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
1. Amirjamshidi A, Mehrazin M, Abbassioun K, Ketabtchi E. Retained broken knife blades within the disc space. Spine (Phila Pa 1976). 1994. 19: 981-4
2. Koutserimpas C, Ioannidis A, Konstantinidis M, Athanasopoulos P, Antonakopoulos F, Konstantinidis K. Robot-assisted removal of a broken scalpel blade following discectomy. Case Rep Surg. 2019. 2019: 8609246
3. Rahimizadeh A, Ghorbani E, Rahimizadeh S. Transforaminal retrieval of intradiscal retained broken surgical knife blade. Spine (Phila Pa 1976). 2013. 38: E1278-81
4. Zheng GB, Wang Z. Removal of the deeply located intradiskal broken knife blade with arthroscopic assistance: Case report and literature review. World Neurosurg. 2020. 137: 272-5